Obstructive lung disease effects — MCQs

Which of the following physiologic changes decreases pulmonary vascular resistance (PVR)?
A previously healthy 64-year-old woman comes to the physician because of a dry cough and progressively worsening shortness of breath for the past 2 months. She has not had fever, chills, or night sweats. She has smoked one pack of cigarettes daily for the past 45 years. She appears thin. Examination of the lung shows a prolonged expiratory phase and end-expiratory wheezing. Spirometry shows decreased FEV1:FVC ratio (< 70% predicted), decreased FEV1, and a total lung capacity of 125% of predicted. The diffusion capacity of the lung (DLCO) is decreased. Which of the following is the most likely diagnosis?
A 57-year-old man presents to the clinic for a chronic cough over the past 4 months. The patient reports a productive yellow/green cough that is worse at night. He denies any significant precipitating event prior to his symptoms. He denies fever, chest pain, palpitations, weight changes, or abdominal pain, but endorses some difficulty breathing that waxes and wanes. He denies alcohol usage but endorses a 35 pack-year smoking history. A physical examination demonstrates mild wheezes, bibasilar crackles, and mild clubbing of his fingertips. A pulmonary function test is subsequently ordered, and partial results are shown below: Tidal volume: 500 mL Residual volume: 1700 mL Expiratory reserve volume: 1500 mL Inspiratory reserve volume: 3000 mL What is the functional residual capacity of this patient?
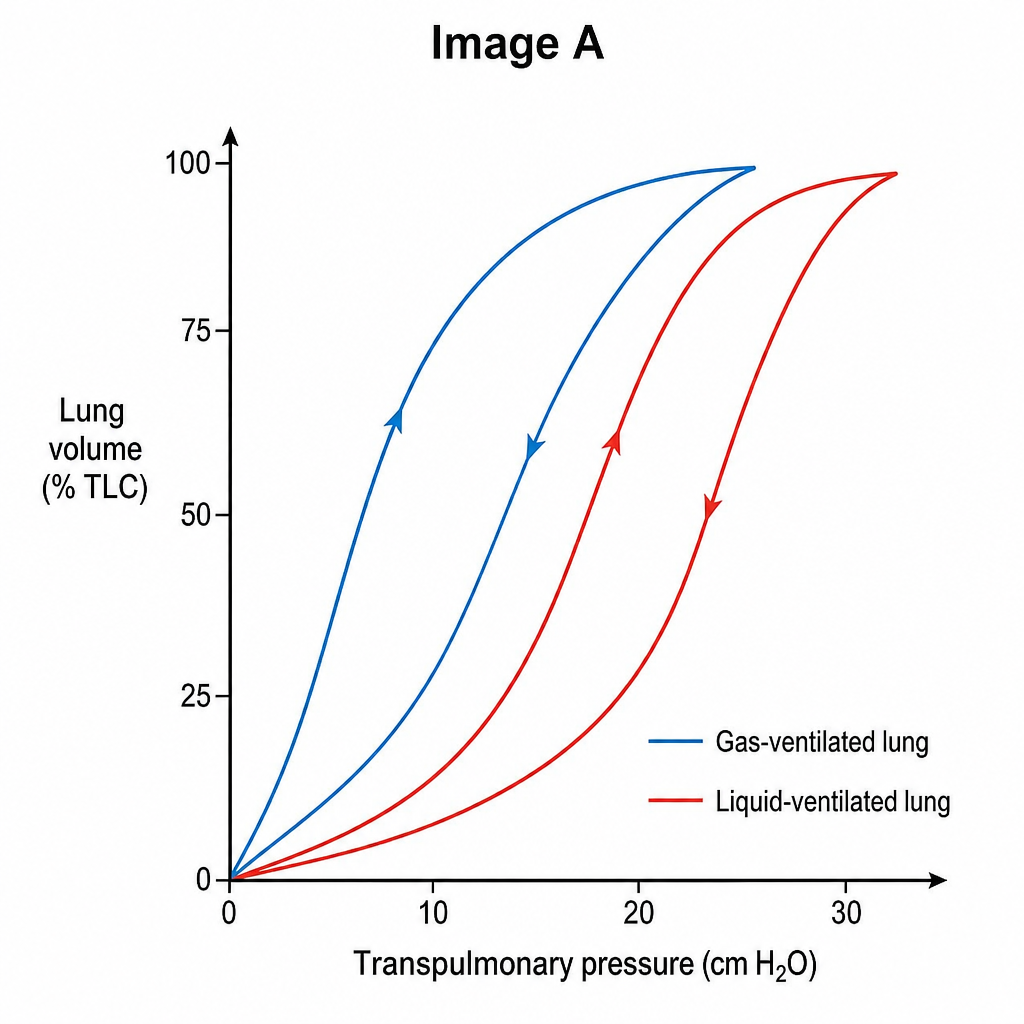
A scientist is designing experiments to better appreciate how the lung expands. He acquires two sets of cat lungs and fills one set with saline. He plots changes in the lungs' volume with respect to pressure as shown in Image A. The pressure-volume loop of the liquid-ventilated lung is different from the gas-ventilated lung because of what property?
A 22-year-old woman presents to the emergency department with a chief concern of shortness of breath. She was hiking when she suddenly felt unable to breathe and had to take slow deep breaths to improve her symptoms. The patient is a Swedish foreign exchange student and does not speak any English. Her past medical history and current medications are unknown. Her temperature is 99.5°F (37.5°C), blood pressure is 127/68 mmHg, pulse is 120/min, respirations are 22/min, and oxygen saturation is 90% on room air. Physical exam is notable for poor air movement bilaterally and tachycardia. The patient is started on treatment. Which of the following best describes this patient's underlying pathology? FEV1 = Forced expiratory volume in 1 second FVC = Forced vital capacity DLCO = Diffusing capacity of carbon monoxide
A 68-year-old man comes to the emergency room with difficulty in breathing. He was diagnosed with severe obstructive lung disease a few years back. He uses his medication but often has to come to the emergency room for intravenous therapy to help him breathe. He was a smoker for 40 years smoking two packs of cigarettes every day. Which of the following best represents the expected changes in his ventilation, perfusion and V/Q ratio?
A 37-year-old woman comes to the physician because of a 10-month history of excessive daytime sleepiness and fatigue. She says she has difficulty concentrating and has fallen asleep at work on numerous occasions. She also reports having frequent headaches during the day. She has no difficulty falling asleep at night, but wakes up gasping for breath at least once. She has always snored loudly and began using an oral device to decrease her snoring a year ago. She has occasional lower back pain, for which she takes tramadol tablets 1–2 times per week. She also began taking one rabeprazole tablet daily 3 weeks ago. She does not smoke. She is 175 cm (5 ft 7 in) tall and weighs 119 kg (262 lb); BMI is 38.8 kg/m2. Her vital signs are within normal limits. Physical and neurologic examinations show no other abnormalities. Arterial blood gas analysis on room air shows: pH 7.35 PCO2 51 mm Hg PO2 64 mm Hg HCO3- 29 mEq/L O2 saturation 92% An x-ray of the chest and ECG show no abnormalities. Which of the following is the most likely cause of this patient's condition?
A 62-year-old man presents to the emergency department for evaluation of a 2-year history of increasing shortness of breath. He also has an occasional nonproductive cough. The symptoms get worse with exertion. The medical history is significant for hypertension and he takes chlorthalidone. He is a smoker with a 40-pack-year smoking history. On physical examination, the patient is afebrile; the vital signs include: blood pressure 125/78 mm Hg, pulse 90/min, and respiratory rate 18/min. The body mass index (BMI) is 31 kg/m2. The oxygen saturation is 94% at rest on room air. A pulmonary examination reveals decreased breath sounds bilaterally, but is otherwise normal with no wheezes or crackles. The remainder of the examination is unremarkable. A chest radiograph shows hyperinflation of both lungs with mildly increased lung markings, but no focal findings. Based on this clinical presentation, which of the following is most likely?
A 3-day-old newborn is brought to the physician because of abdominal distention, inconsolable crying, and 3 episodes of bilious vomiting since the previous evening. He was delivered at home at 40 weeks' gestation by a trained midwife. He has not passed meconium. Physical examination shows abdominal distention, a tight anal sphincter, and an explosive passage of air and feces on removal of the examining finger. Abnormal development of which of the following best explains this patient's condition?
An investigator is studying the outcomes of a malaria outbreak in an endemic region of Africa. 500 men and 500 women with known malaria exposure are selected to participate in the study. Participants with G6PD deficiency are excluded from the study. The clinical records of the study subjects are reviewed and their peripheral blood smears are evaluated for the presence of Plasmodium trophozoites. Results show that 9% of the exposed population does not have clinical or laboratory evidence of malaria infection. Which of the following best explains the absence of infection seen in this subset of participants?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
