Cardiovascular — MCQs

On this page
An 11-year-old boy presents with a 2-day history of uncontrollable shivering. During admission, the patient’s vital signs are within normal limits, except for a fluctuating body temperature registering as low as 35.0°C (95.0°F) and as high as 40.0°C (104.0°F), requiring alternating use of cooling and warming blankets. A complete blood count (CBC) is normal, and a chest radiograph is negative for consolidations and infiltrates. An MRI of the brain reveals a space-occupying lesion infiltrating the posterior hypothalamus and extending laterally. Which of the following additional findings are most likely, based on this patient’s physical examination?
A 25-year-old woman presents to her primary care physician for her yearly physical exam. She has no past medical history and says that she does not currently have any health concerns. On physical exam, she is found to have hyperactive patellar reflexes but says that she has had this finding since she was a child. She asks her physician why this might be the case. Her physician explains that there are certain cells that are responsible for detecting muscle stretch and responding to restore the length of the muscle. Which of the following is most likely a characteristic of these structures?
A 71-year-old man comes to the physician because of decreased sexual performance for the past 2 years. He reports that it takes longer for his penis to become erect, and he cannot maintain an erection for as long as before. His ejaculations have become less forceful. Once he has achieved an orgasm, he requires several hours before he can have another orgasm. He has been happily married for 40 years and he has no marital conflicts. His only medication is esomeprazole for gastroesophageal reflux disease. Examination shows coarse dark pubic and axillary hair. The skin of his lower extremity is warm to the touch; pedal pulses and sensation are intact. Rectal examination shows a symmetrically enlarged prostate with no masses. His fasting serum glucose is 96 mg/dL and his prostate-specific antigen is 3.9 ng/mL (N < 4). Which of the following etiologies is the most likely cause of the patient's symptoms?
A 56-year-old woman presents to the emergency department with an episode of nausea and severe unrelenting right upper abdominal pain. She had a cholecystectomy for gallstones a year earlier and has since experienced frequent recurrences of abdominal pain, most often after a meal. Her past medical history is otherwise unremarkable and she only takes medications for her pain when it becomes intolerable. Her physical exam is normal except for an intense abdominal pain upon deep palpation of her right upper quadrant. Her laboratory values are unremarkable with the exception of a mildly elevated alkaline phosphatase, amylase, and lipase. Her abdominal ultrasound shows a slightly enlarged common bile duct at 8 mm in diameter (N = up to 6 mm) and a normal pancreatic duct. The patient is referred to a gastroenterology service for an ERCP (endoscopic retrograde cholangiopancreatography) to stent her common bile duct. During the procedure the sphincter at the entrance to the duct is constricted. Which statement best describes the regulation of the function of the sphincter which is hampering the cannulation of the pancreatic duct in this patient?
A 34-year-old woman comes to the physician because she has not had her period for 4 months. Menses had previously occurred at regular 28-day intervals with moderate flow. A home pregnancy test was negative. She also reports recurrent headaches and has noticed that when she goes to the movies she cannot see the outer edges of the screen without turning her head to each side. This patient's symptoms are most likely caused by abnormal growth of which of the following?
A 60-year-old male engineer who complains of shortness of breath when walking a few blocks undergoes a cardiac stress test because of concern for coronary artery disease. During the test he asks his cardiologist about what variables are usually used to quantify the functioning of the heart. He learns that one of these variables is stroke volume. Which of the following scenarios would be most likely to lead to a decrease in stroke volume?
A 25-year-old man is admitted to the hospital after a severe motor vehicle accident as an unrestrained front-seat passenger. Appropriate life-saving measures are given, and the patient is now hemodynamically stable. Physical examination shows a complete loss of consciousness. There are no motor or ocular movements with painful stimuli. The patient has bilaterally intact pupillary light reflexes. The patient is placed in a 30° semi-recumbent position for further examination. What is the most likely finding on the examination of this patient's right ear?
A 38-year-old woman presents to the physician’s clinic with a 6-month history of generalized weakness that usually worsens as the day progresses. She also complains of the drooping of her eyelids and double vision that is worse in the evening. Physical examination reveals bilateral ptosis after a sustained upward gaze and loss of eye convergence which improves upon placing ice packs over the eyes and after the administration of edrophonium. Which of the following is an intrinsic property of the muscle group affected in this patient?
A 2-month-old girl with a previous diagnosis of DiGeorge syndrome is brought to the emergency department with her parents following a seizure. Her mother states that the baby had been inconsolable all day and refused to feed. She was born at 39 weeks gestation via spontaneous vaginal delivery. She is up to date on all vaccines. Upon arrival to the hospital her heart rate is 120/min, respiratory rate is 40/min, and temperature of 37.0°C (98.6°F). On examination, she is afebrile and somnolent and her fontanelles are open and soft. While attempting to take her blood pressure, the patient’s arm and hand flex sharply and do not relax until the cuff is released. A light tap on the cheek results in an atypical facial muscle twitch. A CMP and CBC are drawn and sent for analysis. Which of the following is the most likely cause?
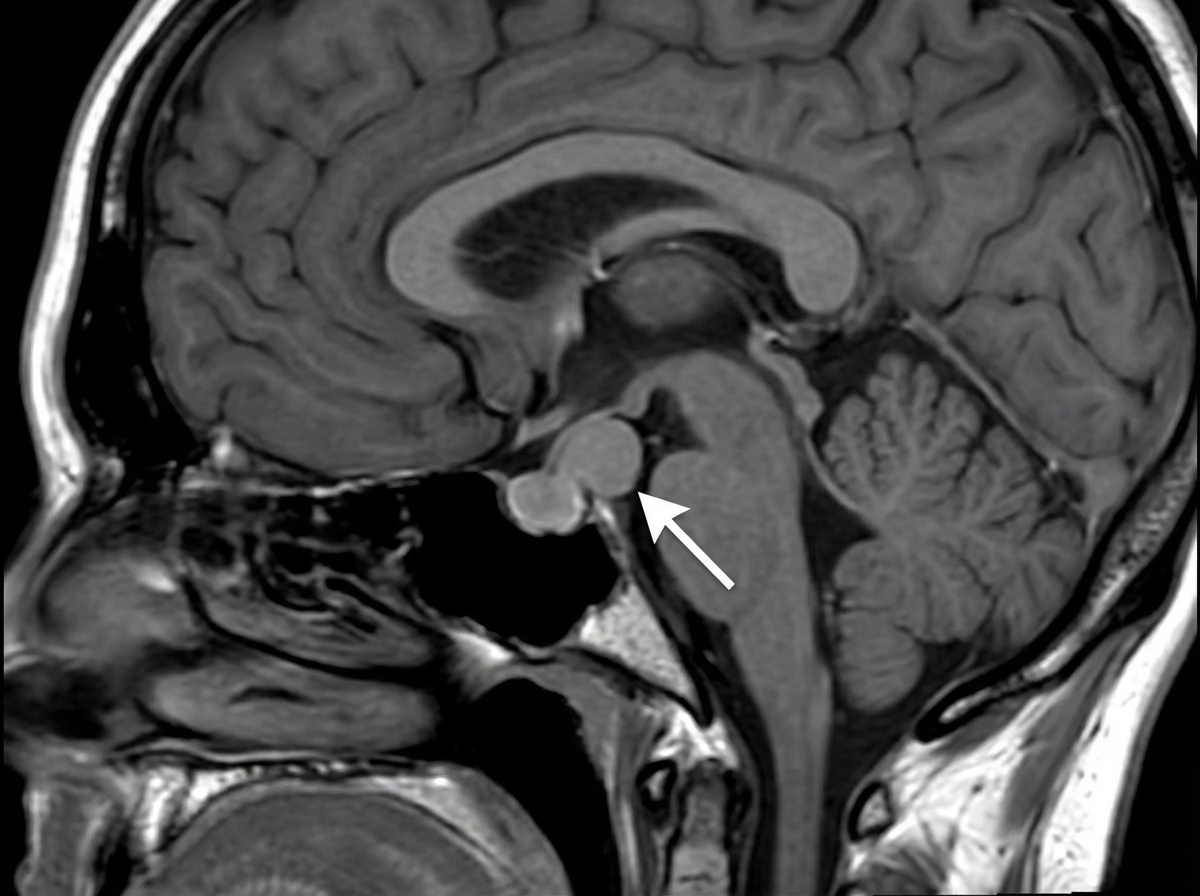
A 17-year-old teenager presents to the clinic with her parents complaining of headaches and loss of vision which began insidiously 3 months ago. She describes her headaches as throbbing, mostly on her forehead, and severe enough to affect her daily activities. She has not experienced menarche. Past medical history is noncontributory. She takes no medication. Both of her parents are alive and well. Today, her blood pressure is 110/70 mm Hg, the heart rate is 90/min, the respiratory rate is 17/min, and the temperature is 37.0°C (98.6°F). Breasts and pubic hair development are in Tanner stage I. Blood work is collected and an MRI is performed (the result is shown). Decreased production of which of the following hormones is the most likely explanation for the patient's signs and symptoms?
Practice by Chapter
Cardiac output determinants
Practice Questions
Starling's law of the heart
Practice Questions
Preload and afterload concepts
Practice Questions
Contractility determinants
Practice Questions
Regulation of blood pressure
Practice Questions
Baroreceptor reflexes
Practice Questions
Neural control of cardiovascular function
Practice Questions
Endothelial function and dysfunction
Practice Questions
Coronary blood flow regulation
Practice Questions
Regional blood flow distribution
Practice Questions
Exercise cardiovascular physiology
Practice Questions
Aging effects on cardiovascular system
Practice Questions
Integrated cardiovascular responses
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
