Cardiovascular — MCQs

On this page
Twenty minutes after delivery of a newborn infant, a 22-year-old woman starts breastfeeding. Initially, the expressed milk is thick and yellowish. Three days later, the mother's breasts swell and the expressed milk becomes thinner and whiter. A decrease in maternal serum concentration of which of the following is most likely responsible for the observed changes in milk production?
A 55-year-old woman has a total thyroidectomy for papillary thyroid carcinoma. She complains of tingling around the mouth 11 hours after the operation. Her condition rapidly deteriorates with difficulty breathing and chest tightness. Which of the following best represent the signaling pathway of the deficient hormone responsible for this patient’s symptoms?
A 28-year-old female comes to the emergency department complaining of heart palpitations. She has had multiple episodes of these in the past few months. She has found that if she wears tight clothing then sometimes these episodes will stop spontaneously. On presentation to the ED, she feels like her heart is pounding and reports feeling nauseous. She appears mildly diaphoretic. Her blood pressure is 125/75 mmHg, pulse is 180/min, and respirations are 22/min with an O2 saturation of 99% on room air. A neck maneuver is performed and her pulse returns to 90/min with improvement of her symptoms. Stimulation of afferent fibers from which nerve are most responsible for the resolution of her symptoms?
A researcher is studying the effects of hormones on different cells within the ovarian follicle. She adds follicle stimulating hormone (FSH) to a culture of ovarian follicle cells. She then measures the activity levels of different enzymes within the cells. Which enzyme and ovarian cell type would be expected to be stimulated by the addition of FSH?
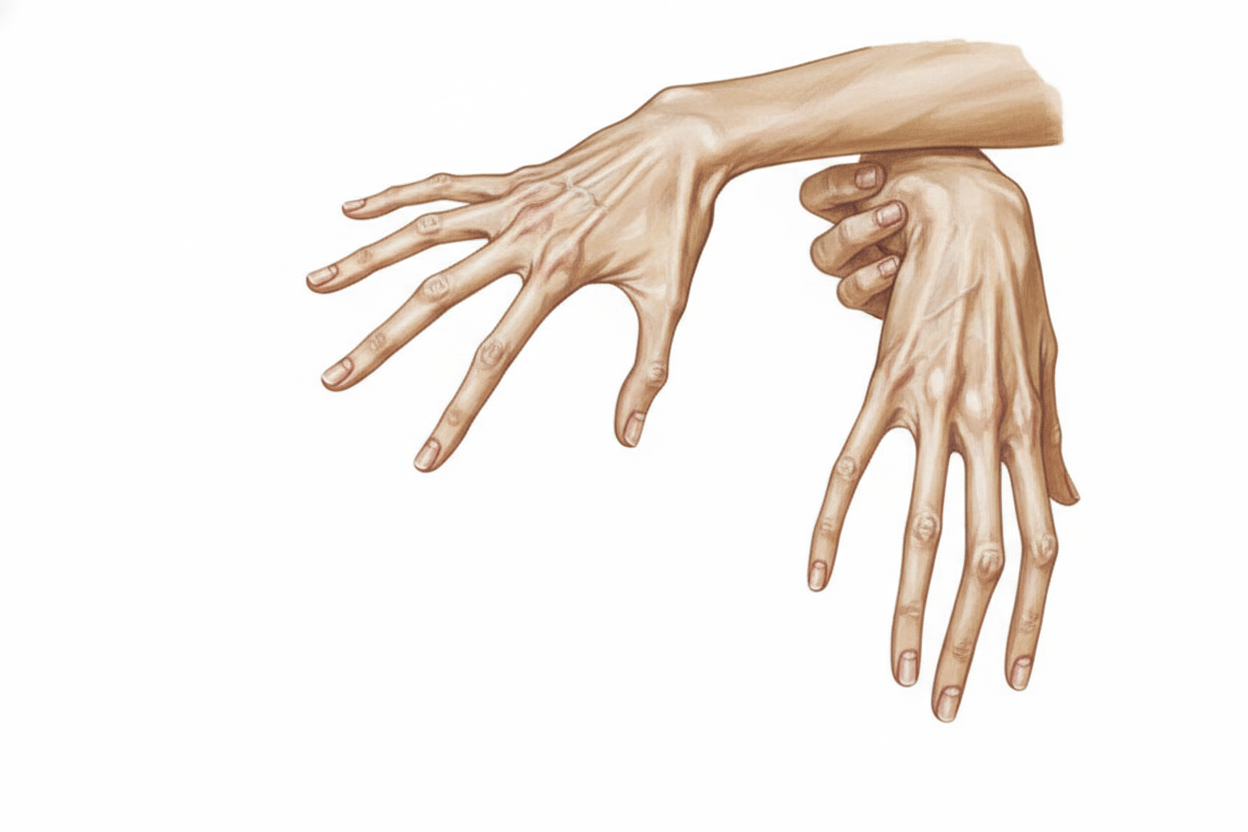
A 27-year-old is going through a pre-employment evaluation. The patient has no history of any medical conditions, but there is a strong family history of ischemic heart disease on his father’s side. The patient drinks alcohol occasionally but does not use any illicit drugs or smoke. On examination, the physician notices that the patient has a very flexible body and long fingers (seen in the image). Auscultation of the heart reveals a mid-systolic click over the apex. What is the most likely mechanism behind this finding?
A 29-year-old woman presents to a physician for evaluation of palpitations, increased sweating, and unintentional weight loss despite a good appetite. She also reports difficulty swallowing and voice changes. All of the symptoms have developed over the past 6 months. The patient has no concurrent illnesses and takes no medications. The vital signs include the following: blood pressure 125/80 mm Hg, heart rate 106/min, respiratory rate 15/min, and temperature 37.0℃ (98.6℉). The physical examination was significant for increased perspiration, fine digital tremors, and a small mass on the posterior aspect of the tongue, which moves with movements of the tongue. There is no neck swelling. The thyroid profile is as follows: Triiodothyronine (T3) 191 ng/dL (2.93 nmol/L) Thyroxine (T4), total 22 µg/dL (283.1 nmol/L) Thyroid-stimulating hormone (TSH) 0.2 µU/mL (0.2 mU/L) A radioiodine thyroid scan reveals hyper-functional thyroid tissue at the base of the patient’s tongue. Which of the following statements is correct?
A 42-year-old man is referred for an endocrinology consult because of decreased triiodothyronine (T3) hormone levels. He presented to the emergency department 1 week prior to this consultation with pneumonia and was admitted to a medicine service for management of his infection. He has since recovered from his infection after intravenous antibiotic administration. He currently has no symptoms and denies feeling cold or lethargic. A panel of laboratory tests are obtained with the following results: Thyroid-stimulating hormone: 4.7 µU/mL Thyroxine (T4): 6 µg/dL Triiodothyronine (T3): 68 ng/dL Which of the following additional findings would most likely also be seen in this patient?
A 15-year-old boy is brought to the emergency department by his father 10 minutes after falling into a frozen lake during ice fishing. He was in the water for less than 1 minute before his father managed to pull him out. On arrival, his clothes are still wet and he appears scared. His body temperature is 36.2°C (97.1°F), pulse is 102/min, blood pressure is 133/88 mm Hg. Which of the following mechanisms contributes most to maintaining this patient's core body temperature?
A 43-year-old woman comes to the physician because of a 3-month history of tremor, diarrhea, and a 5-kg (11-lb) weight loss. Her pulse is 110/min. Examination shows protrusion of the eyeball when looking forward. A bruit is heard over the anterior neck on auscultation. Serum studies show autoantibodies to the thyroid-stimulating hormone receptor. The patient decides to undergo definitive treatment for her condition with a radioactive tracer. The success of this treatment directly depends on the activity of which of the following?
A scientist is studying patients with neuromuscular weakness and discovers a mutation in a plasma membrane ion channel. She thinks that this mutation may have an effect on the dynamics of action potentials so she investigates its effect in an isolated neuronal membrane. She finds that the ion channel has no effect when potassium, sodium, and calcium are placed at physiological concentrations on both sides of the membrane; however, when some additional potassium is placed inside the membrane, the channel rapidly allows for sodium to enter the membrane. She continues to examine the mutant channel and finds that it is more rapidly inactivated compared with the wildtype channel. Which of the following effects would this mutant channel most likely have on the electrical profile of neurons in these patients?
Practice by Chapter
Cardiac output determinants
Practice Questions
Starling's law of the heart
Practice Questions
Preload and afterload concepts
Practice Questions
Contractility determinants
Practice Questions
Regulation of blood pressure
Practice Questions
Baroreceptor reflexes
Practice Questions
Neural control of cardiovascular function
Practice Questions
Endothelial function and dysfunction
Practice Questions
Coronary blood flow regulation
Practice Questions
Regional blood flow distribution
Practice Questions
Exercise cardiovascular physiology
Practice Questions
Aging effects on cardiovascular system
Practice Questions
Integrated cardiovascular responses
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
