Cardiovascular — MCQs

On this page
A team of researchers is investigating different mechanisms of transmitting sensory information in the body. They are particularly interested in the different types of sensory receptors. From a sample of tissue, they isolate a receptor that is encased in deep skin layers and joints. The receptor adapts quickly and they discover its role is to sense vibration and pressure. Which of the following types of nerve fibers is most likely used by this receptor to transmit sensory information?
A 58-year-old man with history of diabetes and hypertension suffers a cardiac arrest at home. The family calls 911, yet no one performs CPR. Five minutes after the arrest, EMS arrives to begin resuscitation. At this point, which region of the CNS is most likely to suffer ischemic damage?
A 4-day-old healthy male infant is born with normal internal and external male reproductive organs. Karyotype analysis reveals a 46XY genotype. Production of what substance by which cell type is responsible for the development of the normal male seminal vesicles, epididymides, ejaculatory ducts, and ductus deferens?
A 39-year-old woman presents to her primary care physician because she has been experiencing intermittent abdominal pain for the last 2 weeks. She says that the pain is squeezing in nature, is located in the right upper quadrant, and is particularly severe after eating a meal. After a diagnosis is made, the patient asks why the pain gets worse after eating. The physician explains that food is detected by the gastrointestinal tract through numerous receptors and that this information is transmitted to other parts of the body to cause compensatory changes. The neurons responsible for transmitting this information are most likely located in a layer of the intestine that has which of the following characteristics?
A 32-year-old woman patient presents to her family physician with recurrent retrosternal chest pain. She has had similar episodes for the past 7 months along with difficulty swallowing solid as well as liquid food. She recently completed an 8-week course of a proton pump inhibitor, but she is still bothered by the feeling that food gets stuck down her 'food pipe'. Her pain is not related to exertion. She denies any history of acid reflux disease. Her blood pressure is 125/81 mm Hg, respirations are 21/min, pulse is 78/min, and temperature is 36.7°C (98.1°F). She currently does not have pain. A barium swallow X-ray image is normal. Which of the following tests would aid in the diagnosis of this patient's condition?
A physiologist is studying various mediators that modulate coronary circulation. He is particularly looking at mediators that are activated via the clotting cascade, primarily activated factor XII. He finds that when the clotting cascade starts, it leads to the activation of factor XII, which in turn activates the enzyme kallikrein. This enzyme activates high and low-molecular-weight precursors of certain mediators, which work by contracting the visceral smooth muscle while relaxing the vascular smooth muscle. They are primarily associated with hypersensitivity and can cause an increase in capillary permeability, pain, and mobilize leukocytes. Which of the following is the precursor protein for the mediators the physiologist is studying?
A 30-year-old woman comes to the physician because of a 1-month history of intermittent abdominal pain, flatulence, and watery diarrhea. The episodes typically occur 2–3 hours after meals, particularly following ingestion of ice cream, cheese, and pizza. She is administered 50 g of lactose orally. Which of the following changes is most likely to be observed in this patient?
A 29-year-old man is brought to the emergency room 6 hours after the onset of severe epigastric pain and vomiting. His heart rate is 110/min and blood pressure is 98/72 mm Hg. He is diagnosed with acute pancreatitis, and fluid resuscitation with normal saline is initiated. Which of the following is the most likely immediate effect of fluid resuscitation in this patient?
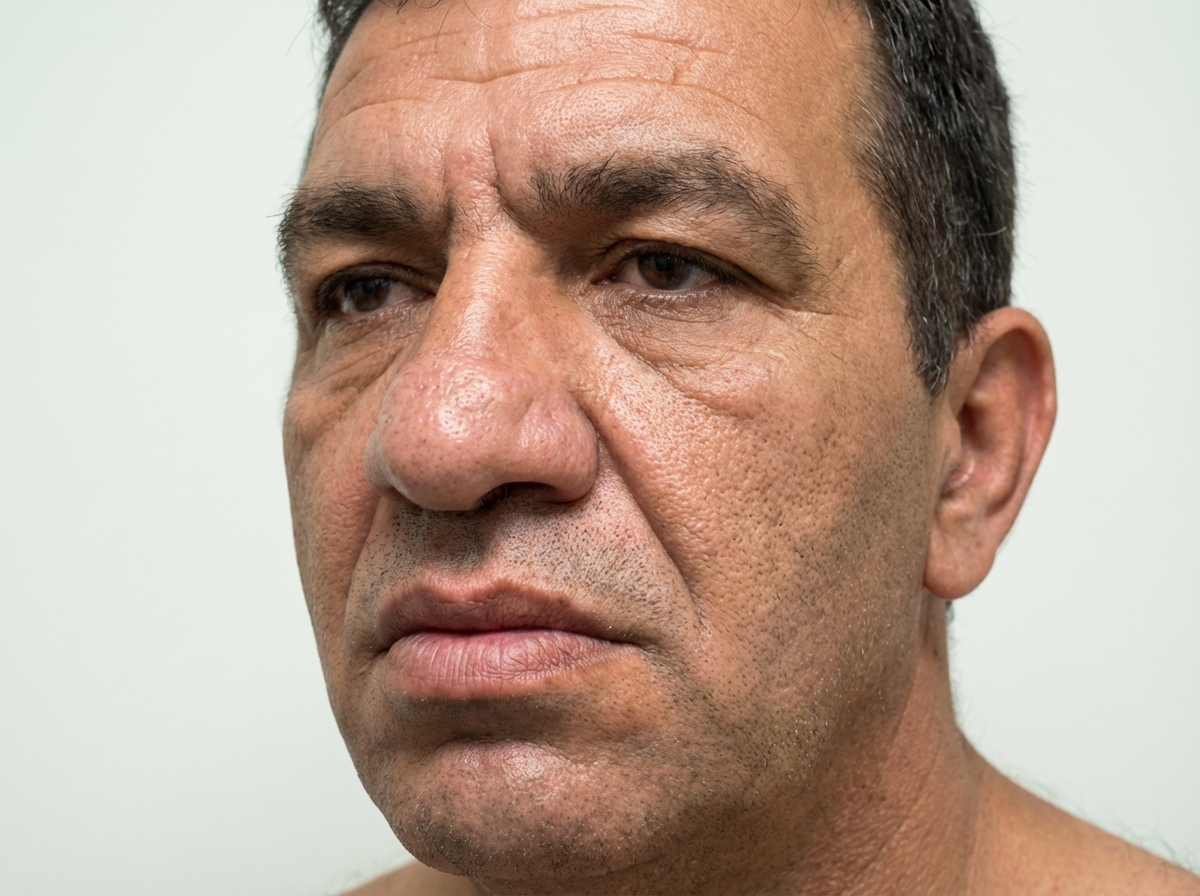
A 38-year-old man presents to the endocrinologist with complaints of increased shoe size and headaches in the morning. These symptoms have developed gradually over the past year but have become especially concerning because he can no longer wear his normal-sized boots. He denies any other symptoms, including visual changes. He was recently started on lisinopril by his primary care physician for high blood pressure. His vital signs are within normal limits and stable. On exam, the endocrinologist notes the findings shown in Figures A and B. These facial features are especially striking when contrasted with his drivers license from 10 years prior, when his jaw was much less prominent. The endocrinologist sends a screening blood test to work-up the likely diagnosis. Which of the following organs or glands produces the molecule being tested in this screening?
A 55-year-old man comes to the physician because of progressive daytime sleepiness and exertional dyspnea for the past 6 months. Physical examination shows conjunctival pallor and several subcutaneous purple spots on his legs. His hemoglobin concentration is 8.5 g/dL, leukocyte count is 3,000/mm3, and platelet count is 16,000/mm3. Which of the following laboratory values is most likely to be increased in this patient?
Practice by Chapter
Cardiac output determinants
Practice Questions
Starling's law of the heart
Practice Questions
Preload and afterload concepts
Practice Questions
Contractility determinants
Practice Questions
Regulation of blood pressure
Practice Questions
Baroreceptor reflexes
Practice Questions
Neural control of cardiovascular function
Practice Questions
Endothelial function and dysfunction
Practice Questions
Coronary blood flow regulation
Practice Questions
Regional blood flow distribution
Practice Questions
Exercise cardiovascular physiology
Practice Questions
Aging effects on cardiovascular system
Practice Questions
Integrated cardiovascular responses
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
