Cytochrome P450 system — MCQs

A 63-year-old man comes to the physician for a routine health maintenance examination. He feels well. He has a history of hypertension, atrial fibrillation, bipolar disorder, and osteoarthritis of the knees. Current medications include lisinopril, amiodarone, lamotrigine, and acetaminophen. He started amiodarone 6 months ago and switched from lithium to lamotrigine 4 months ago. The patient does not smoke. He drinks 1–4 beers per week. He does not use illicit drugs. Vital signs are within normal limits. Examination shows no abnormalities. Laboratory studies show: Serum Na+ 137 mEq/L K+ 4.2 mEq/L Cl- 105 mEq/L HCO3- 24 mEq/L Urea nitrogen 14 mg/dL Creatinine 0.9 mg/dL Alkaline phosphatase 82 U/L Aspartate aminotransferase (AST) 110 U/L Alanine aminotransferase (ALT) 115 U/L Which of the following is the most appropriate next step in management?
A 14-year-old boy is brought to the emergency department because of a 4-hour history of vomiting, lethargy, and confusion. Three days ago, he was treated with an over-the-counter medication for fever and runny nose. He is oriented only to person. His blood pressure is 100/70 mm Hg. Examination shows bilateral optic disc swelling and hepatomegaly. His blood glucose concentration is 65 mg/dL. Toxicology screening for serum acetaminophen is negative. The over-the-counter medication that was most likely used by this patient has which of the following additional effects?
A 75-year-old female patient comes to the emergency department with altered mental status. She is brought in by her daughter with whom the patient lives. The patient’s daughter said they were watching TV when her mother became unresponsive. On exam the patient withdraws to pain but does not open her eyes or speak. An emergent head CT is done and shows an intracranial bleed. The patient is moved to the ICU and intubated. Further history is obtained from the daughter. The patient has a past medical history of diabetes and a previous stroke. Her medications are metformin and warfarin. The patient is compliant with all of her medications. The daughter says that the patient changed her diet about 1 month ago in response to a diet she saw on a talk show. Which of the following foods is most likely to cause the pathology seen in this patient?
A 58-year-old man comes to the physician because of severe muscle aches and fatigue for 3 days. Last week he was diagnosed with atypical pneumonia and treated with clarithromycin. He has hyperlipidemia for which he takes lovastatin. Physical examination shows generalized tenderness of the proximal muscles in the upper and lower extremities. Serum studies show an elevated creatine kinase concentration. This patient's current symptoms are most likely caused by inhibition of which of the following hepatic enzymes?
A 28-year-old woman presents to a psychiatrist with a 10-year history of unexplained anxiety symptoms. To date, she has not visited any psychiatrist, because she believes that she should not take medicines to change her emotions or thoughts. However, after explaining the nature of her disorder, the psychiatrist prescribes daily alprazolam. When she comes for her first follow-up, she reports excellent relief from her symptoms without any side-effects. The psychiatrist encourages her to continue her medication for the next 3 months and then return for a follow-up visit. After 3 months, she tells her psychiatrist that she has been experiencing excessive sedation and drowsiness over the last few weeks. The psychiatrist finds that she is taking alprazolam in the correct dosage, and she is not taking any other medication that causes sedation. Upon asking her about any recent changes in her lifestyle, she mentions that for the last 2 months, she has made a diet change. The psychiatrist tells her that diet change may be the reason why she is experiencing excessive sedation and drowsiness. Which of the following is the most likely diet change the psychiatrist is talking about?
A 76-year-old man comes to the physician for a follow-up examination. One week ago, he was prescribed azithromycin for acute bacterial sinusitis. He has a history of atrial fibrillation treated with warfarin and metoprolol. Physical examination shows no abnormalities. Compared to one month ago, laboratory studies show a mild increase in INR. Which of the following best explains this patient's laboratory finding?
You are currently employed as a clinical researcher working on clinical trials of a new drug to be used for the treatment of Parkinson's disease. Currently, you have already determined the safe clinical dose of the drug in a healthy patient. You are in the phase of drug development where the drug is studied in patients with the target disease to determine its efficacy. Which of the following phases is this new drug currently in?
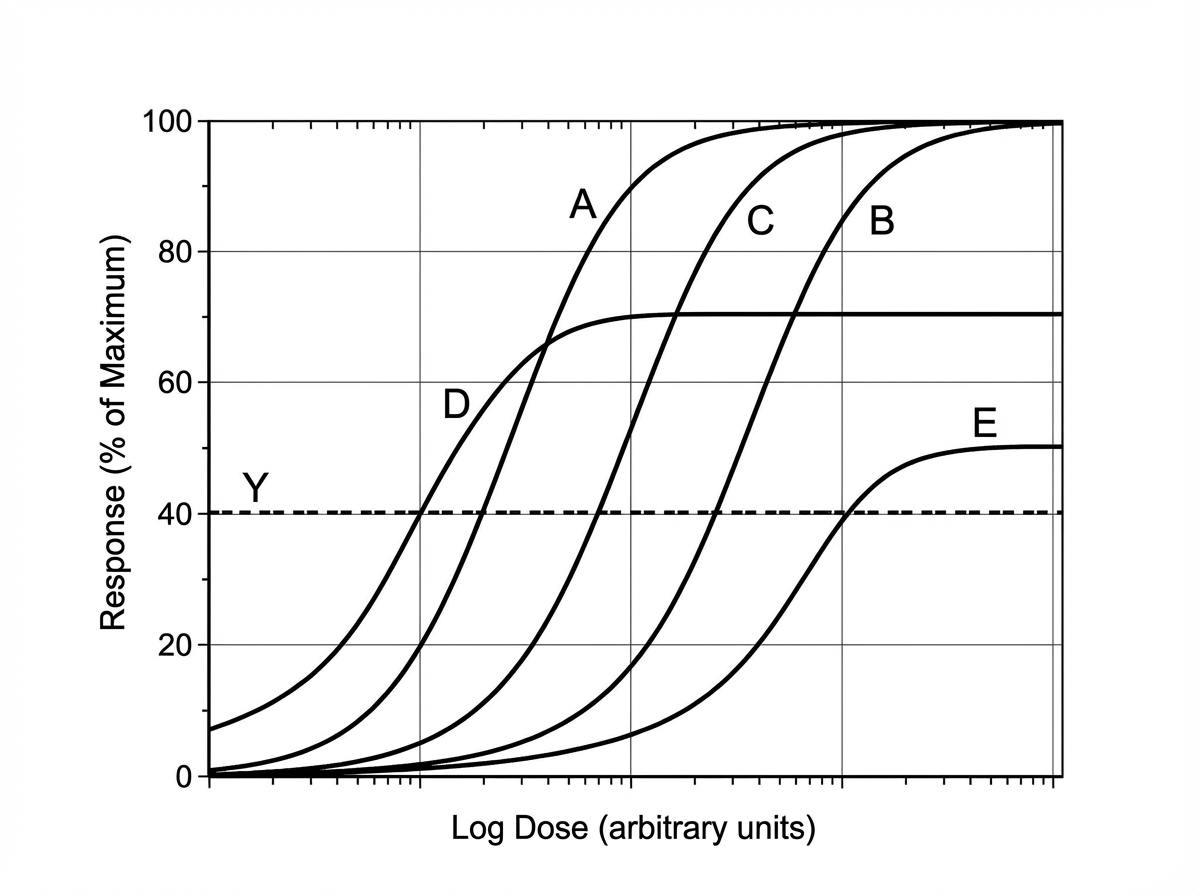
Scientists are developing a new non-steroidal anti-inflammatory drug for osteoarthritis. Their hope is that the new drug will have a higher potency but the same efficacy as ibuprofen in the hope of minimizing gastrointestinal side effects. If ibuprofen is curve C in the figure provided, which of the following would be the curve for the new drug based on the scientists’ specifications? The desired therapeutic effect in patients is represented by the dashed line Y.
Serum studies show a troponin T concentration of 6.73 ng/mL (N < 0.01), and fingerstick blood glucose concentration of 145 mg/dL. The cardiac catheterization team is activated. Treatment with unfractionated heparin, aspirin, ticagrelor, and sublingual nitroglycerin is begun, and the patient's pain subsides. His temperature is 37.3°C (99.1°F), pulse is 65/min, respirations are 23/min, and blood pressure is 91/60 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 96%. Which of the following is the most appropriate additional pharmacotherapy?
A 44-year-old man presents to the clinic with recurrent epigastric pain following meals for a month. He adds that the pain radiates up his neck and throat. Over the counter antacids have not helped. On further questioning, he endorses foul breath upon waking in the morning and worsening of pain when lying down. He denies any recent weight loss. His temperature is 37°C (98.6°F), respirations are 15/min, pulse is 70/min, and blood pressure is 100/84 mm Hg. A physical examination is performed which is within normal limits except for mild tenderness on deep palpation of the epigastrium. An ECG performed in the clinic shows no abnormalities. What is the next best step in the management of this patient?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
