Autonomic/CV Drugs — MCQs

On this page
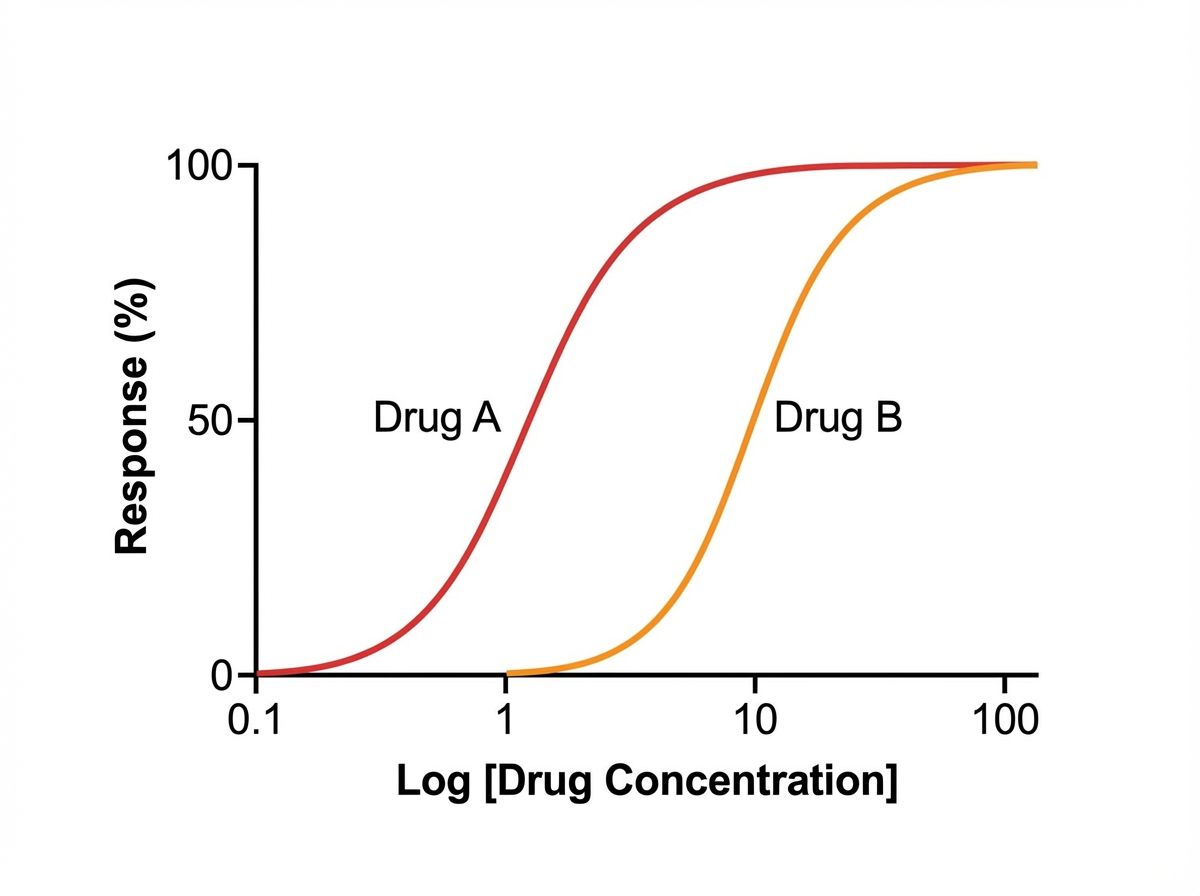
A student is reviewing the various effects that can be plotted on a dose-response curve. He has observed that certain drugs can work as an agonist and an antagonist at a particular site. He has plotted a particular graph (as shown below) and is checking for other responses that can be measured on the same graph. He learned that drug B is less potent than drug A. Drug B also reduces the potency of drug A when combined in the same solution; however, if additional drug A is added to the solution, the maximal efficacy (Emax) of drug A increases. He wishes to plot another curve for drug C. He learns that drug C works on the same molecules as drugs A and B, but drug C reduces the maximal efficacy (Emax) of drug A significantly when combined with drug A. Which of the following best describes drug C?
An obese, 66-year-old woman comes to the physician for a routine health maintenance examination. She feels well but is unhappy about being overweight. She reports that she feels out of breath when walking for more than one block and while climbing stairs. She has tried to lose weight for several years without success. She goes for a walk 3 times a week but she has difficulty following a low-calorie diet. During the past 12 months, she has had two urinary tract infections that were treated with fosfomycin. She has type 2 diabetes mellitus and osteoarthritis. Her only current medication is metformin. She has never smoked. She is 160 cm (5 ft 3 in) tall and weighs 100 kg (220 lb); BMI is 39.1 kg/m2. Vital signs are within normal limits. Physical examination shows cracking in both knees on passive movement. The remainder of the examination shows no abnormalities. Serum studies show an HbA1c of 9.5%, and a fasting serum glucose concentration of 158 mg/dL. An ECG shows no abnormalities. Which of the following is the most appropriate pharmacotherapy?
A 65-year-old male with a history of CHF presents to the emergency room with shortness of breath, lower leg edema, and fatigue. He is diagnosed with acute decompensated congestive heart failure, was admitted to the CCU, and treated with a medication that targets beta-1 adrenergic receptors preferentially over beta-2 adrenergic receptors. The prescribing physician explained that this medication would only be used temporarily as its efficacy decreases within 2-3 days due to receptor downregulation. Which of the following was prescribed?
A 42-year-old male presents to the emergency department due to severe headaches and palpitations. He has had previous episodes of sweating and headache, but this episode was particularly disabling. Upon presentation, he appears pale and diaphoretic. His temperature is 99.3°F (37.4°C), blood pressure is 162/118 mmHg, pulse is 87/min, and respirations are 20/min. Based on clinical suspicion, an abdominal CT scan is obtained, which shows a retroperitoneal mass. This patient's increased heart rate is most likely due to a change in activity of which of the following channels?
A 28-year-old woman comes to the emergency department because of increasing abdominal pain for 2 days. The pain is diffuse and constant, and she describes it as 7 out of 10 in intensity. She has also had numbness in her lower extremities for 12 hours. She has type 1 diabetes mellitus, migraine with aura, and essential tremor. She appears uncomfortable. She is oriented to place and person only. Her temperature is 37°C (98.6°F), pulse is 123/min, and blood pressure is 140/70 mm Hg. Examination shows a distended abdomen with no tenderness to palpation. Bowel sounds are decreased. Muscle strength and sensation is decreased in the lower extremities. There is a tremor of the right upper extremity. Urinalysis shows elevated levels of aminolevulinic acid and porphobilinogen. Which of the following is the most likely cause of this patient's symptoms?
A 10-year-old girl is brought to the emergency department by her mother 30 minutes after having had a seizure. When her mother woke her up that morning, the girl's entire body stiffened and she started shaking vigorously for several minutes. Her mother also reports that over the past few months, her daughter has had multiple episodes of being unresponsive for less than a minute, during which her eyelids were fluttering. The girl did not recall these episodes afterwards. Upon arrival, she appears drowsy. Neurologic examination shows no abnormalities. Which of the following is the most appropriate pharmacotherapy to prevent recurrence of this patient's symptoms?
A man returns home late at night to find his 15-year-old son and 40-year-old wife unconscious in the family room. He immediately summons emergency services. In the field, pulse oximetry shows oxygen saturation at 100% for both patients. 100%, yet they both appear cyanotic. Both patients are provided with 2L of oxygen by way of nasal cannula on the way to the hospital. An arterial blood gas is performed on the teenager and reveals pH of 7.35, PaCO2 of 31.8 mm Hg, PaO2 of 150 mm Hg, HCO3- of 20 mEq/L, SaO2 of 80%, and a COHb of 18%. What is the most likely cause of his condition?
A middle-aged homeless man is found lying unresponsive on the streets by the police and is rushed to the emergency department. His vital signs include: blood pressure 110/80 mm Hg, pulse rate 100/min, and respirations 10/min and shallow. On physical examination, his extremities are cold and clammy. Pupils are constricted and non-reactive. His blood glucose is 55 mg/dL. IV access is established immediately with the administration of dextrose and naloxone. In half an hour, the patient is fully conscious, alert and responsive. He denies any medical illnesses, hospitalizations, or surgeries in the past. Physical examination reveals injection track marks along both arms. He admits to the use of cocaine and heroin. He smokes cigarettes and consumes alcohol. His vital signs are now stable. A urine sample is sent for toxicology screening. Which of the following was the most likely cause of this patient’s respiratory depression?
A 29-year-old woman comes to the physician because of intermittent episodes of sharp chest pain and palpitations. She appears nervous. Her pulse is 115/min and irregularly irregular, and blood pressure is 139/86 mmHg. Examination shows a fine tremor on both hands and digital swelling; the extremities are warm. There is retraction of the right upper eyelid. Which of the following is the most appropriate next step in the management of this patient?
A P1G0 diabetic woman is at risk of delivering at 30 weeks gestation. Her obstetrician counsels her that there is a risk the baby could have significant pulmonary distress after it is born. However, she states she will administer a drug to the mother to help prevent this from occurring. By what action will this drug prevent respiratory distress in the premature infant?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
