Autonomic/CV Drugs — MCQs

On this page
A hospitalized 70-year-old woman, who recently underwent orthopedic surgery, develops severe thrombocytopenia of 40,000/mm3 during her 7th day of hospitalization. She has no other symptoms and has no relevant medical history. All of the appropriate post-surgery prophylactic measures had been taken. Her labs from the 7th day of hospitalization are shown here: The complete blood count results are as follows: Hemoglobin 13 g/dL Hematocrit 38% Leukocyte count 8,000/mm3 Neutrophils 54% Bands 3% Eosinophils 1% Basophils 0% Lymphocytes 33% Monocytes 7% Platelet count 40,000/mm3 The coagulation tests are as follows: Partial thromboplastin time (activated) 85 seconds Prothrombin time 63 seconds Reticulocyte count 1.2% Thrombin time < 2 seconds deviation from control The lab results from previous days were within normal limits. What is the most likely cause of the thrombocytopenia?
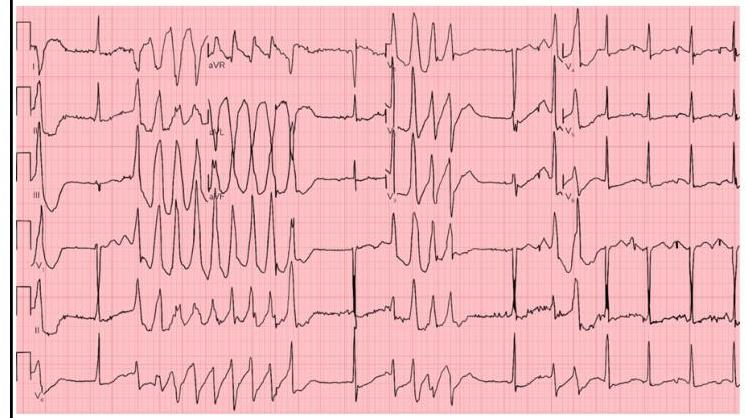
A 53-year-old man with obesity and heart disease presents to your outpatient clinic with complaints of orthopnea, significant dyspnea on minimal exertion, nausea, vomiting, and diarrhea. He says that his old doctor gave him "some pills" that he takes in varying amounts every morning. Physical exam is significant for a severely displaced point of maximal impulse, bilateral rales in the lower lung fields, an S3 gallop, and hepatomegaly. You decide to perform an EKG (shown in figure A). Suddenly, his rhythm changes to ventricular tachycardia followed by ventricular fibrillation, and he syncopizes and expires despite resuscitative efforts. High levels of which medication are most likely responsible?
Four days after admission to the hospital for anorexia nervosa, a 20-year-old woman has new-onset palpitations and paresthesias in all four limbs. Prior to admission, she was found unconscious by her parents on the floor of a residential treatment center. The patient was started on a trial of nutritional rehabilitation upon arrival to the hospital. Her temperature is 36°C (96.8°F), pulse is 47/min, and blood pressure is 90/60 mmHg. She is 160 cm tall and weighs 35 kg; BMI is 14 kg/m2. The patient appears emaciated. Examination shows lower leg edema. A 2/6 holosystolic murmur is heard over the 5th intercostal space at the midclavicular line. An ECG shows intermittent supraventricular tachycardia and QTc prolongation. Serum studies show: Day 2 Day 4 Potassium (mEq/L) 3.5 2.7 Calcium (mg/dL) 8.5 7.8 Magnesium (mEq/L) 1.2 0.5 Phosphorus (mg/dL) 3.6 1.5 Which of the following is the most likely underlying cause of this patient's condition?
A 23-year-old patient with a past medical history of anxiety and appropriately treated schizophrenia presents to the emergency department for a first time seizure. The patient was at home eating dinner when he began moving abnormally and did not respond to his mother, prompting her to bring him in. His symptoms persisted in the emergency department and were successfully treated with diazepam. The patient is discharged and scheduled for a follow up appointment with neurology the next day for treatment. The patient returns to his neurologist 1 month later for a checkup. Physical exam is notable for carpopedal spasm when his blood pressure is being taken. Cranial nerves II-XII are grossly intact and his gait is stable. Which of the following is the most likely explanation of this patient's current presentation?
A 72-year-old man presents to his primary care provider to discuss the frequency with which he wakes up at night to urinate. He avoids drinking liquids at night, but the symptoms have progressively worsened. The medical history is significant for hypertension and hyperlipidemia. He takes lisinopril, atorvastatin, and a multivitamin every day. Today, the vital signs include: blood pressure 120/80 mm Hg, heart rate 90/min, respiratory rate 17/min, and temperature 37.0°C (98.6°F). On physical examination, he appears tired. The heart has a regular rate and rhythm and the lungs are clear to auscultation bilaterally. A bedside bladder ultrasound reveals a full bladder. A digital rectal exam reveals an enlarged and symmetric prostate free of nodules, that is consistent with benign prostatic enlargement. He also has a history of symptomatic hypotension with several episodes of syncope in the past. The patient declines a prostate biopsy that would provide a definitive diagnosis and requests less invasive treatment. Which of the following is recommended to treat this patient’s enlarged prostate?
A 53-year-old woman comes to the physician for a follow-up examination. One month ago, she was diagnosed with carcinoma of the left breast. She underwent a lumpectomy for a 2.1-cm mass and sentinel lymph node biopsy 2 weeks ago. The biopsy of the breast mass showed margin-free invasive ductal carcinoma; immunohistochemistry showed the carcinoma is estrogen-receptor and progesterone-receptor negative, and HER2-receptor positive. The lymph node biopsy was negative for metastases. Examination shows a healing surgical incision over the left breast. There is no palpable axillary lymphadenopathy. Her physician decides to initiate treatment with appropriate pharmacotherapy. Which of the following is the most appropriate next step in management?
Several patients at a local US hospital present with chronic secretory diarrhea. Although there are multiple potential causes of diarrhea present in these patients, which of the following is most likely the common cause of their chronic secretory diarrhea?
A 71-year-old man presents to the clinic with complaints of right wrist pain for 2 days. On examination, redness and swelling were noted on the dorsal aspect of his right wrist. He had pain with extreme range of motion of the wrist. His history includes 2 hip replacements, 2 previous episodes of gout in both first metatarsophalangeal joints, and hypertension. Two days later, the swelling had increased in the dorsal aspect of his right wrist and hand. Wrist flexion was limited to 80% with severe pain. The pain was present on palpation of the scaphoid bone. Due to the suspicion of fracture, the patient was referred to his general practitioner for radiographs. These findings were consistent with gouty arthritis. What is the most likely cytokine involved in this process?
A 23-year-old man comes to the physician because of recurrent episodes of chest pain, shortness of breath, palpitations, and a sensation of choking. The symptoms usually resolve with deep breathing exercises after about 5 minutes. He now avoids going to his graduate school classes because he is worried about having another episode. Physical examination is unremarkable. Treatment with lorazepam is initiated. The concurrent intake of which of the following drugs should be avoided in this patient?
A researcher is studying how arachidonic acid metabolites mediate the inflammatory response in rats. She has developed multiple enzyme inhibitors that specifically target individual proteins in the arachidonic acid pathway. She injects these inhibitors in rats who have been exposed to common bacterial pathogens and analyzes their downstream effects. In one of her experiments, she injects a leukotriene B4 inhibitor into a rat and observes an abnormal cell response. Which of the following interleukins would most closely restore the function of one of the missing products?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
