Autonomic/CV Drugs — MCQs

On this page
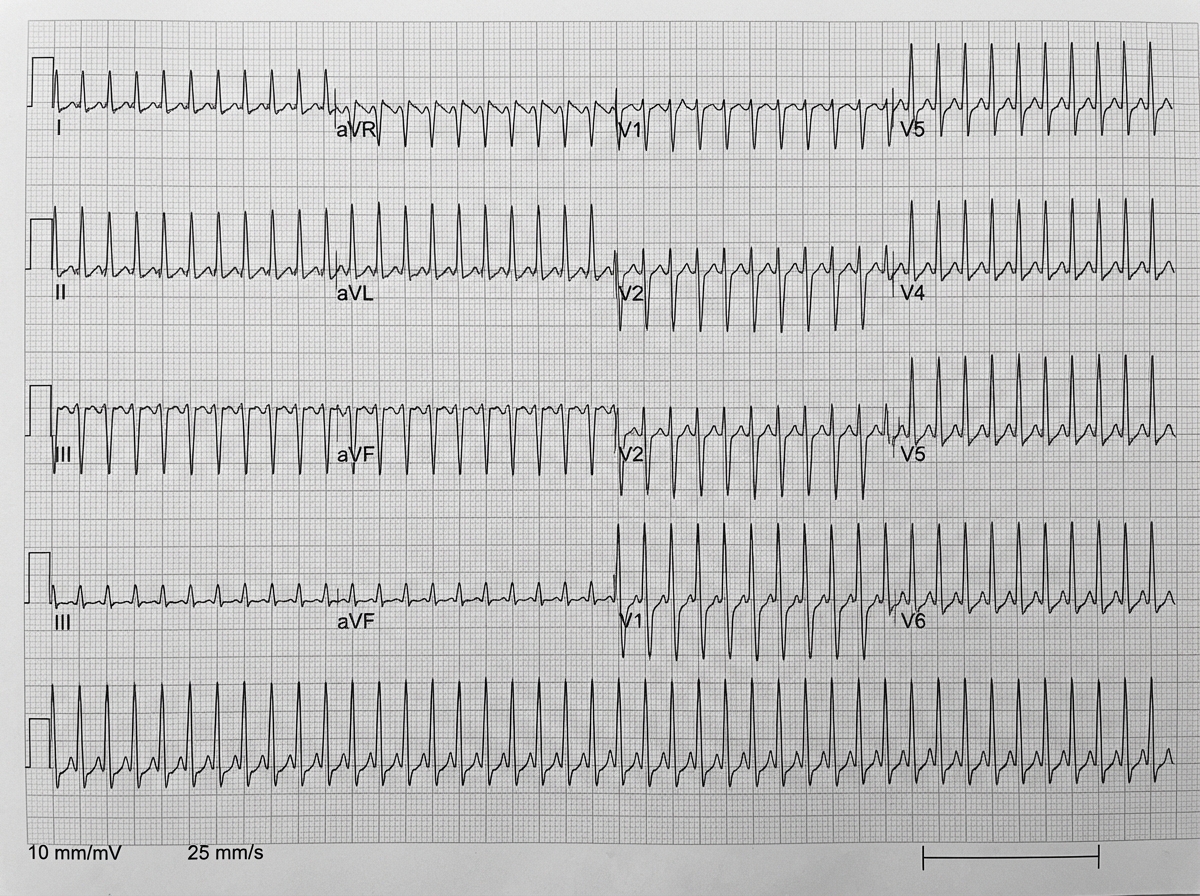
A 26-year-old healthy woman presents with lightheadedness, palpitations, and sweating, which started suddenly after she was frightened by her neighbor’s dog. The patient’s blood pressure is 135/80 mm Hg, the heart rate is 150/min, the respiratory rate is 15/min, and the temperature is 36.6℃ (97.9℉). Her ECG is shown in the exhibit. What is the preferred agent for pharmacologic management of this condition?
A 26-year-old woman comes to the emergency room because she had difficulty breathing during an exercise session. She also has a cough and end-expiratory wheezing. Besides these symptoms, she has a normal physical appearance. She has experienced similar breathing problems during exercise in the past, but never during rest. She is afebrile. What is the best treatment in this case?
Two days after hospitalization for urgent chemotherapy to treat Burkitt’s lymphoma, a 7-year-old boy develops dyspnea and reduced urine output. He also feels a tingling sensation in his fingers and toes. Blood pressure is 100/65 mm Hg, respirations are 28/min, pulse is 100/min, and temperature is 36.2°C (97.2°F). The lungs are clear to auscultation. He has excreted 20 mL of urine in the last 6 hours. Laboratory studies show: Hemoglobin 15 g/dL Leukocyte count 6,000/mm3 with a normal differential serum K+ 6.5 mEq/L Ca+ 7.6 mg/dL Phosphorus 5.4 mg/dL HCO3− 15 mEq/L Uric acid 12 mg/dL Urea nitrogen 44 mg/dL Creatinine 2.4 mg/dL Arterial blood gas analysis on room air: pH 7.30 PCO2 30 mm Hg O2 saturation 95% Which of the following is most likely to have prevented this patient’s condition?
A 21-year-old G1P0 woman presents to the labor and delivery ward at 39 weeks gestation for elective induction of labor. She requests a labor epidural. An epidural catheter is secured at the L4-L5 space. She exhibits no hemodynamic reaction to lidocaine 1.5% with epinephrine 1:200,000. A continuous infusion of bupivacaine 0.0625% is started. After 5 minutes, the nurse informs the anesthesiologist that the patient is hypotensive to 80/50 mmHg with a heart rate increase from 90 bpm to 120 bpm. The patient is asymptomatic and fetal heart rate has not changed significantly from baseline. She says that her legs feel heavy but is still able to move them. What is the most likely cause of the hemodynamic change?
A 25-year-old man presents to the emergency department with a severe pulsatile headache for an hour. He says that he is having palpitations as well. He adds that he has had several episodes of headache in the past which resolved without seeking medical attention. He is a non-smoker and does not drink alcohol. He denies use of any illicit drugs. He looks scared and anxious. His temperature is 37°C (98.6°F), respirations are 25/min, pulse is 107/min, and blood pressure is 221/161 mm Hg. An urgent urinalysis reveals elevated plasma metanephrines. What is the next best step in the management of this patient?
An investigator is comparing the risk of adverse effects among various antiarrhythmic medications. One of the drugs being studied primarily acts by blocking the outward flow of K+ during myocyte repolarization. Further investigation shows that the use of this drug is associated with a lower rate of ventricular tachycardia, ventricular fibrillation, and torsades de pointes when compared to similar drugs. Which of the following drugs is most likely being studied?
A 38-year-old man presents to his primary care provider for abdominal pain. He reports that he has had a dull, burning pain for several months that has progressively gotten worse. He also notes a weight loss of about five pounds over that time frame. The patient endorses nausea and feels that the pain is worse after meals, but he denies any vomiting or diarrhea. He has a past medical history of hypertension, and he reports that he has been under an unusual amount of stress since losing his job as a construction worker. His home medications include enalapril and daily ibuprofen, which he takes for lower back pain he developed at his job. The patient drinks 1-2 beers with dinner and has a 25-pack-year smoking history. His family history is significant for colorectal cancer in his father and leukemia in his grandmother. On physical exam, the patient is moderately tender to palpation in the epigastrium. A fecal occult test is positive for blood in the stool. Which of the following in the patient’s history is most likely causing this condition?
A 26-year-old man being treated for major depressive disorder returns to his psychiatrist complaining that he has grown weary of the sexual side effects. Which other medication used to treat major depressive disorder may be appropriate as a stand-alone or add-on therapy?
A 44-year-old man presents for a checkup. The patient says he has to urinate quite frequently but denies any dysuria or pain on urination. Past medical history is significant for diabetes mellitus type 2 and hypertension, both managed medically, as well as a chronic mild cough for the past several years. Current medications are metformin, aspirin, rosuvastatin, captopril, and furosemide. His vital signs are an irregular pulse of 74/min, a respiratory rate of 14/min, a blood pressure of 130/80 mm Hg, and a temperature of 36.7°C (98.0°F). His BMI is 32 kg/m2. On physical examination, there are visible jugular pulsations present in the neck bilaterally. Laboratory findings are significant for the following: Glycated Hemoglobin (Hb A1c) 7.5% Fasting Blood Glucose 120 mg/dL Serum Electrolytes Sodium 138 mEq/L Potassium 3.9 mEq/L Chloride 101 mEq/L Serum Creatinine 1.3 mg/dL Blood Urea Nitrogen 18 mg/dL Which of the following is the next best step in the management of this patient?
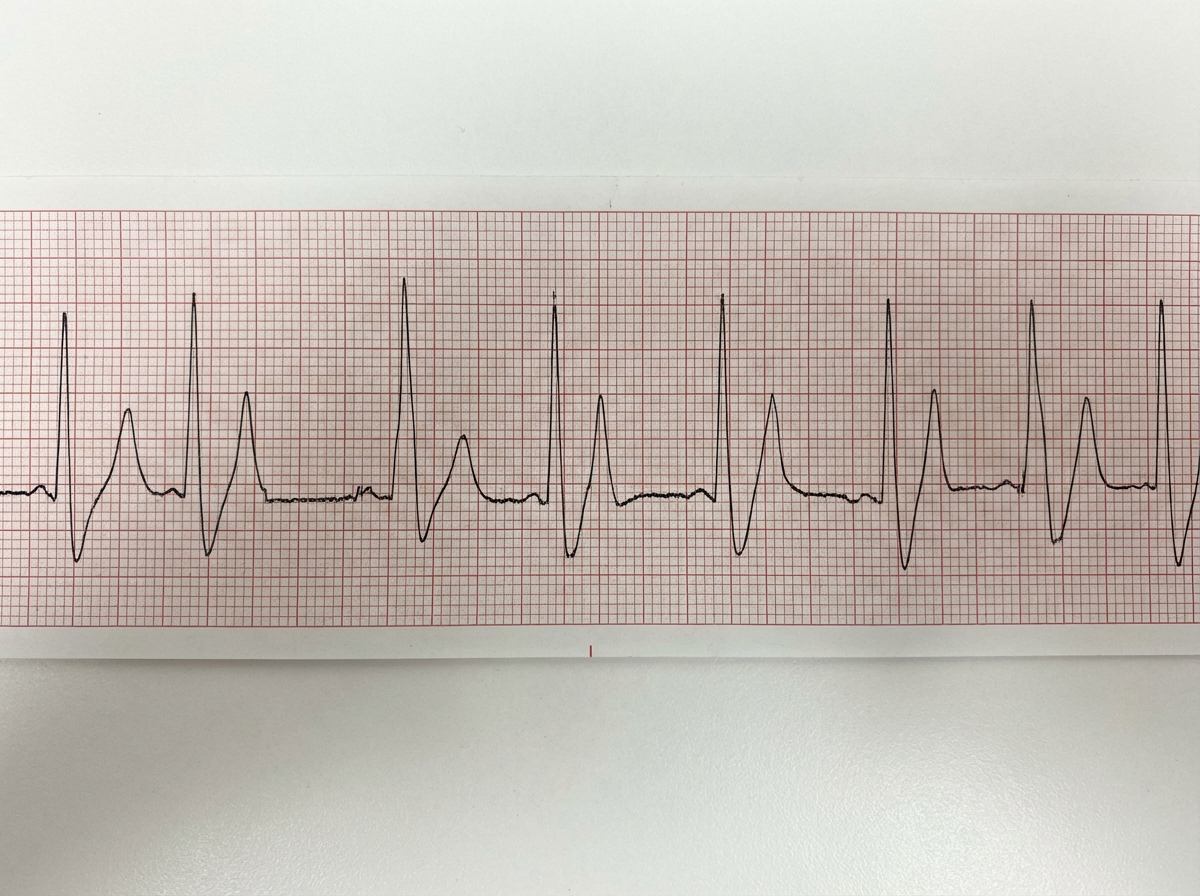
A 25-year-old male is brought into the emergency department by emergency medical services. The patient has a history of bipolar disease complicated by polysubstance use. He was found down in his apartment at the bottom of a staircase lying on his left arm. He was last seen several hours earlier by his roommate. He is disoriented and unable to answer any questions, but is breathing on his own. His vitals are HR 55, T 96.5, RR 18, BP 110/75. You decide to obtain an EKG as shown in Figure 1. What is the next best step in the treatment of this patient?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
