Autonomic/CV Drugs — MCQs

On this page
A 59-year-old man with a history of major depressive disorder, asthma, and erectile dysfunction presents to his family physician complaining of depressed mood, amotivation, overeating, and anhedonia. He currently takes no medications. The patient has a 3 pack-year smoking history and would like to quit but has been unsuccessful in the past. His BMI is 29 kg/m^2. The physician suggests starting an antidepressant for the patient's mood symptoms. The patient is reluctant, as he used to take sertraline, but stopped it after his erectile dysfunction worsened. Which of the following antidepressants would be most appropriate for this patient?
A 32-year-old woman presents for a follow-up visit. She was diagnosed with type 2 diabetes mellitus a month ago but refused to start medications despite counseling due to her fear of gaining weight. She tried exercising and eating healthy in an attempt to ''cure'' her diabetes. She managed to lose 1.8 kg (4 lb) in a month. Today she still complains of increased urinary frequency, the same symptom that leads to her initial suspicion of diabetes. No other significant past medical history. She is happily married and plans on having kids in the next few years. The patient is a non-smoker, denies illicit drug use, and drinks socially. Her vital signs show a pulse of 80/min, a respiratory rate of 16/min, a blood pressure of 120/80 mm Hg, and a temperature of 36.9°C (98.4°F). Her BMI is 33.0 kg/m2. Physical exam findings are unremarkable. Her fingerstick glucose today is 214 mg/dL. Laboratory findings reveal the following: Glycated Hemoglobin (HbA1c) 7.1% Blood glucose (fasting) 130 mg/dL Serum: Sodium 142 mEq/L Potassium 3.9 mEq/L Chloride 101 mEq/L Serum creatinine 0.8 mg/dL Blood urea nitrogen 9 mg/dL Urinalysis shows: Glucose Positive Ketones Negative Leukocytes Negative Nitrites Negative RBCs Negative Casts Negative Which of the following is the best treatment option for this patient?
A 48-year-old woman presents to the emergency room because of severe back pain after a fall. She says that she was walking home from work when she slipped on a patch of ice on the sidewalk. Since she did not have anything to hold onto, she fell backwards and landed on her posterior iliac crests bilaterally. Immediately after the fall, she started experiencing back pain and tenderness that concerned her enough to call for an ambulance. Her past medical history is significant for arthritis, diabetes, and hypertension. On arrival, her temperature is 99°F (37.2°C), blood pressure is 129/86 mmHg, pulse is 112/min, respirations are 19/min. Physical exam reveals tenderness to palpation over the middle of her lower back. A drug that may have predisposed this patient to this outcome most likely has which of the following mechanisms?
A 71-year-old woman presents to the clinic after an X-ray that revealed compression fractures of her L1 and L2 vertebral bodies due to osteoporotic changes. The patient has a history of hypertension for which she takes hydrochlorothiazide, and rheumatoid arthritis, for which she has been taking prednisone for the last 2 years. The patient states that she had a dual-energy X-ray absorptiometry (DEXA) scan 3 years ago that was normal and attributes that finding to regularly taking calcium and vitamin D supplements since then. The patient states that her pain from the fractures is stopping her from participating in her regular activities, such as exercising and gardening. Which of the following is the main cause of her osteoporosis?
You are working in the emergency room of a children's hospital when a 4-year-old girl is brought in by ambulance due to "difficulty breathing." The patient had been eating lunch on a school field trip when she suddenly complained of abdominal pain. Shortly thereafter, she was noted to have swelling of the lips, a rapidly developing red rash and difficulty breathing. In the ambulance her blood pressure was persistently 80/50 mmHg despite intramuscular epinephrine. In the course of stabilization and work up of the patient, you note an elevated tryptase level. What is the mechanism behind this elevated tryptase level?
A research team is studying the effects of a novel drug that was discovered to treat type 2 diabetes. In order to learn more about its effects, they follow patients who are currently taking the drug and determine whether there are adverse effects that exceed anticipated levels and may therefore be drug-related. They discover that the drug causes an excess of sudden cardiac death in 19 patients with renal failure out of 2 million total patients that are followed. Based on these results, an additional warning about this serious adverse effect is added to the investigator brochure for the drug. Which of the following clinical phase studies does this study most likely describe?
A 55-year-old woman comes to the physician because of involuntary hand movements that improve with alcohol consumption. Physical examination shows bilateral hand tremors that worsen when the patient is asked to extend her arms out in front of her. The physician prescribes a medication that is associated with an increased risk of bronchospasms. This drug has which of the following immediate effects on the cardiovascular system? Stroke volume | Heart rate | Peripheral vascular resistance
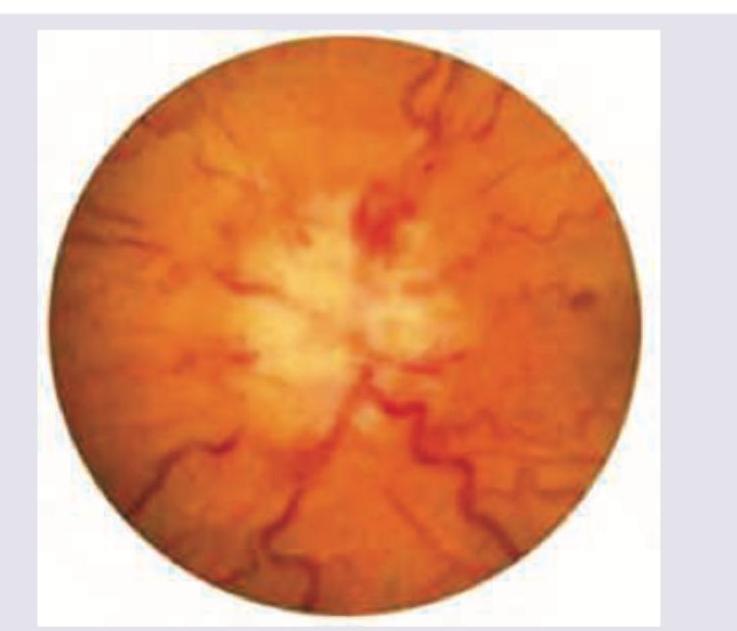
A 30-year-old obese female presents with new-onset headaches, ringing in her ears, and blurry vision. Ibuprofen and avoidance of light has not relieved her symptoms. She denies a history of recent trauma, fever, chills, and fatigue. Past medical history is significant for type 2 diabetes mellitus managed with metformin. She has had 20/20 vision her whole life and wonders if she might need to get eyeglasses. She has 2 healthy school-age children. Her temperature is 36.8°C (98.2°F), heart rate is 90/min, respiratory rate is 15/min, and blood pressure is 135/80 mm Hg. Physical exam is notable for decreased lateral eye movement, and the funduscopic findings are shown in the picture. Laboratory findings are within normal limits and brain imaging is normal. Lumbar puncture demonstrates an elevated opening pressure and normal CSF composition. Which of the following is a side effect of the medication used to treat this condition?
A 66-year-old man with congestive heart failure presents to the emergency department complaining of worsening shortness of breath. These symptoms have worsened over the last 3 days. He has a blood pressure of 126/85 mm Hg and heart rate of 82/min. Physical examination is notable for bibasilar crackles. A chest X-ray reveals bilateral pulmonary edema. His current medications include metoprolol succinate and captopril. You wish to add an additional medication targeted towards his symptoms. Of the following, which statement is correct regarding loop diuretics?
A 26-year-old woman (gravida 3 para 1) with no prenatal care delivers a boy at 37 weeks gestation. His Apgar score is 5 at 1 minute and 8 at 5 minutes. His weight is 2.1 kg (4.2 lb) and length is 47 cm (1 ft 7 in). The mother’s history is significant for chronic pyelonephritis, atrial fibrillation, and gastroesophageal reflux disease. She has a 5-pack-year smoking history and also reports alcohol consumption during pregnancy. Examination of the infant shows a short depressed nasal bridge, wide nose, brachydactyly, and a short neck. Ophthalmoscopy reveals bilateral cataracts. What is the most likely cause of the newborn’s symptoms?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
