Autonomic/CV Drugs — MCQs

On this page
A 19-year-old woman comes to the physician because of a delayed menstrual period. She has had regular menses since menarche at age 11. Her last menstrual period was 7 weeks ago. She is sexually active with two male partners. A urine pregnancy test is positive. An ultrasound of the pelvis shows a viable intrauterine pregnancy with an estimated gestational age of 6 weeks and 5 days. She does not wish to continue with the pregnancy. After carefully weighing the options with her physician, she is prescribed two medications, one of which is mifepristone. Which of the following is this drug's primary mechanism of action?
A 28-year-old woman visits the clinic expressing a desire to become pregnant. She was seen for depressed mood and disinterest in her usual leisure activities a few months ago. She also had decreased sleep and appetite and was not able to concentrate at work. She was started on fluoxetine and has been compliant for the last 6 months despite experiencing some of the side effects. She now feels significantly better and would like to stop the medication because she plans to become pregnant and thinks it is unnecessary now. Which of the following is the most appropriate counseling regarding her antidepressant therapy?
A 52-year-old woman makes a follow-up appointment with her primary care physician for evaluation of her diabetes medications. Specifically, she complains that she has been experiencing flushing, nausea, and palpitations after drinking a glass of wine with dinner after she started the latest regimen for her diabetes. She was warned that this was a side-effect of one of her medications but she did not understand the severity of the reaction. Given this experience, she asks to be placed on an alternative regimen that does not involve the medication that caused this reaction. Her physician therefore replaces the medication with another one that interacts with the same target though at a different binding site. Which of the following is a side-effect of the new medication?
Eight days after sigmoid resection for acute diverticulitis, a 61-year-old man has left-sided flank pain. He has been on bowel rest since admission. Other than multiple admissions for alcohol withdrawal, he has no history of serious illness. Current medications include intravenous cefepime and morphine. His temperature is 36.9°C (98.4°F), pulse is 89/min, and blood pressure is 118/75 mm Hg. Abdominal exam shows a well-healing incision with minimal serous drainage. Examination of the skin shows scattered spider angiomas, a large hematoma on the left flank, and numerous bruises over the abdomen and extremities. He complains of pain when his left hip is extended. Laboratory studies show: Hemoglobin 8.4 g/dL Mean corpuscular volume 102 μm3 Leukocyte count 8,200/mm3 Platelet count 170,000/mm3 Serum Bleeding time 4 minutes Prothrombin time 26 seconds Partial thromboplastin time (activated) 39 seconds Which of the following is the most likely underlying cause of this patient's current symptoms?
A 72-year-old patient is referred to an ophthalmologist because he has noticed some mild discomfort in his eyes though his vision remains unchanged. He cannot recall when this feeling started. His past medical history is significant for diabetes mellitus and two myocardial infarctions that have led to significant cardiac dysfunction. Specifically, he has dyspnea and peripheral edema and occasionally decompensates into more severe pulmonary edema requiring hospitalization. Testing reveals increased intra-ocular pressure so the ophthalmologist prescribes several medications. The medication for this disorder that is most likely to be contraindicated in this patient has which of the following characteristics?
A 25-year-old Caucasian female presents with symptoms of Graves' disease. Her doctor prescribes medications and sends the patient home. After two months of therapy, the patient returns upset that her exophthalmos has not gone away. Which of the following drugs should the physician have prescribed to treat the exophthalmos?
A 23-year-old college student presents with his parents for a follow-up appointment. He was recently diagnosed with schizophrenia and was started on risperidone approx. 2 months ago. He reports a significant improvement since the start of treatment. His parents report that their son’s symptoms of delusions, hallucinations, and paranoid behavior have been ameliorated. On physical examination, the patient seems uncomfortable. He frequently fidgets and repeatedly crosses and uncrosses his legs. When asked if something is troubling him, he gets up and starts pacing. He says, “It’s always like this. I cannot sit still. It is frustrating.” What is the most likely diagnosis?
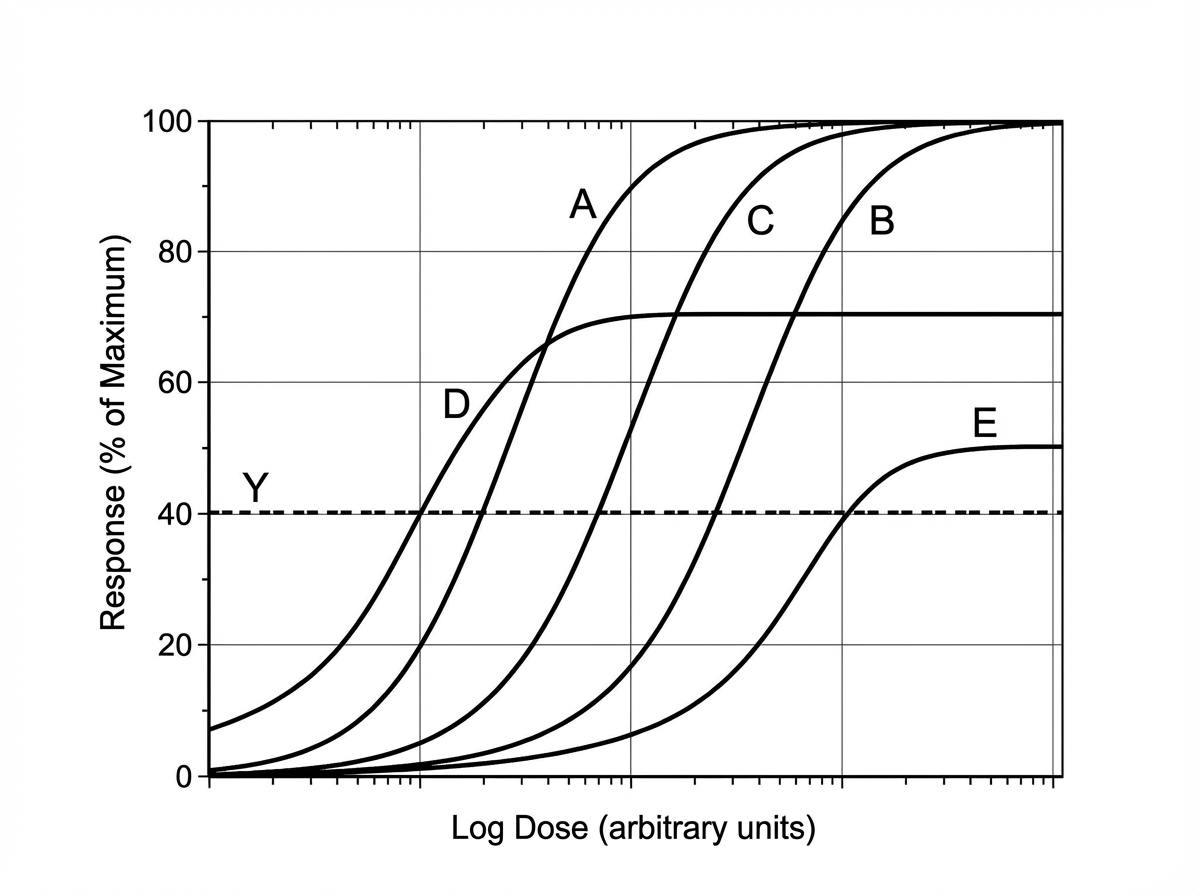
Scientists are developing a new non-steroidal anti-inflammatory drug for osteoarthritis. Their hope is that the new drug will have a higher potency but the same efficacy as ibuprofen in the hope of minimizing gastrointestinal side effects. If ibuprofen is curve C in the figure provided, which of the following would be the curve for the new drug based on the scientists’ specifications? The desired therapeutic effect in patients is represented by the dashed line Y.
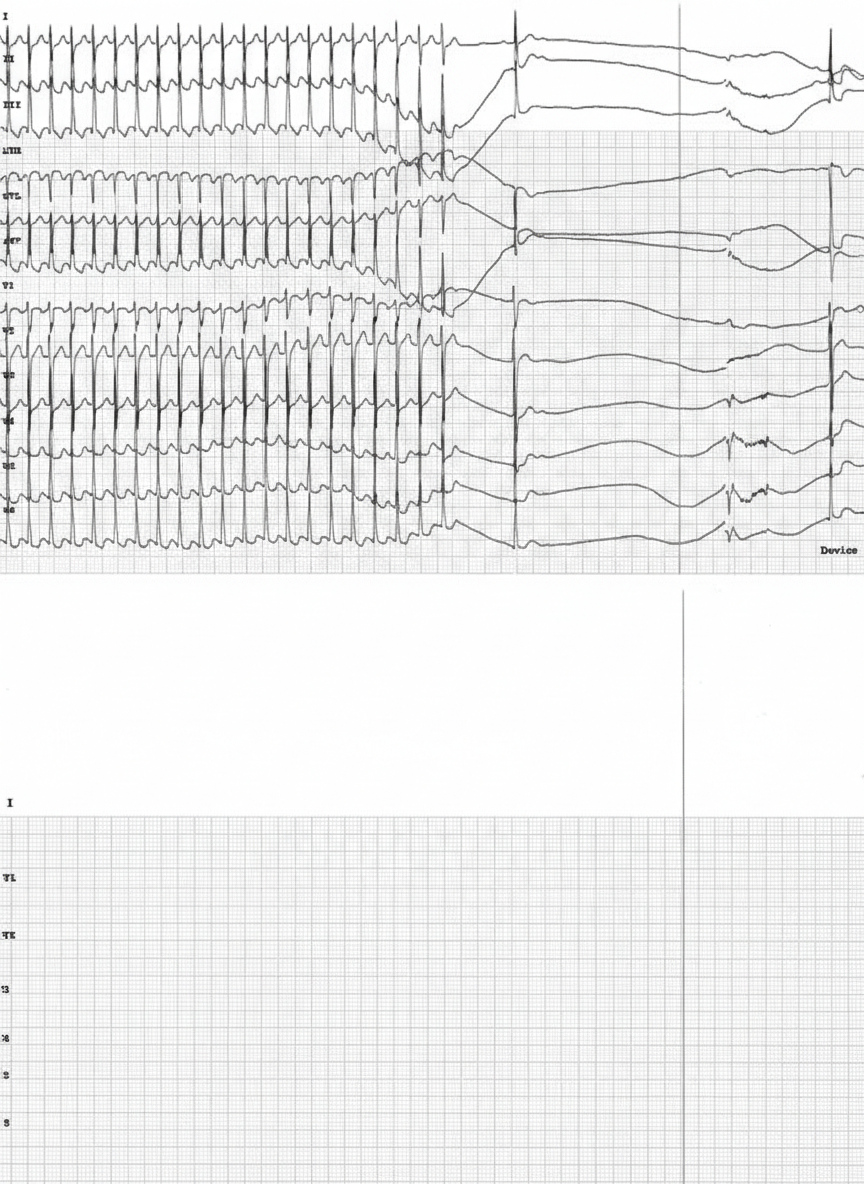
A 46-year-old female is brought to the emergency department by her husband 1 hour after the onset of chest palpitations. Her symptoms began suddenly while she was drinking coffee and have persisted since then. She has not had shortness of breath, chest pain, dizziness, or loss of consciousness. She has experienced these palpitations before, but they typically resolve spontaneously within a few minutes. She has no history of serious illness and takes no medications. Her temperature is 36.8°C (98.2°F), pulse is 155/min, respirations are 18/min, and blood pressure is 130/82 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 97%. Physical examination shows no abnormalities other than tachycardia. An ECG is shown. Repeated, forceful exhalation against a closed glottis while supine fails to relieve her symptoms. Which of the following is the most appropriate next step in management?
A 5-year-old boy is brought to the emergency department by his parents with complaints of severe muscle cramping and abdominal pain. They live in Virginia. The parents state that about 2 hours before, the child was playing in their outdoor shed when he suddenly ran inside crying, saying he was bitten by a bug. One hour following the bite, the child developed the symptoms of cramping and pain. He has no known medical history and takes no medications. His blood pressure is 132/86 mm Hg, the heart rate is 116/min, and the respiratory rate is 20/min. Vital signs reveal tachycardia and hypertension. On exam, there is a 1 cm area of erythema to the dorsum of his right hand without any further dermatologic findings. Palpation of his abdomen reveals firm rigidity but no discernable rebound tenderness. What arthropod is most likely responsible for his symptoms?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
