Autonomic/CV Drugs — MCQs

On this page
A 5-year-old boy is brought to the physician by his parents for the evaluation of an episode of loss of consciousness while he was playing soccer earlier that morning. He was unconscious for about 15 seconds and did not shake, bite his tongue, or lose bowel or bladder control. He has been healthy except for 1 episode of simple febrile seizure. His father died suddenly at the age of 34 of an unknown heart condition. The patient does not take any medications. He is alert and oriented. His temperature is 37°C (98.6°F), pulse is 95/min and regular, and blood pressure is 90/60 mm Hg. Physical examination shows no abnormalities. Laboratory studies are within normal limits. An ECG shows sinus rhythm and a QT interval corrected for heart rate (QTc) of 470 milliseconds. Which of the following is the most appropriate next step in treatment?
A 61-year-old woman presents to her physician with foot tingling, numbness, and pain. She describes her pain as constant and burning and gives it 5 out of 10 on the visual analog pain scale. She also recalls several falls due to the numbness in her feet. She was diagnosed with diabetes mellitus and diabetic retinopathy 5 years ago. Since then, she takes metformin 1000 mg twice daily and had no follow-up visits to adjust her therapy. Her weight is 110 kg (242.5 lb), and her height is 176 cm (5 ft. 7 in). The vital signs are as follows: blood pressure is 150/90 mm Hg, heart rate is 72/min, respiratory rate is 12/min, and the temperature is 36.6°C (97.9°F). The patient has increased adiposity in the abdominal region with stretch marks. The respiratory examination is within normal limits. The cardiovascular exam is significant for a bilateral carotid bruit. The neurological examination shows bilateral decreased ankle reflex, symmetrically decreased touch sensation and absent vibration sensation in both feet up to the ankle. The gait is mildly ataxic. The Romberg test is positive with a tendency to fall to both sides, and significant worsening on eye closure. Which of the following medications should be used to manage the patient’s pain?
A 59-year-old female presents to the emergency department after a fall. She reports severe pain in her right hip and an inability to move her right leg. Her past medical history is notable for osteoporosis, rheumatoid arthritis, and has never undergone surgery before. The patient was adopted, and her family history is unknown. She has never smoked and drinks alcohol socially. Her temperature is 98.8°F (37.1°C), blood pressure is 150/90 mmHg, pulse is 110/min, and respirations are 22/min. Her right leg is shortened, abducted, and externally rotated. A radiograph demonstrates a displaced femoral neck fracture. She is admitted and eventually brought to the operating room to undergo right hip arthroplasty. While undergoing induction anesthesia with inhaled sevoflurane, she develops severe muscle contractions. Her temperature is 103.4°F (39.7°C). A medication with which of the following mechanisms of action is indicated in the acute management of this patient’s condition?
A previously healthy 52-year-old woman comes to the physician because of a 3-month history of chest pain on exertion. She takes no medications. Cardiopulmonary examination shows no abnormalities. Cardiac stress ECG shows inducible ST-segment depressions in the precordial leads that coincide with the patient's report of chest pain and resolve upon cessation of exercise. Pharmacotherapy with verapamil is initiated. This drug is most likely to have which of the following sets of effects? $$$ End-diastolic volume (EDV) %%% Blood pressure (BP) %%% Contractility %%% Heart rate (HR) $$$
A 35-year-old woman is brought to the emergency department 30 minutes after the onset of severe dyspnea. On arrival, she is unresponsive. Her pulse is 160/min, respirations are 32/min, and blood pressure is 60/30 mm Hg. CT angiography of the chest shows extensive pulmonary embolism in both lungs. She is given a drug that inhibits both thrombin and factor Xa. Which of the following medications was most likely administered?
A drug discovery team is conducting research to observe the characteristics of a novel drug under different experimental conditions. The drug is converted into the inactive metabolites by an action of an enzyme E. After multiple experiments, the team concludes that as compared to physiologic pH, the affinity of the enzyme E for the drug decreases markedly in acidic pH. Co-administration of an antioxidant A increases the value of Michaelis-Menten constant (Km) for the enzyme reaction, while co-administration of a drug B decreases the value of Km. Assume the metabolism of the novel drug follows Michaelis-Menten kinetics at the therapeutic dose, and that the effects of different factors on the metabolism of the drug are first-order linear. For which of the following conditions will the metabolism of the drug be the slowest?
A 75-year-old man with a 35-pack-year history of smoking is found to be lethargic three days after being admitted with a femur fracture following a motor vehicle accident. His recovery has been progressing well thus far, though pain continued to be present. On exam, the patient is minimally responsive with pinpoint pupils. Vital signs are blood pressure of 115/65 mmHg, HR 80/min, respiratory rate 6/min, and oxygen saturation of 87% on room air. Arterial blood gas (ABG) shows a pH of 7.24 (Normal: 7.35-7.45), PaCO2 of 60mm Hg (normal 35-45mm Hg), a HCO3 of 23 mEq/L (normal 21-28 mEq/L) and a Pa02 of 60 mmHg (normal 80-100 mmHg). Which of the following is the most appropriate therapy at this time?
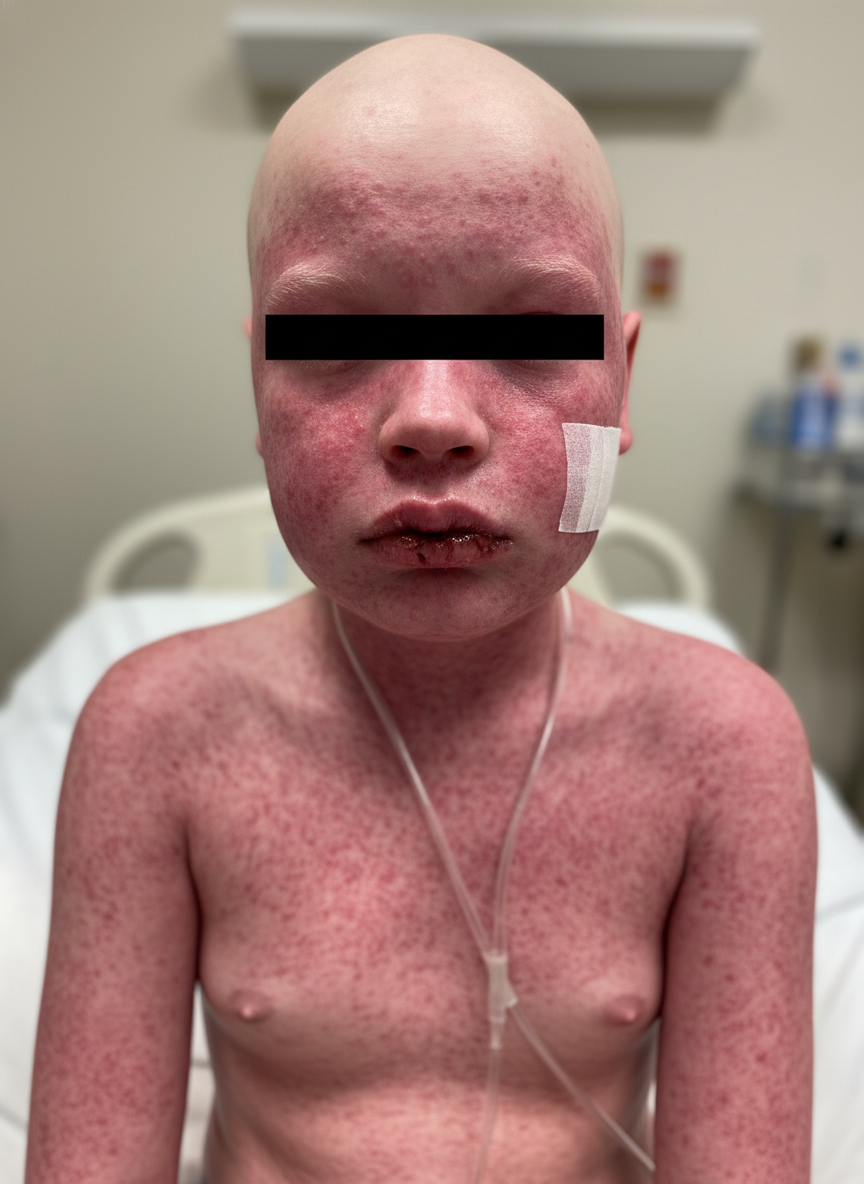
A 10-year-old boy presents with a painful rash for 1 day. He says that the reddish, purple rash started on his forearm but has now spread to his abdomen. He says there is a burning pain in the area where the rash is located. He also says he has had a stuffy nose for several days. Past medical history is significant for asthma and epilepsy, medically managed. Current medications are a daily chewable multivitamin, albuterol, budesonide, and lamotrigine. On physical examination, there is a red-purple maculopapular rash present on upper extremities and torso. There are some blisters present over the rash, as shown in the image, which is also present in the oral mucosa. Which of the following is the most likely cause of this patient’s symptoms?
A 64-year-old man is brought to the emergency department because of dull lower abdominal pain for 3 hours. He has not urinated for 24 hours and has not passed stool for over 3 days. He was diagnosed with herpes zoster 4 weeks ago and continues to have pain even after his rash resolved. He has hypertension, benign prostatic hyperplasia, and coronary artery disease. Physical examination shows a tender, palpable suprapubic mass. Bowel sounds are hypoactive. Abdominal ultrasound shows a large anechoic mass in the pelvis. Which of the following drugs most likely accounts for this patient's current symptoms?
A 16-year-old girl who recently immigrated to the United States from Bolivia presents to her primary care physician with a chief complaint of inattentiveness in school. The patient's teacher describes her as occasionally "day-dreaming" for periods of time during which the patient does not respond or participate in school activities. Nothing has helped the patient change her behavior, including parent-teacher conferences or punishment. The patient has no other complaints herself. The only other concern that the patient's mother has is that upon awakening she notices that sometimes the patient's arm will jerk back and forth. The patient states she is not doing this intentionally. The patient has an unknown past medical history and is currently not on any medications. On physical exam you note a young, healthy girl whose neurological exam is within normal limits. Which of the following is the best initial treatment?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
