Autonomic/CV Drugs — MCQs

On this page
A 27-year-old woman presents for a checkup. She is 20 weeks pregnant and has been admitted to the hospital multiple times during her pregnancy for seizures. She has a known seizure disorder but discontinued her valproic acid when she became pregnant. The patient's past medical history is otherwise unremarkable. She does not smoke, drink alcohol, or use any drugs. She generally prefers not to take medications and sees a shaman for her care typically. Given her recent hospitalization, the patient agrees to start carbamazepine. Which of the following is the most appropriate treatment for this patient at this time?
A 34-year-old woman comes to the emergency department complaining of severe headache and anxiety, diaphoresis, and palpitations for the last 30 minutes. She has had several similar episodes over the past few weeks. She has no significant past medical history and has a 10 pack-year smoking history. She takes no illicit drugs. Her blood pressure on arrival is 181/80 mmHg and her pulse is 134/min. If this patient was given metoprolol, how would her blood pressure respond?
A 43-year-old woman comes to the physician with a 2-week history of new pruritic plaques on the scalp and extensor surfaces of the elbows and knees. Ten years ago, she was diagnosed with psoriasis. Her only medication is topical calcipotriene. Physical examination shows well-demarcated, symmetrical, erythematous plaques with silvery scale. There is pitting of the nails on all fingers. Therapy with a high-potency topical medication that inhibits NF-κB and phospholipase A2 is begun. Long-term use of this agent is most likely to result in which of the following?
A 52-year-old woman status-post liver transplant presents to her transplant surgeon because she has noticed increased urination over the last 3 weeks. Six months ago she received a liver transplant because of fulminant liver failure after viral hepatitis. Since then, she has noticed that she has been drinking more water and urinating more. Her husband has also noticed that she has been eating a lot more. She says that she never had these symptoms prior to her transplant and has been taking her medications on time. After confirmatory tests, she is started on a medication that binds to an ATP-gated potassium channel. The drug that increases the risk of the complication experienced by this patient most likely has which of the following mechanisms of action?
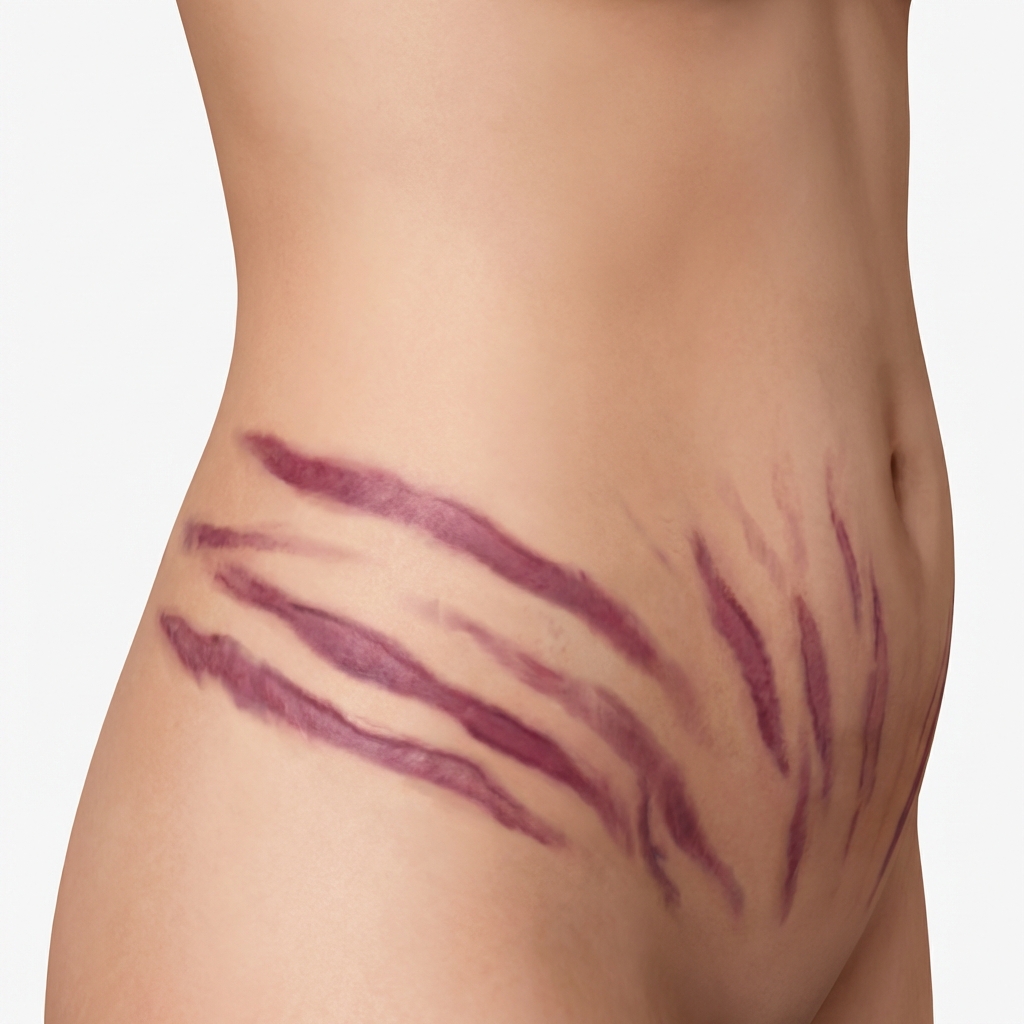
A 33-year-old woman presents with weight gain and marks on her abdomen (as seen in the image below). She does not have any significant past medical history. She is a nonsmoker and denies any alcohol use. Her blood pressure is 160/110 mm Hg and pulse is 77/min. A T1/T2 MRI of the head shows evidence of a pituitary adenoma, and she undergoes surgical resection of the tumor. Which of the following therapies is indicated in this patient to ensure normal functioning of her hypothalamic-pituitary-adrenal (HPA) axis?
A 4-year-old boy presents to the Emergency Department with wheezing and shortness of breath after playing with the new family pet. Which of the following immunological factors is most involved in generating the antibodies necessary for mast cell Fc-receptor cross-linking and degranulation?
A 62-year-old woman is brought to the emergency room at a nearby hospital after being involved in a roadside accident in which she sustained severe chest trauma. Enroute to the hospital, morphine is administered for pain control. Upon arrival, the patient rapidly develops respiratory failure and requires intubation and mechanical ventilation. She is administered pancuronium in preparation for intubation but suddenly develops severe bronchospasm and wheezing. Her blood pressure also quickly falls from 120/80 mm Hg to 100/60 mm Hg. Which of the following best explains the most likely etiology of this complication?
A 45-year-old man is brought into the emergency department after he was hit by a car. The patient was intoxicated and walked into oncoming traffic. He is currently unconscious and has a Glasgow coma scale score of 3. The patient has been admitted multiple times for alcohol intoxication and pancreatitis. The patient is resuscitated with fluid and blood products. An initial trauma survey reveals minor scrapes and abrasions and pelvic instability. The patient’s pelvis is placed in a binder. After further resuscitation the patient becomes responsive and states he is in pain. He is given medications and further resuscitation ensues. One hour later, the patient complains of numbness surrounding his mouth and in his extremities. Which of the following is the most likely explanation of this patient’s current symptoms?
A 37-year-old woman is brought to the emergency department by police after being found naked outside a government building. She is accompanied by her husband who reports that she has been having "crazy" ideas. The patient's speech is pressured and she switches topics quickly from how she is going to be president one day to how she is going to learn 20 languages fluently by the end of the year. Upon further questioning, it is revealed that she has struggled with at least 2 depressive episodes in the past year. Her medical history is significant for hypertension, hyperlipidemia, gout, and chronic migraines. She was recently diagnosed with a urinary tract infection and given nitrofurantoin. She has also been taking indomethacin for an acute gout flare. Her other medications include atorvastatin, allopurinol, metoprolol, and acetazolamide. She is prescribed lithium and instructed to follow-up with a primary care physician. At a follow-up appointment, she complains of nausea, vomiting, and increased urinary frequency. On examination, she has a coarse tremor and diffuse hyperreflexia. Which of the following medications is most likely responsible for the patient's current presentation?
A 9-year-old boy is brought to the emergency department by his mother because of painful swelling in his right knee that started after he collided with another player during a soccer game. He has no history of serious illness except for an episode of prolonged bleeding following a tooth extraction a few months ago. Physical examination shows marked tenderness and swelling of the right knee joint. There are multiple bruises on the lower extremities in various stages of healing. Laboratory studies show a platelet count of 235,000/mm3, partial thromboplastin time of 78 seconds, prothrombin time of 14 seconds, and bleeding time of 4 minutes. The plasma concentration of which of the following is most likely to be decreased in this patient?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
