Autonomic/CV Drugs — MCQs

On this page
An 8-year-old female is given omalizumab for the treatment of bronchial asthma. Omalizumab treats asthma through which mechanism?
A 49-year-old man seeks evaluation at an urgent care clinic with a complaint of palpitations for the past few hours. He denies any chest pain, shortness of breath, or sweating. He is anxious and appears worried. His medical history is unremarkable with the exception of mild bronchial asthma. He only uses medications during an asthma attack and has not used medications since last week. He is a former smoker and drinks a couple of beers on weekends. His heart rate is 146/min, respiratory rate is 16/min, temperature is 37.6°C (99.68°F), and blood pressure is 120/80 mm Hg. The physical examination is unremarkable, and an electrocardiogram is ordered. Which of the following groups of drugs should be given to treat his symptoms?
A 62-year-old man is brought to the emergency room because of pain in his right hip. He was found lying on the floor several hours after falling onto his right side. Ten years ago, he received a renal transplant from a living related donor. He has a 4-year history of type 2 diabetes. Current medications include prednisone, cyclosporine, and metformin. Examination shows a shortened and externally rotated right leg. There is extensive bruising over the right buttock and thigh. X-ray of the right hip shows a displaced femoral neck fracture. The patient is resuscitated in the emergency room and taken to surgery for a right total hip replacement. Post-operative laboratory studies show: Hemoglobin 11.2 g/dL Serum Na+ 148 mmol/L K+ 7.1 mmol/L Cl- 119 mmol/L HCO3- 18 mmol/L Urea nitrogen 22 mg/dL Creatinine 1.6 mg/dL Glucose 200 mg/dL Creatine kinase 1,562 U/L His urine appears brown. Urine dipstick is strongly positive for blood. ECG shows peaked T waves. Intravenous calcium gluconate is administered. What is the most appropriate next step in management?
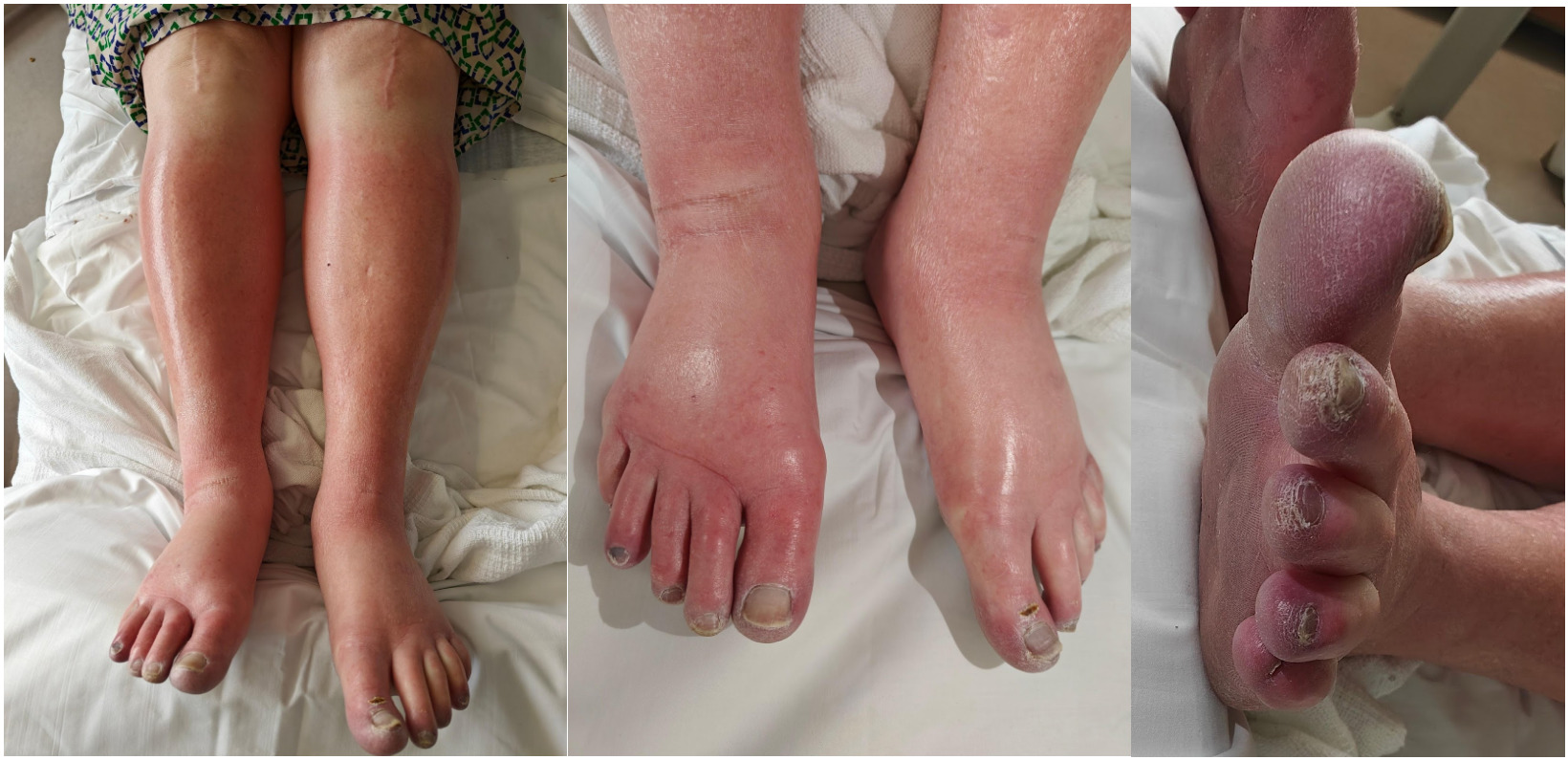
A 65-year-old woman, with end-stage renal disease (ESRD) on hemodialysis, presents with pain, swelling and discoloration of her right leg and foot. She says that she started twice-weekly hemodialysis 2 weeks ago and has had no issues until 1 week ago when she noticed a warm, painful swelling of the back of her right leg and right foot after finishing her dialysis session. Over the week, she says these symptoms have steadily worsened and, in the last few days, her right foot has become discolored. Past medical history is significant for ESRD secondary to long-standing hypertension. Current medications are verapamil 200 mg orally daily and unfractionated heparin that is given during hemodialysis. Her vital signs include: temperature 37.0°C (98.6°F), blood pressure 145/75 mm Hg, pulse 88/min, respirations 15/min, and oxygen saturation 99% on room air. On physical examination, the patient is alert and cooperative. The cardiac exam is normal. Lungs are clear to auscultation. The abdomen is soft and nontender with no hepatosplenomegaly. The right calf is swollen, warm, and erythematous. Physical findings of the patient’s right foot are shown in the exhibit. Laboratory findings are significant for the following: Sodium 141 mEq/L Potassium 4.9 mEq/L Chloride 104 mEq/L Bicarbonate 25 mEq/L BUN 32 mg/dL Creatinine 3.1 mg/dL Glucose (fasting) 75 mg/dL Bilirubin, conjugated 0.5 mg/dL Bilirubin, total 1.0 mg/dL AST (SGOT) 22 U/L ALT (SGPT) 23 U/L Alkaline phosphatase 56 U/L Bleeding time 19 min Prothrombin time (PT) 11 s Partial thromboplastin time (PTT) 30 s WBC 8,500/mm3 RBC 4.10 x 106/mm3 Hematocrit 41.5% Hemoglobin 13.5 g/dL Platelet count 100,000/mm3 (previously 200,000/mm3) Which of the following is the next best diagnostic step in this patient?
A 58-year-old Caucasian male who is being treated for atrial fibrillation and angina complains of dyspnea on exertion. On exam, his heart rate 104-115/min and irregularly irregular at rest. He has no chest pain. You believe his rate control for atrial fibrillation is suboptimal and the likely cause of his dyspnea. You are considering adding verapamil to his current metoprolol for additional rate control of his atrial fibrillation. Which of the following side effects should you be most concerned about with this additional medication?
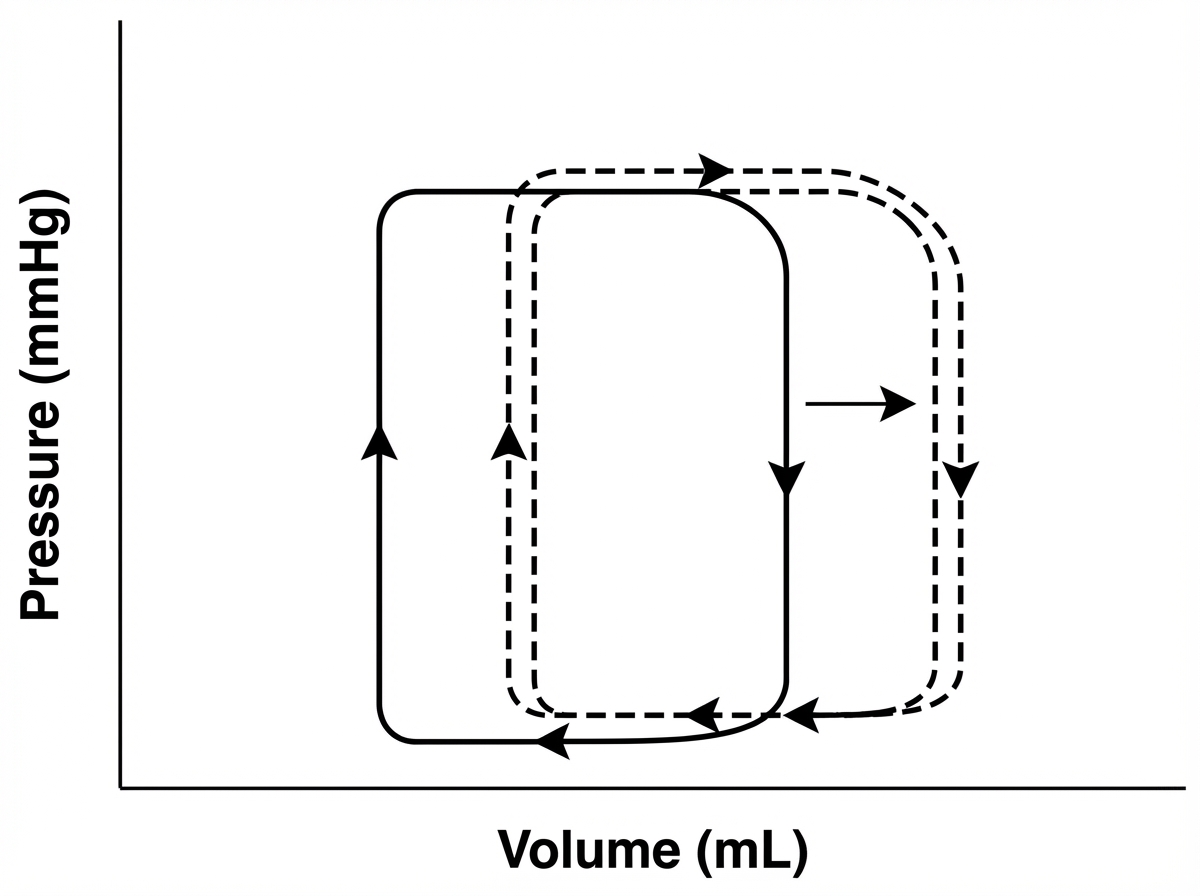
A pharmaceutical company is testing a new antidepressant. During phase I of the drug trial, healthy volunteers are recruited, and the effects of the drug on the cardiovascular system are studied. A graphical representation of the volume-pressure relationship of the left ventricle of the heart is given below with the dashed line representing post medication changes. Which of the following is the most likely mechanism of the drug being studied?
A 67-year-old man presents to his primary care physician for a decline in his hearing that he noticed over the past week. The patient has a past medical history of hypertension and diabetes mellitus and was recently diagnosed with bladder cancer which is currently appropriately being treated. The patient is a hunter and often goes shooting in his spare time. His recent sick contacts include his grandson who is being treated with amoxicillin for ear pain. Physical exam is notable for decreased hearing bilaterally. The Weber test does not localize to either ear, and the Rinne test demonstrates air conduction is louder than bone conduction. Which of the following is the most likely etiology for this patient's hearing loss?
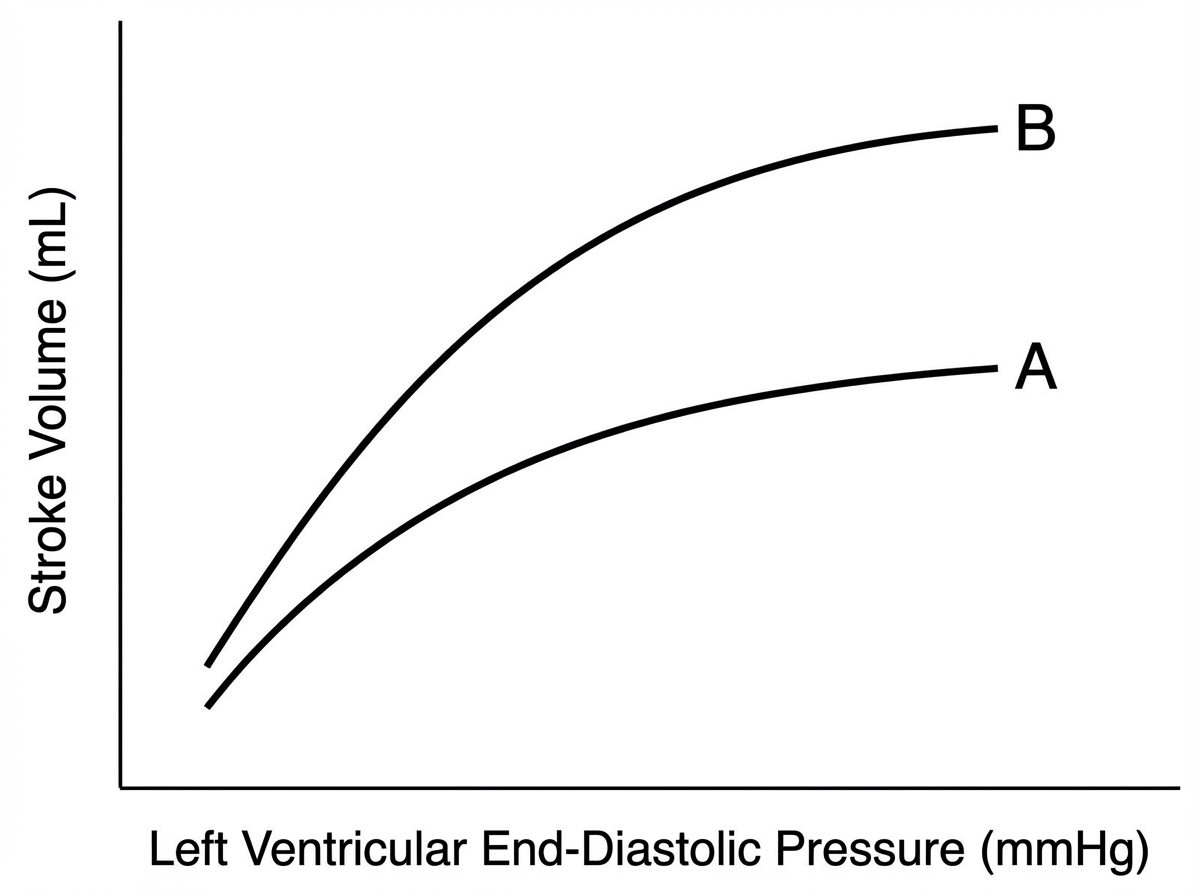
A 78-year-old male comes to the physician’s office for a routine check-up. He complains of increased lower extremity swelling, inability to climb the one flight of stairs in his home, and waking up in the middle of the night 2-3 times gasping for breath. He has had to increase the number of pillows on which he sleeps at night. These symptoms started 9 months ago and have been progressing. The doctor starts him on a medication regimen, one of which changes his Starling curve from A to B as shown in the Figure. Which of the following medications is most consistent with this mechanism of action?
Benzodiazepines are clinically useful because of their inhibitory effects on the central nervous system. Which of the following correctly pairs the site of action of benzodiazepines with the molecular mechanism by which they exert their effects?
A 45-year-old man with type 2 diabetes mellitus presents to his family physician for a follow-up appointment. He is currently using a 3-drug regimen consisting of metformin, sitagliptin, and glipizide. Despite this therapeutic regimen, his most recent hemoglobin A1c level is 8.1%. Which of the following is the next best step for this patient?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
