Autonomic/CV Drugs — MCQs

On this page
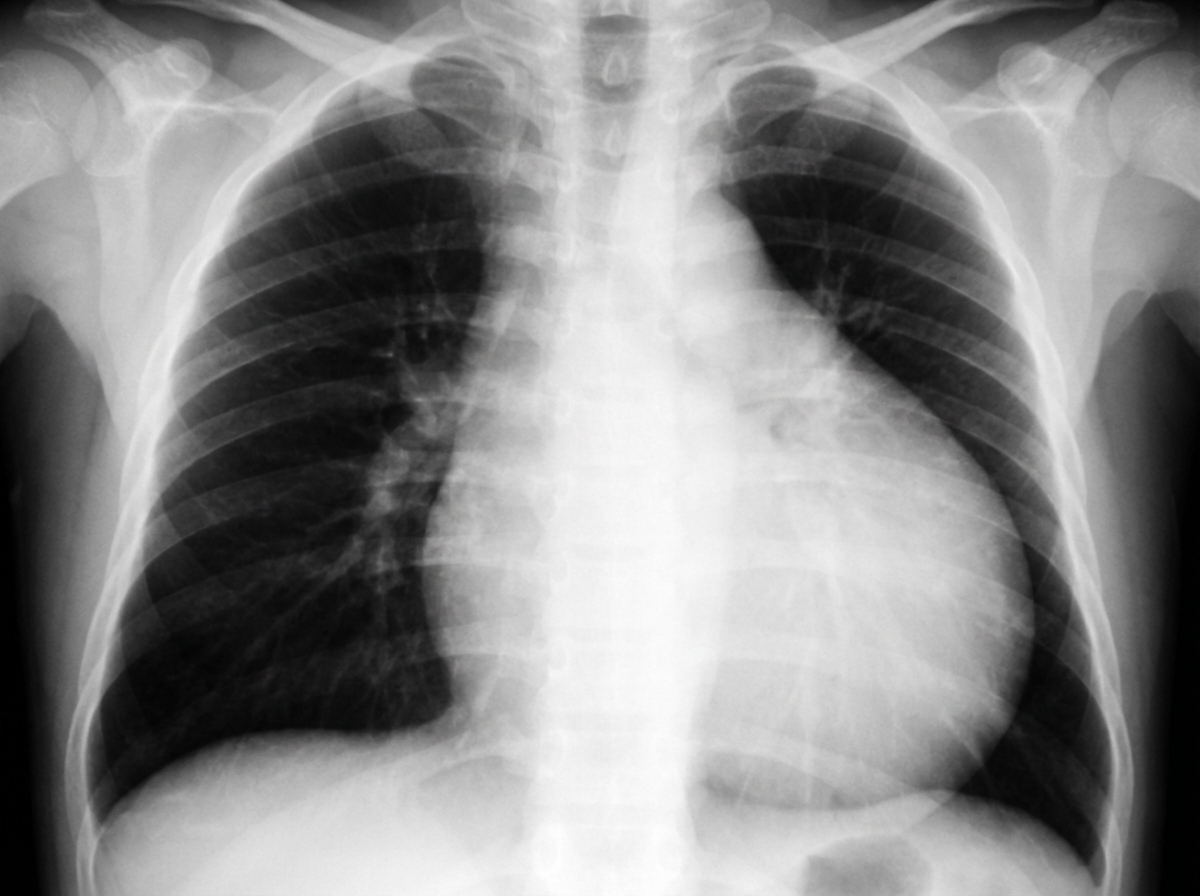
A 27-year-old woman, primigravida, gave birth to a boy 3 months ago and now presents the newborn to your clinic for evaluation. She did not receive prenatal care. She reports that she was taking a medication for her mood swings, but cannot remember the medication’s name. The baby was born cyanotic, with a congenital malformation of the heart that is characterized by apical displacement of the septa and posterior tricuspid valve leaflets. A chest radiograph is shown in the image. Which of the following medications was the mother most likely taking?
Two 19-year-old men are referred by their professor and mentor to a psychiatrist for substance abuse management. The two friends have both used different stimulants for 3 years—Drug A and Drug B, respectively. Both use these substances cyclically. Use of Drug A usually lasts for about 12 hours. The cycle for Drug B lasts several days. A month ago, both men visited the emergency room (ER) due to acute intoxication. Clinical features in the emergency department included hypotension, bradycardia, sweating, chills, mydriasis, nausea, and psychomotor agitation. After a urine drug screen, the psychiatrist identifies both the drugs and informs the professor that although both Drug A and Drug B are stimulants, their mechanisms of action are different. Drug A is an alkaloid that is naturally present in the leaves of the coca plant, while it is possible to make Drug B from over-the-counter nasal decongestant products. Which of the following options best describes the mechanism of action of both drugs?
A 51-year-old man presents to his primary care provider for recurrent epigastric pain. He reports a 3-month history of gnawing epigastric and chest pain that is worse after meals and after lying down. His past medical history is notable for obesity, hypertension, and hyperlipidemia. He takes lisinopril and rosuvastatin. He has a 30 pack-year smoking history and drinks 4-5 beers per day. On exam, he is well-appearing and in no acute distress. He has no epigastric tenderness. He is prescribed an appropriate medication for his symptoms and is told to follow up in 2 weeks. He returns 2 weeks later with improvement in his symptoms, and a decision is made to continue the medication. However, he returns to clinic 3 months later complaining of decreased libido and enlarged breast tissue. Which of the following medications was this patient most likely taking?
A 24-year-old female medical student presents to the emergency department after she develops sudden difficulty breathing and vague chest pain while preparing for exams. The chest pain is non-pleuritic without radiation. She denies any recent travel. She denies any hemoptysis, nausea, vomiting, or leg pain. She only takes oral contraceptives; she denies smoking or alcohol use. Her vitals reveal a heart rate of 120 beats per minute, blood pressure of 100/80 mm Hg, and respiratory rate of 30 per minute. She is afebrile. Otherwise, her physical exam is unremarkable. A CT scan of her chest with IV contrast reveals filling defects along her left pulmonary artery. Which of the following is the most likely mechanism of this finding?
A 59-year-old man comes to the emergency department because of progressively worsening chest pain and nausea that started while visiting a local bar 30 minutes ago. The pain radiates to the epigastric area. He has a 10-year history of untreated hypertension. He has smoked 1 pack of cigarettes daily for 35 years. The patient is diaphoretic and in marked distress. His pulse is 94/min, respirations are 28/min, and blood pressure is 161/92 mm Hg. Pulse oximetry on 2 L/min of oxygen via nasal cannula shows an oxygen saturation of 97%. Cardiac examination shows a regular heartbeat and a systolic ejection murmur heard best over the upper right sternal border. The lungs are clear to auscultation bilaterally. Pedal pulses are intact. An ECG shows inverted T waves in leads I, avL, and V5-6. Urine toxicology screening is positive for cocaine. Which of the following drugs is contraindicated in the management of this patient's condition?
A 28-year-old female patient with a history of schizophrenia, type 2 diabetes mellitus, and hypothyroidism comes to clinic stating she would like to be put back on a medication. She recently stopped taking her haloperidol as it made it hard for her to "sit still." She requests to be put on olanzapine as a friend from a support group said it was helpful. Why should this medication be avoided in this patient?
A 4-year-old boy presents to the ED with a one day history of severe right eye pain accompanied by nausea, vomiting, and headache. He is afebrile and he appears to be alert despite being irritable. Three days ago an ophthalmologist prescribed eye drops for his right eye but his parents do not know the name of the medication. On exam, his right eye is hard to palpation and moderately dilated. His left eye is unremarkable. What is the mechanism of action of the medication that most likely provoked this acute presentation?
A 30-year-old man presents with heartburn for the past couple of weeks. He says he feels a burning sensation in his chest, at times reaching his throat, usually worse after eating spicy foods. He is overweight and actively trying to lose weight. He also has tried other lifestyle modifications for the past couple of months, but symptoms have not improved. He denies any history of cough, difficulty swallowing, hematemesis, or melena. The patient says he often drinks a can of beer in the evening after work and does not smoke. His blood pressure is 124/82 mm Hg, pulse is 72/min and regular, and respiratory rate is 14/min. Abdominal tenderness is absent. Which of the following is the next best step in the management of this patient?
A 65-year-old veteran with a history of hypertension, diabetes, and end-stage renal disease presents with nausea, vomiting, and abdominal pain. The patient was found to have a small bowel obstruction on CT imaging. He is managed conservatively with a nasogastric tube placed for decompression. After several days in the hospital, the patient’s symptoms are gradually improving. Today, he complains of left leg swelling. On physical exam, the patient has a swollen left lower extremity with calf tenderness on forced dorsiflexion of the ankle. An ultrasound confirms a deep vein thrombus. An unfractionated heparin drip is started. What should be monitored to adjust heparin dosing?
A 28-year-old woman presents to a physician with complaints of fever, cough, and cold for the last 2 days. She does not have any other symptoms and she has no significant medical history. She has recently started using combined oral contraceptive pills (OCPs) for birth control. On physical examination, the temperature is 38.3°C (101.0°F), the pulse is 98/min, the blood pressure is 122/80 mm Hg, and the respiratory rate is 14/min. The nasal mucosa and pharynx are inflamed, but there is no purulent discharge. Auscultation of the chest does not reveal any abnormalities. She mentions that she has been a heavy smoker for the last 5 years, smoking about 15–20 cigarettes per day. The physician suggests she should discontinue using combined OCPs and choose an alternative contraception method. Which of the following best explains the rationale behind the physician's suggestion?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
