Autonomic/CV Drugs — MCQs

On this page
A 24-year-old woman, gravida 2, para 1, at 33 weeks’ gestation, is admitted to the hospital for treatment of preterm labor. She has no history of serious illness and her only medication is a multivitamin. Her temperature is 37.2°C (99.0°F), pulse is 100/min, respirations are 20/min, and blood pressure is 100/75 mm Hg. Therapy with nifedipine and betamethasone is begun. The patient continues to have contractions; nifedipine is discontinued and treatment with high-dose terbutaline is initiated. Her contractions resolve. Three hours later, the patient reports fatigue and weakness. Neurologic examination shows proximal muscle weakness of the lower extremities. Deep tendon reflexes are 1+ bilaterally. Which of the following is most likely to confirm the diagnosis?
A 48-year-old male with a history of rhinitis presents to the emergency department with complaints of shortness of breath and wheezing over the past 2 days. He reports bilateral knee pain over the past month for which he recently began taking naproxen 1 week ago. Physical examination is significant for a nasal polyp and disappearance of bilateral radial pulses on deep inspiration. Which of the following is the most likely cause of this patient's physical examination findings?
A 58-year-old female presents to her primary care physician with a 1-month history of facial and chest flushing, as well as intermittent diarrhea and occasional difficulty breathing. On physical exam, a new-onset systolic ejection murmur is auscultated and is loudest at the left second intercostal space. Subsequent echocardiography reveals leaflet thickening secondary to fibrous plaque deposition on both the pulmonic and tricuspid valves. Which of the following laboratory abnormalities would most likely be found in this patient?
One month after undergoing surgical spinal fusion because of a traumatic spinal cord injury, a 68-year-old man comes to the physician because of lower abdominal pain. He last voided yesterday. Physical examination shows a suprapubic mass and decreased sensation below the umbilicus. Urodynamic studies show simultaneous contractions of the detrusor muscle and the internal urethral sphincter. Urinary catheterization drains 900 mL of urine from the bladder. Which of the following is the most appropriate pharmacotherapy for this patient’s urinary symptoms?
A 24-year-old African American male with sickle cell disease has been followed by a hematologist since infancy. Two years ago, he was started on hydroxyurea for frequent pain crises but has not achieved good control. The addition of a Gardos channel blocking agent is being considered. What is the mechanism of action of this class of medications?
A 60-year-old woman presents to you with vision problems. Objects appear clear, but she just can't see as well as before. She says she first noticed this when she went to the movies with her grandkids, and she could not see the whole screen. She denies any complaints of redness, itchiness, or excessive tearing of her eyes. Current medications are captopril for her hypertension, acetaminophen for occasional headaches, and a daily multivitamin. Her vital signs are a blood pressure 130/80 mm Hg, pulse 80/min and regular, respiratory rate 14/min, and a temperature of 36.7°C (98.0°F). Eye examination reveals that her visual acuity is normal but the visual field is reduced with enlarged blind spots. Tonometry reveals mildly increased IOP. The patient is started on brimonidine. Which of the following statements best describes the therapeutic mechanism of action of this medication in this patient?
A 47-year-old woman comes to the physician because of a 5-month history of insomnia. She frequently experiences leg discomfort when trying to fall asleep that is relieved temporarily by movement. Her husband tells her that she frequently flexes her ankles upward when she sleeps. She appears fatigued and anxious. Physical examination shows no abnormalities. Laboratory studies including a complete blood count and iron studies are within the reference range. Which of the following is the most appropriate pharmacotherapy?
A 51-year-old man is undergoing chemotherapy treatment for a rapidly progressive newly-diagnosed acute myelogenous leukemia. On day 4 of his hospitalization, the patient is noted to be obtunded. Other than the chemotherapy, he is receiving lansoprazole, acetaminophen, and an infusion of D5–0.9% normal saline at 50 mL/h. On examination, the patient’s blood pressure is 94/50 mm Hg, heart rate is 52/min, and respiratory rate is 14/min. The patient appears weak but is in no acute distress. Chest auscultation reveals bibasilar crackles and scattered wheezing. His abdomen is soft, non-distended, and with a palpable liver and spleen. His ECG shows peaked T waves and widened QRS complexes. What is the best next step in the management of this patient?
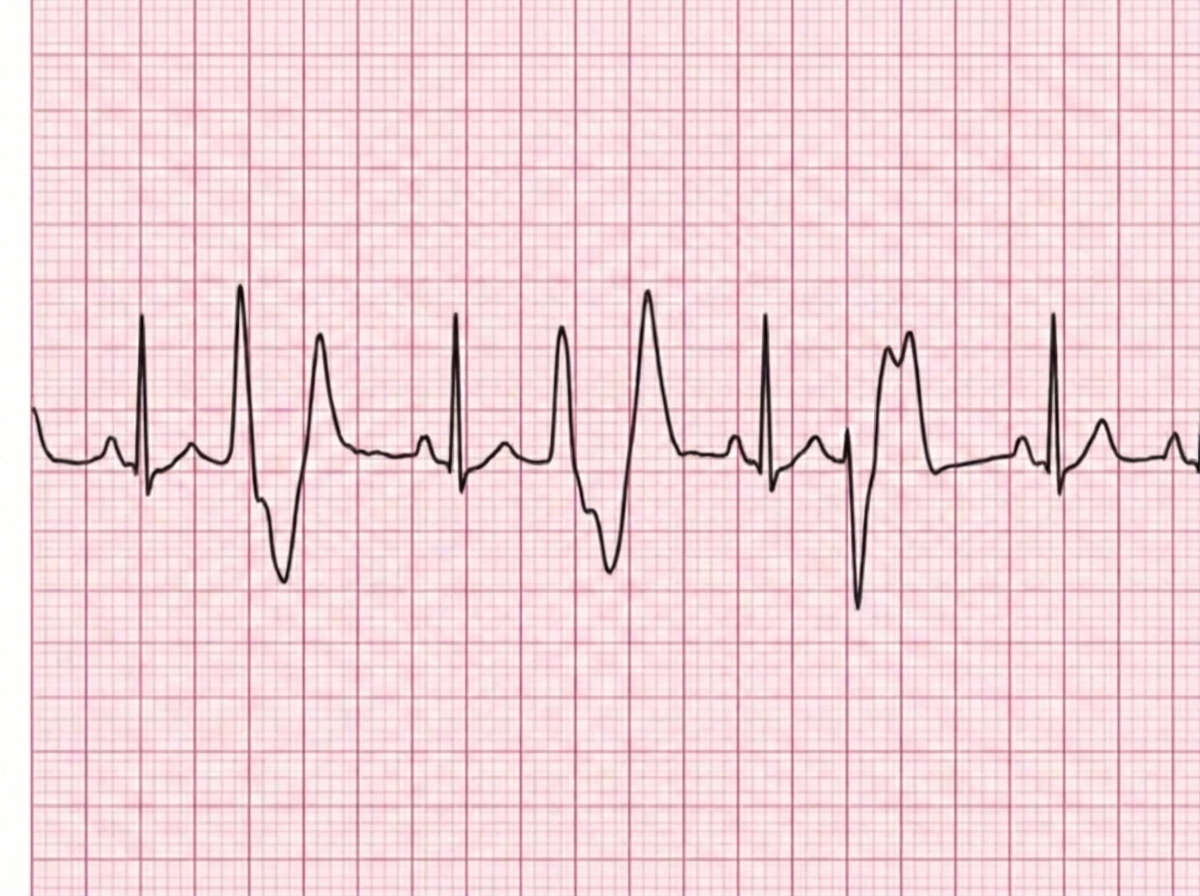
A 59-year-old man is brought to the emergency department because of a 2-hour history of abdominal pain and severe vomiting after ingesting an unknown medication in a suicide attempt. On the way to the hospital, he had a generalized tonic-clonic seizure. He has chronic obstructive pulmonary disease, coronary artery disease, and chronic back pain. His pulse is 130/min, respirations are 16/min, and blood pressure is 110/60 mm Hg. Serum studies show a glucose concentration of 180 mg/dL and a potassium concentration of 2.8 mEq/L. An ECG shows ventricular tachycardia. This patient's current findings are most likely caused by an overdose of which of the following drugs?
A 78-year-old female presents to her primary care provider complaining of shaking of her hands. She reports that her hands shake when she is pouring her coffee in the morning and when she is buttoning her shirt. She has noticed that her tremor improves with the several beers she has every night with dinner. She has a past medical history of hypertension, atrial fibrillation, moderate persistent asthma, acute intermittent porphyria, and urinary retention. Her home medications include hydrochlorothiazide, warfarin, bethanechol, low-dose inhaled fluticasone, and an albuterol inhaler as needed. On physical exam, she has an irregularly irregular heart rhythm without S3/S4. She has mild wheezing on pulmonary exam. She has no tremor when her hands are in her lap. A low-amplitude tremor is present during finger-to-nose testing. Her neurological exam is otherwise unremarkable. Which of the following is a contraindication to the first-line treatment of this condition?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
