Autonomic/CV Drugs — MCQs

On this page
A 7-year-old boy is brought to the physician by his mother because of a 2-week history of intermittent shortness of breath and a dry cough that is worse at night. He had an upper respiratory tract infection 3 weeks ago. Lungs are clear to auscultation. Spirometry shows normal forced vital capacity and peak expiratory flow rate. The physician administers a drug, after which repeat spirometry shows a reduced peak expiratory flow rate. Which of the following drugs was most likely administered?
A 27-year-old woman presents to the clinic with a runny nose and productive cough for the past two weeks. She also complains of headaches and lethargy. She was started on sertraline after she was diagnosed with major depressive disorder 2 months ago and had the dosage periodically increased to achieve symptom control. She is afraid of starting any other medication because of possible side-effects or life-threatening drug interactions. What advice is most accurate regarding possible complications to her current pharmacotherapy?
A 28-year-old woman presents with severe diarrhea and abdominal pain. She says she has had 10 watery stools since the previous morning and is experiencing severe cramping in her abdomen. She reports similar past episodes of diarrhea with excruciating abdominal pain and mentions that she has taken diphenoxylate and atropine before which had helped her diarrhea and pain but resulted in severe constipation for a week. Which of the following receptors does diphenoxylate activate to cause the effects mentioned by this patient?
A 28-year-old man presents to his primary care physician because he has been experiencing constipation for the last 6 days. He says that the constipation started 1 day after he started taking an over the counter medication for sinus congestion and a chronic cough. He has no other findings associated with the constipation. His past medical history is significant for seasonal allergies but he is not currently taking any other medications besides the one he reported. Which of the following drugs was most likely responsible for this patient's symptoms?
A 30-year-old man presents with a 1-month history of frequent intermittent headaches. He says the headaches typically occur between 3–4 times/day, mostly at night, each lasting minutes to 1–2 hours. He describes the pain as severe, stabbing, unilateral, and localized to the left periorbital region. He says he frequently notes increased tear production and conjunctival injection in the left eye and rhinorrhea during these headaches. He mentions that he had a similar 3-week episode of these same, frequent intermittent headaches 3 months ago which stopped completely until 1 month ago. He denies any seizures, loss of consciousness, nausea, vomiting, photophobia, or phonophobia. His past medical history is significant for stable angina secondary to coronary artery disease diagnosed on a stress echocardiogram 1 year ago. He reports occasional alcohol use, which he says precipitates the headaches, but denies any smoking or recreational drug use. The patient is afebrile, and his vital signs are within normal limits. A physical examination is unremarkable. A noncontrast computed tomography (CT) scan of the head is normal. Which of the following is the best abortive treatment for this patient?
A 55-year-old obese woman is referred to the cardiology clinic for progressive dyspnea. She has had no recent travel or sick contacts. Besides a multivitamin, she has only tried online weight-loss medications for the past five years, including fenfluramine-phentermine. An echocardiogram reveals a dilated right ventricle with systolic pressure of 60 mmHg as well as both tricuspid and pulmonary regurgitation. A right heart catheterization shows a mean pulmonary artery pressure of 40 mmHg. What disease process is most analogous to this patient's presentation?
A 21-year-old woman with type 1 diabetes mellitus suddenly develops tremors, cold sweats, and confusion while on a backpacking trip with friends. She is only oriented to person and is unable to follow commands. Her fingerstick blood glucose concentration is 28 mg/dL. Her friend administers an intramuscular injection with a substance that reverses her symptoms. Which of the following is the most likely mechanism of action of this drug?
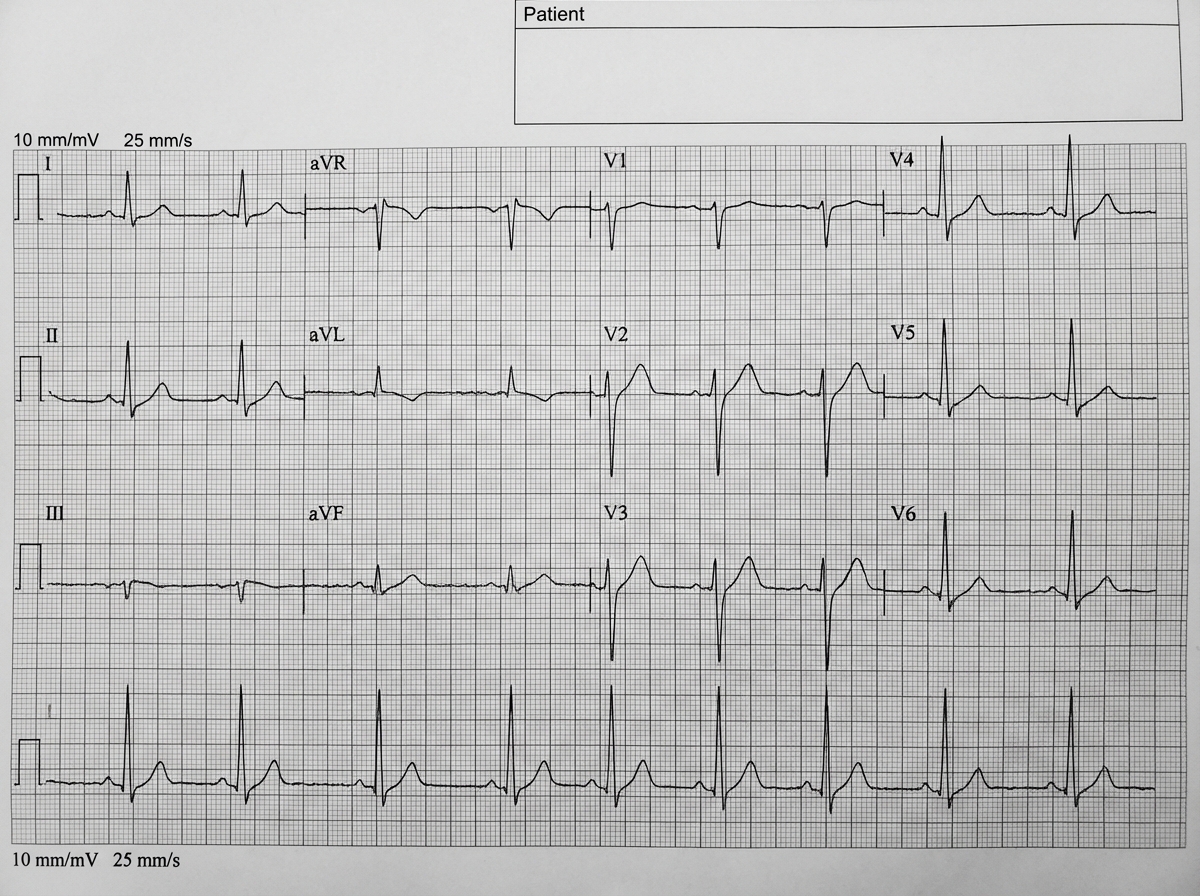
A 17-year-old boy was brought to the emergency department because of palpitations and lightheadedness that began 16 hours ago. He admitted to binge drinking the night before. He was sedated and electrically cardioverted. An ECG that was recorded following cardioversion is shown. After regaining consciousness, he was admitted for observation. Serum concentration of creatinine and electrolytes were measured to be within the reference range. Twelve hours after cardioversion, the patient complains again of palpitations. He does not have lightheadedness or chest pain. His temperature is 37.1°C (98.8°F), pulse is 220/min, respirations are 20/min, and blood pressure is 112/84 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 98%. Physical examination shows no abnormalities. A newly recorded ECG shows a shortened PR interval, and wide, monomorphic QRS complexes with a regular rhythm. Which of the following is the most appropriate next best step in management?
A 49-year-old man with alcohol use disorder is brought to the emergency department immediately after two episodes of coffee-ground emesis. His pulse is 116/min and blood pressure is 92/54 mm Hg. Physical examination shows a distended abdomen with shifting dullness. Skin examination shows jaundice, erythematous palms, and dilated veins in the anterior abdominal wall. After fluid resuscitation, he is given a drug that decreases portal venous pressure. The drug works by inhibiting the secretion of splanchnic vasodilatory hormones as well as blocking glucagon and insulin release. This drug is a synthetic analog of a substance normally produced in which of the following cells?
A 24-year-old man presents to his family practitioner for routine follow-up of asthma. He is currently on albuterol, corticosteroids, and salmeterol, all via inhalation. The patient is compliant with his medications, but he still complains of episodic shortness of breath and wheezing. The peak expiratory flow (PEF) has improved since the last visit, but it is still less than the ideal predicted values based on age, gender, and height. Montelukast is added to his treatment regimen. What is the mechanism of action of this drug?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
