Autonomic/CV Drugs — MCQs

On this page
A 27-year-old man presents to the outpatient clinic with a swollen and painful toe. The pain intensity increased further after he went to a party last night. Which of the following is the drug of choice for the treatment of this patient's condition?
A 43-year-old man presents to the emergency department with nausea and vomiting. He says symptoms onset 4 hours ago and is progressively worsening. He denies any hematemesis. Past medical history is significant for a recent negative screening colonoscopy that was performed due to a family history of colon cancer. His vital signs are significant for a temperature of 39.5°C (103.1°F). Physical examination is unremarkable. A contrast CT of the abdomen reveals a colonic perforation. Laboratory findings are significant for an elevated WBC count with a predominant left shift, a decreased platelet count, increased PT and PTT, slightly decreased hemoglobin/hematocrit, and prolonged bleeding time. Which of the following is most closely related to this patient's prolonged PT and PTT?
A 37-year-old previously healthy woman presents to the emergency room with right leg pain and difficulty breathing. She recently returned from a trip to Alaska and noticed her leg started to swell when she got home. Her medications include a multivitamin and oral contraceptives. She is diagnosed with a deep venous thrombosis complicated by a pulmonary embolism and started on anticoagulation. She remains stable and is discharged on the third hospital day with long-term anticoagulation. During the 2 month follow-up visit, the patient's lab results are as follows: Hemoglobin: 14 g/dL Hematocrit: 44% Leukocyte count: 5,000/mm^3 with normal differential Platelet count: 300,000/mm^3 Prothrombin time: 23 seconds Partial thromboplastin time (activated): 20 seconds Bleeding time: 4 minutes Which of the following factors is initially inhibited in the target pathway for her long-term treatment?
A 50-year-old woman, gravida 5, para 5, comes to the physician for the evaluation of decreased sexual desire for approximately 6 months. She has been sexually active with her husband but reports that she has no desire in having sexual intercourse anymore. She states that she feels guilty and is worried about losing her husband if this problem goes on for a longer period of time. She also reports that they have had several fights recently due to financial problems. She has problems going to sleep and wakes up often, and is tired throughout the day. One year ago, the patient underwent hysterectomy with bilateral salpingo-oophorectomy due to uterine prolapse. Her last menstrual period was 2 years ago. She does not smoke. She drinks 3–4 glasses of wine daily. Vital signs are within normal limits. Physical examination shows no abnormalities except for an enlarged liver. Which of the following most likely explains this patient's loss of libido?
A 73-year-old woman presents to the emergency department with diffuse abdominal pain, nausea, and vomiting. Her daughter who accompanies her says she was in her usual state of health until two days ago when she started to complain of abdominal pain and was unable to tolerate oral intake. She has hypertension, congestive heart failure, atrial fibrillation, and osteoarthritis. She underwent an exploratory laparotomy for an ovarian mass a year ago where a mucinous cystadenoma was excised. Her medications include aspirin, nifedipine, lisinopril, metoprolol, warfarin, and Tylenol as needed for pain. She does not drink alcohol or smoke cigarettes. She appears ill and disoriented. Her temperature is 37.9°C (100.3°F), blood pressure is 102/60 mm Hg, pulse is 110/min and irregular, and respirations are 16/min. Examination shows diffuse tenderness to palpation of the abdomen. The abdomen is tympanitic on percussion. Bowel sounds are hyperactive. The lungs are clear to auscultation bilaterally. There is a soft crescendo-decrescendo murmur best auscultated in the right second intercostal space. Laboratory studies show: Hemoglobin 10.2 g/dL Leukocyte count 14,000/mm3 Platelet count 130,000/mm3 Prothrombin time 38 seconds INR 3.2 Serum Na+ 132 mEq/dL K+ 3.6 mEq/dL Cl- 102 mEq/dL HCO3- 19 mEq/dL Urea nitrogen 36 mg/dl Creatinine 2.3 mg/dL Lactate 2.8 mEq/dL (N= 0.5-2.2 mEq/dL) An x-ray of the abdomen shows multiple centrally located dilated loops of gas filled bowel. There is no free air under the diaphragm. A nasogastric tube is inserted and IV fluids and empiric antibiotic therapy are started. Emergent exploratory laparotomy is planned. Which of the following is the next best step in management?
A 60-year-old man is brought to the emergency room because of fever and increasing confusion for the past 2 days. He has paranoid schizophrenia treated with chlorpromazine. He appears diaphoretic. His temperature is 40°C (104°F), pulse is 130/min, respirations are 29/min, and blood pressure is 155/100 mm Hg. Neurologic examination shows psychomotor agitation and incoherent speech. There is generalized muscle rigidity. His deep tendon reflexes are decreased bilaterally. Serum laboratory analysis shows a leukocyte count of 11,300/mm3 and serum creatine kinase concentration of 833 U/L. The most appropriate drug for this patient acts by inhibiting which of the following?
A 49-year-old man comes to the physician because of a 5-month history of progressive fatigue and exertional dyspnea. Cardiac examination shows a loud S2 in the 2nd left intercostal space. Right heart catheterization shows a pulmonary artery pressure of 32 mm Hg. Treatment with bosentan is initiated. The beneficial effect of this drug is due to binding to which of the following?
A 69-year-old woman with type 2 diabetes mellitus has an HbA1c of 7.9% and has been using basal-bolus insulin to manage her diabetes for the past 5 years. She has been maintaining a healthy diet, taking her insulin as scheduled but her records show morning hyperglycemia before eating breakfast. To determine the cause of this hyperglycemia, you ask her to set an alarm and take her blood glucose at 3 am. At 3 am her blood glucose is 49 mg/dL. Which of the following statements best describes the management of this patient's current condition?
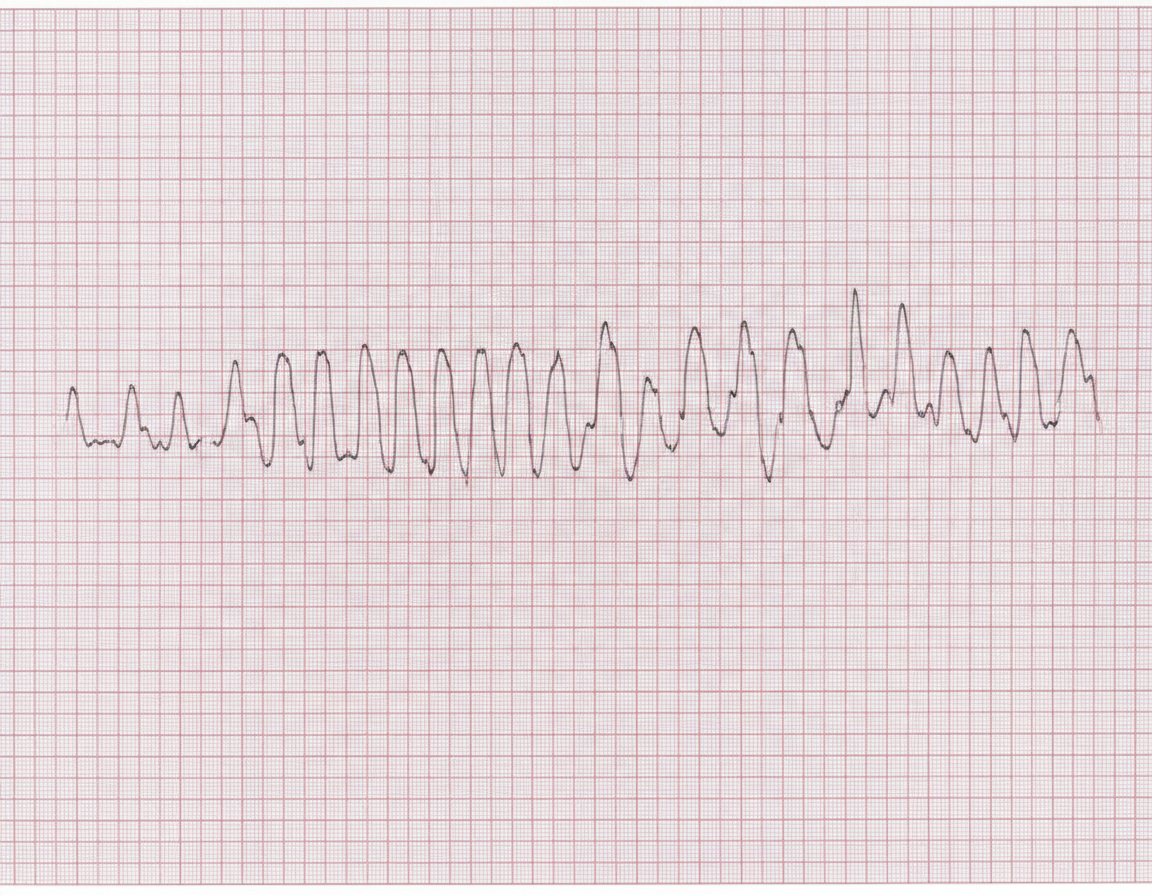
A 44-year-old woman is admitted after an episode of dizziness and palpitations with a subsequent loss of consciousness. At the time of admission, the patient is alert, but then quickly becomes lethargic and reports reoccurrence of palpitations. Past medical history is significant for an episode of ventricular tachycardia 4 months ago, now managed with pharmacologic antiarrhythmic prophylaxis. An ECG is obtained and is shown on the image. Which of the following antiarrhythmic drugs is most likely responsible for this patient's condition?
A 48-year-old homeless man is brought to the emergency department 2 hours after his right arm was burned by a fire. He is diagnosed with extensive third-degree burns of the right forearm and upper arm and is admitted to the hospital for debridement and grafting. During his stay in the hospital, he suddenly develops confusion and agitation. Neurologic examination shows horizontal nystagmus and a broad-based gait. Laboratory studies show decreased erythrocyte transketolase activity. Administration of which of the following most likely caused this patient's current condition?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
