Autonomic/CV Drugs — MCQs

On this page
A 54-year-old man electively underwent an open cholecystectomy for cholelithiasis. The procedure was performed under general anesthesia with inhaled anesthetic agents, including nitrous oxide, after induction with an intravenous agent. The surgeon operated quickly, and the procedure was uncomplicated. As the surgery ended, the anesthesia resident stopped the anesthesia and noticed the oxygen saturation gradually decreasing to 84%. He quickly administers 100% oxygen, and the hypoxia improves. Which of the following most likely accounts for the decreased oxygen saturation seen after the anesthesia was stopped in this patient?
A previously healthy 32-year-old man comes to the physician because of a 2-month history of fatigue and daytime sleepiness. He works as an accountant and cannot concentrate at work anymore. He also has depressed mood and no longer takes pleasure in activities he used to enjoy, such as playing tennis with his friends. He has decreased appetite and has had a 4-kg (8.8-lb) weight loss of over the past 2 months. He does not have suicidal ideation. He is diagnosed with major depressive disorder and treatment with paroxetine is begun. The patient is at greatest risk for which of the following adverse effects?
A 60-year-old man is brought to the emergency room because of fever and increasing confusion for the past 2 days. He has paranoid schizophrenia and hypertension. His current medications are chlorpromazine and amlodipine. He appears ill. He is not oriented to time, place, or person. His temperature is 40°C (104°F), pulse is 130/min, respirations are 29/min and blood pressure is 155/100 mm Hg. Examination shows diaphoresis. Muscle tone is increased bilaterally. Deep tendon reflexes are 1+ bilaterally. Neurologic examination shows psychomotor agitation. His speech is incoherent. Lungs are clear to auscultation. His neck is supple. The abdomen is soft and nontender. Serum laboratory analysis shows a leukocyte count of 11,300/mm3 and serum creatine kinase concentration of 833 U/L. Which of the following is the most appropriate initial pharmacotherapy?
A 42-year-old man is brought to the emergency department after having a seizure. His wife states that the patient has been struggling with alcohol abuse and has recently decided to "quit once and for all". Physical exam is notable for a malnourished patient responsive to verbal stimuli. He has moderate extremity weakness, occasional palpitations, and brisk deep tendon reflexes (DTRs). EKG demonstrates normal sinus rhythm and a prolonged QT interval. What nutritional deficiency most likely contributed to these findings?
A 65-year-old woman with COPD comes to the emergency department with 2-day history of worsening shortness of breath and cough. She often has a mild productive cough, but she noticed that her sputum is more yellow than usual. She has not had any recent fevers, chills, sore throat, or a runny nose. Her only medication is a salmeterol inhaler that she uses twice daily. Her temperature is 36.7°C (98°F), pulse is 104/min, blood pressure is 134/73 mm Hg, respiratory rate is 22/min, and oxygen saturation is 85%. She appears uncomfortable and shows labored breathing. Lung auscultation reveals coarse bibasilar inspiratory crackles. A plain film of the chest shows mild hyperinflation and flattening of the diaphragm but no consolidation. She is started on supplemental oxygen via nasal cannula. Which of the following is the most appropriate initial pharmacotherapy?
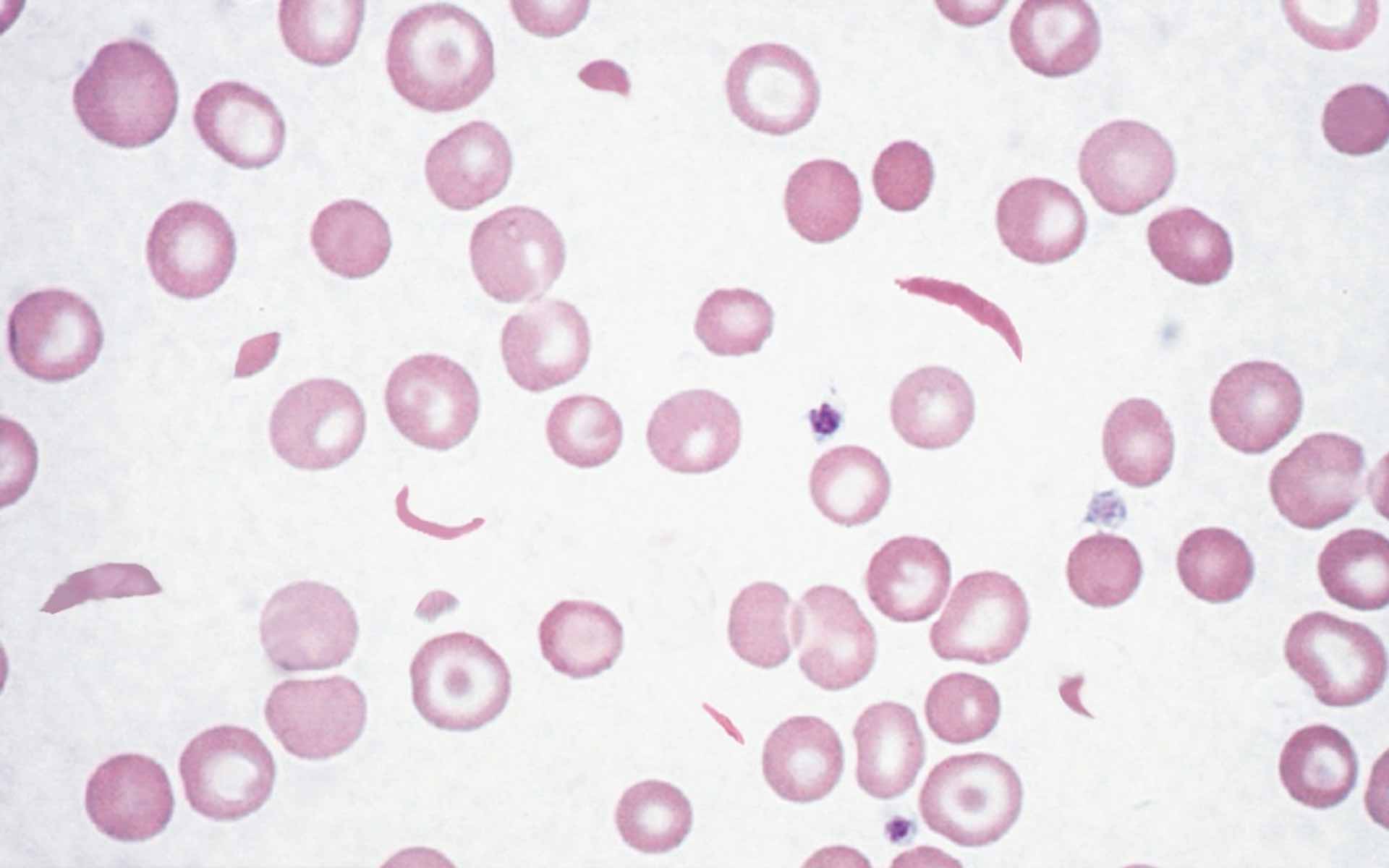
A 3-year-old boy is brought to the emergency department because of worsening pain and swelling in both of his hands for 1 week. He appears distressed. His temperature is 38.5°C (101.4°F). Examination shows erythema, swelling, warmth, and tenderness on the dorsum of his hands. His hemoglobin concentration is 9.1 g/dL. A peripheral blood smear is shown. The drug indicated to prevent recurrence of this patient's symptoms is also used to treat which of the following conditions?
A 48-year-old man with a long history of mild persistent asthma on daily fluticasone therapy has been using his albuterol inhaler every day for the past month and presents requesting a refill. He denies any recent upper respiratory infections, but he says he has felt much more short of breath throughout this time frame. He works as a landscaper, and he informs you that he has been taking longer to complete some of his daily activities on the job. The vital signs include: temperature 36.7°C (98.0°F), blood pressure 126/74 mm Hg, heart rate 74/min, and respiratory rate 14/min. His physical exam reveals mild bilateral wheezes and normal heart sounds. What changes should be made to his current regimen?
A 28-year-old man visits his physician complaining of hematochezia over the last several days. He also has tenesmus and bowel urgency without any abdominal pain. He has had several milder episodes over the past several years that resolved on their own. He has no history of a serious illness and takes no medications. His blood pressure is 129/85 mm Hg; temperature, 37.4°C (99.3°F); and pulse, 75/min. On physical exam, his abdominal examination shows mild tenderness on deep palpation of the left lower quadrant. Digital rectal examination reveals anal tenderness and fresh blood. Stool examination is negative for pathogenic bacteria and an ova and parasite test is negative. Erythrocyte sedimentation rate is 28 mm/h. Colonoscopy shows diffuse erythema involving the rectum and extending to the distal sigmoid. The mucosa also shows a decreased vascular pattern with fine granularity. The remaining colon and distal ileum are normal. Biopsy of the inflamed mucosa of the sigmoid colon shows distorted crypt architecture. The most appropriate next step is to administer which of the following?
A 73-year-old man presents to his primary care physician with chest pain. He noticed the pain after walking several blocks, and the pain is relieved by sitting. On exam, he has a BP 155/89 mmHg, HR 79 bpm, and T 98.9 F. The physician refers the patient to a cardiologist and offers prescriptions for carvedilol and nitroglycerin. Which of the following describes the mechanism or effects of each of these medications, respectively?
A 33-year-old woman comes to the physician for a follow-up examination. She has a history of Crohn disease, for which she takes methotrexate. She and her husband would like to start trying to have a child. Because of the teratogenicity of methotrexate, the physician switches the patient from methotrexate to a purine analog drug that inhibits lymphocyte proliferation by blocking nucleotide synthesis. Toxicity of the newly prescribed purine analog would most likely increase if the patient was also being treated with which of the following medications?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
