Autonomic/CV Drugs — MCQs

On this page
A 32-year-old woman brought to the emergency department because of a 1-week history of palpitations and shortness of breath. She has congestive heart failure. Current medications include furosemide, lisinopril, and atenolol. Her pulse is 124/min and irregularly irregular, and blood pressure is 110/70 mm Hg. Examination shows coarse crackles over the lower lung fields bilaterally. Treatment with digoxin is started. Five days later, an ECG shows prolongation of the PR interval. Which of the following is the most likely explanation for the observed effect of this drug?
A 2-year-old boy is brought to the physician for evaluation of delayed onset of speech. Over the past year, he has also had recurrent dizziness and three episodes of syncope. Examination of the ears shows clear auditory canals and intact tympanic membranes with normal light reflexes. Visual reinforcement audiometry shows bilateral sensorineural deafness. Genetic analysis reveals a mutation in the KCNQ1 gene causing a defect in slow voltage-gated potassium channels. An electrocardiogram of this patient is most likely to show which of the following?
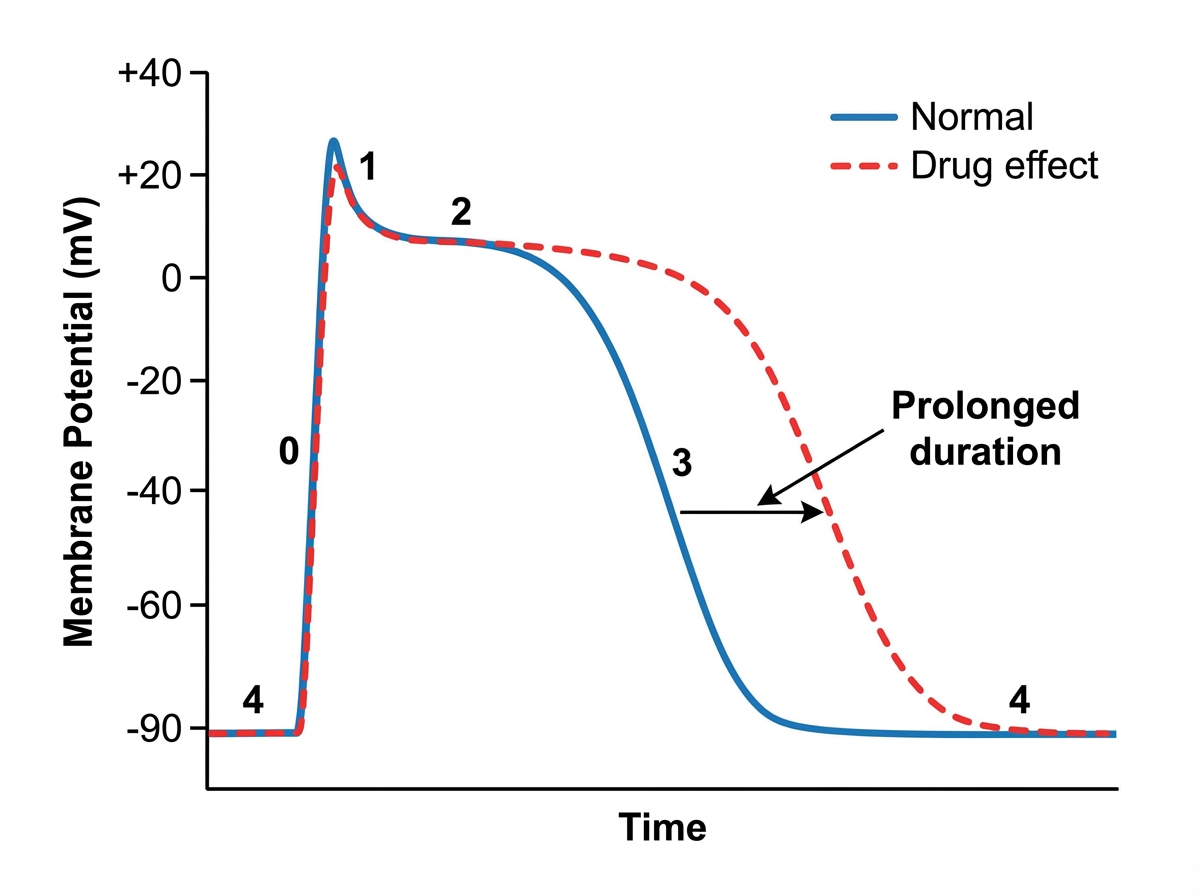
A 71-year-old woman comes to the physician because of dizziness and intermittent episodes of heart palpitations for 5 days. During this time, she has also had one episode of syncope. An ECG shows absence of P waves and irregular RR intervals. Treatment with an antiarrhythmic drug is initiated. The effect of the drug on the cardiac action potential is shown. Which of the following cardiac ion channels is most likely targeted by this drug?
A 45-year-old Caucasian male presents complaining of inability to open his mouth. Patient history reveals that he recently injured his foot from an exposed floor nail in his house. This patient's symptoms are likely the result of:
An 18-year-old college student presents to the ED straight from chemistry lab where he ingested an unknown compound. He complains of a headache, and is flushed, tachypneic and tachycardic. Suspecting cyanide poisoning, you administer amyl nitrite which causes which of the following?
A pharmaceutical company has created an experimental medication, Drug Z, for patients with relapsing-remitting multiple sclerosis. Drug Z has been deemed to be safe in rats and is nearly ready for human trials. Before initiating a Phase I clinical trial, the company would like to study the medication’s pharmacokinetic properties in humans. The drug was found to have a half-life of 2.5 hours and is eliminated by first-order kinetics. The volume of distribution of the drug is determined to be 0.5 L/kg. The drug is administered intravenously and sublingually and plasma drug concentration vs. time plots are obtained. Intravenous administration of 10 mg of Drug Z yields an area under the curve (AUC) of 15 mg hr/L. Sublingual administration of 25 mg of Drug Z yields an area under the curve of 20 mg hr/L. What is the absolute bioavailability of this medication?
A goalkeeper of a famous soccer team gives an interview with a health agency regarding his childhood. He describes how when he was a child, he would constantly clear his throat in class and the teachers would write a note to his mother with advice to go see an ENT doctor. He complained of being restless, fidgety, and sometimes hyperactive in class, disrupting the environment and causing him many social problems. He would blurt out the answer at times and keep repeating it without any control, leading to some embarrassing timeouts. But he was always nice to his teachers, so he calls it a “benign frustration” rather than aggressively causing distress. He also talked about how his symptoms were dramatically improved with medication. Which of the following is an FDA approved drug for this patient’s most likely condition?
A 32-year-old man presents to the emergency department with vomiting, diarrhea, and abdominal pain 2 hours after eating seafood in a restaurant. He also mentions that immediately after ingestion of the food, he experienced tingling and numbness over the lips and face. On physical examination, his vital signs are stable. On neurological examination, he has reduced strength in the lower extremities, but deep tendon reflexes are present and normal. Laboratory evaluation of the seafood from the restaurant confirms the presence of a toxin which is known to block voltage-gated fast sodium channels. Which of the following toxins is the most likely cause of the patient’s symptoms?
A 44-year-old man presents to the clinic with recurrent epigastric pain following meals for a month. He adds that the pain radiates up his neck and throat. Over the counter antacids have not helped. On further questioning, he endorses foul breath upon waking in the morning and worsening of pain when lying down. He denies any recent weight loss. His temperature is 37°C (98.6°F), respirations are 15/min, pulse is 70/min, and blood pressure is 100/84 mm Hg. A physical examination is performed which is within normal limits except for mild tenderness on deep palpation of the epigastrium. An ECG performed in the clinic shows no abnormalities. What is the next best step in the management of this patient?
A 57-year-old man comes to the emergency department because of shortness of breath and palpitations for 3 hours. He has had similar episodes intermittently for 4 months. His pulse is 140/min and blood pressure is 90/60 mm Hg. An ECG shows irregular narrow-complex tachycardia with no discernable P waves. Emergent electrical cardioversion is performed and the patient reverts to normal sinus rhythm. Pharmacotherapy with sotalol is begun. Which of the following is the most likely physiologic effect of this drug?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
