Autonomic/CV Drugs — MCQs

On this page
A 33-year-old woman comes to the physician because of a 3-day history of dry cough and low-grade fever. Four months ago, she was diagnosed with major depressive disorder and started treatment with fluoxetine. Physical examination shows no abnormalities. A diagnosis of upper respiratory infection is made and medication is prescribed to relieve her symptoms. A drug with which of the following mechanisms of action should be avoided in this patient?
A 64-year-old man presents to his physician for a scheduled follow-up visit. He has chronic left-sided heart failure with systolic dysfunction. His current regular medications include captopril and digoxin, which were started after his last episode of symptomatic heart failure approximately 3 months ago. His last episode of heart failure was accompanied by atrial fibrillation, which followed an alcohol binge over a weekend. Since then he stopped drinking. He reports that he has no current symptoms at rest and is able to perform regular physical exercise without limitation. On physical examination, mild bipedal edema is noted. The physician suggested to him that he should discontinue digoxin and continue captopril and scheduled him for the next follow-up visit. Which of the following statements best justifies the suggestion made by the physician?
A 19-year-old G1P0 presents to the emergency department with severe abdominal pain. She states that the pain has been recurring every 3 to 5 minutes for the past 5 hours. She denies having regular prenatal care but recalls that her last menstrual period was about 9 months ago. She initially denies substance use but later admits to occasional prescription pain medication use during pregnancy. Her temperature is 98°F (37°C), blood pressure is 120/60 mmHg, pulse is 120/min, and respirations are 18/min. Tenderness is elicited in the lower abdominal quadrants. Clear fluid is seen in her vaginal vault with a fetal crown seen at 10 cm cervical dilation and +1 station. The patient is emergently taken into the labor and delivery suite, where she delivers a male infant with APGAR scores of 9 and 9 at 5 and 10 minutes, respectively. Several hours after delivery, the nurse notes that the infant is very irritable and crying in high pitches. The infant appears very diaphoretic with a runny nose and flailing limbs. What is the necessary pharmacological treatment for this patient?
A 25-year-old woman presents to the ED with nausea, vomiting, diarrhea, abdominal pain, and hematemesis after ingesting large quantities of a drug. Which of the following pairs a drug overdose with the correct antidote for this scenario?
A 48-year-old woman comes to the physician for a follow-up examination. At her visit 1 month ago, her glomerular filtration rate (GFR) was 100 mL/min/1.73 m2 and her renal plasma flow (RPF) was 588 mL/min. Today, her RPF is 540 mL/min and her filtration fraction (FF) is 0.2. After her previous appointment, this patient was most likely started on a drug that has which of the following effects?
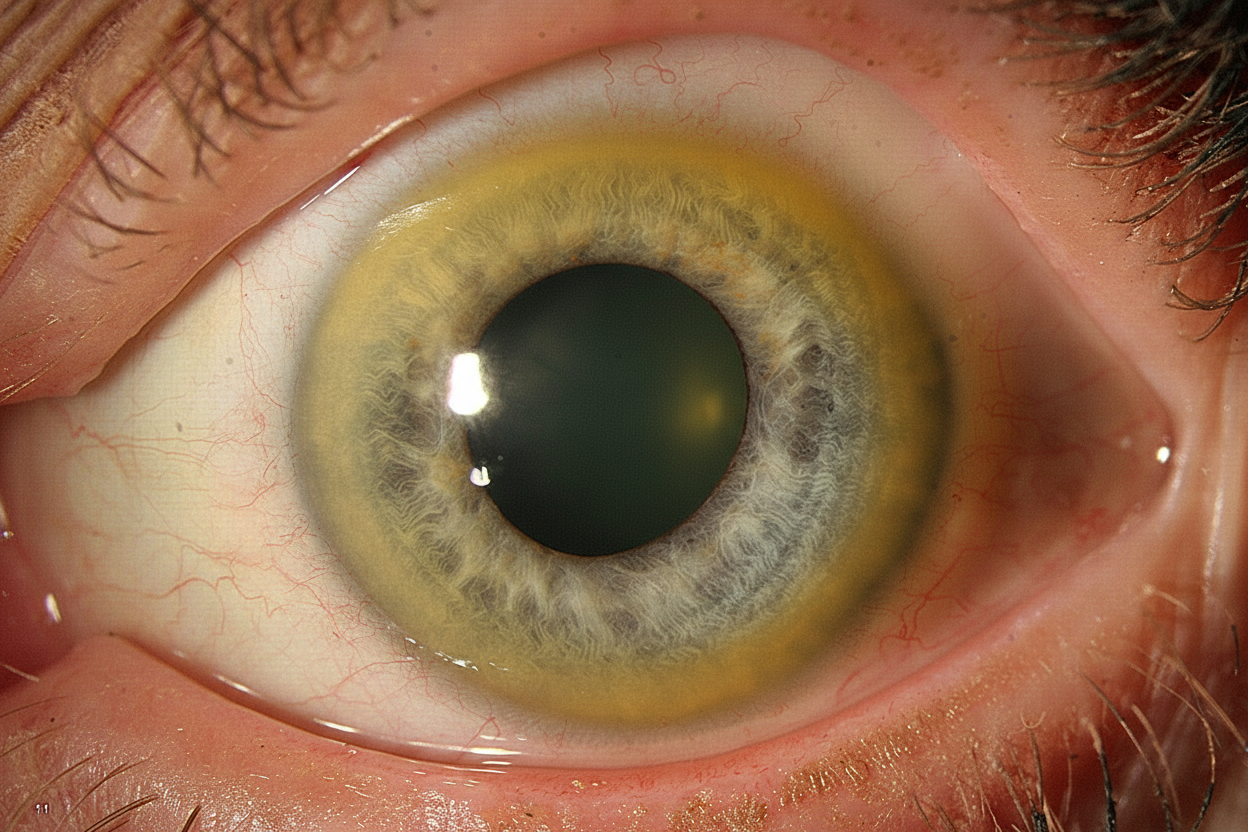
A 17-year-old man presents to his primary care physician with bilateral tremor of the hands. He is a senior in high school and during the year, his grades have plummeted to the point that he is failing. He says his memory is now poor, and he has trouble focusing on tasks. His behavior has changed in the past 6 months in that he has frequent episodes of depression, separated by episodes of bizarre behavior, including excessive alcohol drinking and shoplifting. His parents have started to suspect that he is using street drugs, which he denies. His handwriting has become very sloppy. His parents have noted slight slurring of his speech. Family history is irrelevant. Physical examination reveals upper extremity tremors, mild dystonia of the upper extremities, and mild incoordination involving his hands. The patient’s eye is shown. Which of the following is the best initial management of this patient’s condition?
A 23-year-old male is brought into the emergency department by his girlfriend following an argument. The patient’s girlfriend claims that she threatened to break up with him. He then called her saying he was going to kill himself. When she arrived at the patient’s home, she found him lying on the couch with empty alcohol bottles and multiple pill containers. The patient reports he does not remember everything he took, but says he ingested many pills about four hours ago. The patient’s temperature is 99°F (37.2°C), blood pressure is 110/68 mmHg, pulse is 88/min, and respirations are 25/min with an oxygen saturation of 98% O2 on room air. An arterial blood gas (ABG) is obtained, with results shown below: pH: 7.47 pO2: 94 mmHg pCO2: 24 mmHg HCO3-: 22 mEq/L You check on him a couple hours later, and the patient appears agitated. His girlfriend says he keeps grabbing his head, yelling about non-stop ringing in his ears. Labs and a repeat ABG shows: pH: 7.30 pO2: 90 mmHg pCO2: 22 mmHg HCO3-: 9 mEq/L Na+: 144 mEq/L Cl-: 98 mEq/L K+: 3.6 mEq/L BUN: 18 mg/dL Glucose: 100 mg/dL Creatinine: 1.4 mg/dL Which of the following is the best next step in management?
A 45-year-old woman comes to the physician because of a 6-month history of worsening involuntary movement of the left hand. Her symptoms are worse when she feels stressed at work. She has no history of serious illness and takes no medications. Neurological examination shows difficulty initiating movement and a tremor in the left hand at rest. The tremor decreases when the patient is asked to draw a circle. Which of the following is the most appropriate pharmacotherapy?
A previously healthy 29-year-old man comes to the emergency department because of a 4-day history of abdominal pain and confusion. Prior to the onset of the abdominal pain, he visited a festival where he consumed large amounts of alcohol. Examination shows a distended abdomen, decreased bowel sounds, and diffuse tenderness to palpation. There is motor weakness in the upper extremities. Sensation is decreased over the upper and lower extremities. Laboratory studies show no abnormalities. Which of the following is the most appropriate therapy for this patient's condition?
A 45-year-old male presents to the emergency room for toe pain. He reports that his right great toe became acutely painful, red, and swollen approximately five hours prior. He has had one similar prior episode six months ago that resolved with indomethacin. His medical history is notable for obesity, hypertension, and alcohol abuse. He currently takes hydrochlorothiazide (HCTZ). On physical examination, his right great toe is swollen, erythematous, and exquisitely tender to light touch. The patient is started on a new medication that decreases leukocyte migration and mitosis, and his pain eventually resolves; however, he develops nausea and vomiting as a result of therapy. Which of the following underlying mechanisms of action is characteristic of this patient’s new medication?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
