Autonomic/CV Drugs — MCQs

On this page
A 25-year-old man presents to the emergency department with pain in his leg. He states that the pain was sudden and that his leg feels very tender. This has happened before, but symptoms resolved a few days later with acetaminophen. His temperature is 98.5°F (36.9°C), blood pressure is 129/88 mmHg, pulse is 90/min, respirations are 12/min, and oxygen saturation is 98% on room air. Physical exam reveals clear breath sounds bilaterally and a normal S1 and S2. The patient’s right leg is red, inflamed, and tender to palpation inferior to the popliteal fossa. Which of the following is the best treatment for this patient?
A 42-year-old man is brought in to the emergency department by his daughter. She reports that her father drank heavily for the last 16 years, but he stopped 4 days ago after he decided to quit drinking on his birthday. She also reports that he has been talking about seeing cats running in his room since this morning, although there were no cats. There is no history of any known medical problems or any other substance use. On physical examination, his temperature is 38.4ºC (101.2ºF), heart rate is 116/min, blood pressure is 160/94 mm Hg, and respiratory rate is 22/min. He is severely agitated and is not oriented to his name, time, or place. On physical examination, profuse perspiration and tremors are present. Which of the following best describes the pathophysiologic mechanism underlying his condition?
A 47-year-old African-American woman presents to her primary care physician for a general checkup appointment. She works as a middle school teacher and has a 25 pack-year smoking history. She has a body mass index (BMI) of 22 kg/m^2 and is a vegetarian. Her last menstrual period was 1 week ago. Her current medications include oral contraceptive pills. Which of the following is a risk factor for osteoporosis in this patient?
A 33-year-old man comes to the emergency department because of a pounding headache for the past 3 hours. The pain is 8 out of 10 in intensity, does not radiate, and is not relieved by ibuprofen. He also has associated dizziness, blurring of vision, and palpitations. He has had similar episodes over the last 6 months but none this severe. He has not had fever, weight change, or loss of appetite. He underwent an appendectomy at the age of 18. His father died of renal cancer. He is diaphoretic. His temperature is 36.8°C (98.4°F), pulse is 112/min, and blood pressure is 220/130 mm Hg. Physical examination shows no abnormalities. Laboratory studies show: Hemoglobin 14.8 g/dL Leukocyte count 9600/mm3 Platelet count 345,000/mm3 Serum Glucose 112 mg/dL Na+ 137 mEq/L K+ 4.2 mEq/L Cl- 105 mEq/L Creatinine 1.0 mg/dL Urine dipstick shows no abnormalities. Which of the following findings on imaging is the most likely explanation for this patient's symptoms?
A 25-year-old man presents to the clinic with a complaint of lightheadedness when standing up from his bed in the morning and then from his chair at work. He has had similar complaints for many months, and the symptoms have not improved despite drinking lots of fluids, eating regular meals, and taking daily multivitamin. His daily routine is disturbed as he finds himself getting up very slowly to avoid the problem. This has created some awkward situations at his workplace and in social settings. His blood pressure while seated is 120/80 mm Hg, and upon standing it falls to 100/68 mm Hg. The physical examination is unremarkable except for a strong odor suggestive of marijuana use. The patient denies drug use and insists the odor is due to his roommate who smokes marijuana for medical purposes. No pallor or signs of dehydration are seen. The lab results are as follows: Serum Glucose 90 mg/dL Sodium 140 mEq/L Potassium 4.1 mEq/L Chloride 100 mEq/L Serum Creatinine 0.8 mg/dL Blood Urea Nitrogen 9 mg/dL Hemoglobin (Hb) Concentration 15.3 g/dL Mean Corpuscular Volume (MCV) 83 fl Reticulocyte count 0.5% Erythrocyte count 5.3 million/mm3 Platelet count 200,000/mm3 The ECG shows no abnormal finding. Which of the following could alleviate this patient’s symptoms?
A 7-year-old boy with asthma is brought to the physician because of a 1-month history of worsening shortness of breath and cough. The mother reports that the shortness of breath usually occurs when he is exercising with his older brother. His only medication is an albuterol inhaler that is taken as needed. The physician considers adding zafirlukast to his drug regimen. Which of the following is the most likely mechanism of action of this drug?
A 38-year-old man comes to the physician because of a 2-year-history of cough and progressively worsening breathlessness. He has smoked 1 pack of cigarettes daily for the past 10 years. Physical examination shows contraction of the anterior scalene and sternocleidomastoid muscles during inspiration. An x-ray of the chest shows flattening of the diaphragm and increased radiolucency in the lower lung fields. Further analysis shows increased activity of an isoform of elastase that is normally inhibited by alpha-1-antitrypsin. The cells that produce this isoform of elastase were most likely stimulated to enter the site of inflammation by which of the following substances?
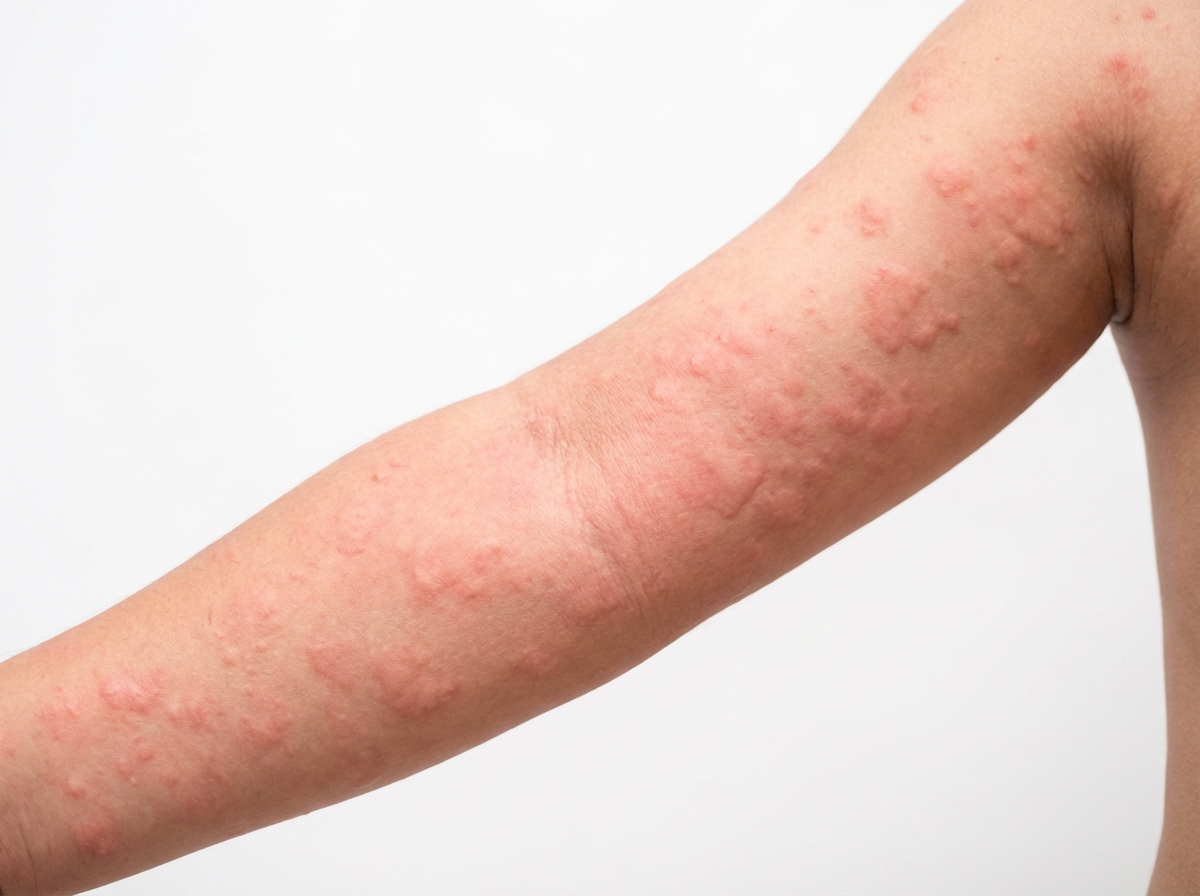
A 10-year-old boy presents to the emergency department with sudden shortness of breath. He was playing in the school garden and suddenly started to complain of abdominal pain. He then vomited a few times. An hour later in the hospital, he slowly developed a rash on his chest, arms, and legs. His breathing became faster with audible wheezing. On physical examination, his vital signs are as follows: the temperature is 37.0°C (98.6°F), the blood pressure is 100/60 mm Hg, the pulse is 130/min, and the respiratory rate is 25/min. A rash is on his right arm, as shown in the image. After being administered appropriate treatment, the boy improves significantly, and he is able to breathe comfortably. Which of the following is the best marker that could be measured in the serum of this boy to help establish a definitive diagnosis?
A 17-year-old high school student is brought to the emergency department because of irritability and rapid breathing. He appears agitated and is diaphoretic. His temperature is 38.3°C (101°F), pulse is 129/min, respirations are 28/min, and blood pressure is 158/95 mmHg. His pupils are dilated. An ECG shows sinus tachycardia. Which of the following substances is used to make the drug this patient has most likely taken?
A 60-year-old man is brought to the emergency department because of a 30-minute history of dizziness and shortness of breath. After establishing the diagnosis, treatment with a drug is administered. Shortly after administration, the patient develops severe left eye pain and decreased vision of the left eye, along with nausea and vomiting. Ophthalmologic examination shows a fixed, mid-dilated pupil and a narrowed anterior chamber of the left eye. The patient was most likely treated for which of the following conditions?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
