Autonomic/CV Drugs — MCQs

On this page
A 48-year-old woman underwent a thyroidectomy with central neck dissection due to papillary thyroid carcinoma. On day 2 postoperatively, she developed irritability, dysphagia, difficulty breathing, and spasms in different muscle groups in her upper and lower extremities. The vital signs include blood pressure 102/65 mm Hg, heart rate 93/min, respiratory rate 17/min, and temperature 36.1℃ (97.0℉). Physical examination shows several petechiae on her forearms, muscle twitching in her upper and lower extremities, expiratory wheezes on lung auscultation, decreased S1 and S2 and the presence of an S3 on cardiac auscultation, and positive Trousseau and Chvostek signs. Laboratory studies show: Ca2+ 4.4 mg/dL Mg2+ 1.7 mEq/L Na+ 140 mEq/L K+ 4.3 mEq/L Cl- 107 mEq/L HCO3- 25 mEq/L Administration of which of the following agents could prevent the patient’s condition?
A 25-year-old man presents to the emergency department after a motor vehicle accident. He was the unrestrained front seat driver in a head on collision. The patient is unresponsive and his medical history is unknown. His temperature is 99.5°F (37.5°C), blood pressure is 67/38 mmHg, pulse is 190/min, respirations are 33/min, and oxygen saturation is 98% on room air. The patient is started on IV fluids, blood products, and norepinephrine. A FAST exam is performed and a pelvic binder is placed. One hour later, his temperature is 98.3°F (36.8°C), blood pressure is 119/66 mmHg, pulse is 110/min, respirations are 15/min, and oxygen saturation is 97% on room air. The patient is currently responsive. Management of the patient's pelvic fracture is scheduled by the orthopedic service. While the patient is waiting in the emergency department he suddenly complains of feeling hot, aches, and a headache. The patient's temperature is currently 101°F (38.3°C). He has not been given any pain medications and his past medical history is still unknown. Which of the following is the most likely diagnosis?
A 16-year-old boy with history of seizure disorder is rushed to the Emergency Department with multiple generalized tonic-clonic seizures that have spanned more than 30 minutes in duration. He has not regained consciousness between these episodes. In addition to taking measures to ensure that he maintains adequate respiration, which of the following is appropriate for initial pharmacological therapy?
A 60-year-old male presents to the emergency room complaining of substernal chest pain. He reports a three-hour history of dull substernal chest pain that radiates into his left arm and jaw. He had a similar incident two months ago after walking one mile, but this pain is more severe. His past medical history is notable for hypertension and hyperlipidemia. An EKG demonstrates non-specific changes. Serum troponins are normal. In addition to aspirin, oxygen, and morphine, he is started on a medication that releases nitric oxide. Which of the following is a downstream effect of this molecule?
A 5-year-old boy undergoes MRI neuroimaging for the evaluation of worsening headaches and intermittent nausea upon awakening. He receives a bolus of intravenous thiopental for sedation during the procedure. Ten minutes after the MRI, the patient is awake and responsive. Which of the following pharmacological properties is most likely responsible for this patient's rapid recovery from this anesthetic agent?
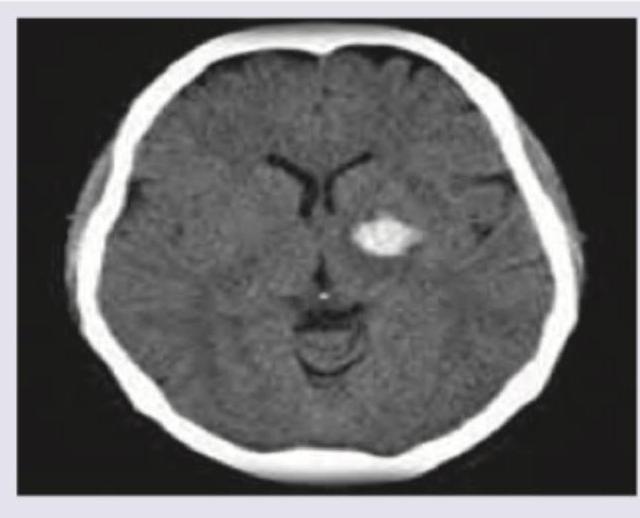
A 70-year-old Caucasian male presents to the emergency room following a fall. The patient's past medical history is significant for myocardial infarction and atrial fibrillation. His home medications are unknown. The patient's head CT is shown in Image A. Laboratory results reveal an International Normalized Ratio (INR) of 6. Which of the following is the most appropriate pharmacologic therapy for this patient?
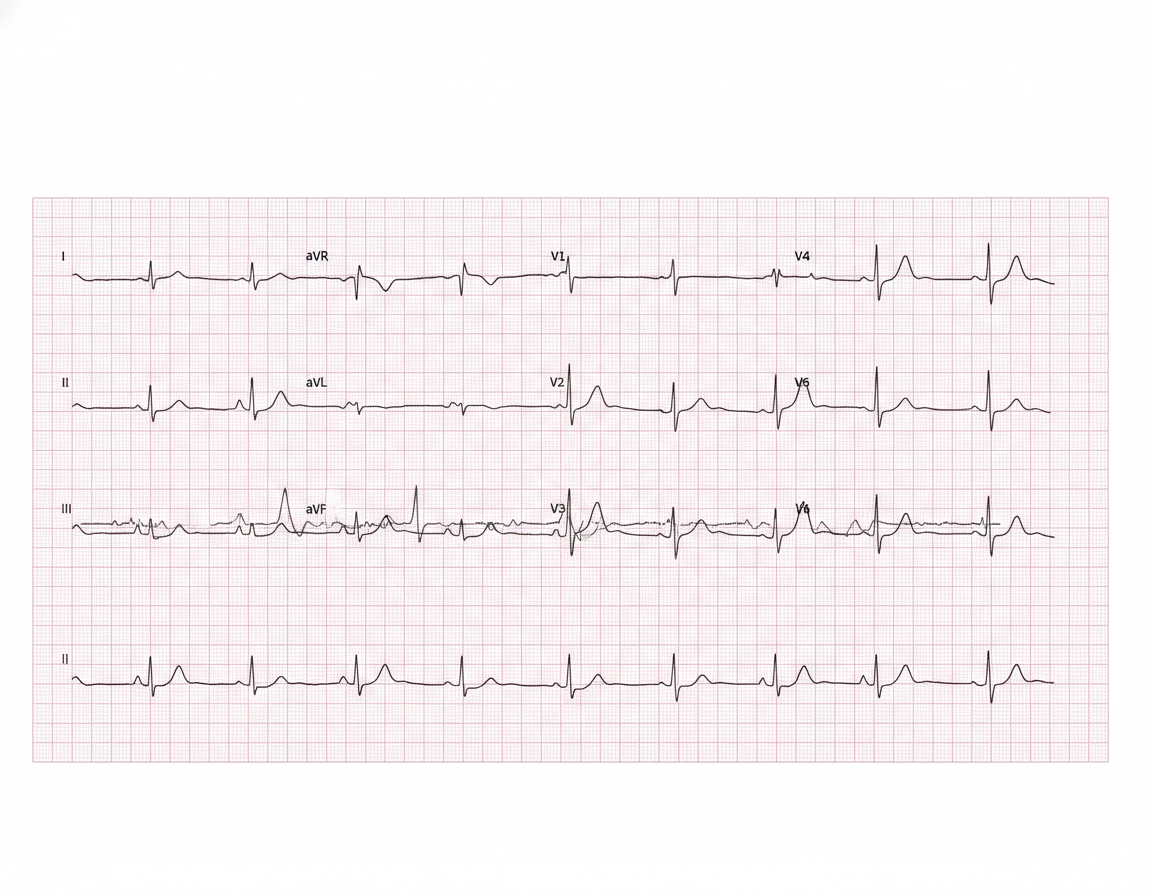
A 57-year-old man presents to the emergency department for evaluation of slurred speech and left arm and leg weakness over the last 3 hours. History reveals hypertension that is being treated with hydrochlorothiazide. Vital signs include: blood pressure of 110/70 mm Hg, heart rate 104/min, respiratory rate 18/min, and temperature 36.6°C (98.0°F). Physical examination reveals 2/5 strength in both left upper and lower extremities. After 2 hours, the patient’s symptoms suddenly disappear. An electrocardiogram (ECG) is obtained (see image). Which of the following medications could prevent ischemic attacks in this patient in the future?
A 66-year-old man is brought to the emergency department 1 hour after the abrupt onset of painless loss of vision in his left eye. Over the last several years, he has noticed increased blurring of vision; he says the blurring has made it difficult to read, but he can read better if he holds the book below or above eye level. He has smoked 1 pack of cigarettes daily for 40 years. Fundoscopic examination shows subretinal fluid and small hemorrhage with grayish-green discoloration in the macular area in the left eye, and multiple drusen in the right eye with retinal pigment epithelial changes. Which of the following is the most appropriate pharmacotherapy for this patient's eye condition?
A 35-year-old woman presents to the clinic with a 2-week history of headaches. She was in her usual state of health until 2 weeks ago, when she started having headaches. The headaches are throughout her whole head and rated as a 7/10. They are worse in the mornings and when she bends over. She has some mild nausea, but no vomiting. The headaches are not throbbing and are not associated with photophobia or phonophobia. On further questioning, she has noticed more hair than usual on her pillow in the morning and coming out in her hands when she washes her hair. The past medical history is unremarkable; she takes no prescription medications, but for the past year she has been taking an oral 'health supplement' recommended by her sister, which she orders over the internet. She cannot recall the supplement's name and does not know its contents. The physical exam is notable for some mild hepatomegaly but is otherwise unremarkable. This patient's presentation is most likely related to which of the following micronutrients?
A 22-year-old woman with type 1 diabetes mellitus and mild asthma comes to the physician for a follow-up examination. She has had several episodes of sweating, dizziness, and nausea in the past 2 months that occur during the day and always resolve after she drinks orange juice. She is compliant with her diet and insulin regimen. The physician recommends lowering her insulin dose in certain situations. This recommendation is most important in which of the following situations?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
