Autonomic/CV Drugs — MCQs

On this page
A 31-year-old male with bipolar disorder comes to the physician because of erectile dysfunction for the past month. He cannot maintain an erection during intercourse and rarely wakes up with an erection. He says he is happy in his current relationship, but admits to decreased desire for sex and feeling embarrassed about his sexual performance. He sustained a lumbar vertebral injury one year ago following a motor vehicle accident. He takes medication for his bipolar disorder but does not remember the name. Physical examination shows testicular atrophy with otherwise normal genitalia. Which of the following is the most likely cause of this patient's symptoms?
A 23-year-old man comes to the emergency department because of a rash on his neck and back for the past 6 hours. He says that he first noticed some reddening of the skin on his back the previous evening, which turned into a blistering, red rash overnight. He went surfing the previous day and spent 5 hours at the beach. He reports having applied at least 1 oz of water-resistant SPF 30 sunscreen 30 minutes before leaving his home. His vitals are within normal limits. Physical examination shows erythema of the skin over the upper back and dorsum of the neck, with 3 vesicles filled with clear fluid. The affected area is edematous and tender to touch. Which of the following recommendations is most appropriate to prevent a recurrence of this patient's symptoms in the future?
A 58-year-old woman presents to the office after receiving a bone mineral density screening test result with a T score of -4.1 and a Z score of -3.8. She is diagnosed with osteoporosis. A review of her medical history reveals that she has taken estrogen-containing oral contraceptive pills from the age of 20 to 30. She suffered from heartburn from the age of 45 and took lansoprazole and ranitidine often for her symptoms. She also was on lithium for 2 years after being diagnosed with bipolar disorder at the age of 54. Last year she was diagnosed with congestive heart failure and was started on low dose hydrochlorothiazide. Which of her medications most likely contributed to the development of her osteoporosis?
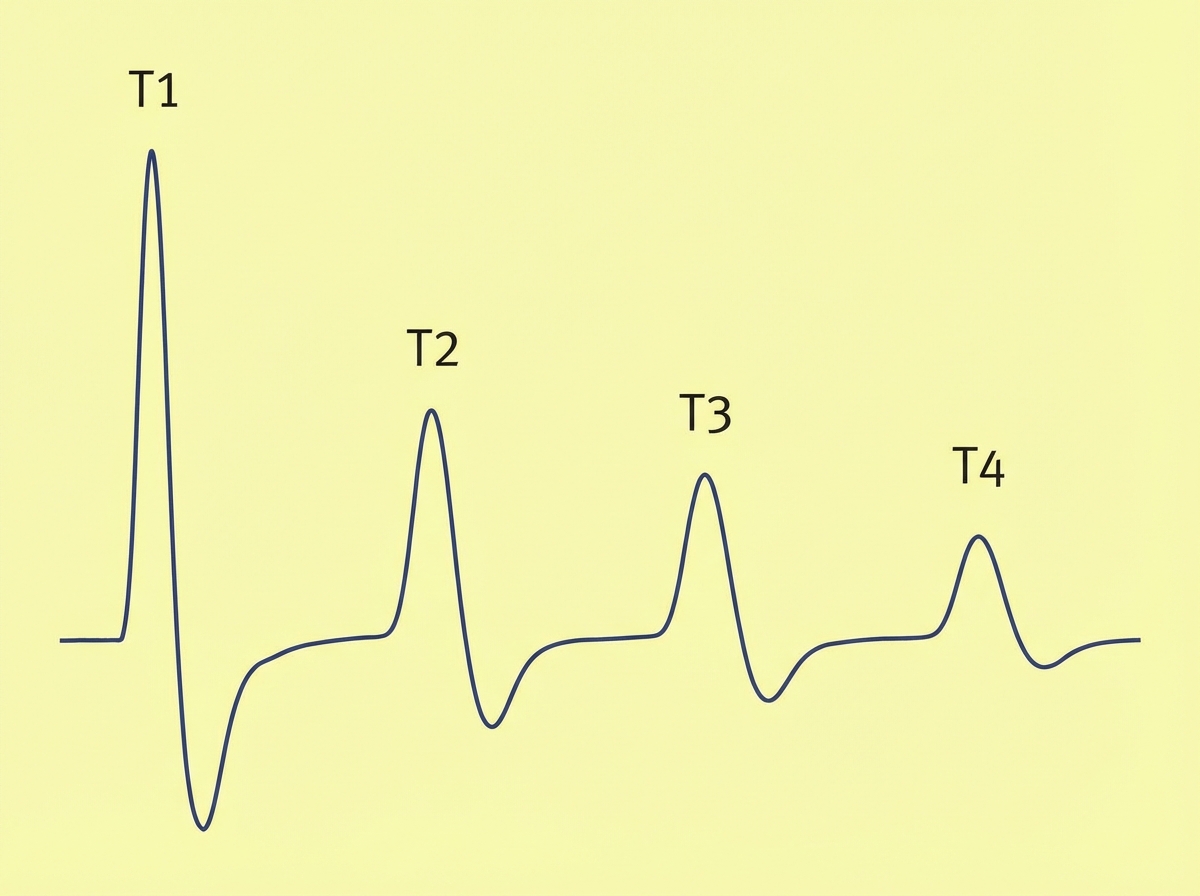
A 37-year-old woman undergoes diagnostic laparoscopy under general anesthesia for evaluation of chronic pelvic pain. Postoperatively, the patient requires prolonged intubation. Neostigmine is administered. Results of acceleromyography during train-of-four ulnar nerve stimulation are shown. Which of the following drugs is most likely to have been used intraoperatively in this patient?
A 56-year-old man comes to the physician because of a painless blistering rash on his hands, forearms, and face for 2 weeks. The rash is not itchy and seems to get worse in the sunlight. He has also noticed that his urine is darker than usual. His aunt and sister have a history of similar skin lesions. Examination of the skin shows multiple fluid-filled blisters and oozing erosions on the forearms, dorsal side of both hands, and forehead. There are areas of hyperpigmented scarring and patches of bald skin along the sides of the blisters. Which of the following is the most appropriate pharmacotherapy to treat this patient's condition?
A 57-year-old man presents to his family physician for a checkup. He has had type 2 diabetes mellitus for 13 years, for which he has been taking metformin and vildagliptin. He has smoked 10–15 cigarettes daily for 29 years. Family history is irrelevant. Vital signs include: temperature 36.6°C (97.8°F), blood pressure 152/87 mm Hg and pulse 88/min. Examination reveals moderate abdominal obesity with a body mass index of 32 kg/m². The remainder of the examination is unremarkable. His fasting lipid profile is shown: Total cholesterol (TC) 280 mg/dL Low-density lipoprotein (LDL)-cholesterol 210 mg/dL High-density lipoprotein (HDL)-cholesterol 40 mg/dL Triglycerides (TGs) 230 mg/dL Which of the following is the mechanism of action of the best initial therapy for this patient?
A 56-year-old man presents for a follow-up regarding his management for type 2 diabetes mellitus (DM). He was diagnosed with type 2 DM about 7 years ago and was recently started on insulin therapy because oral agents were insufficient to control his glucose levels. He is currently following a regimen combining insulin lispro and neutral protamine Hagedorn (NPH) insulin. He is taking insulin lispro 3 times a day before meals and NPH insulin once in the morning. He has been on this regimen for about 2 months. He says that his glucose reading at night averages around 200 mg/dL and remains close to 180 mg/dL before his shot of NPH in the morning. The readings during the rest of the day range between 100–120 mg/dL. The patient denies any changes in vision or tingling or numbness in his hands or feet. His latest HbA1C level was 6.2%. Which of the following adjustments to his insulin regimen would be most effective in helping this patient achieve better glycemic control?
A 52-year-old man who was recently hospitalized with a pulmonary embolism is put on an unfractionated heparin drip as a bridge to chronic warfarin therapy. During morning rounds, he is found to have diffuse bruising despite minimal trauma, and his heparin infusion rate is found to be faster than prescribed. A coagulation panel is obtained, which shows a aPTT of 130 seconds (therapeutic 70-120 seconds), and the decision is made to reverse the effects of heparin. Which of the following would most likely be administered in order to do this?
Background: Beta-blockers reduce mortality in patients who have chronic heart failure, systolic dysfunction, and are on background treatment with diuretics and angiotensin-converting enzyme inhibitors. We aimed to compare the effects of carvedilol and metoprolol on clinical outcome. Methods: In a multicenter, double-blind, and randomized parallel group trial, we assigned 1,511 patients with chronic heart failure to treatment with carvedilol (target dose 25 mg twice daily) and 1,518 to metoprolol (metoprolol tartrate, target dose 50 mg twice daily). Patients were required to have chronic heart failure (NYHA II-IV), previous admission for a cardiovascular reason, an ejection fraction of less than 0.35, and to have been treated optimally with diuretics and angiotensin-converting enzyme inhibitors unless not tolerated. The primary endpoints were all-cause mortality, the composite endpoint of all-cause mortality, or all-cause admission. Analysis was done by intention to treat Findings: The mean study duration was 58 months (SD 6). The mean ejection fraction was 0.26 (0.07) and the mean age was 62 years (11). The all-cause mortality was 34% (512 of 1,511) for carvedilol and 40% (600 of 1,518) for metoprolol (hazard ratio 0.83 [95% CI 0.74-0.93], p = 0.0017). The reduction of all-cause mortality was consistent across predefined subgroups. Incidence of side effects and drug withdrawals did not differ by much between the 2 study groups. Which of the following represents the number of patients needed to treat to save one life?
A 56-year-old man presents with sudden-onset severe eye pain and blurred vision. He says the symptoms onset an hour ago and his vision has progressively worsened. Physical examination reveals a cloudy cornea and decreased visual acuity. Timolol is administered into the eyes to treat this patient’s symptoms. Which of the following best describes the mechanism of action of this drug in the treatment of this patient’s condition?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
