Autonomic/CV Drugs — MCQs

On this page
A 52-year-old man is seen by his endocrinologist for routine followup of his type 2 diabetes. Although he has previously been on a number of medication regimens, his A1C has remained significantly elevated. In order to try to better control his glucose level, the endocrinologist prescribes a new medication. He explains that this new medication works by blocking the ability of his kidneys to reabsorb glucose and therefore causes glucose wasting in the urine. Which of the following medications has this mechanism of action?
A 25-year-old woman presents to her college campus clinic with the complaint of being unable to get up for her morning classes. She says that, because of this, her grades are being affected. For the past 6 weeks, she says she has been feeling depressed because her boyfriend dumped her. She finds herself very sleepy, sleeping in most mornings, eating more snacks and fast foods, and feeling drained of energy. She is comforted by her friend’s efforts to cheer her up but still feels guarded around any other boy that shows interest in her. The patient says she had similar symptoms 7 years ago for which she was prescribed several selective serotonin reuptake inhibitors (SSRIs) and a tricyclic antidepressant (TCA). However, none of the medications provided any long-term relief. She has prescribed a trial of Phenelzine to treat her symptoms. Past medical history is significant for a long-standing seizure disorder well managed with phenytoin. Which of the following statements would most likely be relevant to this patient’s new medication?
A 54-year-old male has a history of gout complicated by several prior episodes of acute gouty arthritis and 3 prior instances of nephrolithiasis secondary to uric acid stones. He has a serum uric acid level of 11 mg/dL (normal range 3-8 mg/dL), a 24 hr urine collection of 1300 mg uric acid (normal range 250-750 mg), and a serum creatinine of 0.8 mg/dL with a normal estimated glomerular filtration rate (GFR). Which of the following drugs should be avoided in this patient?
A 28-year-old woman has a follow-up visit with her physician. She was diagnosed with allergic rhinitis and bronchial asthma at 11 years of age. Her regular controller medications include daily high-dose inhaled corticosteroids and montelukast, but she still needs to use a rescue inhaler 3–4 times a week following exercise. She also becomes breathless with moderate exertion. After a thorough evaluation, the physician explains that her medication dosages need to be increased. She declines taking oral corticosteroids daily due to concerns about side effects. The physician prescribes omalizumab, which is administered subcutaneously every 3 weeks. Which of the following best explains the mechanism of action of the new medication that has been added to the controller medications?
A 34-year-old man was brought into the emergency room after he was found running in the streets. Upon arrival to the emergency room, he keeps screaming, “they are eating me alive," and swatting his hands. He reports that there are spiders crawling all over him. His girlfriend, who arrives shortly after, claims that he has been forgetful and would forget his keys from time to time. He denies weight loss, fever, shortness of breath, abdominal pain, or urinary changes but endorses chest pain. His temperature is 98.9°F (37.2°C), blood pressure is 160/110 mmHg, pulse is 112/min, respirations are 15/min, and oxygen saturation is 98%. He becomes increasingly agitated as he believes the healthcare providers are trying to sacrifice him to the “spider gods.” What is the most likely explanation for this patient’s symptoms?
A 53-year-old man presents with swelling of the right knee. He says that the pain began the previous night and was reduced by ibuprofen and an ice-pack. The pain persists but is tolerable. He denies any recent fever, chills, or joint pains in the past. Past medical history includes a coronary artery bypass graft (CABG) a year ago for which he takes aspirin, atorvastatin, captopril, and carvedilol. The patient reports a 20-pack-year history of smoking but quit 5 years ago. He also says he was a heavy drinker for the past 30 years but now drinks only a few drinks on the weekends. On physical examination, the right knee is erythematous, warm, swollen, and mildly tender to palpation. Cardiac exam is significant for a mild systolic ejection murmur. The remainder of the examination is unremarkable. Arthrocentesis of the right knee joint is performed, which reveals the presence of urate crystals. Which of the following medications is most likely responsible for this patient's symptoms?
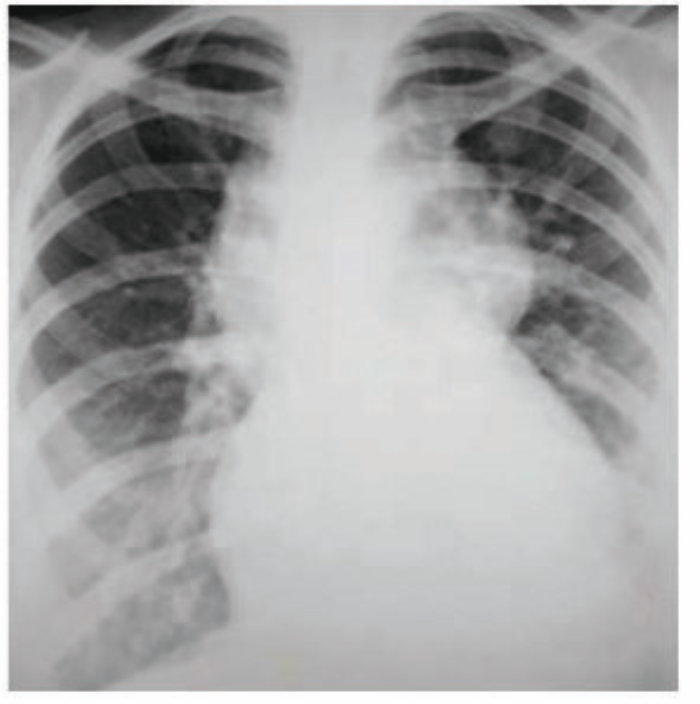
A 27-year-old healthy college student presents to the clinic with her boyfriend complaining of a productive cough with rust-colored sputum associated with breathlessness for the past week. She also reports symptoms of the common cold which began about 1 week ago. She reports that her weekly routine has not changed despite feelings of being sick and generally weak. The vitals signs include a blood pressure 120/80 mm Hg, pulse rate 68/min, respiratory rate 12/min, and temperature 36.6°C (97.9°F). On pulmonary examination, inspiratory crackles were heard. The cardiac examination revealed an S3 sound but was otherwise normal. A chest X-ray was performed and is shown in the picture below. What medication is known to be associated with the same condition that she is suffering from?
A 42-year-old woman comes to the physician for evaluation of a 6-month history of irregular menstrual periods. Her last period was 3 months ago. Previously, her periods occurred at regular 28-day intervals and lasted 4–5 days with moderate flow. She has also noticed breast tenderness and scant nipple discharge. She has type 2 diabetes mellitus and refractory bipolar I disorder. Current medications include metformin, glipizide, lithium, and risperidone. Physical examination shows no abnormalities. A urine pregnancy test is negative. Which of the following is the most likely cause of the changes in her menstrual cycle?
A 65-year-old gentleman presents to his primary care physician for difficulties with his gait and recent fatigue. The patient works in a health food store, follows a strict vegan diet, and takes an array of supplements. He noticed that his symptoms have progressed over the past year and decided to see a physician when he found himself feeling abnormally weak on a daily basis in conjunction with his trouble walking. The patient has a past medical history of Crohn's disease, diagnosed in his early 20's, as well as Celiac disease. He states that he has infrequent exacerbations of his Crohn's disease. Recently, the patient has been having worsening bouts of diarrhea that the patient claims is non-bloody. The patient is not currently taking any medications and is currently taking traditional Chinese medicine supplements. Physical exam is notable for 3/5 strength in the upper and lower extremities, absent upper and lower extremity reflexes, and a staggering, unbalanced gait. Laboratory values reveal the following: Serum: Na+: 135 mEq/L Cl-: 100 mEq/L K+: 5.6 mEq/L HCO3-: 22 mEq/L BUN: 27 mg/dL Glucose: 79 mg/dL Creatinine: 1.1 mg/dL Ca2+: 8.4 mg/dL Mg2+: 1.5 mEq/L Leukocyte count and differential: Leukocyte count: 4,522/mm^3 Hemoglobin: 9.2 g/dL Hematocrit: 29% Platelet count: 169,000/mm^3 Reticulocyte count: 2.5% Lactate dehydrogenase: 340 U/L Mean corpuscular volume: 97 fL Which of the following is most likely deficient in this patient?
A 55-year-old woman comes to the clinic complaining of joint pain and stiffness for the past year. The pain is mainly concentrated in her hands and is usually worse towards the late afternoon. It is described with a burning quality that surrounds the joint with some numbness and tingling. The stiffness is especially worse in the morning and lasts approximately for 15-20 minutes. Her past medical history is significant for recurrent gastric ulcers. She reports that her mother struggled with lupus and is concerned that she might have the same thing. She denies fever, rashes, ulcers, genitourinary symptoms, weight loss, or bowel changes. Physical examination is significant for mild tenderness at the distal interphalangeal joints bilaterally. What is the best initial medication to prescribe to this patient?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
