Autonomic/CV Drugs — MCQs

On this page
A 70-year-old woman with history of coronary artery disease status-post coronary artery bypass graft presents with a stroke due to an infarction in the right middle cerebral artery territory. She is admitted to the intensive care unit for neurological monitoring following a successful thrombectomy. Overnight, the patient complains of difficulty breathing, chest pain, and jaw pain. Her temperature is 98.6°F (37°C), blood pressure is 160/80 mmHg, pulse is 100/min, respirations are 30/min, and oxygen saturation is 90% on 2L O2 via nasal cannula. Rales are heard in the lower lung bases. Electrocardiogram reveals left ventricular hypertrophy with repolarization but no acute ST or T wave changes. Troponin is 2.8 ng/mL. Chest radiograph reveals Kerley B lines. After administration of oxygen, aspirin, carvedilol, and furosemide, the patient improves. The next troponin is 3.9 ng/mL. Upon further discussion with the consulting cardiologist and neurologist, a heparin infusion is started. After transfer to a general medicine ward floor four days later, the patient complains of a headache. The patient's laboratory results are notable for the following: Hemoglobin: 11 g/dL Hematocrit: 36% Leukocyte count: 11,000 /mm^3 with normal differential Platelet count: 130,000 /mm^3 On admission, the patient's platelet count was 300,000/mm^3. What medication is appropriate at this time?
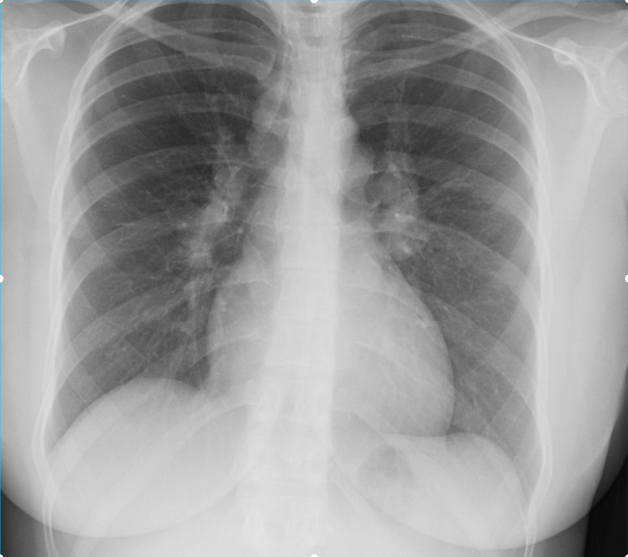
A 26-year-old man comes to the physician because of a 1-week history of left-sided chest pain. The pain is worse when he takes deep breaths. Over the past 6 weeks, he had been training daily for an upcoming hockey tournament. He does not smoke cigarettes or drink alcohol but has used cocaine once. His temperature is 37.1°C (98.7°F), pulse is 75/min, and blood pressure is 128/85 mm Hg. Physical examination shows tenderness to palpation of the left chest. An x-ray of the chest is shown. Which of the following is the most appropriate initial pharmacotherapy?
A 55-year-old man presents to the emergency department with shortness of breath and weakness. Past medical history includes coronary artery disease, arterial hypertension, and chronic heart failure. He reports that the symptoms started around 2 weeks ago and have been gradually worsening. His temperature is 36.5°C (97.7°F), blood pressure is 135/90 mm Hg, heart rate is 95/min, respiratory rate is 24/min, and oxygen saturation is 94% on room air. On examination, mild jugular venous distention is noted. Auscultation reveals bilateral loud crackles. Pitting edema of the lower extremities is noted symmetrically. His plasma brain natriuretic peptide level on rapid bedside assay is 500 pg/mL (reference range < 125 pg/mL). A chest X-ray shows enlarged cardiac silhouette. He is diagnosed with acute on chronic left heart failure with pulmonary edema and receives immediate care with furosemide. The physician proposes a drug trial with a new BNP stabilizing agent. Which of the following changes below are expected to happen if the patient is enrolled in this trial?
A 13-year-old boy is brought to the emergency room by his mother for a generalized tonic-clonic seizure that occurred while attending a laser light show. His mother says that he has been otherwise healthy but “he often daydreams”. Over the past several months, he has reported recurrent episodes of jerky movements of his fingers and arms. These episodes usually occurred shortly after waking up in the morning. He has not lost consciousness during these episodes. Which of the following is the most appropriate treatment for this patient's condition?
A 25-year-old G1P1 with a history of diabetes and epilepsy gives birth to a female infant at 32 weeks gestation. The mother had no prenatal care and took no prenatal vitamins. The child's temperature is 98.6°F (37°C), blood pressure is 100/70 mmHg, pulse is 130/min, and respirations are 25/min. On physical examination in the delivery room, the child's skin is pink throughout and she cries on stimulation. All four extremities are moving spontaneously. A tuft of hair is found overlying the infant's lumbosacral region. Which of the following medications was this patient most likely taking during her pregnancy?
A 50-year-old man presents to the office with the complaint of pain in his left great toe. The pain started 2 days ago and has been progressively getting worse to the point that it is difficult to walk even a few steps. He adds that his left big toe is swollen and hot to the touch. He has never had similar symptoms in the past. He normally drinks 2–3 cans of beer every night but recently binge drank 3 nights ago. Physical examination is notable for an overweight gentleman (BMI of 35) in moderate pain, with an erythematous, swollen, and exquisitely tender left great toe. Laboratory results reveal a uric acid level of 9 mg/dL. A complete blood count shows: Hemoglobin % 12 gm/dL Hematocrit 45% Mean corpuscular volume (MCV) 90 fL Platelets 160,000/mm3 Leukocytes 8,000/mm3 Segmented neutrophils 65% Lymphocytes 25% Eosinophils 3% Monocytes 7% RBCs 5.6 million/mm3 Synovial fluid analysis shows: Cell count 55,000 cells/mm3 (80% neutrophils) Crystals negatively birefringent crystals present Culture pending Gram stain no organisms seen Which of the following is the mechanism of action of the drug that will most likely be used in the long-term management of this patient?
A 55-year-old man comes to the physician because of a 4-month history of fatigue, increased sweating, and a 5.4-kg (12-lb) weight loss. Over the past 3 weeks, he has had gingival bleeding when brushing his teeth. Twenty years ago, he was diagnosed with a testicular tumor and treated with radiation therapy. His temperature is 37.8°C (100°F), pulse is 70/min, respirations are 12/min, and blood pressure is 130/80 mm Hg. He takes no medications. Cardiopulmonary examination shows no abnormalities. The spleen is palpated 4 cm below the left costal margin. Laboratory studies show: Hemoglobin 9 g/dL Mean corpuscular volume 86 μm3 Leukocyte count 110,000/mm3 Segmented neutrophils 24% Metamyelocytes 6% Myelocytes 34% Promyelocytes 14% Blasts 1% Lymphocytes 11% Monocytes 4% Eosinophils 4% Basophils 2% Platelet count 650,000/mm3 Molecular testing confirms the diagnosis. Which of the following is the most appropriate next step in treatment?
A 72-year-old woman with a history of atrial fibrillation on warfarin, diabetes, seizure disorder and recent MRSA infection is admitted to the hospital. She subsequently begins therapy with another drug and is found to have a supratherapeutic International Normalized Ratio (INR). Which of the following drugs is likely contributing to this patient's elevated INR?
A 42-year-old man presents to his family physician for evaluation of oral pain. He states that he has increasing pain in a molar on the top left of his mouth. The pain started 1 week ago and has been progressively worsening since then. His medical history is significant for hypertension and type 2 diabetes mellitus, both of which are currently controlled with lifestyle modifications. His blood pressure is 124/86 mm Hg, heart rate is 86/min, and respiratory rate is 14/min. Physical examination is notable for a yellow-black discoloration of the second molar on his left upper mouth. The decision is made to refer him to a dentist for further management of this cavity. The patient has never had any dental procedures and is nervous about what type of sedation will be used. Which of the following forms of anesthesia utilizes solely an oral or intravenous anti-anxiety medication?
A 23-year-old male presents with complaints of polydipsia and frequent, large-volume urination. Laboratory testing does not demonstrate any evidence of diabetes; however, a reduced urine osmolality of 120 mOsm/L is measured. Which of the following findings on a desmopressin test would be most consistent with a diagnosis of central diabetes insipidus?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
