Autonomic/CV Drugs — MCQs

On this page
A 59-year-old healthy woman presents to her primary care physician’s office six weeks after undergoing an elective breast augmentation procedure in the Dominican Republic. She was told by her surgeon to establish post-operative care once back in the United States. Today she is bothered by nausea and early satiety. Her past medical history is significant only for GERD for which she takes ranitidine. Since the surgery, she has also taken an unknown opioid pain medication that was given to her by the surgeon. She reports that she has been taking approximately ten pills a day. On examination she is afebrile with normal vital signs and her surgical incisions are healing well. Her abdomen is distended and tympanitic. The patient refuses to stop her pain medicine and laxatives are not effective; what medication could be prescribed to ameliorate her gastrointestinal symptoms?
A 68-year-old man comes to the emergency department 12 hours after the appearance of tender, purple discolorations on his thighs and lower abdomen. He began taking a medication 4 days ago after failed cardioversion for atrial fibrillation, but he cannot remember the name. Physical examination shows a tender bluish-black discoloration on the anterior abdominal wall. A photograph of the right thigh is shown. Which of the following is the most likely explanation for this patient's skin findings?
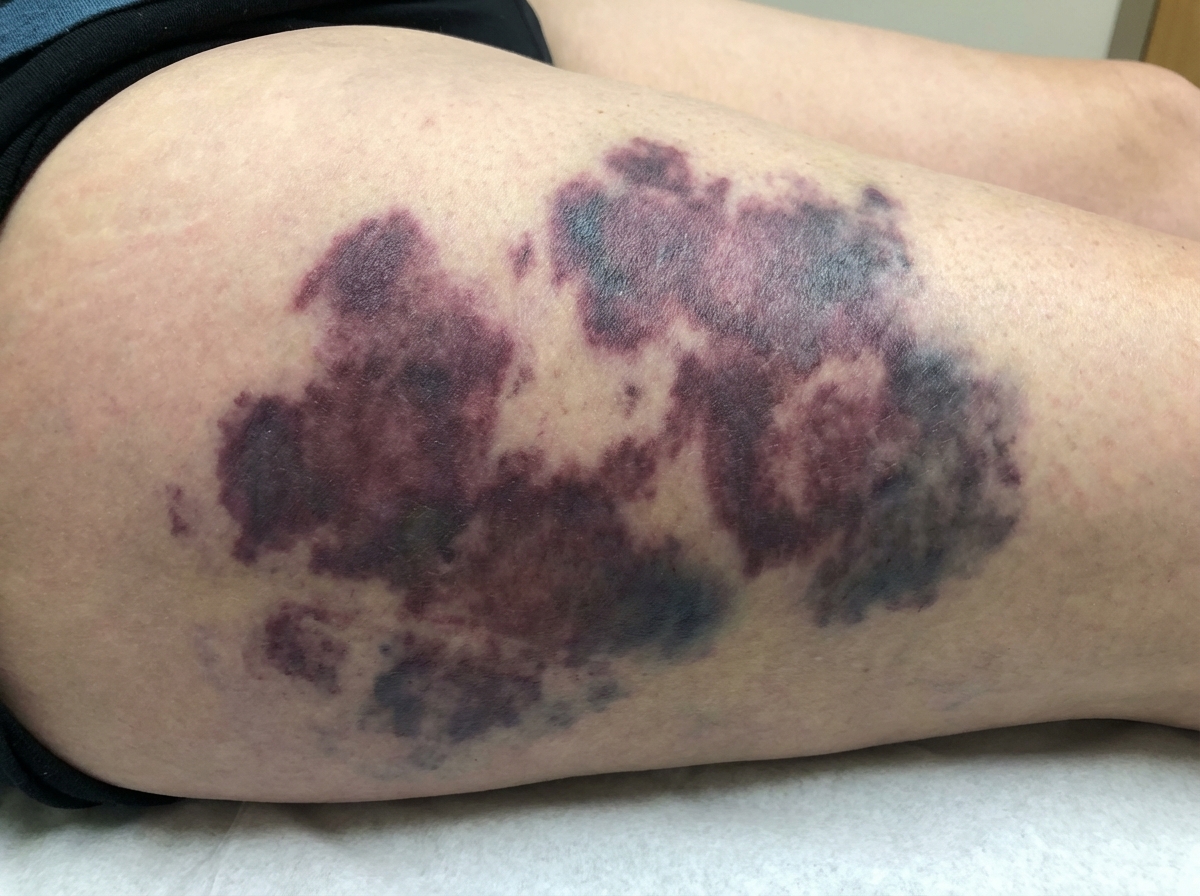
A 35-year-old female presents to her primary care physician complaining of right upper quadrant pain over the last 6 months. Pain is worst after eating and feels like intermittent squeezing. She also admits to lighter colored stools and a feeling of itchiness on her skin. Physical exam demonstrates a positive Murphy's sign. The vitamin level least likely to be affected by this condition is associated with which of the following deficiency syndromes?
A 59-year-old male with a 1-year history of bilateral knee arthritis presents with epigastric pain that intensifies with meals. He has been self-medicating with aspirin, taking up to 2,000 mg per day for the past six months. Which of the following medications, if taken instead of aspirin, could have minimized his risk of experiencing this epigastric pain?
A 62-year-old man presents to his primary care provider complaining of leg pain with exertion for the past 6 months. He notices that he has bilateral calf cramping with walking. He states that it is worse in his right calf than in his left, and it goes away when he stops walking. He has also noticed that his symptoms are progressing and that this pain is occurring sooner than before. His medical history is remarkable for type 2 diabetes mellitus and 30-pack-year smoking history. His ankle-brachial index (ABI) is found to be 0.80. Which of the following can be used as initial therapy for this patient's condition?
A 26-year-old G1P0 woman is brought to the emergency room by her spouse for persistently erratic behavior. Her spouse reports that she has been sleeping > 1 hour a night, and it sometimes seems like she’s talking to herself. She has maxed out their credit cards on baby clothes. The patient’s spouse reports this has been going on for over a month. Since first seeing a physician, she has been prescribed multiple first and second generation antipsychotics, but the patient’s spouse reports that her behavior has failed to improve. Upon examination, the patient is speaking rapidly and occasionally gets up to pace the room. She reports she is doing “amazing,” and that she is “so excited for the baby to get here because I’m going to be the best mom.” She denies illicit drug use, audiovisual hallucinations, or suicidal ideation. The attending psychiatrist prescribes a class of medication the patient has not yet tried to treat the patient’s psychiatric condition. In terms of this new medication, which of the following is the patient’s newborn most likely at increased risk for?
A 27-year-old man presents to the emergency department for bizarre behavior. The patient had boarded up his house and had been refusing to leave for several weeks. The police were called when a foul odor emanated from his property prompting his neighbors to contact the authorities. Upon questioning, the patient states that he has been pursued by elves for his entire life. He states that he was tired of living in fear, so he decided to lock himself in his house. The patient is poorly kempt and has very poor dentition. The patient has a past medical history of schizophrenia which was previously well controlled with olanzapine. The patient is restarted on olanzapine and monitored over the next several days. Which of the following needs to be monitored long term in this patient?
A 53-year-old man is brought to the emergency department because of wheezing and shortness of breath that began 1 hour after he took a new medication. Earlier in the day he was diagnosed with stable angina pectoris and prescribed a drug that irreversibly inhibits cyclooxygenase-1 and 2. He has chronic rhinosinusitis and asthma treated with inhaled β-adrenergic agonists and corticosteroids. His respirations are 26/min. Examination shows multiple small, erythematous nasal mucosal lesions. After the patient is stabilized, therapy for primary prevention of coronary artery disease should be switched to a drug with which of the following mechanisms of action?
A 37-year-old man presents with back pain which began 3 days ago when he was lifting heavy boxes. The pain radiates from the right hip to the back of the thigh. The pain is exacerbated when he bends at the waist. He rates the severity of the pain as 6 out of 10. The patient has asthma and mitral insufficiency due to untreated rheumatic fever in childhood. He has a smoking history of 40 pack-years. His family history is remarkable for rheumatoid arthritis, diabetes, and hypertension. Vital signs are within normal limits. On physical examination, the pain is elicited when the patient is asked to raise his leg without extending his knee. The patient has difficulty walking on his heels. Peripheral pulses are equal and brisk bilaterally. No hair loss, temperature changes, or evidence of peripheral vascular disease is observed. Which of the following is considered the best management option for this patient?
A 17-year-old white male is brought to the emergency department after being struck by a car. He complains of pain in his right leg and left wrist, and slowly recounts how he was hit by a car while being chased by a lion. In between sentences of the story, he repeatedly complains of dry mouth and severe hunger and requests something to eat and drink. His mother arrives and is very concerned about this behavior, noting that he has been withdrawn lately and doing very poorly in school the past several months. Notable findings on physical exam include conjunctival injection bilaterally and a pulse of 107. What drug is this patient most likely currently abusing?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
