Autonomic/CV Drugs — MCQs

On this page
A 57-year-old woman with a history of diabetes and hypertension accidentally overdoses on antiarrhythmic medication. Upon arrival in the ER, she is administered a drug to counteract the effects of the overdose. Which of the following matches an antiarrhythmic with its correct treatment in overdose?
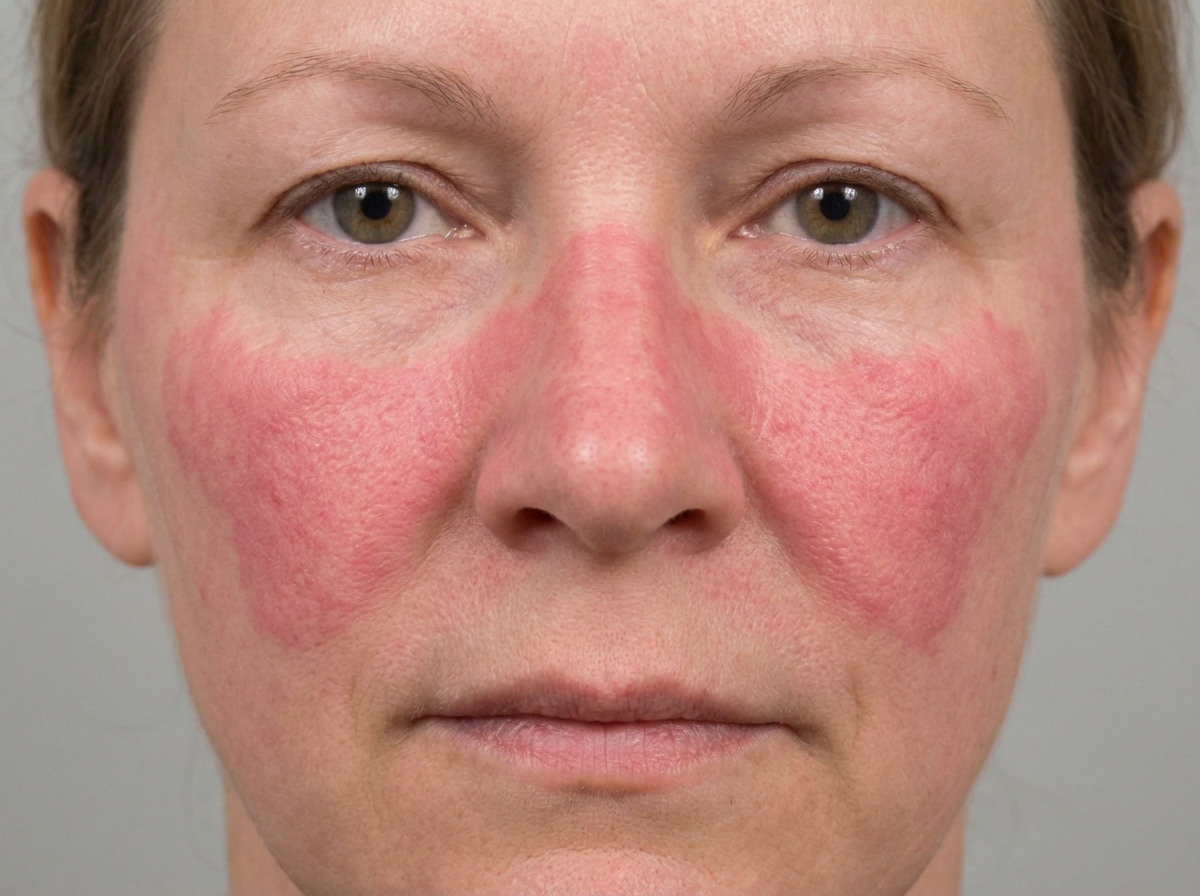
A 20-year-old woman presents with shortness of breath and chest pain for 1 week. She says the chest pain is severe, sharp in character, and aggravated upon deep breathing. She says she becomes short of breath while walking upstairs in her home or with any type of exertion. She says she frequently feels feverish and fatigued. No significant past medical history and no current medications. Review of systems is significant for a weight loss of 4.5 kg (10.0 lb) over the past month and joint pain in her wrists, hands, and knees. Vital signs are within normal limits. On physical examination, there is a pink rash over her face which is aggravated by sunlight (shown in the image). There are decreased breath sounds on the right. A chest radiograph reveals evidence of a right-sided pleural effusion. Routine urinalysis and urine dipstick are normal. Serum antinuclear antibody (ANA) and anti-double-stranded DNA levels are positive. The patient is started on prednisone therapy and 2 weeks later her CBC is obtained and compared to the one on admission: On admission Leukocytes 8,000/mm3 Neutrophils 60% Lymphocytes 23% Eosinophils 2% Basophils 1% Monocyte 5% Hemoglobin 10 g/dL Creatinine 0.8 mg/dL BUN 15 mg/dL 2 weeks later Leukocytes 13,000/mm3 Neutrophils 90% Lymphocytes 8% Eosinophils 0% Basophils 0% Monocyte 1% Hemoglobin 12g/dL Creatinine 0.8 mg/dL BUN 15 mg/dL Which of the following best describes the most likely mechanism that accounts for the difference between these 2 complete blood counts (CBCs)?
A 14-year-old boy has undergone kidney transplantation due to stage V chronic kidney disease. A pre-transplantation serologic assessment showed that he is negative for past or present HIV infection, viral hepatitis, EBV, and CMV infection. He has a known allergy for macrolides. The patient has no complaints 1 day after transplantation. His vital signs include: blood pressure 120/70 mm Hg, heart rate 89/min, respiratory rate 17/min, and temperature 37.0°C (98.6°F). On physical examination, the patient appears to be pale, his lungs are clear on auscultation, heart sounds are normal, and his abdomen is non-tender on palpation. His creatinine is 0.65 mg/dL (57.5 µmol/L), GFR is 71.3 mL/min/1.73 m2, and urine output is 0.9 mL/kg/h. Which of the following drugs should be used in the immunosuppressive regimen in this patient?
A 10-year-old boy presents to the emergency department with a swollen and painful elbow after accidentally bumping his arm into the kitchen table. His mom notes that he seems to bruise and bleed easily, but this is the first time he has had a swollen joint. She also remembers that her uncle had a bleeding disorder, but cannot remember the diagnosis. Physical exam reveals a warm and tender elbow joint, but is otherwise unremarkable. Based on clinical suspicion, a bleeding panel is ordered with the following findings: Bleeding time: 3 minutes Prothrombin time (PT): 13 seconds Partial thromboplastin time (PTT): 54 seconds Which of the following treatments would most likely be effective in preventing further bleeding episodes for this patient?
A 45-year-old woman, suspected of having colon cancer, is advised to undergo a contrast-CT scan of the abdomen. She has no comorbidities and no significant past medical history. There is also no history of drug allergy. However, she reports that she is allergic to certain kinds of seafood. After tests confirm normal renal function, she is taken to the CT scan room where radiocontrast dye is injected intravenously and a CT scan of her abdomen is conducted. While being transferred to her ward, she develops generalized itching and urticarial rashes, with facial angioedema. She becomes dyspneic. Her pulse is 110/min, the blood pressure is 80/50 mm Hg, and the respirations are 30/min. Her upper and lower extremities are pink and warm. What is the most appropriate management of this patient?
A 60-year-old man comes to the emergency room for a persistent painful erection for the last 5 hours. He has a history of sickle cell trait, osteoarthritis, insomnia, social anxiety disorder, gout, type 2 diabetes mellitus, major depressive disorder, and hypertension. He drinks 1 can of beer daily, and smokes marijuana on the weekends. He takes propranolol, citalopram, trazodone, allopurinol, metformin, glyburide, lisinopril, and occasionally ibuprofen. He is alert and oriented but in acute distress. Temperature is 36.5°C(97.7°F), pulse is 105/min, and blood pressure is 145/95 mm Hg. Examination shows a rigid erection with no evidence of trauma, penile discharge, injection, or prosthesis. Which of the following is the most likely cause of his condition?
A 56-year-old man comes to the physician for a follow-up examination. One month ago, he was diagnosed with a focal seizure and treatment with a drug that blocks voltage-gated sodium channels was begun. Today, he reports that he has not had any abnormal body movements, but he has noticed occasional double vision. His serum sodium is 132 mEq/L, alanine aminotransferase is 49 U/L, and aspartate aminotransferase is 46 U/L. This patient has most likely been taking which of the following drugs?
A 22-year-old woman comes to the physician to discuss the prescription of an oral contraceptive. She has no history of major medical illness and takes no medications. She does not smoke cigarettes. She is sexually active with her boyfriend and has been using condoms for contraception. Physical examination shows no abnormalities. She is prescribed combined levonorgestrel and ethinylestradiol tablets. Which of the following is the most important mechanism of action of this drug in the prevention of pregnancy?
A 64-year-old woman presents to the clinic with a history of 3 fractures in the past year with the last one being last month. Her bone-density screening from last year reported a T-score of -3.1 and she was diagnosed with osteoporosis. She was advised to quit smoking and was asked to adapt to a healthy lifestyle to which she complied. She was also given calcium and vitamin D supplements. After a detailed discussion with the patient, the physician decides to start her on weekly alendronate. Which of the following statements best describes this patient’s new therapy?
A 7-year-old boy presents to an urgent care clinic from his friend’s birthday party after experiencing trouble breathing. His father explains that the patient had eaten peanut butter at the party, and soon after, he developed facial flushing and began scratching his face and neck. This has never happened before but his father says that they have avoided peanuts and peanut butter in the past because they were worried about their son having an allergic reaction. The patient has no significant medical history and takes no medications. His blood pressure is 94/62 mm Hg, heart rate is 125/min, and respiratory rate is 22/min. On physical examination, his lips are edematous and he has severe audible stridor. Of the following, which type of hypersensitivity reaction is this patient experiencing?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
