Autonomic/CV Drugs — MCQs

On this page
A 24-year-old woman comes to the physician because of excessive hair growth. She has noticed increasing numbers of dark hairs on her upper lip and on her abdomen over the past 8 years. Menarche was at the age of 13 years. Menses occur at regular 28-day intervals and last 5–6 days with moderate flow. She is sexually active with one male partner. Her only medication is a combination oral contraceptive. She is 168 cm (5 ft 6 in) tall and weighs 88 kg (193 lb); BMI is 31 kg/m2. Vital signs are within normal limits. Physical examination shows coarse dark hair on the upper lip and periumbilical and periareolar skin. Her external genitalia appear normal. The remainder of the examination shows no abnormalities. Midcycle serum studies show: Fasting glucose 95 mg/dL Dehydroepiandrosterone sulfate 3.1 μg/mL (N = 0.5–5.4) Luteinizing hormone 95 mIU/mL Follicle-stimulating hormone 75 mIU/mL 17α-Hydroxyprogesterone 190 ng/dL (N = 20–300) Testosterone 1.1 nmol/L (N < 3.5) Dihydrotestosterone 435 pg/mL (N < 300) A urine pregnancy test is negative. Which of the following is the most likely underlying cause of this patient's symptom?
A 14-year-old female with no past medical history presents to the emergency department with nausea and abdominal pain. On physical examination, her blood pressure is 78/65, her respiratory rate is 30, her breath has a fruity odor, and capillary refill is > 3 seconds. Serum glucose is 820 mg/dL. After starting IV fluids, what is the next best step in the management of this patient?
A 52-year-old man comes to the physician because of increasing weakness of his arms and legs over the past year. He has also had difficulty speaking for the past 5 months. He underwent a partial gastrectomy for gastric cancer 10 years ago. His temperature is 37.1°C (98.8°F), pulse is 88/min, and blood pressure is 118/70 mm Hg. Examination shows dysarthria. There is mild atrophy and twitching of the tongue. Muscle strength is decreased in all extremities. Muscle tone is decreased in the right lower extremity and increased in the other extremities. Deep tendon reflexes are absent in the right lower extremity and 4+ in the other extremities. Plantar reflex shows an extensor response on the left. Sensation is intact in all extremities. Which of the following is the most appropriate pharmacotherapy for this patient?
A 56-year-old man with substernal chest pain calls 911. When paramedics arrive, they administer drug X sublingually for the immediate relief of angina. What is the most likely site of action of drug X?
A 78-year-old woman with a history of cerebrovascular accident (CVA) presents to the emergency department with slurred speech, diplopia and dizziness that has persisted for eight hours. Upon further questioning you find that since her CVA one year ago, she has struggled with depression and poor nutrition. Her dose of paroxetine has been recently increased. Additionally, she is on anti-seizure prophylaxis due to sequelae from her CVA. CT scan reveals an old infarct with no acute pathology. Vital signs are within normal limits. On physical exam you find the patient appears frail. She is confused and has nystagmus and an ataxic gait. What would be an appropriate next step?
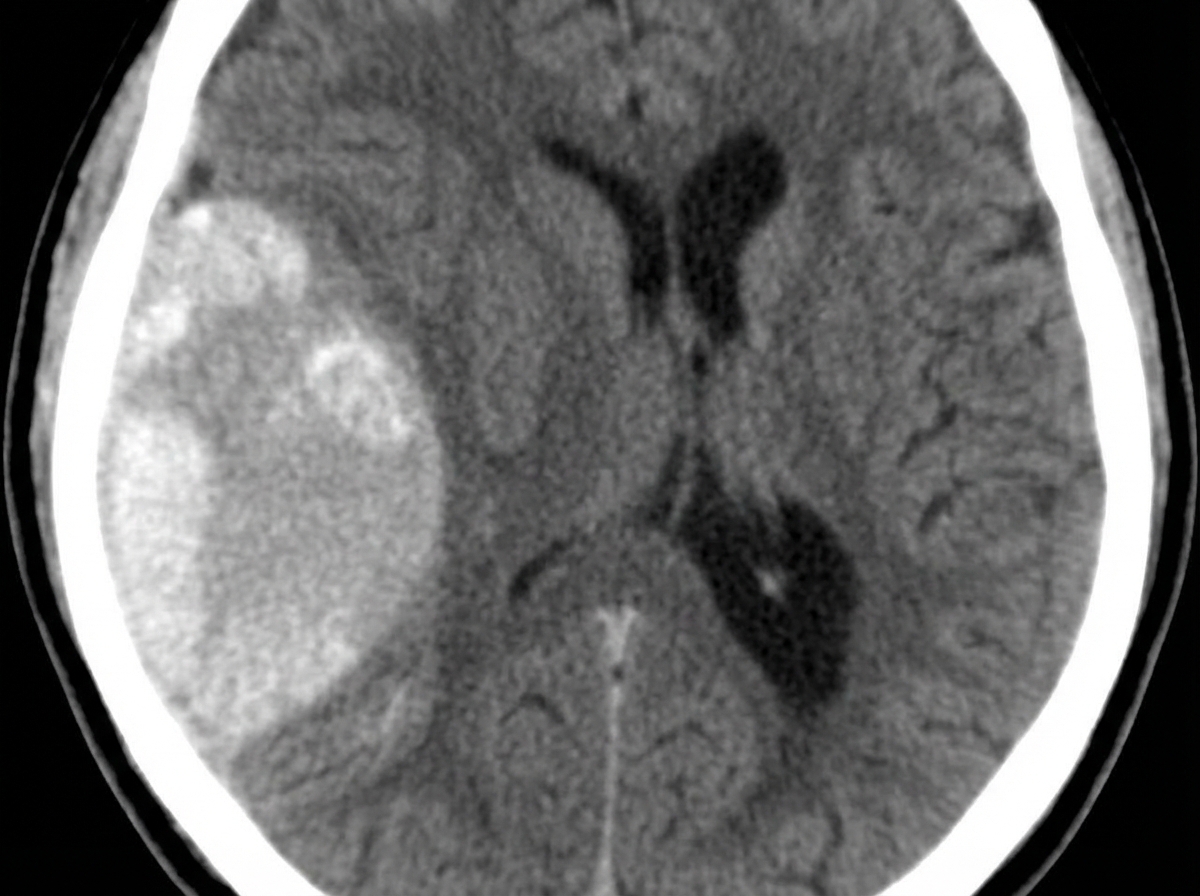
A 23-year-old man presents with a blunt force injury to the head from a baseball bat. He is currently unconscious, although his friends say he was awake and speaking with them en route to the hospital. He has no significant past medical history and takes no current medications. The vital signs include: temperature 37.0°C (98.6°F), blood pressure 165/85 mm Hg, pulse 50/min, and respiratory rate 19/min. On physical examination, there is a blunt force injury to the left temporoparietal region approximately 10.1–12.7 cm (4–5 in) in diameter. There is anisocoria of the left pupil, which is unresponsive to light. The patient is intubated and fluid resuscitation is initiated. A noncontrast computed tomography (CT) scan of the head is acquired and shown in the exhibit (see image). Which of the following is the most appropriate medical treatment for this patient?
A patient in a phase 1 trial for a novel epoxide reductase inhibitor, being studied for stroke prophylaxis, develops pain and erythema on the right thigh two days after starting the trial. This rapidly progresses to a purpuric rash with necrotic bullae within 24 hours. Lab results show a PTT of 29 seconds, PT of 28 seconds, and INR of 2.15. What is the most likely pathogenesis of this condition?
A 32-year-old man comes to the physician because of a 2-week history of diarrhea. During this period, he has had about 10 bowel movements per day. He states that his stools are light brown and watery, with no blood or mucus. He also reports mild abdominal pain and nausea. Over the past year, he has had 6 episodes of diarrhea that lasted several days and resolved spontaneously. Over this time, he also noticed frequent episodes of reddening in his face and neck. He returned from a 10-day trip to Nigeria 3 weeks ago. There is no personal or family history of serious illness. He has smoked a pack of cigarettes daily for the past 13 years. His temperature is 37°C (98.6°F), pulse is 110/min, and blood pressure is 100/60 mm Hg. Physical examination shows dry mucous membranes. The abdomen is tender with no rebound or guarding. The remainder of the examination shows no abnormalities. Serum studies show: Na+ 136 mEq/L Cl- 102 mEq/L K+ 2.3 mEq/L HCO3- 22 mEq/L Mg2+ 1.7 mEq/L Ca2+ 12.3 mg/dL Glucose (fasting) 169 mg/dL Nasogastric tube aspiration reveals significantly decreased gastric acid production. Which of the following is the most likely underlying cause of this patient's symptoms?
A 25-year-old man is rushed to the emergency department following a motor vehicle accident. After an initial evaluation, he is found to have bilateral femoral fractures. After surgical fixation of his fractures, he suddenly starts to feel nauseated and becomes agitated. Past medical history is significant for a thyroid disorder. His temperature is 40.0°C (104°F), blood pressure is 165/100 mm Hg, pulse is 170/min and irregularly irregular, and respirations are 20/min. On physical examination, the patient is confused and delirious. Oriented x 0. Laboratory studies are significant for the following: Thyroxine (T4), free 5 ng/dL Thyroid stimulating hormone (TSH) 0.001 mU/L The patient is started on propranolol to control his current symptoms. Which of the following best describes the mechanism of action of this new medication?
A 31-year-old man presents with a headache, myalgias, nausea, irritability, and forgetfulness. He developed these symptoms gradually over the past 3 months. He is a motor mechanic, and he changed his place of work 4 months ago. He smokes a half a pack of cigarettes per day. His vaccinations are up to date. On presentation, his vital signs are as follows: blood pressure is 145/70 mm Hg, heart rate is 94/min, respiratory rate is 17/min, and temperature is 36.8℃ (98.2℉). Physical examination reveals diffuse erythema of the face and chest and slight abdominal distention. Neurological examination shows symmetrical brisk upper and lower extremities reflexes. Blood tests show the following results: pH 7.31 Po2 301 mm Hg Pco2 28 mm Hg Na+ 141 mEq/L K+ 4.3 mEq/L Cl- 109 mEq/L HCO3- 17 mEq/L Base Excess -3 mEq/L Carboxyhemoglobin 38% Methemoglobin 1% Serum cyanide 0.35 mcg/mL (Reference range 0.5–1 mcg/mL) Which of the following statements about the patient’s condition is true?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
