Autonomic/CV Drugs — MCQs

On this page
A 19-year-old male college student is brought to the emergency department by his girlfriend complaining of intense pain. They had been playing outside in the snow when the patient started to have severe hand and feet pain. He says the pain is 9 out of 10 and causing him to have trouble moving his fingers and toes. He also reports some difficulty “catching his breath.” He notes that he has been tiring easily for the past month but thought it was because he was studying and going out late. On physical examination, the patient appears uncomfortable. Bilateral conjunctivae are pale. His hands are swollen and tender to palpation. Cardiopulmonary examination is normal. Hemoglobin is 9.0 g/dL. An electrocardiogram shows mild sinus tachycardia. Hemoglobin electrophoresis is performed, which confirms sickle cell disease. The patient’s pain is managed, and he is discharged on hydroxyurea. Which of the following is the most likely to occur as a result of the new medication?
A 38-year-old male is brought to the emergency department by ambulance after a motor vehicle collision. He is found to have a broken femur and multiple soft tissue injuries and is admitted to the hospital. During the hospital course, he is found to have lower extremity swelling, redness, and pain, so he is given an infusion of a medication. The intravenous medication is discontinued in favor of an oral medication in preparation for discharge; however, the patient leaves against medical advice prior to receiving the full set of instructions. The next day, the patient is found to have black lesions on his trunk and his leg. The protein involved in this patient's underlying abnormality most likely affects the function of which of the following factors?
A 61-year-old woman comes to the physician because of a 6-month history of left knee pain and stiffness. Examination of the left knee shows tenderness to palpation along the joint line; there is crepitus with full flexion and extension. An x-ray of the knee shows osteophytes with joint-space narrowing. Arthrocentesis of the knee joint yields clear fluid with a leukocyte count of 120/mm3. Treatment with ibuprofen during the next week significantly improves her condition. The beneficial effect of this drug is most likely due to inhibition of which of the following?
A 31-year-old female receives a kidney transplant for autosomal dominant polycystic kidney disease (ADPKD). Three weeks later, the patient experiences acute, T-cell mediated rejection of the allograft and is given sirolimus. Which of the following are side effects of this medication?
A 29-year-old woman presents to the primary care office for a recent history of falls. She has fallen 5 times over the last year. These falls are not associated with any preceding symptoms; she specifically denies dizziness, lightheadedness, or visual changes. However, she has started noticing that both of her legs feel weak. She's also noticed that her carpet feels strange beneath her bare feet. Her mother and grandmother have a history of similar problems. On physical exam, she has notable leg and foot muscular atrophy and 4/5 strength throughout her bilateral lower extremities. Sensation to light touch and pinprick is decreased up to the mid-calf. Ankle jerk reflex is absent bilaterally. Which of the following is the next best diagnostic test for this patient?
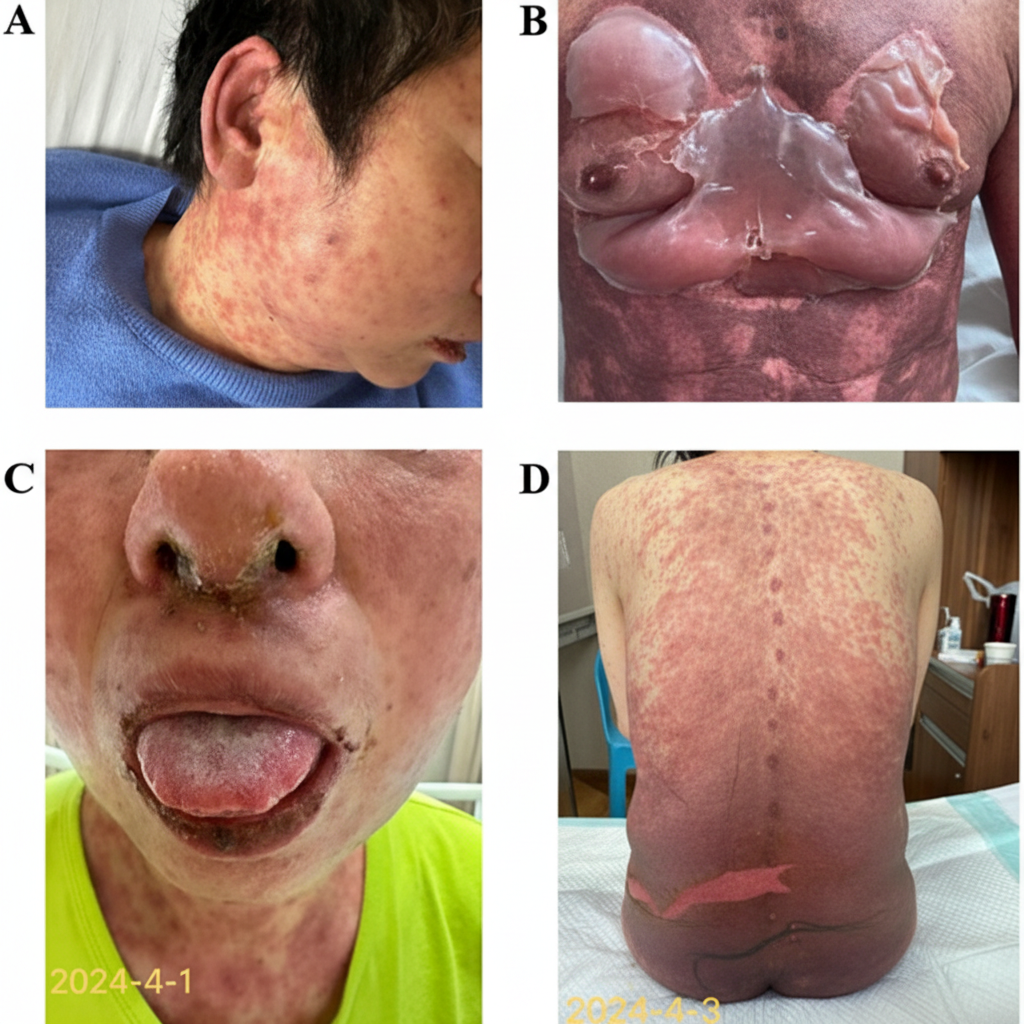
A 17-year-old male with a history of bipolar disorder presents to clinic with a rash (Image A) that he noticed one week after starting a medication to stabilize his mood. The medication blocks voltage-gated sodium channels and can be used to treat partial simple, partial complex, and generalized tonic-clonic seizures. Regarding the patient's rash, what is the next step in management?
A 3-year-old boy is brought in by his parents to the emergency department for lethargy and vomiting. The patient was fine until this afternoon, when his parents found him in the garage with an unlabeled open bottle containing an odorless liquid. On exam, the patient is not alert or oriented, but is responsive to touch and pain. The patient is afebrile and pulse is 90/min, blood pressure is 100/60 mmHg, and respirations are 20/min. Which of the following is an antidote for the most likely cause of this patient’s presentation?
A 27-year-old woman was found lying unconscious on the side of the street by her friend. He immediately called the ambulance who were close to this neighborhood. On initial examination, she appears barely able to breathe. Her pupils are pinpoint. The needles she likely used were found on site but the drug she injected was unknown. The first responders were quick to administer a drug which is effectively used in these situations and her symptoms slowly began to reverse. She was taken to the nearest emergency department for further workup. Which of the following best describes the mechanism of action of the drug administered by the first responders?
A 40-year-old man presents to the emergency department with a chief complaint of chest pain for the last 3 hours. His ECG shows normal sinus rhythm with ST-segment elevation in leads II, III, and aVF and reciprocal segment depression in leads V1–V6. On physical examination, cardiac sounds are normal on auscultation. His blood pressure is 92/64 mm Hg and heart rate is 93/min. A tissue plasminogen activator is administered to the patient intravenously within 1 hour of hospital arrival due to a lack of available percutaneous coronary intervention. After 6 hours of therapy, the patient's clinical condition starts to deteriorate. ECG on the monitor shows accelerated idioventricular rhythm, which within a couple of minutes changes to ventricular fibrillation. Before any measures could be started, the patient deteriorates further and must be transferred to the ICU. What is the most likely etiology of the ECG findings in this patient?
A 50-year-old male is brought to the dermatologist's office with complaints of a pigmented lesion. The lesion is uniformly dark with clean borders and no asymmetry and has been increasing in size over the past two weeks. He works in construction and spends large portions of his day outside. The dermatologist believes that this mole should be biopsied. To prepare the patient for the biopsy, the dermatologist injects a small amount of lidocaine into the skin around the lesion. Which of the following nerve functions would be the last to be blocked by the lidocaine?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
