Autonomic/CV Drugs — MCQs

On this page
A 22-year-old woman presents to the emergency department because of agitation and sweating. History shows she is currently being treated for depression with citalopram. She also takes tramadol for back pain. Her temperature is 38.6°C (101.5°F), the pulse is 108/min, the respirations are 18/min, and the blood pressure is 165/110 mm Hg. Physical examination shows hyperreflexia and mild tremors in all 4 extremities. Which of the following should be used in the next step of management for this patient?
A 44-year-old man seeks evaluation at a clinic because he is experiencing a problem with his sexual health for the past month. He says he does not get erections like he used to, despite feeling the urge. In addition to heart failure, he has angina and hypertension. His regular oral medications include amlodipine, atorvastatin, nitroglycerin, spironolactone, and losartan. After a detailed evaluation of his current medications, it is concluded that he has drug-induced erectile dysfunction. Which one of the following medications may have caused this patient's symptom?
A 28-year-old man comes to the emergency department for an injury sustained while doing construction. Physical examination shows a long, deep, irregular laceration on the lateral aspect of the left forearm with exposed fascia. Prior to surgical repair of the injury, a brachial plexus block is performed using a local anesthetic. Shortly after the nerve block is performed, he complains of dizziness and then loses consciousness. His radial pulse is faint and a continuous cardiac monitor shows a heart rate of 24/min. Which of the following is the most likely mechanism of action of the anesthetic that was administered?
A 9-year-old boy is brought to the physician by his mother to establish care after moving to a new city. He lives at home with his mother and older brother. He was having trouble in school until he was started on ethosuximide by a previous physician; he is now performing well in school. This patient is undergoing treatment for a condition that most likely presented with which of the following symptoms?
A 41-year-old woman is brought to the emergency department by ambulance because of a sudden onset severe headache. On presentation, the patient also says that she is not able to see well. Physical examination shows ptosis of the right eye with a dilated pupil that is deviated inferiorly and laterally. Based on the clinical presentation, neurosurgery is immediately consulted and the patient is taken for an early trans-sphenoidal surgical decompression. Which of the following will also most likely need to be supplemented in this patient?
A 70-year-old female with a history of congestive heart failure presents to the emergency room with dyspnea. She reports progressive difficulty breathing which began when she ran out of her furosemide and lisinopril prescriptions 1-2 weeks ago. She states the dyspnea is worse at night and when lying down. She denies any fever, cough, or GI symptoms. Her medication list reveals she is also taking digoxin. Physical exam is significant for normal vital signs, crackles at both lung bases and 2+ pitting edema of both legs. The resident orders the medical student to place the head of the patient's bed at 30 degrees. Additionally, he writes orders for the patient to be given furosemide, morphine, nitrates, and oxygen. Which of the following should be checked before starting this medication regimen?
A 41-year-old woman comes to the emergency room because she has been taking phenelzine for a few years and her doctor warned her that she should not eat aged cheese while on the medication. That night, she unknowingly ate an appetizer at a friend's party that was filled with cheese. She is concerned and wants to make sure that everything is all right. What vital sign or blood test is the most important to monitor in this patient?
A 21-year-old college student comes to the physician for intermittent palpitations. She does not have chest pain or shortness of breath. The symptoms started 2 days ago, on the night after she came back to her dormitory after a 4-hour-long bus trip from home. A day ago, she went to a party with friends. The palpitations have gotten worse since then and occur more frequently. The patient has smoked 5 cigarettes daily for the past 3 years. She drinks 4–6 alcoholic beverages with friends once or twice a week and occasionally uses marijuana. She is sexually active with her boyfriend and takes oral contraceptive pills. She does not appear distressed. Her pulse is 100/min and irregular, blood pressure is 140/85 mm Hg, and respirations are at 25/min. Physical examination shows a fine tremor in both hands, warm extremities, and swollen lower legs. The lungs are clear to auscultation. An ECG is shown below. Which of the following is the most appropriate next step in management?
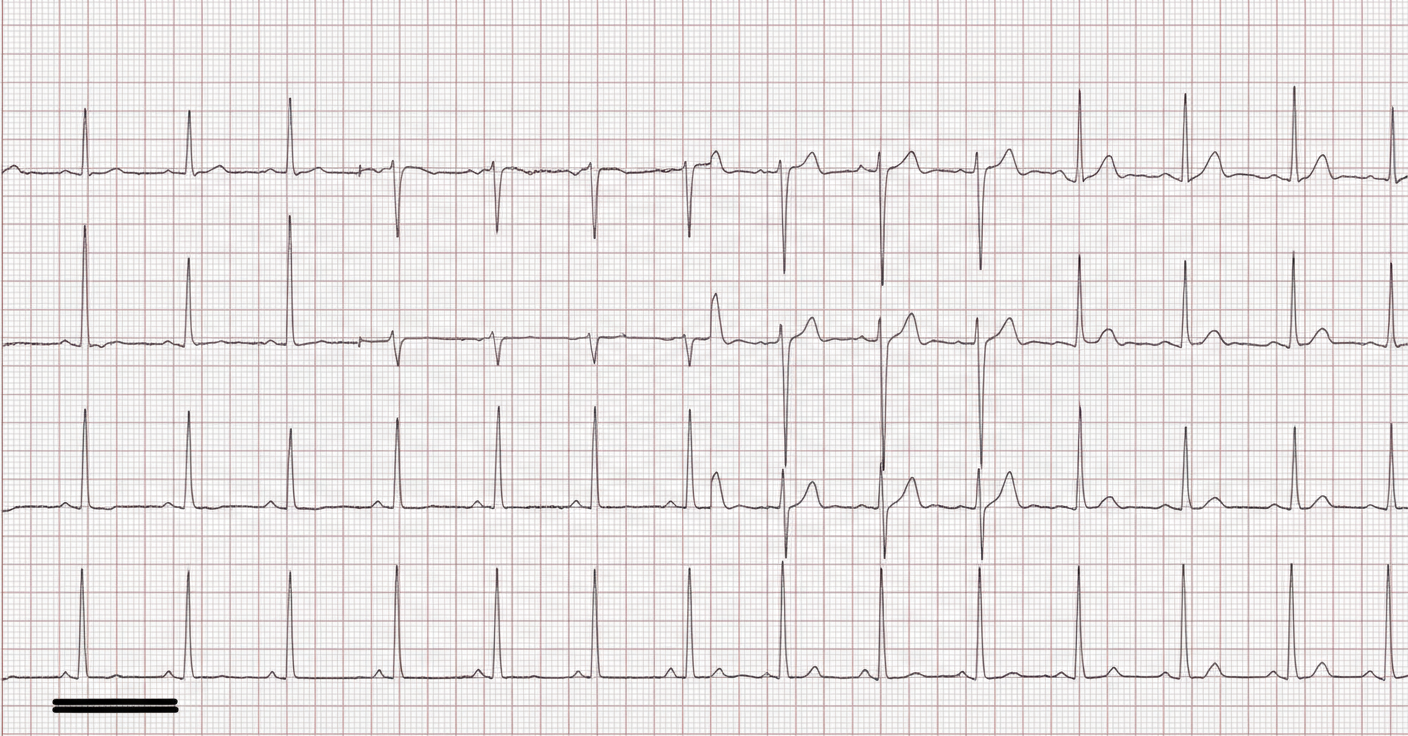
A 69-year-old woman comes to the clinic for an annual well exam. She reports no significant changes to her health except for an arm fracture 3 weeks ago while she was lifting some heavy bags. Her diabetes is well controlled with metformin. She reports some vaginal dryness that she manages with adequate lubrication. She denies any weight changes, fevers, chills, palpitations, nausea/vomiting, incontinence, or bowel changes. A dual-energy X-ray absorptiometry (DEXA) scan was done and demonstrated a T-score of -2.7. She was subsequently prescribed a selective estrogen receptor modulator, in addition to vitamin and weight-bearing exercises, for the management of her symptoms. What is the mechanism of action of the prescribed medication?
A 58-year-old man with a 10-year history of type 2 diabetes mellitus and hypertension comes to the physician for a routine examination. Current medications include metformin and captopril. His pulse is 84/min and blood pressure is 120/75 mm Hg. His hemoglobin A1c concentration is 9.5%. The physician adds repaglinide to his treatment regimen. The mechanism of action of this agent is most similar to that of which of the following drugs?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
