Autonomic/CV Drugs — MCQs

On this page
A 13-year-old male presents to his primary care provider with joint pain in his right knee. He has had multiple episodes of pain and effusion in both knees throughout his life as well as easy bruising. Most of these episodes followed minor trauma, including accidentally hitting his knee on a coffee table, but they occasionally occurred spontaneously. Both his uncle and grandfather have had similar problems. The patient denies any recent trauma and reports that his current pain is dull in nature. The patient is a long distance runner and jogs frequently. He is currently training for an upcoming track and field meet. On physical exam, the joint is warm and nonerythematous and with a large effusion. The patient endorses pain on both passive and active range of motion. Which of the following prophylactic treatments could have prevented this complication?
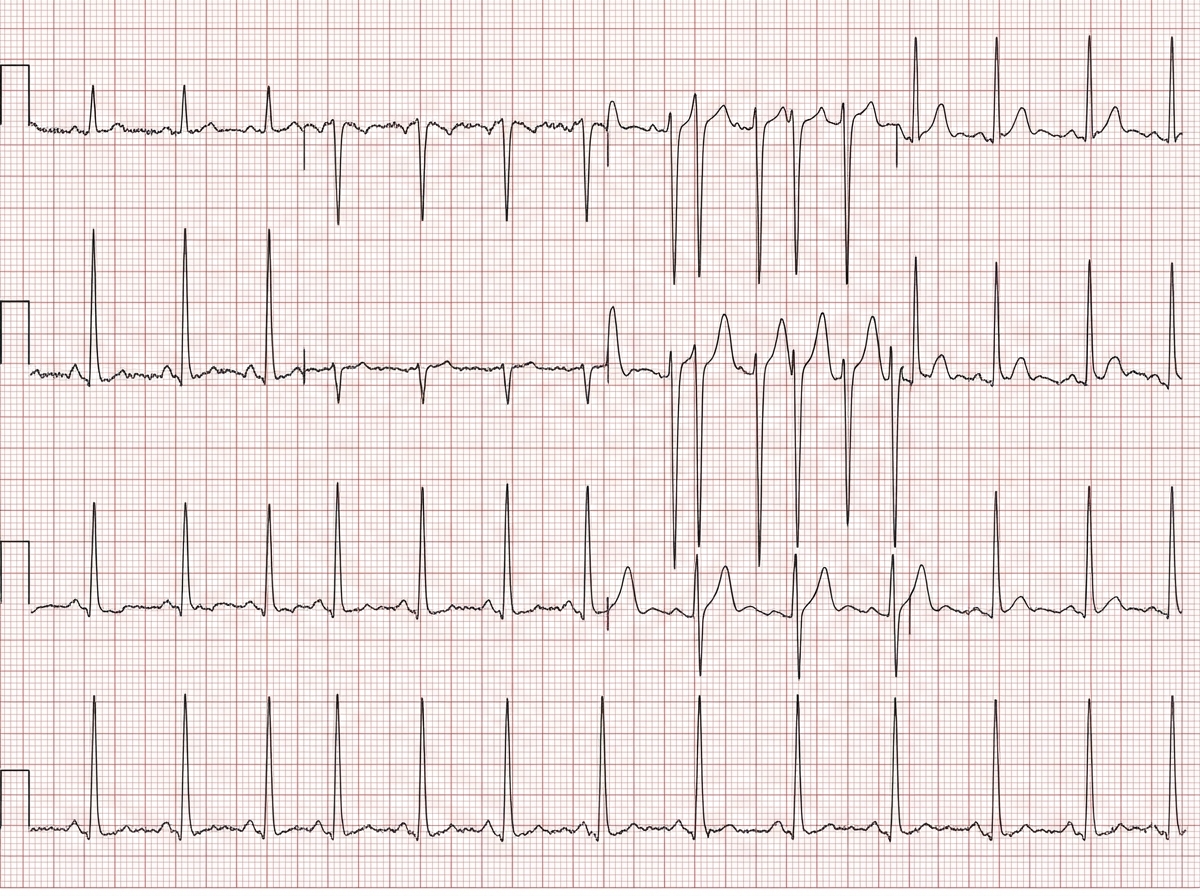
A 32-year-old female with a history of depression presents to the emergency department after a suspected ingestion. She is confused, reporting blurry vision, and responding to visual hallucinations. Vital signs are as follows: Temperature: 98.9 degrees Fahrenheit (37.2 Celsius) Heart Rate: 105 bpm Blood Pressure: 90/65 mmHg Respiratory Rate: 21 respirations per minute O2 Saturation: 99% on room air Upon reviewing her ECG (shown in Image A), the emergency room physician orders sodium bicarbonate. What medication was the likely cause of this patient's cardiac abnormality?
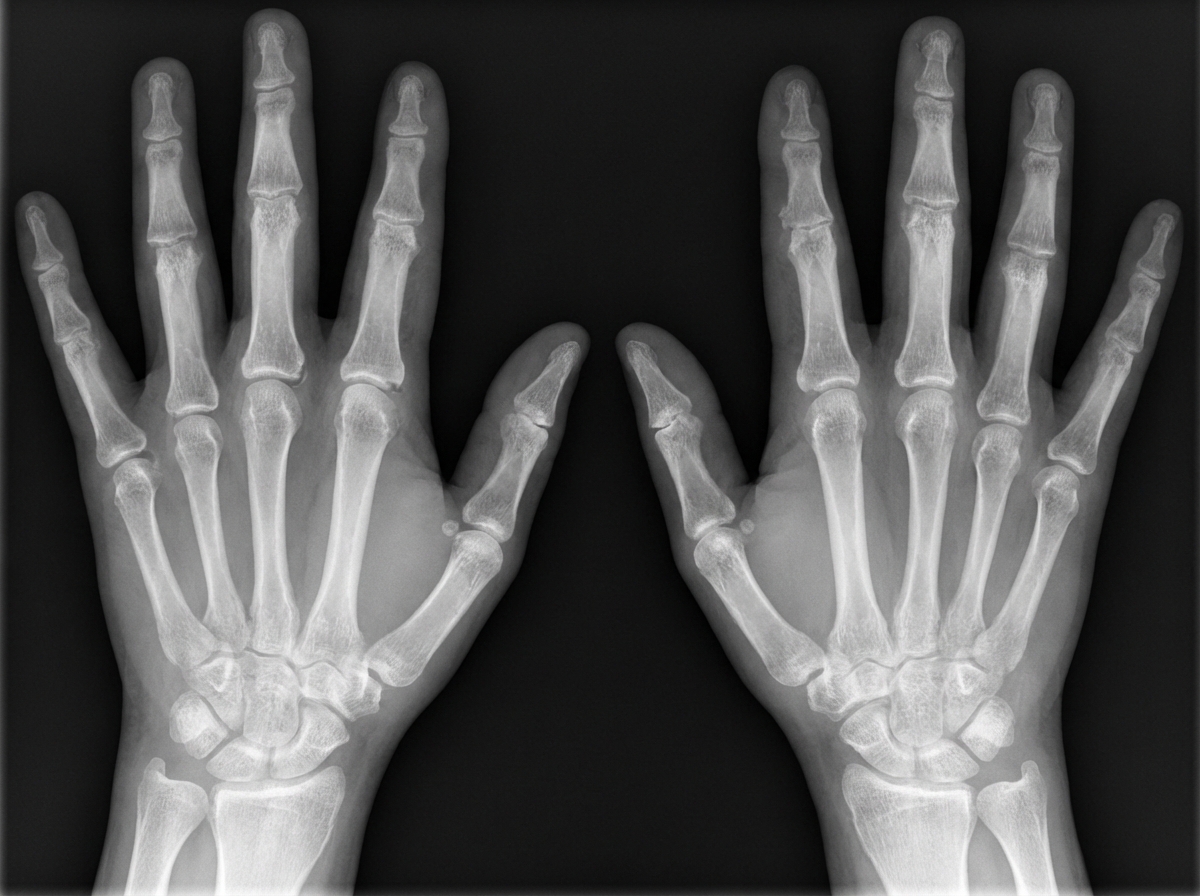
A 65-year-old woman is brought to the emergency department because of left wrist pain and swelling that began after she fell from a seated position. Menopause occurred 15 years ago. Her serum parathyroid hormone level is within normal limits. An x-ray of the left wrist shows a nondisplaced fracture of the distal radial metaphysis and decreased bone mineral density. The patient would likely benefit from an agent with a structure analogous to which of the following substances?
A 25-year-old woman presents to her primary care physician with complaints of chronic congestion. She notes that she has always had trouble breathing through her nose, and her new husband has told her that she breathes loudly when she sleeps. She denies frequent infections or allergies. She has no chronic medical problems and takes no medications. Family history is also insignificant. The blood pressure is 124/78 mm Hg, heart rate is 74/min, and respiratory rate is 14/min. On physical examination, her lungs are clear to auscultation bilaterally. Intranasal inspection reveals a deviated septum. She is referred to an otolaryngologist for surgical evaluation. When discussing the surgical options for this condition, she asks if she will be given propofol for anesthesia. Which of the following is the most appropriate classification of anesthesia primarily achieved with intravenous propofol?
A 42-year-old woman comes to the physician because of an 8 month history of intermittent pain and stiffness in her hands and feet. She reports that these episodes occur about three times a month after she wakes up and last for approximately one hour. She often also experiences fever and myalgia on the days that these episodes occur. During these attacks, she takes ibuprofen for the pain, which provides good relief. She had her last attack 5 days ago. She is otherwise healthy and takes no medications. Her sister has systemic lupus erythematosus. Vital signs are within normal limits. Examination shows mild swelling and tenderness of the wrists and the proximal interphalangeal joints of both hands. The remainder of the examination shows no abnormalities. An x-ray of her hands is shown. Which of the following is the most appropriate pharmacotherapy?
A 33-year-old man comes to the physician for evaluation of progressive hair loss from his scalp. He first noticed receding of the hairline over the bitemporal regions of his scalp 5 years ago. Since then, his hair has gradually become thinner over the crown of his head. He is otherwise healthy and takes no medications. Examination shows diffuse, nonscarring hair loss over the scalp with a bitemporal pattern of recession. Administration of which of the following drugs is most appropriate to treat this patient's hair loss?
A 35-year-old woman with irritable bowel syndrome comes to the physician because of increased diarrhea. She has not had any fever, bloody stools, nausea, or vomiting. The increase in stool frequency began when she started a new job. She is started on loperamide, and her symptoms improve. Which of the following is the primary mechanism of action of this drug?
A 41-year-old woman arrives to her primary care physician with abnormal labs. She states that 1 week ago she had laboratory work done as part of her company’s health initiative. During the past month, she has been walking 3 miles a day and has increased the amount of fruits and vegetables in her diet. Her medical history is significant for obesity, hypertension, and obstructive sleep apnea. She takes hydrochlorothiazide and wears a continuous positive airway pressure machine at night. Her recent labs are shown below: Serum: Na+: 140 mEq/L K+: 4.1 mEq/L Cl-: 101 mEq/L BUN: 16 mg/dL Glucose: 95 mg/dL Creatinine: 0.9 mg/dL Total cholesterol: 255 mg/dL (normal < 200 mg/dL) Low-density lipoprotein (LDL) cholesterol: 115 mg/dL (normal < 100 mg/dL) High-density lipoprotein (HDL) cholesterol: 40 (normal > 50 mg/dL) Triglycerides: 163 mg/dL (normal < 150 mg/dL) The patient is started on atorvastatin. Which of the following is the most common adverse effect of the patient’s new medication?
A preterm neonate, born at 28 weeks of gestation, is in the neonatal intensive care unit as he developed respiratory distress during the 4th hour after birth. On the 2nd day of life, he required ventilator support. Today, on the 5th day of life, he developed generalized purpura and a hemorrhagic aspirate from the stomach. His laboratory workup is suggestive of thrombocytopenia, prolonged prothrombin time, and prolonged activated partial thromboplastin time. Which of the following statements is correct regarding the coagulation system of this patient?
A 35-year-old woman is brought to the emergency department by her husband after she lost consciousness 30 minutes ago. The patient's husband says that she has been in a bad mood lately and getting upset over small things. He also says she has been crying a lot and staying up late at night. Her husband mentions that her mother died earlier this year, and she hasn't been coping well with this loss. He says that he came home an hour ago and found her lying on the floor next to a bottle of pills. The patient's husband knows that they were a bottle of her migraine prevention pills (propranolol) but cannot remember the exact name of the medication. On examination, the patient's blood pressure is 75/50 mm Hg, the pulse is 50/min, and the respiratory rate is 12/min. Which of the following is the best course of treatment for this patient?
Practice by Chapter
Antiarrhythmic classification and mechanisms
Practice Questions
Class I antiarrhythmics (sodium channel blockers)
Practice Questions
Class II antiarrhythmics (beta blockers)
Practice Questions
Class III antiarrhythmics (potassium channel blockers)
Practice Questions
Class IV antiarrhythmics (calcium channel blockers)
Practice Questions
Other antiarrhythmic agents
Practice Questions
Antianginal drugs
Practice Questions
Positive inotropic agents
Practice Questions
Phosphodiesterase inhibitors
Practice Questions
Cardiac glycosides
Practice Questions
Vasopressors and inotropes
Practice Questions
Pulmonary hypertension therapies
Practice Questions
Peripheral vascular disease therapies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
