Antivirals — MCQs

On this page
An HIV-positive patient with a CD4+ count of 45 is receiving recommended first-line treatment for a case of cytomegalovirus retinitis. Coadministration with which of the following agents would be most likely to precipitate a deficiency of neutrophils in this patient?
A 26-year-old nurse presents 12 hours after she accidentally stuck herself with a blood-contaminated needle. She reported the accident appropriately and now seeks post-exposure prophylaxis. She does not have any complaints at the moment of presentation. Her vital signs include: blood pressure 125/80 mm Hg, heart rate 71/min, respiratory rate 15/min, and temperature 36.5℃ (97.7℉). Physical examination is unremarkable. The nurse has prescribed a post-exposure prophylaxis regimen which includes tenofovir, emtricitabine, and raltegravir. How will tenofovir change the maximum reaction rate (Vm) and Michaelis constant (Km) of the viral reverse transcriptase?
A previously healthy 26-year-old man is brought to the emergency department because of extreme agitation and confusion. He is unable to give a clear history. His mother says he returned from a hiking trip 4 weeks ago on which he also explored caves. Over the past few days, he has had generalized fever and malaise with a sore throat. He has refused to drink any liquids for the last day. His immunizations are up-to-date. His temperature is 100.6°F (38.1°C), pulse is 92/min, respirations are 18/min, and blood pressure is 110/75 mm Hg. His pupils are 6 mm wide and reactive to light. He has a moderate amount of drool. Muscle tone is greatly increased in both the upper and lower extremities. The remainder of the examination is not performed because the patient becomes combative and refuses further assessment. Serum and urine toxicology screens are negative. Which of the following is most likely to have prevented this patient's condition?
A 27-year-old woman consults an obstetrician as she is planning to become pregnant. She has been diagnosed with HIV (human immunodeficiency virus) infection recently and is currently taking antiretroviral therapy (HAART), as prescribed by her physician. The obstetrician emphasizes the importance of antenatal and peripartum antiretroviral therapy for reducing the risk of mother-to-child transmission of HIV. She also tells the patient that certain antiretroviral drugs, if taken during pregnancy, increase the risk of birth defects in the fetus. She gives a printed list of such drugs to the woman for educational and informational purposes. Which of the following drugs are most likely to be present on the list?
A 49-year-old woman presents to her primary care doctor in late December with malaise. She reports worsening fatigue, myalgias, headache, and malaise that started 1 day ago. She works as a lunch lady at an elementary school. Her past medical history is notable for a distal radius fracture after a fall 2 years ago, but she is otherwise healthy and takes no medications. She does not smoke or drink alcohol. She is married and has 3 adult children who are healthy. Her temperature is 102.9°F (39.4°C), blood pressure is 101/61 mmHg, pulse is 112/min, and respirations are 21/min. On exam, she appears lethargic and uncomfortable but is able to answer questions appropriately. Breath sounds are normal bilaterally. She is started on intravenous fluids and a pharmacologic agent for treatment. Which of the following is the most likely mechanism of action of the drug being used to treat this patient?
A 35-year-old woman presents to a physician’s office for a follow-up visit. She recently underwent a complete physical examination with routine laboratory tests. She also had a Pap smear and testing for sexually transmitted diseases. Since her divorce 2 years ago, she had sexual encounters with random men at bars or social events and frequently did not use any form of contraception during sexual intercourse. She was shown to be positive for the human immunodeficiency virus (HIV). Combination anti-retroviral treatment is initiated including zidovudine, didanosine, and efavirenz. One week later, she is rushed to the hospital where she is diagnosed with acute pancreatitis. Which of the following precautions will be required after pancreatitis resolves with treatment?
A 49-year-old man presents to a new primary care provider complaining of fatigue and occasional fever over the last month. These symptoms are starting to affect his job and he would like treatment. The physician runs a standard metabolic panel that shows elevated AST and ALT. The patient is then tested for hepatitis viruses. He is hepatitis C positive. The patient and his doctor discuss treatment options and agree upon pegylated interferon and oral ribavirin. Which side-effect is most likely while taking the ribavirin?
A 60-year-old man comes to the physician’s office with jaundice. Liver ultrasound reveals a shrunken liver and biopsy reveals cirrhosis. Hepatitis serologies are below: Anti-HAV: negative HBsAg: negative HBsAb: positive HBeAg: negative Anti-HBe: negative Anti-HBc: negative Anti-HCV: positive The hepatitis C viral load is 1,000,000 copies/mL. The patient is started on an antiviral regimen including sofosbuvir. What is the mechanism of action of this drug?
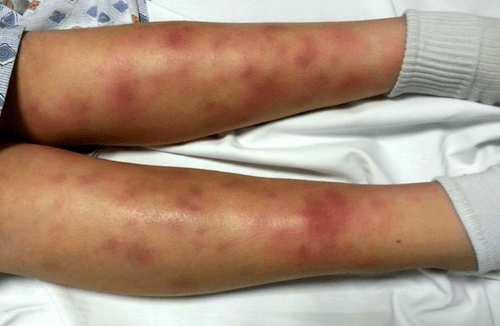
A 45-year-old man with HIV comes to the physician because of multiple lesions on his chest and lower extremities. The lesions have progressively increased in size and are not painful or pruritic. Current medications include abacavir, dolutegravir, and lamivudine. A photograph of the lesions is shown. His CD4+ T-lymphocyte count is 450/mm3 (normal ≥ 500/mm3). A skin biopsy shows multiple spindle-shaped cells and lymphocytic infiltrate. Which of the following is the most appropriate pharmacotherapy?
A 53-year-old woman comes to the physician in February because of a 1-day history of fever, chills, headache, and dry cough. She also reports malaise and generalized muscle aches. She works as a teacher at a local high school, where there was recently an outbreak of influenza. She has a history of intermittent asthma, for which she takes albuterol as needed. She declined the influenza vaccine offered in the fall because her sister told her that a friend developed a flulike illness after receiving the vaccine. She is worried about possibly becoming ill and cannot afford to miss work. Her temperature is 37.9°C (100.3°F), heart rate is 58/min, and her respirations are 12/min. Physical examination is unremarkable. Her hemoglobin concentration is 14.5 g/dL, leukocyte count is 9,400/mm3, and platelet count is 280,000/mm3. In addition to analgesia, which of the following is the most appropriate next step in management?
Practice by Chapter
HIV protease inhibitors
Practice Questions
HIV reverse transcriptase inhibitors
Practice Questions
HIV integrase inhibitors
Practice Questions
HIV entry inhibitors
Practice Questions
Hepatitis B antivirals
Practice Questions
Hepatitis C direct-acting antivirals
Practice Questions
Influenza antivirals
Practice Questions
Herpesvirus antivirals
Practice Questions
Cytomegalovirus antivirals
Practice Questions
Respiratory syncytial virus therapies
Practice Questions
Broad-spectrum antivirals
Practice Questions
Antiretroviral resistance
Practice Questions
Antiviral prophylaxis strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
