Antivirals — MCQs

On this page
A 45-year-old man comes to the emergency department with fever, nonproductive cough, and difficulty breathing. Three years ago, he underwent lung transplantation. A CT scan of the chest shows diffuse bilateral ground-glass opacities. Pathologic examination of a transbronchial lung biopsy specimen shows several large cells containing intranuclear inclusions with a clear halo. Treatment with ganciclovir fails to improve his symptoms. He is subsequently treated successfully with another medication. This drug does not require activation by viral kinases and also has known in-vitro activity against HIV and HBV. The patient was most likely treated with which of the following drugs?
A 37-year-old man comes to the physician because of a 6-month history of progressive breast enlargement. Two years ago, he was diagnosed with HIV infection and started treatment with antiretroviral medications. Examination shows a soft, non-tender, ill-defined swelling at the nape of the neck. The cheeks appear hollowed. Serum studies show increased total cholesterol and LDL concentration. Which of the following medications is the most likely cause of these findings?
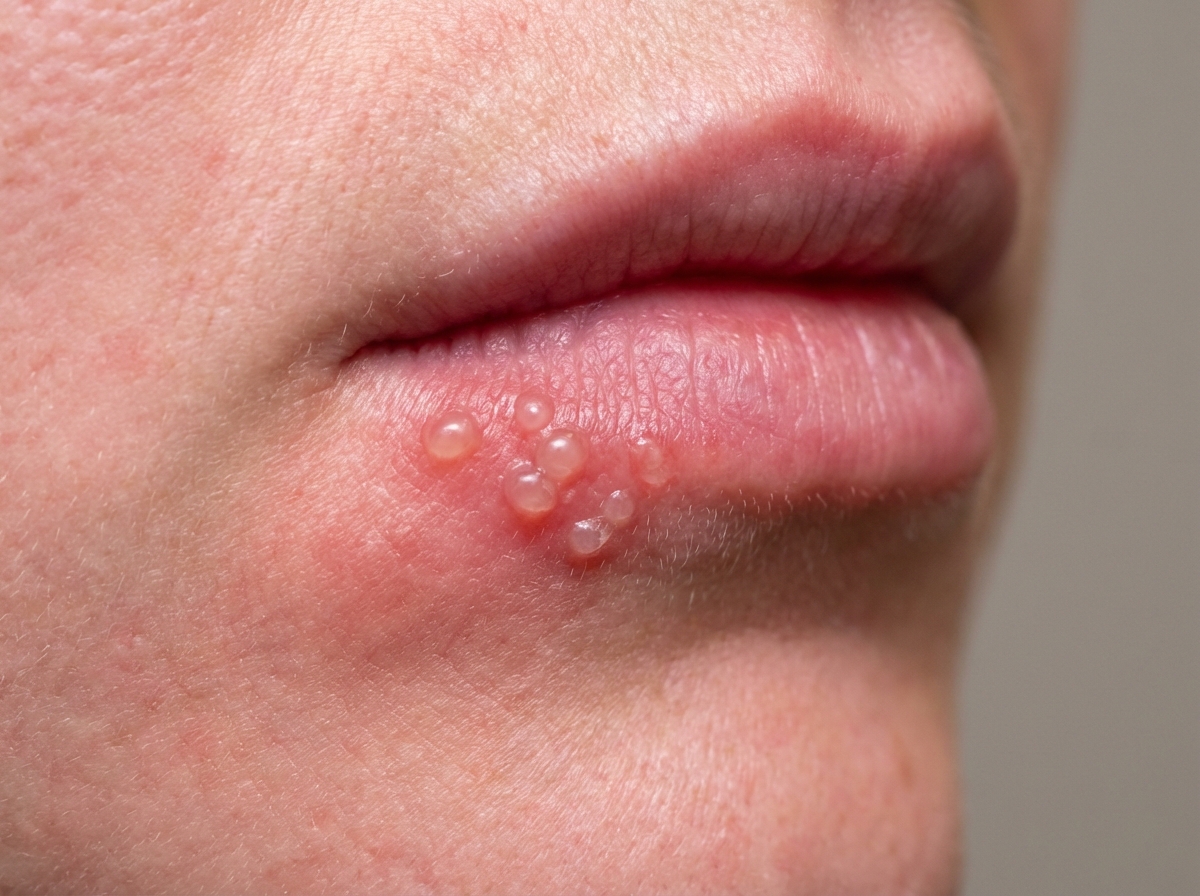
A 44-year-old man presents to a family medical center for evaluation of multiple, painful lesions on the lower lip. He says that the lesions appeared 1 day ago after spending a weekend vacation at the beach. He reports having experienced a tingling sensation before the lesions appeared. This is the 3rd time in the past year that the lesions have occurred. There are no past medical conditions to document. He appears well-nourished and does not exhibit poor hygiene. His vital signs include the following: the heart rate is 66/min, the respiratory rate is 14/min, the temperature is 37.3°C (99.2°F), and the blood pressure is 124/76 mm Hg. Inspection of the lips at the vermillion border reveals 2 vesicular lesions (refer to picture). Palpation of the neck reveals cervical lymphadenopathy. What is the most appropriate treatment at this time?
A 56-year-old African American presents to the emergency department due to abdominal pain, fatigue, and weight loss over the past 3 months. He has a long-standing history of chronic hepatitis B virus infection complicated by cirrhosis. On examination, he has jaundice, leg edema, and a palpable mass in the right upper abdominal quadrant. Abdominal ultrasound shows a 3-cm liver mass with poorly defined margins and coarse, irregular internal echoes. Blood investigations are shown: Aspartate aminotransferase (AST) 90 U/L Alanine aminotransferase (ALT) 50 U/L Total bilirubin 2 mg/dL Albumin 3 g/dL Alkaline phosphatase 100 U/L Alpha fetoprotein 600 micrograms/L Which of the following targeted agents is approved for advanced-stage hepatoma?
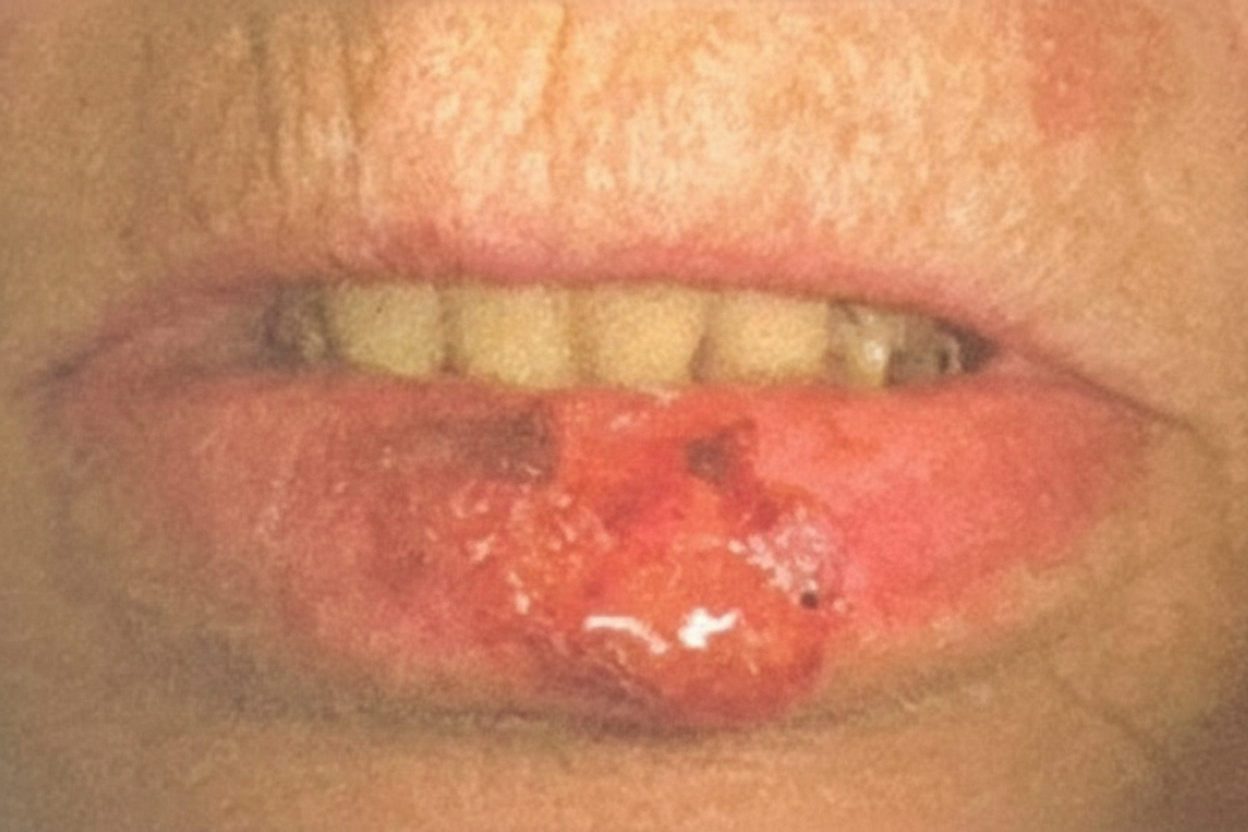
A 20-year-old medical student presents to the clinic with a very painful lesion on her lower lip, as shown in the photograph below. She admits that she applied polymyxin ointment to the lesion without improvement. A few months ago, she used the same antibiotic ointment to treat an infected cut on her arm. At that time, she had read in her microbiology book that polymyxin is an antibiotic that disrupts cell membranes. Why did the treatment fail this time?
A 65-year-old man presents to his primary care physician for a rash. He states that for the past several days he has felt burning and itching around his eye. Yesterday, he noticed that a rash had formed. Review of systems is notable for mild diarrhea for the past week. The patient has a past medical history of diabetes, asthma, seasonal allergies, and hypertension. He is not currently taking any medications. Physical exam is notable for a vesicular rash surrounding the orbit. Which of the following is the best next step in management?
A 5-year-old boy is brought to the emergency department because of a generalized pruritic rash for 14 hours. Five days ago, he had pink eyes that resolved spontaneously. He has acute lymphoblastic leukemia. He has received 3 cycles of chemotherapy with vincristine, asparaginase, dexamethasone, and doxorubicin. His last treatment cycle was 2 weeks ago. The patient's other medications include multivitamin supplements. His temperature is 38°C (100.4°F), pulse 90/min, and blood pressure is 105/65 mm Hg. Examination of the skin shows multiple crops of macules and papules over the face, trunk, and extremities. There are also excoriation marks and crusted lesions. The remainder of the examination shows no abnormalities. Which of the following is the most appropriate next step in the treatment of this patient?
An HIV-positive 48-year-old man comes to the emergency department because of a 3-month history of recurrent, painful mouth ulcers. This time, the pain is so severe that the patient cannot eat. He has a history of a seizure disorder but currently does not take any medications. He appears very ill. His temperature is 39.0°C (102.2°F). Physical examination shows numerous vesicular ulcerations on the lips and sloughing of the gums, buccal mucosa, and hard palate. Genetic analysis of the pathogen isolated from the lesions shows a mutation in a gene encoding viral phosphotransferases. Which of the following drugs is the most appropriate treatment?
A 10-year-old boy presents to the emergency department with his parents. The boy complains of fever, neck stiffness, and drowsiness for the last several days. His past medical history is noncontributory. The boy was born at 39 weeks gestation via spontaneous vaginal delivery. He is up to date on all vaccines and is meeting all developmental milestones. There were no sick contacts at home or at school. The family did not travel out of the area recently. His heart rate is 100/min, respiratory rate is 22/min, blood pressure is 105/65 mm Hg, and temperature is 40.5ºC (104.9°F). On physical examination, he appears unwell and confused. His heart rate is elevated with a regular rhythm and his lungs are clear to auscultation bilaterally. During the examination, he experiences a right-sided focal seizure, which is controlled with lorazepam. A head CT reveals bilateral asymmetrical hypodensities of the temporal region. A lumbar puncture is performed and reveals the following: WBC count 25/mm3 Cell predominance lymphocytes Protein elevated The patient is started on a medication to treat the underlying cause of his symptoms. What is the mechanism of action of this medication?
A 52-year-old woman comes to the physician because of abdominal discomfort, anorexia, and mild fatigue. She has systemic lupus erythematosus and takes hydroxychloroquine. She does not drink alcohol or use illicit drugs. Physical examination shows no abnormalities. Laboratory studies show: Alanine aminotransferase 455 U/L Aspartate aminotransferase 205 U/L Hepatitis B surface antigen positive Hepatitis B surface antibody negative Hepatitis B envelope antigen positive Hepatitis B core antigen IgG antibody positive Which of the following is the most appropriate pharmacotherapy for this patient?
Practice by Chapter
HIV protease inhibitors
Practice Questions
HIV reverse transcriptase inhibitors
Practice Questions
HIV integrase inhibitors
Practice Questions
HIV entry inhibitors
Practice Questions
Hepatitis B antivirals
Practice Questions
Hepatitis C direct-acting antivirals
Practice Questions
Influenza antivirals
Practice Questions
Herpesvirus antivirals
Practice Questions
Cytomegalovirus antivirals
Practice Questions
Respiratory syncytial virus therapies
Practice Questions
Broad-spectrum antivirals
Practice Questions
Antiretroviral resistance
Practice Questions
Antiviral prophylaxis strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
