Antimicrobials — MCQs

On this page
A 47-year-old woman presents to the physician with complaints of fatigue accompanied by symmetric pain, swelling, and stiffness in her wrists, fingers, knees, and other joints. She describes the stiffness as being particularly severe upon awakening, but gradually improves as she moves throughout her day. Her physician initially suggests that she take NSAIDs. However, after a few months of minimal symptomatic improvement, she is prescribed an immunosuppressive drug that has a mechanism of preventing IL-2 transcription. What is the main toxicity that the patient must be aware of with this particular class of drugs?
A 33-year-old woman with a history of multiple sclerosis is brought to the physician because of dizziness, urinary incontinence, loss of vision in her right eye, and numbness and weakness of the left leg. She has had recurrent episodes of neurological symptoms despite several changes in her medication regimen. An MRI of the brain shows several new enhancing lesions in the periventricular white matter and the brainstem. Treatment with a drug that binds to CD52 is initiated. Which of the following agents was most likely prescribed?
A 65-year-old male presents to the physician after noticing gross blood with urination. He reports that this is not associated with pain. The patient smokes 1.5 packs per day for 45 years. Dipstick analysis is positive for blood, with 5 RBC per high-power field (HPF) on urinalysis. A cystoscopy is performed, which is significant for a lesion suspicious for malignancy. A biopsy was obtained, which is suggestive of muscle-invasive transitional cell carcinoma. Before radical cystectomy is performed, the patient is started on cisplatin-based chemotherapy. Which of the following is most likely associated with this chemotherapeutic drug?
A 32-year-old woman comes to the physician with fever and malaise. For the past 2 days, she has felt fatigued and weak and has had chills. Last night, she had a temperature of 40.8°C (104.2°F). She has had a sore throat since this morning. The patient was recently diagnosed with Graves disease and started on methimazole. Laboratory studies show: Hemoglobin 13.3 g/dL Leukocyte count 3,200/mm3 Segmented neutrophils 8% Basophils < 1% Eosinophils < 1% Lymphocytes 80% Monocytes 11% Platelet count 220,000/mm3 Which of the following is the most appropriate next step in management?
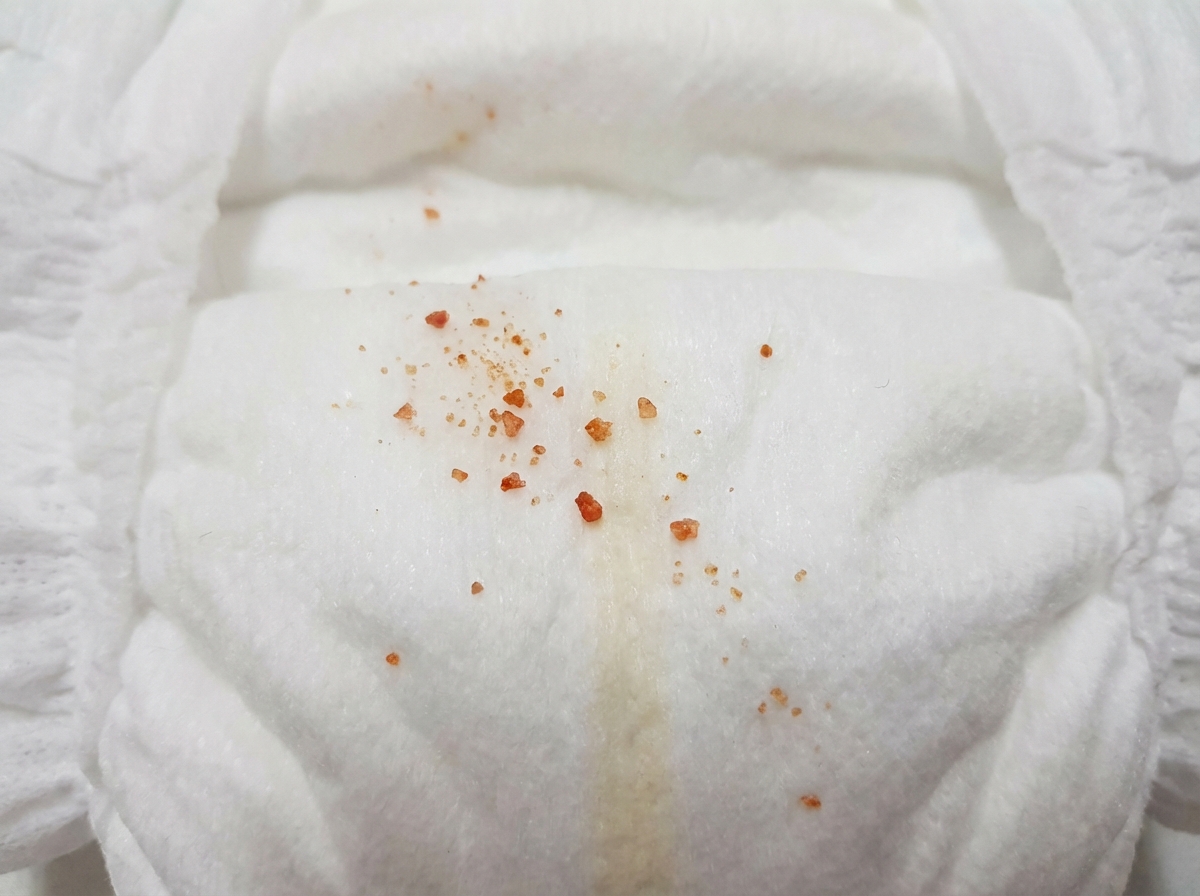
A 2-year-old boy is brought to his pediatrician for evaluation of a tender red big toe. His mother also notes that she has seen him recently starting to bite his own fingers and also exhibits spasms of muscle tightness. She reports that his diapers often contain the substance shown in the photograph. On exam he is noted to be significantly developmentally delayed as he is neither walking nor talking. Which of the following would be the first-line pharmacologic treatment for this patient's disorder?
A 17-year-old girl is brought into the physician's office with complaints of nausea, vomiting, headache, and blurry vision. In preparation for final exams the patient's mother started her on an array of supplements and herbal preparations given the "viral illness" that is prevalent at her school. Despite these remedies, the girl has been feeling perpetually worse, and yesterday during cheerleading practice had to sit out after vomiting and feeling dizzy. The patient admits to falling during one of the exercises and hitting her head on another girl's shin due to her dizziness. When asked to clarify her dizziness, the patient states that she feels rather lightheaded at times. The patient's BMI is 19 kg/m^2. She endorses diarrhea of recent onset, and some non-specific, diffuse pruritus of her skin which she attributes to stress from her finals. The patient has a past medical history of anxiety, depression, and excessive exercise habits. On physical exam the patient is alert and oriented to place, person, and time, and answers questions appropriately. She denies any decreased ability to participate in school or to focus. Her skin is dry and peeling with a minor yellow discoloration. Her memory is intact at 1 minute and 5 minutes for 3 objects. The patient's pupils are equal and reactive to light and there are no abnormalities upon examination of cranial nerve III, IV or VI. Which of the following is the most likely cause of this patient's symptoms?
A 50-year-old male with HIV presents to his primary care provider complaining of persistent fevers and night sweats over the past four months. He has also experienced a productive cough. He has been poorly adherent to his HAART regimen. His past medical history also includes gout, hypertension, and diabetes mellitus. He takes allopurinol, enalapril, and metformin. His temperature is 100.9°F (38.3°C), blood pressure is 125/75 mmHg, pulse is 95/min, and respirations are 20/min. His CD4 count is 85 cell/mm^3 and a PPD is negative. A chest radiograph reveals cavitations in the left upper lobe and left lower lobe. Bronchoalveolar lavage reveals the presence of partially acid-fast gram-positive branching rods. A head CT is negative for any intracranial process. A drug with which of the following mechanisms of action is most appropriate for the management of this patient?
A 3-month-old infant is brought to the emergency department because of lethargy and skin discoloration that started after he was fed some locally prepared baby food from a farmer's market. On presentation, he appears irritable and responds slowly to stimuli. Physical examination reveals rapid, labored breathing and a blue tinge to the infant's skin. A blood sample drawn for testing is found to be darker than normal. Which of the following is the most likely cause of this infant's presentation?
A previously healthy 48-year-old man comes to the physician because of a 2-month history of weight loss and yellowing of the skin. He works as a farmer and cultivates soybean and corn. He does not smoke, drink alcohol, or use illicit drugs. His vital signs are within normal limits. Physical examination shows scleral icterus and tender hepatomegaly. Ultrasonography of the abdomen shows a 5-cm nodular lesion in the right lobe of the liver. Further evaluation of the lesion confirms hepatocellular carcinoma. The activity of which of the following enzymes most likely contributed to the pathogenesis of this patient's condition?
A 66-year-old man presents to your office for a regular checkup. His only current complaint is periodic difficulty falling asleep at night. He takes captopril and hydrochlorothiazide for hypertension, atorvastatin for hyperlipidemia, and aspirin for cardiovascular disease prevention. His past medical history is significant for tympanoplasty performed 8 years ago for tympanic membrane rupture after an episode of purulent otitis media and intussusception that required surgical intervention 10 years ago. He also had a severe anaphylactic reaction after his 2nd Tdap administration 3 years ago. His blood pressure is 145/90 mm Hg, heart rate is 88/min, respiratory rate is 12/min, and temperature is 36.4°C (97.5°F). Physical examination only reveals a laterally displaced point of maximum impulse. Blood analysis shows the following findings: Sodium: 139 mEq/L (139 mmol/L) Potassium: 5.0 mEq/L (5.0 mmol/L) Chloride: 100 mEq/L (100 mmol/L) Bicarbonate: 22 mEq/L (22 mmol/L) Albumin: 3.8 mg/dL (38 g/L) Urea nitrogen: 8 mg/dL (2.86 mmol/L) Creatinine: 2.1 mg/dL (0.185 mmol/L) Uric acid: 5.8 mg/dL (0.34 mmol/L) Calcium: 8.9 mg/dL (2.22 mmol/L) Glucose: 106 mg/dL (5.89 mmol/L) Total cholesterol: 254 mg/dL (5.57 mmol/L) Low-density lipoprotein: 58 mg/dL (1.5 mmol/L) High-density lipoprotein: 77 mg/dL (2.0 mmol/L) Triglycerides: 159 mg/dL (1.8 mmol/L) The patient is concerned about pneumococcal infection and has never been vaccinated against pneumococcus. He should receive pneumococcal vaccination today. Which of the following statements regarding contraindications to pneumococcal vaccination in this patient is correct?
Practice by Chapter
Antiparasitic drugs (antiprotozoals)
Practice Questions
Antimalarial medications
Practice Questions
Anthelmintics
Practice Questions
Antiseptics and disinfectants
Practice Questions
Antimicrobial stewardship principles
Practice Questions
Empiric antimicrobial selection
Practice Questions
Antimicrobial dosing in special populations
Practice Questions
Antimicrobial pharmacokinetics/pharmacodynamics
Practice Questions
Antimicrobial toxicities
Practice Questions
Antimicrobial allergies and cross-reactivity
Practice Questions
Combination antimicrobial therapy
Practice Questions
Cost-effective antimicrobial strategies
Practice Questions
New antimicrobial development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
