Antimicrobials — MCQs

On this page
A 4-year-old boy is brought by his mother to the emergency room for malaise, dizziness, and sleepiness. The mother owns a dry cleaning shop and found her son in the back room with an open canister of carbon tetrachloride, one of their cleaning fluids. The boy reports feeling nauseous and has a mild headache. He has a history of spastic hemiplegic cerebral palsy and is seen regularly by a pediatric neurologist. He is otherwise healthy and takes no medications. His temperature is 98.6°F (37°C), blood pressure is 105/55 mmHg, pulse is 105/min, and respirations are 22/min. On exam, he appears tired and drowsy but is able to answer questions. He has increased tone in his left upper and lower extremities. Which of the following is most likely to be affected by this patient's exposure to the dry cleaning fluid?
A 2-week-old boy presents to the pediatrics clinic. The medical records note a full-term delivery, however, the boy was born with chorioretinitis and swelling and calcifications in his brain secondary to an in utero infection. In immunocompromised patients, a drug can be used for prophylaxis against the pathogen responsible for this neonate's findings. This same drug also provides protection against which other microorganism?
At 10 a.m. this morning, a semi-truck carrying radioactive waste toppled over due to a blown tire. One container was damaged, and a small amount of its contents leaked into the nearby river. You are a physician on the government's hazardous waste committee and must work to alleviate the town's worries and minimize the health hazards due to the radioactive leak. You decide to prescribe a prophylactic agent to minimize any retention of radioactive substances in the body. Which of the following do you prescribe?
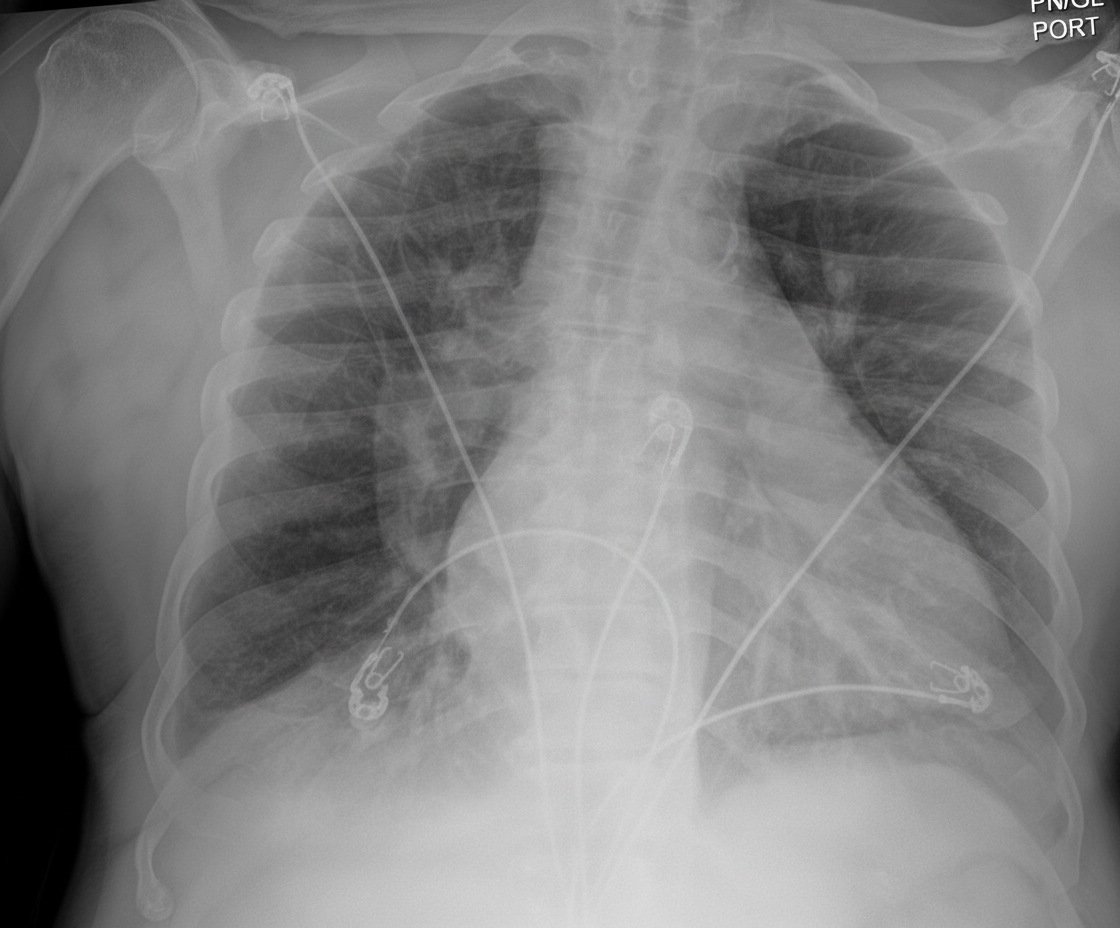
A 25-year-old male graduate student is brought to the emergency department for respiratory distress after he was found by his roommate coughing and severely short of breath. He was diagnosed with HIV infection 3 months ago but is not compliant with his antiretroviral therapy. He is from Chile and moved here 5 years ago. He appears unwell and is unable to speak in full sentences. His temperature is 38.2°C (100.7°F), pulse is 127/min, respirations are 32/min, and blood pressure is 95/65 mm Hg. Pulse oximetry shows an oxygen saturation of 86% on room air. No oral thrush is seen. The patient is placed on supplemental oxygen. Serum studies show: Lactate dehydrogenase 364 IU/L CD4 cell count 98/mm3 Beta-D-glucan elevated Arterial blood gas analysis shows: pH 7.50 PaCO2 22 mm Hg PaO2 60 mm Hg HCO3 20 mEq/L An x-ray of the chest is shown. Standard antibiotic therapy is begun immediately. The most appropriate next step in management is administration of which of the following?
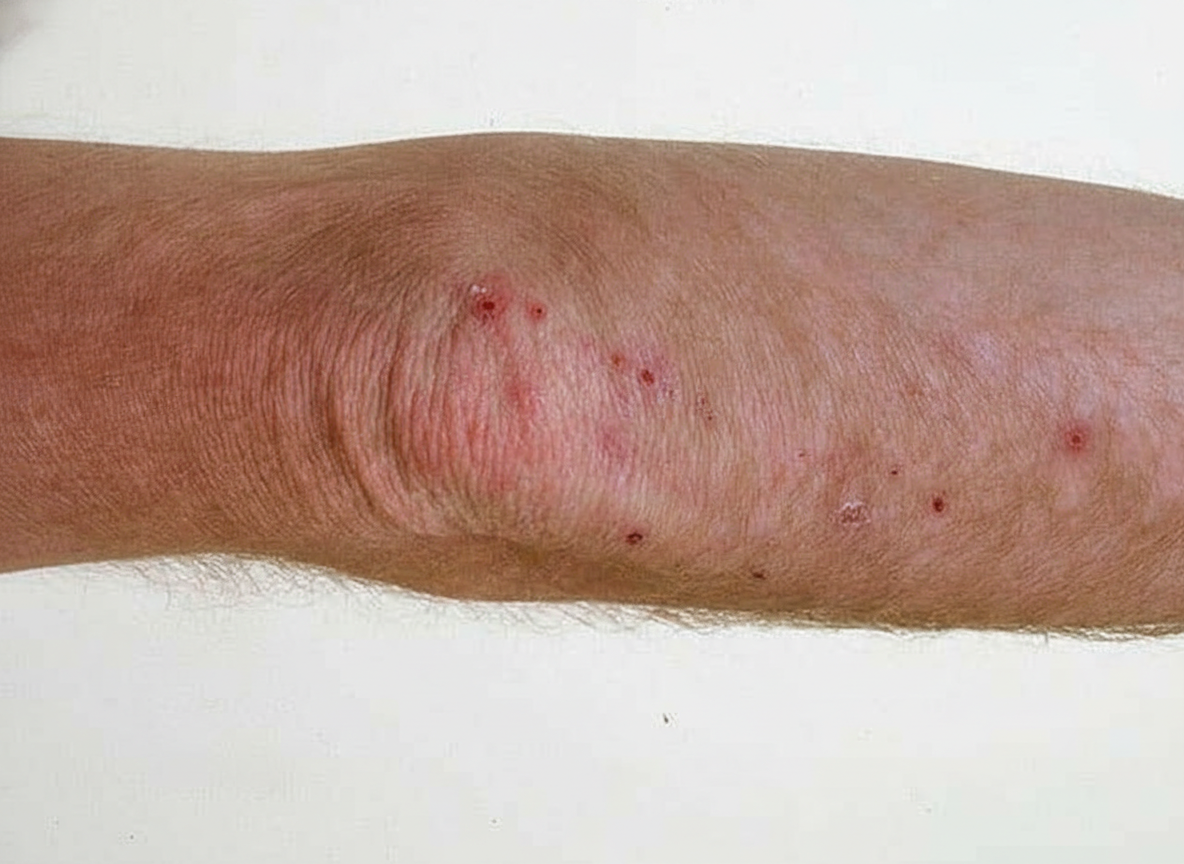
A 22-year-old man comes to the physician for the evaluation of a skin rash over both of his shoulders and elbows for the past 5 days. The patient reports severe itching and burning sensation. He has no history of serious illness except for recurrent episodes of diarrhea and abdominal cramps, which have occurred every once in a while over the past three months. He describes his stools as greasy and foul-smelling. He does not smoke or drink alcohol. He does not take illicit drugs. He takes no medications. He is 180 cm (5 ft 11 in) tall and weighs 60 kg (132 lb); BMI is 18.5 kg/m2. His temperature is 37°C (98.6°F), pulse is 70/min, and blood pressure is 110/70 mm Hg. Physical examination shows a symmetrical rash over his shoulders and knees. A photograph of the rash on his left shoulder is shown. Rubbing the affected skin does not lead to upper epidermal layer separation from the lower layer. His hemoglobin concentration is 10.2 g/dL, mean corpuscular volume is 63.2 μm3, and platelet count is 450,000/mm3. Which of the following is the most appropriate pharmacotherapy for this skin condition?
A 45-year-old woman presents to the emergency department with fever, cough, tonsillar enlargement, and bleeding lips. She has a diffuse blistering rash that encompasses the palms and soles of her feet, in total covering 55% of her total body surface area (TBSA). The upper epidermal layer easily slips away with slight rubbing. Within 24 hours the rash progresses to 88% TBSA involvement and the patient requires mechanical ventilation for respiratory distress. Which of the following is the most likely etiology of this patient’s condition?
A 28-year-old man comes to the physician for the evaluation of a progressively worsening tremor in his hands and multiple falls over the past 3 months. The tremor occurs both at rest and with movement. He also reports decreased concentration and a loss of interest in his normal activities over this time period. He has no history of serious medical illness and takes no medications. He drinks two alcoholic beverages daily and does not use illicit drugs. Vital signs are within normal limits. Physical exam shows mild jaundice, a flapping tremor, and a broad-based gait. Serum studies show: Aspartate aminotransferase 554 U/L Hepatitis B surface antibody positive Hepatitis B surface antigen negative Ceruloplasmin 5.5 mg/dL (normal: 19.0-31.0 mg/dL) Which of the following is the most appropriate pharmacotherapy for this patient?
A 56-year-old woman comes to the physician with a 6-month history of black spots in her vision. She has been unable to drive at night for the past 4 months. The patient has rheumatoid arthritis, type 2 diabetes mellitus, and depression. Her mother has glaucoma. She has never smoked. She drinks one or two glasses of homemade moonshine every day after dinner. Current medications include metformin, citalopram, and chloroquine. She is 168 cm (5 ft 6 in) tall and weighs 79 kg (174 lb); BMI is 28 kg/m2. Her temperature is 36.8°C (98.2°F), pulse is 68/min, and blood pressure is 138/83 mm Hg. Examination shows swan neck deformities of both hands. The patient's vision is 20/20 in both eyes. She has difficulty adapting to changes in lighting in both eyes. Slit lamp examination shows a normal anterior segment. The posterior segment shows bilateral bull's eye macular lesions. Hemoglobin 11.7 g/dL Mean corpuscular volume 98 μm3 Serum Alkaline phosphatase 65 U/L Aspartate aminotransferase (AST, GOT) 20 U/L Alanine aminotransferase (ALT, GPT) 17 U/L γ-Glutamyltransferase (GGT) 90 U/L (N=5–50 U/L) Which of the following is the most likely cause of this patient's symptoms?
A 74-year-old woman presents to the emergency department for shortness of breath and bilateral lower extremity pitting edema. She has had exacerbations like this in the past and notes that she has not been taking her home heart medications as scheduled. Review of systems is negative for any other symptoms including GI, urinary, and musculoskeletal symptoms. Physical exam reveals bilateral pulmonary crackles, lower extremity pitting edema that extends to the hip, and no abdominal tenderness. Neurological exam is unremarkable and the patient is at her baseline mental status. She is subsequently started on BiPAP, given furosemide, and admitted to the hospital. Routine admission workup includes urinalysis, which shows >100,000 cfu/mL of E. coli. She has no known drug allergies. Which of the following is the most appropriate treatment for this patient for this finding?
A 15-year-old boy with Down syndrome is admitted to the hospital because of a 2-week history of pallor, easy bruising, and progressive fatigue. He has a history of acute lymphoblastic leukemia that has been in remission for 2 years. Examination shows cervical and axillary lymphadenopathy. Bone marrow biopsy predominantly shows immature cells that stain positive for terminal deoxynucleotidyl transferase. A diagnosis of relapsed acute lymphoblastic leukemia is made. Treatment with a combination chemotherapeutic regimen including teniposide is initiated. The effect of this drug is best explained by which of the following mechanisms of action?
Practice by Chapter
Antiparasitic drugs (antiprotozoals)
Practice Questions
Antimalarial medications
Practice Questions
Anthelmintics
Practice Questions
Antiseptics and disinfectants
Practice Questions
Antimicrobial stewardship principles
Practice Questions
Empiric antimicrobial selection
Practice Questions
Antimicrobial dosing in special populations
Practice Questions
Antimicrobial pharmacokinetics/pharmacodynamics
Practice Questions
Antimicrobial toxicities
Practice Questions
Antimicrobial allergies and cross-reactivity
Practice Questions
Combination antimicrobial therapy
Practice Questions
Cost-effective antimicrobial strategies
Practice Questions
New antimicrobial development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
