Antimicrobials — MCQs

On this page
A 36-year-old male with fluctuating levels of consciousness is brought to the emergency department by ambulance due to a fire in his home. He currently opens his eyes to voice, localizes painful stimuli, responds when asked questions, but is disoriented and cannot obey commands. The patient’s temperature is 99°F (37.2°C), blood pressure is 86/52 mmHg, pulse is 88/min, and respirations are 14/min with an oxygen saturation of 97% O2 on room air. Physical exam shows evidence of soot around the patient’s nose and mouth, but no burns, airway obstruction, nor accessory muscle use. A blood lactate is 14 mmol/L. The patient is started on intravenous fluids. What is the next best step in management?
A 62-year-old woman presents with abdominal pain and blood in her urine. Since the acute onset of symptoms 3 days ago, there has been no improvement. She describes the pain as moderate, sharp and burning in character, non-radiating, and localized to the suprapubic region. She also has noted some mild urinary frequency and urgency for the past 5 days, which has been getting progressively worse. She denies any flank pain, fever, chills, night sweats, dysuria, or pain on urination. The patient has a history of an abdominal leiomyosarcoma, which was diagnosed 6 months ago. The course of her disease is complicated by hepatic metastases, for which she recently started receiving a new therapy. The patient reports a 15-pack-year smoking history, but no alcohol or recreational drug use. Her temperature is 37.0℃ (98.6℉), pulse is 84/min, respiratory rate is 18/min, and blood pressure is 110/75 mm Hg. On physical examination, there is some mild suprapubic tenderness to palpation. The remainder of the exam is unremarkable. Laboratory findings include a mild leukopenia of 3,000/mm3. A urine dipstick reveals 3+ blood. Which of the following best describes the medication that could have prevented this patient’s symptoms?
A 38-year-old woman presents to her primary care physician for a new patient appointment. She states that she feels well and has no current complaints. The patient recently started seeing a specialist for treatment for another medical condition but otherwise has had no medical problems. The patient lives alone and drinks 2 alcoholic beverages every night. She has had 3 sexual partners in her lifetime, uses oral contraceptive pills for contraception, and has never been pregnant. Physical exam reveals a pleasant, obese woman with normal S1 and S2 on cardiac exam. Musculoskeletal exam reveals swelling of the MCP and PIP joints of the hands as well as ulnar deviation of the fingers. Laboratory tests are ordered and results are below: Serum: Na+: 139 mEq/L Cl-: 100 mEq/L K+: 4.3 mEq/L HCO3-: 25 mEq/L BUN: 20 mg/dL Glucose: 99 mg/dL Creatinine: 1.1 mg/dL Ca2+: 10.2 mg/dL AST: 95 U/L ALT: 68 U/L Which of the following best explains this patient's abnormal laboratory values?
A 67-year-old man comes to the physician for a follow-up examination after he was diagnosed with mantle cell lymphoma. The physician recommends a chemotherapeutic regimen containing bortezomib. Which of the following best describes the effect of this drug?
A 55-year-old man with a history of fatigue and exertional dyspnea presents to the urgent care clinic following an acute upper respiratory illness. On physical examination, his pulses are bounding, his complexion is very pale, and scleral icterus is apparent. The spleen is moderately enlarged. Oxygen saturation is 79% at rest, with a new oxygen requirement of 9 L by a non-rebreather mask. Laboratory analysis results show a hemoglobin level of 6.8 g/dL. Of the following options, which hypersensitivity reaction does this condition represent?
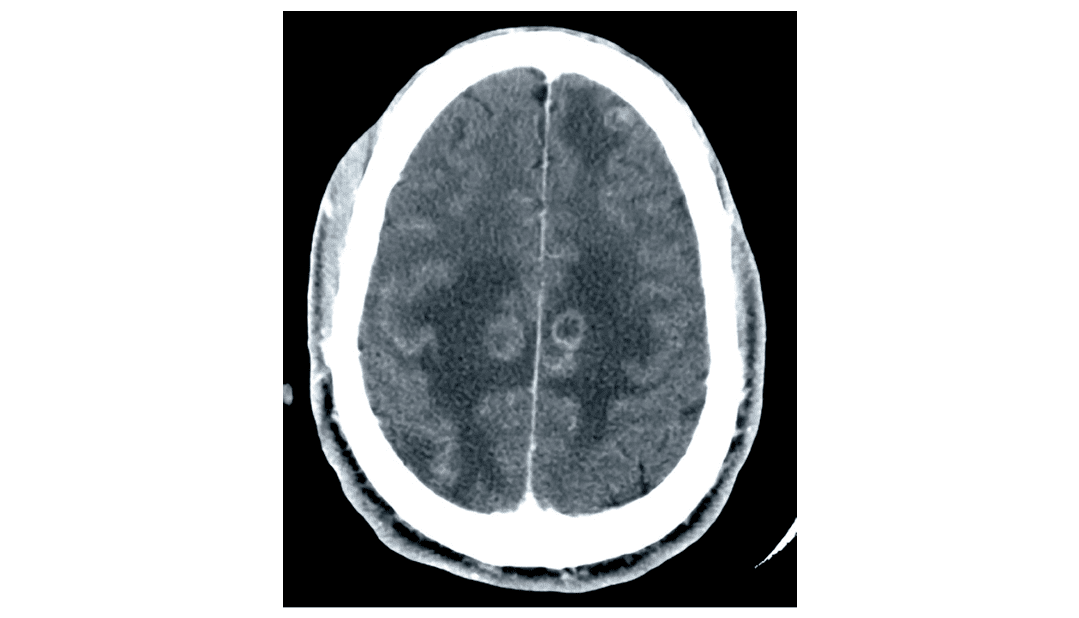
A 35-year-old man is brought to the emergency department after experiencing a seizure. According to his girlfriend, he has had fatigue for the last 3 days and became confused this morning, after which he started having uncontrollable convulsions throughout his entire body. He was unconscious throughout the episode, which lasted about 4 minutes. He has not visited a physician for over 10 years. He has smoked one pack of cigarettes daily for 12 years. His girlfriend admits they occasionally use heroin together with their friends. His temperature is 38.8°C (101.8°F), pulse is 93/min, respirations are 20/min, and blood pressure is 110/70 mm Hg. The lungs are clear to auscultation and examination shows normal heart sounds and no carotid or femoral bruits. He appears emaciated and somnolent. There are multiple track marks on both his arms. He is unable to cooperate for a neurological exam. Laboratory studies show a leukocyte count of 3,000/mm3, a hematocrit of 34%, a platelet count of 354,000/mm3, and an erythrocyte sedimentation rate of 27 mm/h. His CD4+ T-lymphocyte count is 84/mm3 (normal ≥ 500). A CT scan of the head is shown. Which of the following is the most appropriate next step considering this patient's CT scan findings?
A 56-year-old man of Nepalese origin presents to a clinic complaining of skin rashes that have been troubling him for years. On examination, there are numerous poorly demarcated skin lesions present on all parts of the body. There is also evidence of significant facial thickening, eyebrow loss, and symmetrical sensory neuropathy in a ‘glove and stocking’ distribution. An examination of the hands reveals bilateral weakness. A skin biopsy is taken from one of the lesions, and the culture is positive for acid-fast bacilli. Which of the following pharmacological therapies is involved in the treatment of this condition?
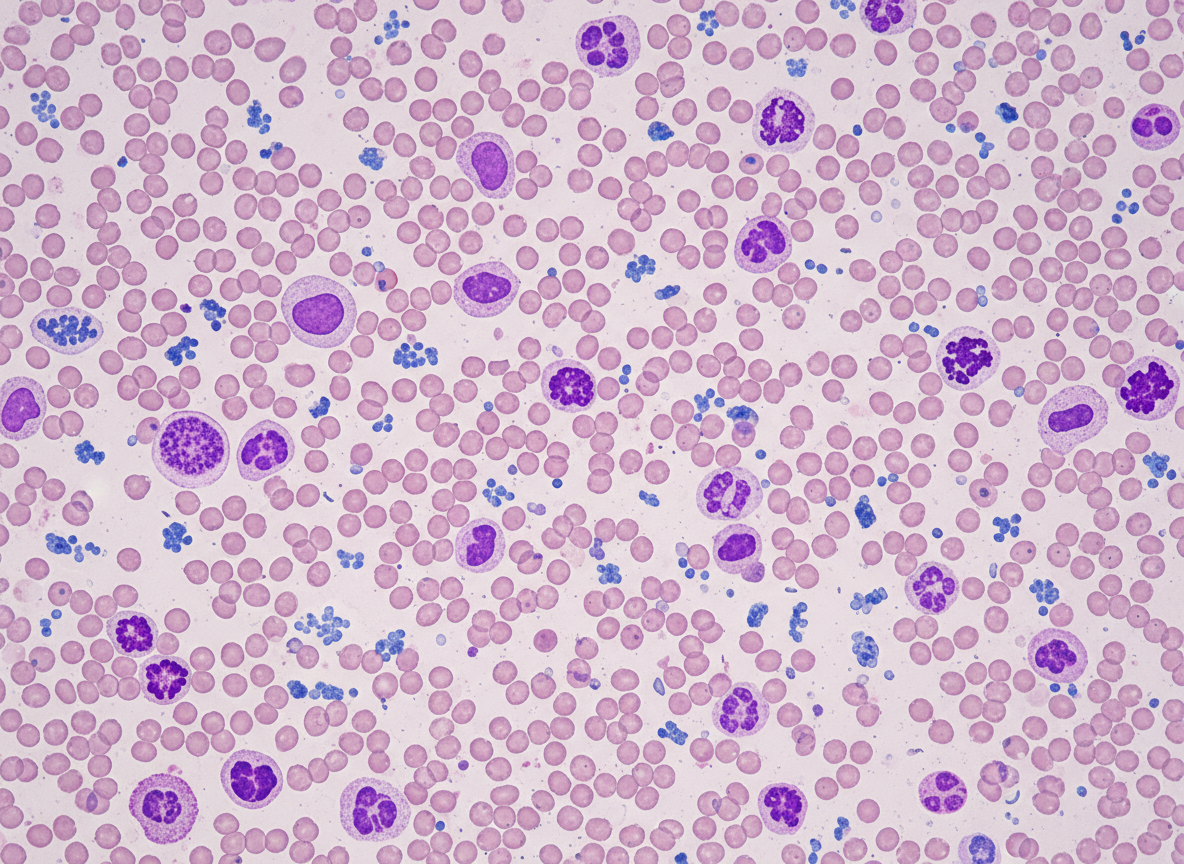
A 64-year-old woman comes to the physician for her routine health maintenance examination. She feels well. She had cervical cancer and received radiotherapy 8 years ago. Her vital signs are within normal limits. On percussion, the spleen size is 15 cm. Otherwise, the physical examination shows no abnormalities. The laboratory test results are as follows: Hemoglobin 10 g/dL Mean corpuscular volume 88 μm3 Leukocyte count 65,000/mm3 Platelet count 500,000/mm3 Two images of the peripheral blood smear are shown on the image. Which of the following is the most appropriate next step in management?
A 65-year-old female patient with a past medical history of diabetes mellitus and an allergy to penicillin develops an infected abscess positive for MRSA on the third day of her hospital stay. She is started on an IV infusion of vancomycin at a dose of 1000 mg every 12 hours. Vancomycin is eliminated by first-order kinetics and has a half life of 6 hours. The volume of distribution of vancomycin is 0.5 L/kg. Assuming no loading dose is given, how long will it take for the drug to reach 94% of its plasma steady state concentration?
A 55-year-old man presents to the urgent clinic complaining of pain in his right foot. He reported that the pain is intense that he had to remove his shoe and sock, and rates the pain level as 6 out of 10. He does not report trauma or recent infection. The past medical history includes hypertension. The medications include hydrochlorothiazide, enalapril, and a daily multivitamin. The family history is noncontributory. He consumes alcohol in moderation. His diet mostly consists of red meat and white rice. The blood pressure is 137/85 mm Hg, heart rate is 74/min, respiratory rate is 12/min, and the temperature is 36.9°C (98.4°F). The physical examination demonstrates swelling, redness, and tenderness to palpation in the first metatarsophalangeal joint of his right foot. There are no skin lesions. The rest of the patient’s examination is normal. An arthrocentesis procedure is scheduled. Which of the following is the most likely pharmacological treatment for the presented patient?
Practice by Chapter
Antiparasitic drugs (antiprotozoals)
Practice Questions
Antimalarial medications
Practice Questions
Anthelmintics
Practice Questions
Antiseptics and disinfectants
Practice Questions
Antimicrobial stewardship principles
Practice Questions
Empiric antimicrobial selection
Practice Questions
Antimicrobial dosing in special populations
Practice Questions
Antimicrobial pharmacokinetics/pharmacodynamics
Practice Questions
Antimicrobial toxicities
Practice Questions
Antimicrobial allergies and cross-reactivity
Practice Questions
Combination antimicrobial therapy
Practice Questions
Cost-effective antimicrobial strategies
Practice Questions
New antimicrobial development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
