Antimicrobials — MCQs

On this page
A 4-year-old boy is brought to the physician by his mother because of left-sided neck swelling that has slowly progressed over the past 4 weeks. He has no history of serious illness. Temperature is 38°C (100.4°F). Physical examination shows a non-tender, mobile mass in the left submandibular region with overlying erythema. A biopsy of the mass shows caseating granulomas. Pharmacotherapy with azithromycin and ethambutol is initiated. This patient is most likely to experience which of the following adverse effects related to ethambutol use?
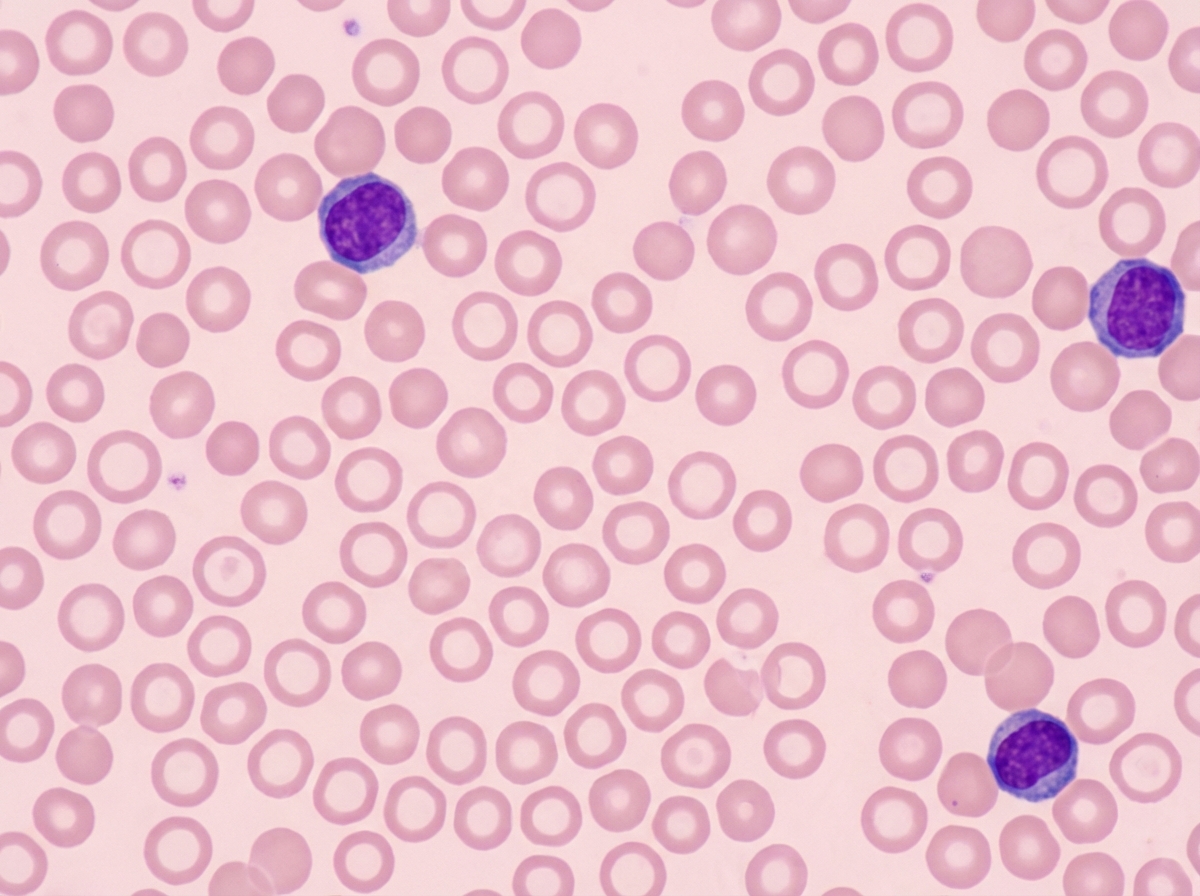
A 47-year-old woman with a history of recent gastric bypass surgery presents for a follow-up visit. 8 months ago, she underwent gastric bypass surgery because she was struggling with maintaining her BMI below 42 kg/m². She previously weighed 120 kg (265 lb), and now she weighs 74.8 kg (165 lb). She says that she has low energy and is easily fatigued. These symptoms have become progressively worse over the past month. She is struggling to get through the day and sometimes has to nap before she can continue with her work. She has also recently noticed that she gets cramps in her legs, especially after a long day. The patient is afebrile and vital signs are within normal limits. Physical examination is unremarkable. Her hemoglobin is 9.5 mg/dL with an MCV of 75 fl. Her peripheral smear is shown in the exhibit. Which of the following supplements would most likely improve this patient’s symptoms?
A 62-year-old man is brought to the emergency department from a senior-care facility after he was found with a decreased level of consciousness and fever. His personal history is relevant for colorectal cancer that was managed with surgical excision of the tumor. Upon admission, he is found to have a blood pressure of 130/80 mm Hg, a pulse of 102/min, a respiratory rate of 20/min, and a body temperature 38.8°C (101.8°F). There is no rash on physical examination; he is found to have neck rigidity, confusion, and photophobia. There are no focal neurological deficits. A head CT is normal without mass or hydrocephalus. A lumbar puncture was performed and cerebrospinal fluid (CSF) is sent to analysis while ceftriaxone and vancomycin are started. Which of the following additional antimicrobials should be added in the management of this patient?
A 72-year-old man has been recently diagnosed with stage 3 squamous cell carcinoma of the oral cavity. After the necessary laboratory workup, concurrent chemoradiation therapy has been planned. Radiation therapy is planned to take place over 7 weeks and he will receive radiation doses daily, Monday–Friday, in 2.0 Gy fractions. For concurrent chemotherapy, he will receive intravenous cisplatin at a dosage of 50 mg/m2 weekly for 7 weeks. Which of the following best explains the mechanism of action of the antineoplastic drug that the patient will receive?
A 66-year-old man comes to the physician because of a 3-month history of constipation and streaks of blood in his stool. He has had a 10-kg (22-lb) weight loss during this period. Colonoscopy shows an exophytic tumor in the sigmoid colon. A CT scan of the abdomen shows liver metastases and enlarged mesenteric and para-aortic lymph nodes. A diagnosis of stage IV colorectal cancer is made, and palliative chemotherapy is initiated. The chemotherapy regimen includes a monoclonal antibody that inhibits tumor growth by preventing ligand binding to a protein directly responsible for epithelial cell proliferation and organogenesis. Which of the following proteins is most likely inhibited by this drug?
A 65-year-old male with diffuse large B cell lymphoma is treated with a chemotherapy regimen including 6-mercaptopurine. Administration of which of the following agents would increase this patient’s risk for mercaptopurine toxicity?
A 40-year-old woman comes to the physician for the evaluation of a 4-month history of reddening of the nose and cheeks. She has no itching or pain. She first noticed the redness while on a recent holiday in Spain, where she stayed at the beach and did daily wine tastings. She has tried several brands of sunscreen, stopped going outside in the middle of the day, and has not drunk alcohol since her trip, but the facial redness persists. She has no history of serious illness. Her younger sister has acne vulgaris, and her mother has systemic lupus erythematosus. The patient reports that she has had a lot of stress lately due to relationship problems with her husband. She does not smoke. Her vital signs are within normal limits. Examination shows erythema of the nose, chin, and medial cheeks with scant papules and telangiectasias. There are no comedones or blisters. The remainder of the examination shows no abnormalities. In addition to behavioral modifications, which of the following is the most appropriate initial treatment?
A 49-year-old man presents with an 11-month history of progressive fatigue. He denies any night sweats, weight loss, abdominal pain, nausea, vomiting, change in bowel habits, or bleeding. He has no significant past medical history. His vital signs include: temperature 37.0°C (98.6°F), blood pressure 119/81 mm Hg, pulse 83/min, and respiratory rate 19/min. On physical examination, mild splenomegaly is noted on abdominal percussion. Laboratory findings are significant for a leukocyte count of 16,700/mm3 and a low serum leukocyte alkaline phosphatase (LAP) score. A bone marrow biopsy is performed, which shows marked hypercellularity with a clear dominance of granulocytes. Cytogenetic analysis is positive for the Ph1 gene. Which of the following is the best course of treatment for this patient?
A 20-year-old college student is brought to the ED after a motor vehicle accident. Primary and secondary surveys reveal no significant compromise to his airway, his cardiovascular system, or to his motor function. However, his conjunctiva appear injected and he maintains combative behavior towards staff. What is the gold standard confirmatory test for substance use?
A hospitalized 45-year-old man has had mild flank pain since awakening 3 hours ago. He also reports a new generalized rash. Two weeks ago, he was diagnosed with pulmonary tuberculosis. Current medications include isoniazid, pyrazinamide, rifampin, ethambutol, and pyridoxine. His temperature is 38.3°C (100.9°F), pulse is 74/min, and blood pressure is 128/72 mm Hg. Examination of the skin shows diffuse erythema with confluent papules. There is no costovertebral angle tenderness. Laboratory studies show: Leukocyte count 9,800/mm3 Segmented neutrophils 59% Bands 3% Eosinophils 4% Lymphocytes 29% Monocytes 5% Serum Urea nitrogen 25 mg/dL Creatinine 1.9 mg/dL Urine WBC 8–10/hpf Eosinophils numerous RBC 5–6/hpf RBC casts negative WBC casts numerous In addition to intravenous fluid resuscitation, which of the following is the most appropriate next step in management?
Practice by Chapter
Antiparasitic drugs (antiprotozoals)
Practice Questions
Antimalarial medications
Practice Questions
Anthelmintics
Practice Questions
Antiseptics and disinfectants
Practice Questions
Antimicrobial stewardship principles
Practice Questions
Empiric antimicrobial selection
Practice Questions
Antimicrobial dosing in special populations
Practice Questions
Antimicrobial pharmacokinetics/pharmacodynamics
Practice Questions
Antimicrobial toxicities
Practice Questions
Antimicrobial allergies and cross-reactivity
Practice Questions
Combination antimicrobial therapy
Practice Questions
Cost-effective antimicrobial strategies
Practice Questions
New antimicrobial development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
