Antimicrobials — MCQs

On this page
A 33-year-old man is being evaluated for malaise and fatigability. He says that he hasn’t been able to perform at work, can’t exercise like before, and is constantly tired. He also says that his clothes have ‘become larger’ in the past few months. Past medical history is significant for gastroesophageal reflux disease, which is under control with lifestyle changes. His blood pressure is 110/70 mm Hg, the temperature is 37.0°C (98.6°F), the respiratory rate is 17/min, and the pulse is 82/min. On physical examination, an enlarged, painless, mobile, cervical lymph node is palpable. A complete blood count is performed. Hemoglobin 9.0 g/dL Hematocrit 37.7% Leukocyte count 5,500/mm3 Neutrophils 65% Lymphocytes 30% Monocytes 5% Mean corpuscular volume 82.2 μm3 Platelet count 190,000 mm3 Erythrocyte sedimentation rate 35 mm/h C-reactive protein 8 mg/dL A biopsy of the lymph node is performed which reveals both multinucleated and bilobed cells. The patient is started on a regimen of drugs for his condition. Echocardiography is performed before treatment is started and shows normal ejection fraction, ventricle function, and wall motion. After 2 rounds of chemotherapy, another echocardiography is performed by protocol, but this time all heart chambers are enlarged, and the patient is suffering from severe exertion dyspnea. Which of the drugs below is most likely responsible for these side effects?
A 41-year-old man presents to the emergency department with several days of hand tremor, vomiting, and persistent diarrhea. His wife, who accompanies him, notes that he seems very “out of it.” He was in his usual state of health last week and is now having difficulties at work. He has tried several over-the-counter medications without success. His past medical history is significant for bipolar disorder and both type 1 and type 2 diabetes. He takes lithium, metformin, and a multivitamin every day. At the hospital, his heart rate is 90/min, respiratory rate is 17/min, blood pressure is 130/85 mm Hg, and temperature is 37.0°C (98.6°F). The man appears uncomfortable. His cardiac and respiratory exams are normal and his bowel sounds are hyperactive. His lithium level is 1.8 mEq/L (therapeutic range, 0.6–1.2 mEq/L). Which of the following may have contributed to this patient’s elevated lithium level?
A 47-year-old female with a history of poorly controlled type I diabetes mellitus and end-stage renal disease undergoes an allogeneic renal transplant. Her immediate post-operative period is unremarkable and she is discharged from the hospital on post-operative day 4. Her past medical history is also notable for major depressive disorder, obesity, and gout. She takes sertraline, allopurinol, and insulin. She does not smoke or drink alcohol. To decrease the risk of transplant rejection, her nephrologist adds a medication known to serve as a precursor to 6-mercaptopurine. Following initiation of this medication, which of the following toxicities should this patient be monitored for?
A 58-year-old woman comes to the physician for evaluation of worsening fatigue for 1 week. She also has a 1-year history of hand pain and stiffness. Four months ago, she started a new medication for these symptoms. Medications used prior to that included ibuprofen, prednisone, and hydroxychloroquine. Examination shows a subcutaneous nodule on her left elbow and old joint destruction with Boutonniere deformity. Her hemoglobin concentration is 10.1 g/dL, leukocyte count is 3400/mm3, and platelet count is 101,000/mm3. Methylmalonic acid levels are normal. Which of the following could have prevented this patient's laboratory abnormalities?
A 46-year-old woman comes to the physician because of a 3-day history of diarrhea and abdominal pain. She returned from a trip to Egypt 4 weeks ago. Her vital signs are within normal limits. There is mild tenderness in the right lower quadrant. Stool studies show occult blood and unicellular organisms with engulfed erythrocytes. Which of the following is the most appropriate initial pharmacotherapy for this patient?
A previously healthy 5-year-old boy is brought to the emergency department because of abdominal pain and vomiting for 6 hours. His mother immediately brought him after noticing that he had gotten into the medicine cabinet. He appears uncomfortable. His temperature is 37.2°C (99°F), pulse is 133/min and blood pressure is 80/50 mm Hg. Examination shows diffuse abdominal tenderness; there is no guarding or rigidity. Digital rectal examination shows dark-colored stools. Laboratory studies show: Hemoglobin 13.2 g/dL Leukocyte count 14,100/mm3 Serum Na+ 136 mEq/L K+ 3.3 mEq/L Cl- 105 mEq/L Urea nitrogen 26 mg/dL Glucose 98 mg/dL Creatinine 1.1 mg/dL Arterial blood gas analysis on room air shows: pH 7.31 pCO2 32 mm Hg HCO3- 16 mEq/L Intravenous fluids are administered. Which of the following is the most appropriate next step in management?
A 33-year-old man presents to the emergency room for diarrhea. He states it is profuse and watery and has not been improving over the past week. He is generally healthy; however, he was recently hospitalized during spring break and treated for alcohol intoxication and an aspiration pneumonia. While on spring break, the patient also went camping and admits eating undercooked chicken and drinking from mountain streams. His temperature is 100.5°F (38.1°C), blood pressure is 111/74 mmHg, pulse is 110/min, respirations are 16/min, and oxygen saturation is 98% on room air. Physical exam is notable for a fatigued appearing man. His abdomen is non-tender. Which of the following is the best management of this patient?
A 45-year-old man presents with worsening joint pain and stiffness. Past medical history is significant for rheumatoid arthritis, diagnosed 3 months ago and managed with celecoxib and methotrexate, and occasional gastric reflux, managed with omeprazole. His vitals are a pulse of 80/min, a respiratory rate of 16/min, and blood pressure of 122/80 mm Hg. On physical examination, the left wrist is swollen, stiff, and warm to touch, and the right wrist is red and warm. There is limited active and passive range of motion at the proximal interphalangeal and metacarpophalangeal joints of both hands. The remainder of the examination is unremarkable. A plain radiograph of the hands shows progressive degeneration of multiple joints. Another drug, etanercept, is added to help control progressive arthritis. Which of the following diagnostic tests should be ordered before starting this new medication in this patient?
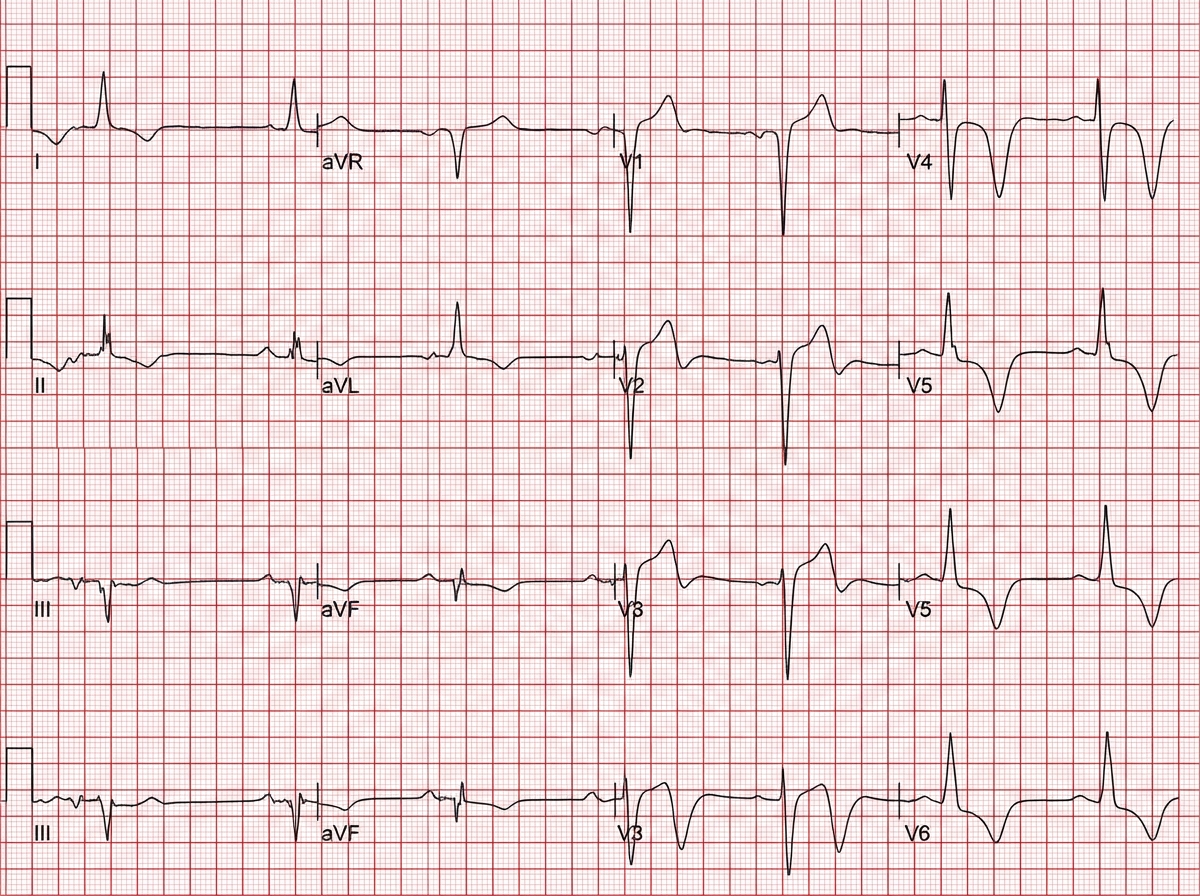
A 54-year-old man with a past medical history significant for hypertension, type 2 diabetes, and chronic obstructive pulmonary disease presents with complaints of nausea and abdominal pain for the past month. The pain is located in the epigastric region and is described as “burning” in quality, often following food intake. The patient denies any changes in bowel movements, fever, or significant weight loss. Medications include metformin, lisinopril, hydrochlorothiazide, albuterol inhaler, and fluconazole for a recent fungal infection. Physical examination was unremarkable except for a mildly distended abdomen that is diffusely tender to palpation and decreased sensation at lower extremities bilaterally. A medication was started for the symptoms. Two days later, the patient reports heart palpitations. An EKG is shown below. Which of the following is the medication most likely prescribed?
Several weeks after starting a new medication for rheumatoid arthritis, a 44-year-old woman comes to the physician because of painful ulcers in her mouth. Oral examination shows inflammation and swelling of the tongue and oropharynx and ulcers on the buccal mucosa bilaterally. Skin examination shows soft tissue swelling over her proximal interphalangeal joints and subcutaneous nodules over her elbows. Serum studies show an alanine aminotransferase level of 220 U/L, aspartate aminotransferase level of 214 U/L, and creatinine level of 1.7 mg/dL. Which of the following is the most likely primary mechanism of action of the drug she is taking?
Practice by Chapter
Antiparasitic drugs (antiprotozoals)
Practice Questions
Antimalarial medications
Practice Questions
Anthelmintics
Practice Questions
Antiseptics and disinfectants
Practice Questions
Antimicrobial stewardship principles
Practice Questions
Empiric antimicrobial selection
Practice Questions
Antimicrobial dosing in special populations
Practice Questions
Antimicrobial pharmacokinetics/pharmacodynamics
Practice Questions
Antimicrobial toxicities
Practice Questions
Antimicrobial allergies and cross-reactivity
Practice Questions
Combination antimicrobial therapy
Practice Questions
Cost-effective antimicrobial strategies
Practice Questions
New antimicrobial development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
