Antimicrobials — MCQs

On this page
An experimental drug, ES 62, is being studied. It prohibits the growth of vancomycin-resistant Staphylococcus aureus. It is highly lipid-soluble. The experimental design is dependent on a certain plasma concentration of the drug. The target plasma concentration is 100 mmol/dL. Which of the following factors is most important for calculating the appropriate loading dose?
A 33-year-old man with recently diagnosed testicular cancer visits his oncologist to discuss the treatment plan. His left testicle was removed after a thorough workup of a lump. A pelvic CT showed no enlarged lymph nodes and a simple orchiectomy and pelvic lymph node dissection was completed. The final diagnosis was stage IB non-seminoma testicular cancer (pT2N0M0). A combination of different chemotherapeutic medications is recommended including bleomycin, etoposide, and cisplatin. Each of the antineoplastic drugs has a different mechanism of action targeting cancer cells. What is the primary mechanism of action of bleomycin in cancer treatment?
A 32-year-old man presents to an outpatient clinic for tuberculosis prophylaxis before leaving for a trip to Asia, where tuberculosis is endemic. The Mantoux test is positive, but the chest X-ray and AFB sputum culture are negative. He was started on isoniazid. What is the most likely mechanism of resistance to isoniazid?
A 55-year-old man with a history of hypertension and benign prostate hyperplasia presents for follow-up 4 days into the treatment of a urinary tract infection with trimethoprim-sulfamethoxazole. His symptoms have resolved, and he reports no problems with urination, with the exception of a weak urine stream and hesitancy, which he has had for the past 2 years. At the time of this visit, the patient is afebrile; the blood pressure is 130/88 mm Hg and the heart rate is 80/min. There is no flank tenderness. A urinalysis reveals no leukocytes and is negative for esterase. The urinalysis reveals 2 red blood cells (RBCs)/ high power field (HPF), and there are no casts on urinary sediment analysis. The physician, however, notices the following abnormality: Prior treatment BUN 12 mg/dL Creatinine 1.2 mg/dL Today’s visit BUN 13 mg/dL Creatinine 2.1 mg/dL
A 59-year-old man presents to the health clinic for evaluation of severe itching for the past week. The itching is worse at night while lying in bed. The patient has a past medical history of hyperlipidemia, atrial fibrillation, and colon cancer. The patient takes rivaroxaban, simvastatin, and aspirin. The patient has a surgical history of colon resection, appendectomy, and tonsillectomy. He drinks a 6-pack of beer almost every night of the week. He smokes 2 packs of cigarettes daily and has been living at a homeless shelter for the past 6 months. Examination of the skin shows small crusted sores and superficial, wavy gray lines along the wrists and interdigital spaces of both hands as seen in the image. Small vesicles are also present along with excoriations. Which of the following is the most appropriate treatment option for this patient?
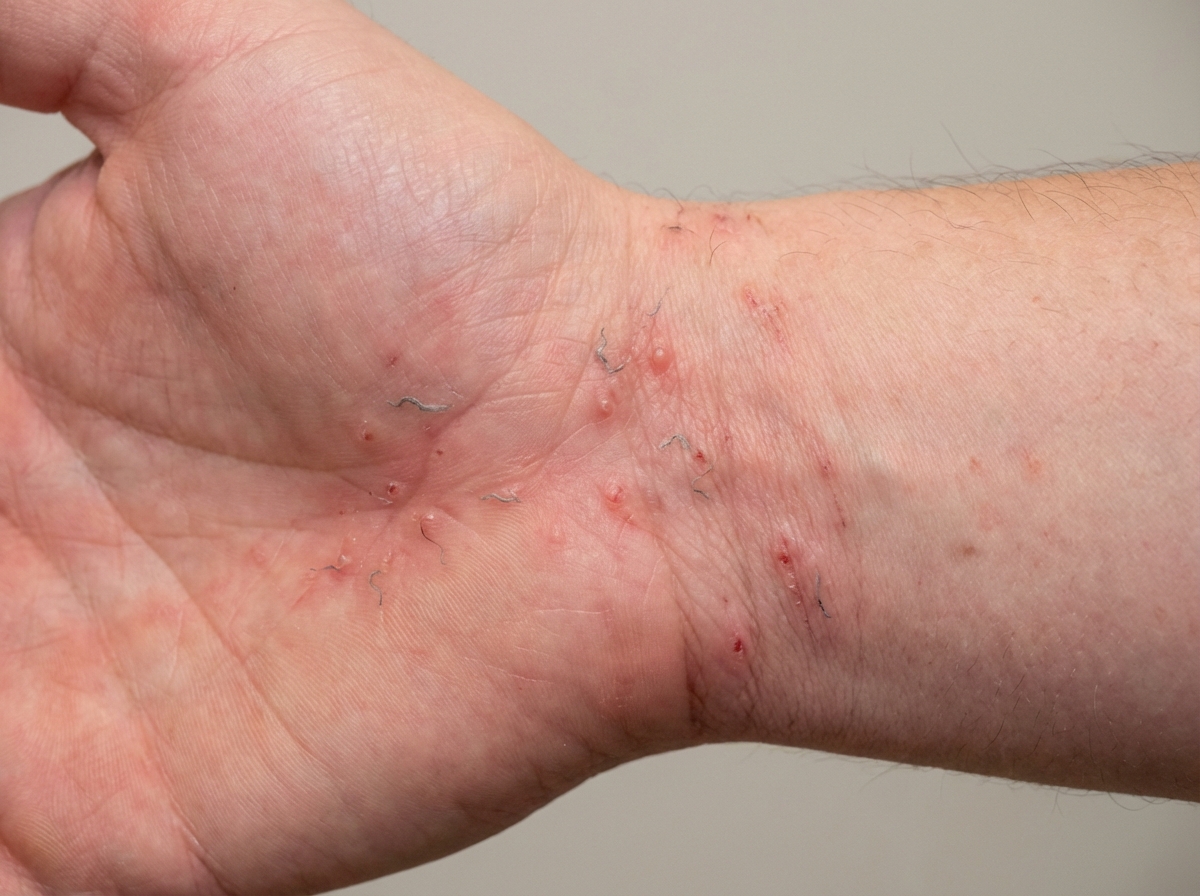
A 56-year-old woman undergoes open reduction and internal fixation of the distal tibia 1 day after a fall. She has had rheumatoid arthritis for 12 years and diabetes mellitus for 2 years. Her medications over the past year have included metformin, prednisone, calcium supplements, and methotrexate. Prior to surgery, insulin was added to her medications, and the dose of prednisone was increased. She has had appropriate nutrition over the years with regular follow-ups with her healthcare professional. Which of the following is the most appropriate supplement to prevent wound failure in this patient?
A 25-year-old woman presented to an urgent care center with a complaint of a cough for more than 3 weeks that was accompanied by night sweats, weight loss, and malaise. On physical examination, the patient had slightly pale palpebral conjunctivae, bilateral posterior cervical lymphadenopathy, but with no adventitious breath sounds in the lung fields bilaterally. The remainder of the physical examination was routine. The patient was started on a drug regimen that was to be taken for 6 months. On follow-up after 2 months, the ALT and AST levels were elevated. Which of the following anti-tubercular drugs could have contributed to this laboratory result?
A 24-year-old man presents to his primary care provider with complaints of 2 days of profuse diarrhea. He states that his stool started to turn watery and lighter in color beginning yesterday, and he has not noticed any fevers. His diarrhea episodes have become more frequent and white-colored over the past day. He has also noticed dry mouth symptoms and darker urine today. He is otherwise healthy but recently returned from a trip with friends to South Asia. None of his friends have reported any symptoms. On exam, his temperature is 98.6°F (37.0°C), blood pressure is 110/68 mmHg, pulse is 80/min, respirations are 14/min. The patient has normal skin turgor, but he has noticeably dry oral mucosa and chapped lips. The patient has dull abdominal aching but no tenderness to palpation. The stool is found to contain large quantities of comma-shaped organisms. Fecal occult blood testing is negative and no steatorrhea is found. The provider recommends immediate oral rehydration therapy. Which of the following is the likely mechanism of this patient’s diarrhea?
A 19-year-old woman presents to the emergency department with chronic diarrhea, fatigue, and weakness. She also had mild lower extremity edema. On examination, she was noted to be pale. Blood testing revealed peripheral eosinophilia (60%) and a Hb concentration of 8 g/dL. The stool examination revealed Fasciolopsis buski eggs. Which of the following drugs would most likely be effective?
A 31-year-old man comes to the physician because of several months of recurrent abdominal pain and diarrhea. Six months ago, he traveled to Lake Superior for a fishing trip with his friends, during which they often ate their day's catch for dinner. Physical examination shows pallor. Laboratory studies show macrocytic anemia with eosinophilia. A peripheral blood smear shows megaloblasts and hypersegmented neutrophils. A cestode infection is suspected and a drug is prescribed that kills cestodes by inducing uncontrollable muscle spasm in the parasite. The drug prescribed for this patient most likely acts by which of the following mechanisms of action?
Practice by Chapter
Antiparasitic drugs (antiprotozoals)
Practice Questions
Antimalarial medications
Practice Questions
Anthelmintics
Practice Questions
Antiseptics and disinfectants
Practice Questions
Antimicrobial stewardship principles
Practice Questions
Empiric antimicrobial selection
Practice Questions
Antimicrobial dosing in special populations
Practice Questions
Antimicrobial pharmacokinetics/pharmacodynamics
Practice Questions
Antimicrobial toxicities
Practice Questions
Antimicrobial allergies and cross-reactivity
Practice Questions
Combination antimicrobial therapy
Practice Questions
Cost-effective antimicrobial strategies
Practice Questions
New antimicrobial development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
