Antimicrobials — MCQs

On this page
A 40-year-old man with AIDS comes to the physician because of a 3-week history of intermittent fever, abdominal pain, and diarrhea. He has also had a nonproductive cough and a 3.6-kg (8-lb) weight loss in this period. He was treated for pneumocystis pneumonia 2 years ago. He has had skin lesions on his chest for 6 months. Five weeks ago, he went on a week-long hiking trip in Oregon. Current medications include efavirenz, tenofovir, and emtricitabine. He says he has had trouble adhering to his medication. His temperature is 38.3°C (100.9°F), pulse is 96/min, and blood pressure is 110/70 mm Hg. Examination shows oral thrush on his palate and a white, non-scrapable plaque on the left side of the tongue. There is axillary and inguinal lymphadenopathy. There are multiple violaceous plaques on the chest. Crackles are heard on auscultation of the chest. Abdominal examination shows mild, diffuse tenderness throughout the lower quadrants. The liver is palpated 2 to 3 cm below the right costal margin, and the spleen is palpated 1 to 2 cm below the left costal margin. Laboratory studies show: Hemoglobin 12.2 g/dL Leukocyte count 4,800/mm3 CD4+ T-lymphocytes 44/mm3 (Normal ≥ 500 mm3) Platelet count 258,000/mm3 Serum Na+ 137 mEq/L Cl- 102 mEq/L K+ 4.9 mEq/L Alkaline phosphatase 202 U/L One set of blood culture grows acid-fast organisms. A PPD skin test shows 4 mm of induration. Which of the following is the most appropriate pharmacotherapy for this patient's condition?
For which patient would isoniazid monotherapy be most appropriate?
A 32-year-old man is admitted to the hospital for evaluation of a 3-month history of insomnia, odynophagia, and irritability. He works in a metal refinery. He appears distracted and irritable. Oral examination shows inflammation of the gums and buccal mucosa with excessive salivation. Neurological examination shows a broad-based gait and an intention tremor in both hands. After treatment with dimercaprol is begun, his symptoms slowly improve. This patient was most likely exposed to which of the following?
A 25-year-old man presents with jaw discomfort and the inability to open his mouth fully for about 3 days. About a week ago, he says he cut himself while preparing a chicken dinner but did not seek medical assistance. Five days after the original injury, he started noticing jaw discomfort and an inability to open his mouth completely. He has no history of a serious illness or allergies and takes no medications. The patient says he had received his primary tetanus series in childhood, and that his last booster was more than 10 years ago. His blood pressure is 125/70 mm Hg and temperature is 36.9℃ (98.5°F). On physical examination, the patient is unable to open his jaw wider than 2.5 cm. Head and neck examinations are otherwise unremarkable. There is a 5 cm linear shallow laceration with some granulation tissue on the right index finger without necrosis, erythema, or pus. After wound care and initiation of metronidazole, which of the following is the next best step in the management of this patient?
A 46-year-old woman presents to her family physician for a general wellness checkup with a chief complaint of high levels of anxiety over the past year. Her anxiety has started to affect her performance at work, making her even more anxious and concerned that she will lose her job. She started psychotherapy several months ago and has experienced minimal improvement in her symptoms from this treatment. The patient is vehemently opposed to beginning any pharmacologic treatment for anxiety; however, she is interested in potential herbal remedies and has started taking kava. She also takes vitamin D, a multivitamin, fish oil, protein powder, and drinks goat milk regularly. The patient works as a commercial sex worker and has a history of IV drug abuse and alcohol abuse which she states she has not used in over a year. She has chronic tension headaches for which she self-administers acetaminophen usually multiple times per day. Her last wellness appointment was unremarkable and these problems are new. Laboratory values are ordered as seen below. Hemoglobin: 13 g/dL Hematocrit: 38% Leukocyte count: 6,870/mm^3 with normal differential Platelet count: 227,000/mm^3 Serum: Na+: 138 mEq/L Cl-: 102 mEq/L K+: 4.1 mEq/L HCO3-: 25 mEq/L BUN: 20 mg/dL Glucose: 111 mg/dL Creatinine: 1.0 mg/dL Ca2+: 10.2 mg/dL AST: 82 U/L ALT: 90 U/L Which of the following is the most likely cause of this patient's lab derangements?
A 29-year-old woman presents to the physician with a blurred vision of her right eye over the past day. She has pain around her right eye during eye movement. She has a history of tingling in her left leg 5 months ago, which spontaneously resolved after 2 weeks. She takes no medications. Her blood pressure is 110/70 mm Hg, the pulse is 72/min, the respirations are 15/min, and the temperature is 36.5℃ (97.7℉). On physical examination, after illumination of the left eye and bilateral pupillary constriction, illumination of the right eye shows pupillary dilation. Fundoscopic examination shows optic disk swelling in the right eye. A color vision test shows decreased perception in the right eye. The remainder of the physical examination shows no abnormalities. A brain MRI shows several foci of hyperintensity in the periventricular and juxtacortical regions. Which of the following is the most appropriate next step in management?
A 25-year-old medical student returns from a volunteer mission trip in Nicaragua with persistent cough and occasional hemoptysis for 3 weeks. A purified protein derivative test revealing a 20 mm wheal and a chest radiograph with hilar lymphadenopathy support a diagnosis of active tuberculosis. The patient is started on appropriate therapy. Among the prescribed medications, one drug inhibits carbohydrate polymerization of the pathogen's cell wall. What is the most likely complaint that the patient may present with because of this drug?
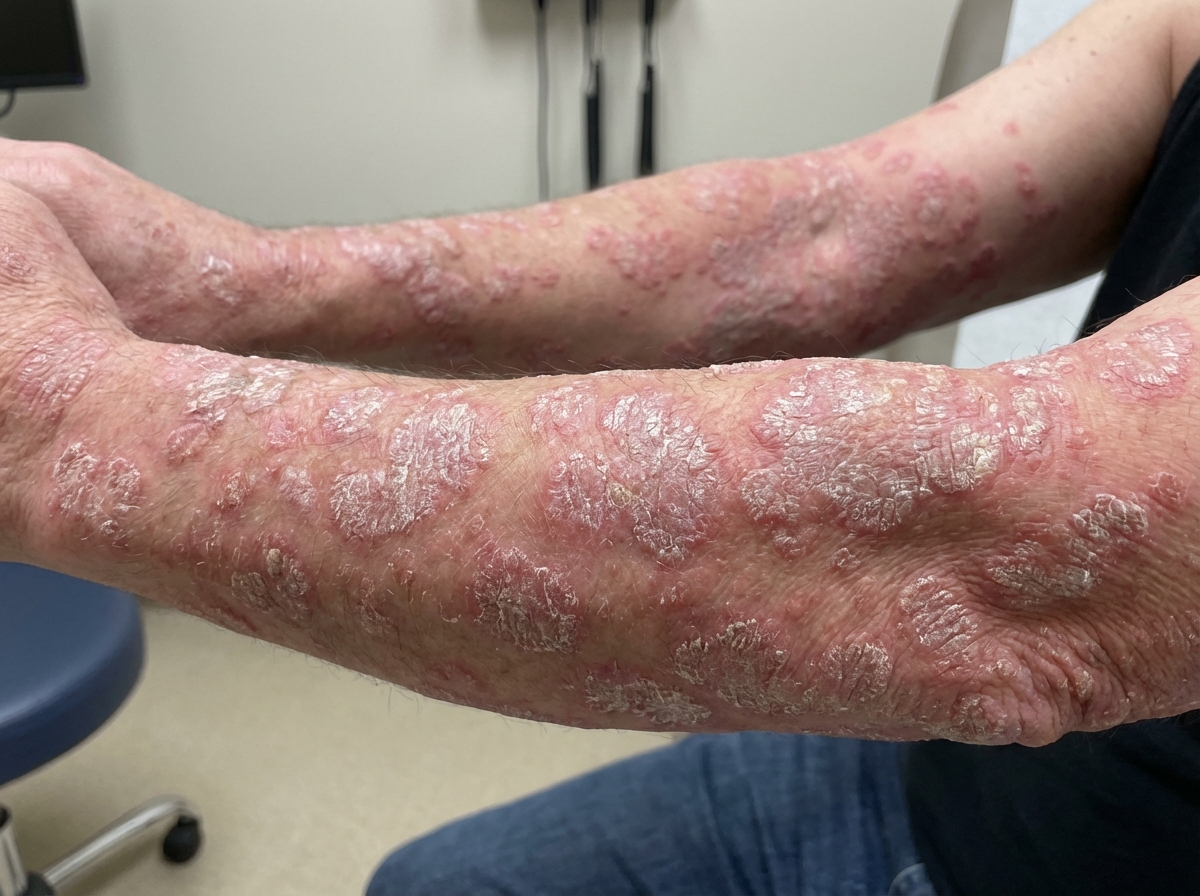
A 50-year-old woman presents with an acute worsening of a chronic rash on her arms and hands for the past week. She says she first noticed the rash 1 year ago which started as little red spots and gradually increased in size. 7 days ago, she noticed the rash suddenly got much worse and spread to her inguinal area, scalp, and knees, which has steadily worsened. She describes the rash as itchy but generally not painful. She says she feels it is very noticeable now and is causing her significant anxiety and depression in addition to the discomfort. The patient denies any fever, chills, sick contacts, or recent travel, and has no significant past medical history. She denies any alcohol use, smoking history, or recreational drug use. Her family history is significant for Crohn disease in her mother and maternal grandmother. She mentions that she has been excessively stressed the past few weeks as she is starting a new job. Review of systems is significant for early morning swelling of the distal joints in her hands and feet for the past 3 months. The patient is afebrile and her vital signs are within normal limits. On physical examination, there are multiple silvery scaly plaques on the extensor surfaces of her upper extremities bilaterally as shown in the exhibit (see image). Similar lesions are present on both knees, inguinal area, and scalp, involving > 10% of her total body surface area. Laboratory tests are unremarkable. Which of the following is the next best step in the management of this patient?
A 67-year-old man is seen on the surgical floor after a transplant procedure. The previous day, the patient had a renal transplant from a matched donor. He is currently recovering and doing well. The patient has a past medical history of IV drug use, diabetes mellitus, oral cold sores, hypertension, renal failure, and dyslipidemia. The patient's current medications include lisinopril, atorvastatin, insulin, and aspirin. Prior to the procedure, he was also on dialysis. The patient is started on cyclosporine. The patient successfully recovers over the next few days. Which of the following medications should be started in this patient?
A 49-year-old African American female with a history of chronic myeloid leukemia for which she is receiving chemotherapy presents to the emergency room with oliguria and colicky left flank pain. Her serum creatinine is 3.3 mg/dL. What is the preferred preventative therapy that could have been administered to this patient to prevent her complication of chemotherapy?
Practice by Chapter
Antiparasitic drugs (antiprotozoals)
Practice Questions
Antimalarial medications
Practice Questions
Anthelmintics
Practice Questions
Antiseptics and disinfectants
Practice Questions
Antimicrobial stewardship principles
Practice Questions
Empiric antimicrobial selection
Practice Questions
Antimicrobial dosing in special populations
Practice Questions
Antimicrobial pharmacokinetics/pharmacodynamics
Practice Questions
Antimicrobial toxicities
Practice Questions
Antimicrobial allergies and cross-reactivity
Practice Questions
Combination antimicrobial therapy
Practice Questions
Cost-effective antimicrobial strategies
Practice Questions
New antimicrobial development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
