Antimicrobials — MCQs

On this page
A 24-year-old woman comes to the emergency department because of a 4-hour history of headaches, nausea, and vomiting. During this time, she has also had recurrent dizziness and palpitations. The symptoms started while she was at a friend's birthday party, where she had one beer. One week ago, the patient was diagnosed with a genitourinary infection and started on antimicrobial therapy. She has no history of major medical illness. Her pulse is 106/min and blood pressure is 102/73 mm Hg. Physical examination shows facial flushing and profuse sweating. The patient is most likely experiencing adverse effects caused by treatment for an infection with which of the following pathogens?
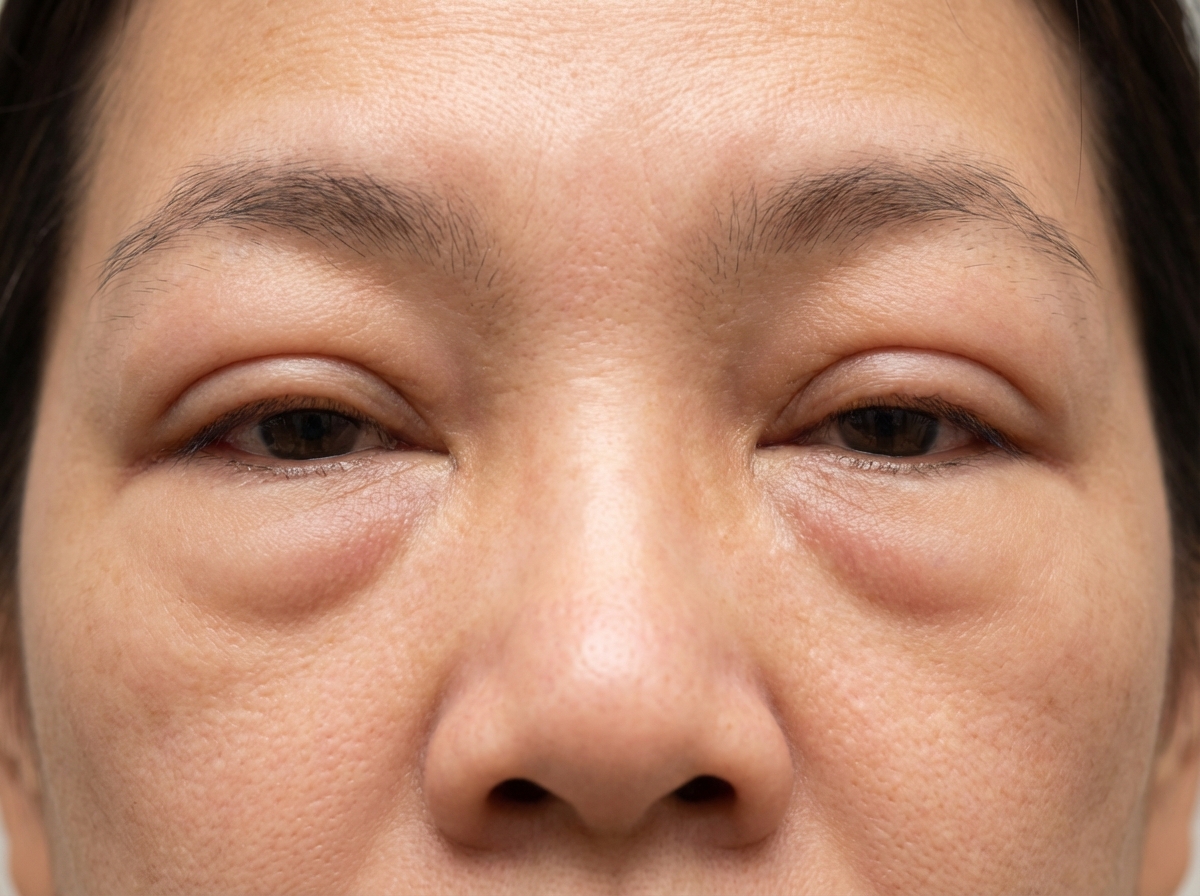
A 40-year-old woman presents to clinic with multiple complaints. She complains of swelling around her eyes (Image A) and generalized weakness. A complete blood count reveals eosinophilia. She recently returned from a trip to Asia where she reports having eaten street food, including pork. If this patient's disease is explained by a parasite that causes inflammation of skeletal muscle, what would be the appropriate treatment?
A 56-year-old man with a history of HIV presents with diarrhea. The patient has had diarrhea for the past week and it has been gradually worsening. The patient describes it as profuse and watery. He has lost 15 pounds during this time frame and feels very weak. The patient is not currently taking his antiretroviral medications and historically has been non-compliant with his medications. His temperature is 98.5°F (36.9°C), blood pressure is 122/58 mmHg, pulse is 127/min, respirations are 14/min, and oxygen saturation is 99% on room air. Physical exam is notable for an emaciated man who is tachycardic. Stool exam with a modified acid-fast stain reveals organisms. The patient is started on IV fluids. Which of the following is the best treatment for this patient?
A 62-year-old woman presents to her oncologist to discuss the chemotherapy options for her newly diagnosed breast cancer. During the meeting, they discuss a drug that inhibits the breakdown of mitotic spindles in cells. Her oncologist explains that this will be more toxic to cancer cells because those cells are dividing more rapidly. Which of the following side effects is closely associated with the use of this chemotherapeutic agent?
A 32-year-old female presents to her gynecologist complaining of heavy and irregular vaginal bleeding. One month ago, she underwent a dilation and curettage procedure to remove a hydatidiform mole. On examination, her uterus appears enlarged. Serum ß-hCG is highly elevated. Biopsy of her uterus reveals avillous proliferation of cytotrophoblasts and syncytiotrophoblasts. She is eventually diagnosed with choriocarcinoma and initiates treatment with a medication known to affect folate metabolism. Which of the following complications should this patient most likely be monitored for following initiation of the medication?
A 67-year-old woman who was diagnosed with cancer 2 months ago presents to her oncologist with a 6-day history of numbness and tingling in her hands and feet. She is concerned that these symptoms may be related to progression of her cancer even though she has been faithfully following her chemotherapy regimen. She is not currently taking any other medications and has never previously experienced these symptoms. On physical exam, she is found to have decreased sensation to pinprick and fine touch over hands, wrists, ankles, and feet. Furthermore, she is found to have decreased reflexes throughout. Her oncologist assures her that these symptoms are a side effect from her chemotherapy regimen rather than progression of the cancer. The drug most likely responsible for her symptoms has which of the following mechanisms?
A 69-year-old male with past medical history of hypertension, hyperlipidemia, and diabetes mellitus complicated by end stage renal disease on dialysis presents to his nephrologist for a follow-up appointment. A few weeks ago, the patient saw his nephrologist because he had been feeling tired despite efforts to get enough sleep, eat a well-balanced diet, and exercise. At the time, laboratory studies revealed a hemoglobin of 9.7 g/dL, and the patient’s nephrologist suggested starting recombinant human erythropoietin (EPO). Since then, the patient has been receiving EPO intravenously three times per week. The patient reports today that he continues to feel tired despite the new treatment. His temperature is 98.0°F (36.7°C), blood pressure is 134/83 mmHg, pulse is 65/min, and respirations are 12/min. On physical exam, he has conjunctival pallor, and laboratory studies show a hemoglobin of 9.8 g/dL. Which of the following laboratory findings would currently be seen in this patient?
A 23-year-old man is admitted to the hospital for observation because of a headache, dizziness, and nausea that started earlier in the day while he was working. He moves supplies for a refrigeration company and was handling a barrel of carbon tetrachloride before the symptoms began. He was not wearing a mask. One day after admission, he develops a fever and is confused. His temperature is 38.4°C (101.1°F). Serum studies show a creatinine concentration of 2.0 mg/dL and alanine aminotransferase concentration of 96 U/L. This patient's laboratory abnormalities are most likely due to which of the following processes?
A 15-year-old boy presents to the emergency department after a rusty nail pierced through his right foot. He was able to pull out the nail, but is unable to walk on his foot. He believes he had all his shots as a child, but his mother is unsure and cannot recall the specific vaccination dates or details. His last documented tetanus vaccination was at age 12. The vital signs are within normal limits. Physical examination reveals a 0.5-inch puncture wound on the right heel. The site is tender, erythematous, with flecks of reddish-brown particles in the base. No blood or discharge is seen. Which of the following is the most appropriate next step in management?
A 65-year-old man comes to the physician because of a 1-month history of progressive back pain. He has also had a 5-kg (11-lb) weight loss over the past 3 months. His only medications are a daily multivitamin and ibuprofen, which he takes daily for the back pain. Physical examination shows tenderness to palpation over the lower spine and the left iliac crest. His hemoglobin concentration is 9.3 g/dL, his serum calcium concentration is 12 mg/dL, and his serum creatinine concentration is 2.1 mg/dL. A bone marrow biopsy shows 21% plasma cells. A diagnosis of multiple myeloma is established. In preparation for an autologous hematopoietic stem cell transplantation, the patient receives a myeloablative treatment regimen that includes busulfan. Which of the following drugs acts via a similar mechanism of action to busulfan?
Practice by Chapter
Antiparasitic drugs (antiprotozoals)
Practice Questions
Antimalarial medications
Practice Questions
Anthelmintics
Practice Questions
Antiseptics and disinfectants
Practice Questions
Antimicrobial stewardship principles
Practice Questions
Empiric antimicrobial selection
Practice Questions
Antimicrobial dosing in special populations
Practice Questions
Antimicrobial pharmacokinetics/pharmacodynamics
Practice Questions
Antimicrobial toxicities
Practice Questions
Antimicrobial allergies and cross-reactivity
Practice Questions
Combination antimicrobial therapy
Practice Questions
Cost-effective antimicrobial strategies
Practice Questions
New antimicrobial development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
