Antihypertensives — MCQs

On this page
A 63-year-old African American man presents to the emergency department with edema over his face and difficulty breathing. Past medical history is significant for hypertension and dyslipidemia. He recently began lisinopril and atorvastatin several weeks ago. His father died at 80 years from complications of a stroke and his mother lives in a nursing home. His blood pressure is 135/92 mm Hg, the heart rate is 101/min, the respiratory rate is 21/min, the temperature is 37.0°C (98.6°F). Clinical pathology results suggest a normal C1 esterase inhibitor level. Of the following options, which is the most likely diagnosis?
A 26-year-old male is brought into the emergency room because he collapsed after working out. The patient is a jockey, and he states that he feels dehydrated and has an upcoming meet for which he needs to lose some weight. On exam, the patient has dry mucosa with cracked lips. His temperature is 98.9 deg F (37.2 deg C), blood pressure is 115/70 mmHg, pulse is 105/min, and respirations are 18/min. The patient's blood pressure upon standing up is 94/65 mmHg. His serum Na+ is 125 mEq/L and K+ is 3.0 mEq/L. His urinalysis reveals Na+ of 35 mEq/L and K+ of 32 mEq/L. The abuse of which of the following is most likely responsible for the patient's presentation?
A 57-year-old man with a history of long-standing hypertension is brought to the emergency department because of headache, dyspnea, and blurry vision for 2 hours. He says that he forgot to fill his prescription for his antihypertensive medications last week. His blood pressure is 230/130 mm Hg. Intravenous infusion of sodium nitroprusside is begun and the patient's symptoms slowly resolve. The next day, the patient develops confusion, abdominal pain, and flushing of the skin. Laboratory studies show metabolic acidosis and an elevated serum lactic acid concentration. Treatment is started with a drug that directly binds the toxin responsible for the patient's new symptoms. The patient was most likely given which of the following drugs?
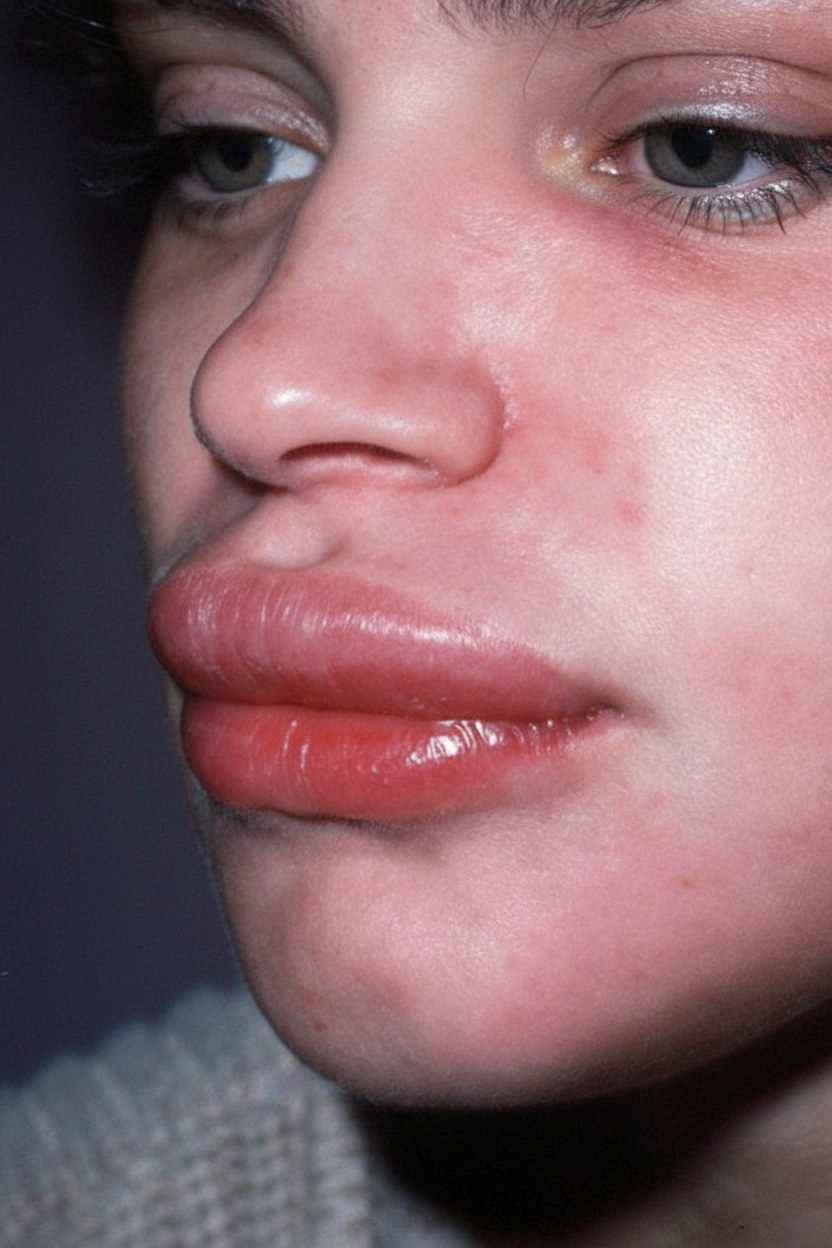
A 47-year-old female with a history of mild asthma, type II diabetes, hypertension, and hyperlipidemia presents to clinic complaining of swelling in her lips (Image A). She has had no changes to her medications within the past two years. Vital signs are stable. Physical exam is notable for significant erythema around and swelling of the lips. The remainder of her exam is unremarkable. What is the mechanism of action of the drug that has caused her current symptoms?
A 48-year-old woman with a history of type 2 diabetes mellitus presents to her primary care physician with complaints of headaches, fatigue, dry cough, and frequent episodes of bronchospasm. She was diagnosed with moderate nonproliferative diabetic retinopathy by an ophthalmologist last month. Her blood pressure measured in the clinic is 158/95 mmHg. A 24-hour urine collection is obtained and reveals 9.5 g of protein. On physical examination, the patient has diffuse wheezing, jugular venous distention, and 2+ pitting pretibial edema. Labs are notable for a potassium level of 5.2 mEq/L. Which of the following medications is most likely contributing to this patient’s current presentation?
A 25-year-old female presents to the emergency room with a heart rate of 32 BPM and a blood pressure of 80/40. She was found by emergency medical services with an empty bottle of propranolol that was taken from her grandmother. Her vital signs do not improve despite IV fluids and oxygen. Which of the following is a first line treatment for overdose?
A 34-year-old man is being evaluated in an emergency clinic for dizziness and headache after a stressful event at work. He also reports that his face often becomes swollen and he occasionally has difficulty breathing during these spells. Family history is significant for his father who died of a stroke and his mother who often suffers from similar facial swelling. The patient’s blood pressure is 170/80 mm Hg. On physical examination, the patient appears well. Which of the following medications is most likely contraindicated in this patient?
A 72-year-old man comes to the emergency department because of blurry vision for the past 3 days. He has also had 4 episodes of right-sided headaches over the past month. He has no significant past medical history. His father died of coronary artery disease at the age of 62 years. His temperature is 37.2°C (99°F), pulse is 94/min, and blood pressure is 232/128 mm Hg. Fundoscopy shows right-sided optic disc blurring and retinal hemorrhages. A medication is given immediately. Five minutes later, his pulse is 75/min and blood pressure is 190/105 mm Hg. Which of the following drugs was most likely administered?
A 67-year-old woman comes to the physician with a 4-month history of chest pain that occurs on exertion. The pain is dull, and she experiences retrosternal pressure when she walks up the stairs to her apartment on the fifth floor. The pain disappears shortly after stopping for one minute. She has hypertension, for which she takes lisinopril and metoprolol daily. She does not smoke or drink alcohol. She is 158 cm (5 ft 2 in) tall and weighs 82 kg (180 lb); BMI is 33 kg/m2. Her pulse is 72/min and blood pressure is 140/85 mm Hg. Cardiac examination shows no murmurs, rubs, or gallops. Fasting lipid studies show: Total cholesterol 196 mg/dL LDL 110 mg/dL HDL 50 mg/dL A resting ECG shows no abnormalities. A week after uneventful initiation of aspirin, the patient is started on atorvastatin. This patient is most likely to develop which of the following?
A 67-year-old woman with chronic kidney disease, hypertension, and diabetes mellitus presented with congestive heart failure and underwent uneventful 3-vessel coronary artery bypass surgery. Within 20 hours, she was extubated and all infusions except nitroprusside were stopped. On the 4th postoperative day, she deteriorated, exhibiting restlessness, tachypnea, tachycardia, and hypotension. Inotropes, vasopressors and bicarbonate infusions were started. Continuous hemodialysis was initiated, yet lactate levels continued to rise. Her chart clarified that she had received 319 mg of nitroprusside over 72 hours. What is the most likely cause of her condition?
Practice by Chapter
Diuretic classes and mechanisms
Practice Questions
ACE inhibitors
Practice Questions
Angiotensin II receptor blockers
Practice Questions
Calcium channel blockers (dihydropyridine/non-dihydropyridine)
Practice Questions
Beta-blockers (cardioselective/non-selective)
Practice Questions
Alpha-blockers
Practice Questions
Alpha-2 agonists
Practice Questions
Direct vasodilators
Practice Questions
Direct renin inhibitors
Practice Questions
SGLT2 inhibitors in hypertension
Practice Questions
Mineralocorticoid receptor antagonists
Practice Questions
Combination antihypertensive therapy
Practice Questions
Resistant hypertension management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
