Antihypertensives — MCQs

On this page
A 74-year-old man presents to the clinic for a routine health checkup. He has been hypertensive for the past 20 years, and he has had congestive heart failure for the past 2 years. He is currently on captopril and claims to be compliant with his medication. His most recent echocardiogram report shows that his ejection fraction has been decreasing, so the physician decides to add spironolactone to his drug regimen. Which of the following complications should be most closely monitored for in this patient?
A 42-year-old African American woman presents to the physician’s office complaining of sudden onset chest pain. She describes the pain as sharp, non-radiating with improvement when she is sitting up and leaning forward. She denies fever, chills, or a cough, but she has had swollen hands and wrists for the past 3 weeks. Medical history is significant for chronic hypertension. She had an appendectomy at age 12. Medications include hydralazine and folic acid. Vital signs are normal except for a low-grade fever. On examination, the patient is in mild distress, especially in the supine position. The metacarpophalangeal and proximal interphalangeal joints are swollen and tender bilaterally. ECG shows diffuse ST elevations. Her antinuclear antibody is negative. Which of the following additional antibodies are expected to be found in this patient’s serum?
A 65-year-old man presents with hypercholesterolemia. Family history is significant for multiple cardiac deaths and other cardiovascular diseases. The patient reports a 40-pack-year smoking history. BMI is 28 kg/m2. Total cholesterol is 255 mg/dL and low-density lipoprotein (LDL) is more than 175 mg/dL. Lifestyle and dietary modifications are recommended, and the patient is prescribed a hypolipidemic drug. He returns for follow-up 4 weeks later complaining of muscle pains. Laboratory findings are significant for a significant increase in serum transaminases. Which of the following drugs is most likely responsible for this patient's symptoms on follow-up?
A 42-year-old man presents to the emergency room complaining of a painful, swollen tongue that is making it hard to talk and swallow. The patient denies trauma, trouble breathing, and skin rashes. The patient has no known allergies and a minimal past medical history, except for newly diagnosed hypertension for which he was just started on a new medication. The patient is afebrile, the blood pressure is 145/110 mm Hg, the heart rate is 88/min, and the O2 saturation is 97% on room air. What is the mechanism of this reaction?
A 44-year-old woman comes to the emergency department after waking up with facial swelling and with difficulties speaking and swallowing. She states that she does not have allergies or recently had insect bites. She has a 4-year history of hypertension and type 2 diabetes mellitus controlled with medication. Her pulse is 110/min, respirations are 20/min, and blood pressure is 140/90 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 97%. On physical exam, she appears uncomfortable, with notable swelling of the lips and tongue. The remainder of the examination shows no abnormalities. Serum C4 levels are within normal limits. Which of the following is the most likely underlying mechanism of this patient's symptoms?
A 34-year-old gravida 2, para 1 woman at 37+6 weeks of gestation presents for elective cesarean delivery. She says she has been having increased fatigue over the past few weeks. Past medical history includes gestational hypertension for which she has been taking an antihypertensive drug twice daily since week 24. Her vital signs include: temperature 36.7°C (98.0°F), blood pressure 120/75 mm Hg, pulse 127/min. Physical examination reveals generalized pallor. Her laboratory results reveal normocytic anemia with anisocytosis, hemoglobin of 9 g/dL, a differential with 14% lymphocytes, an ESR of 22 mm/hr, and a reticulocyte production index of 3.1. A direct antiglobulin test is positive. LFTs, creatinine, ferritin level, vitamin B12 level, coagulation studies, and urinalysis are normal. Which of the following is the most likely diagnosis in this patient?
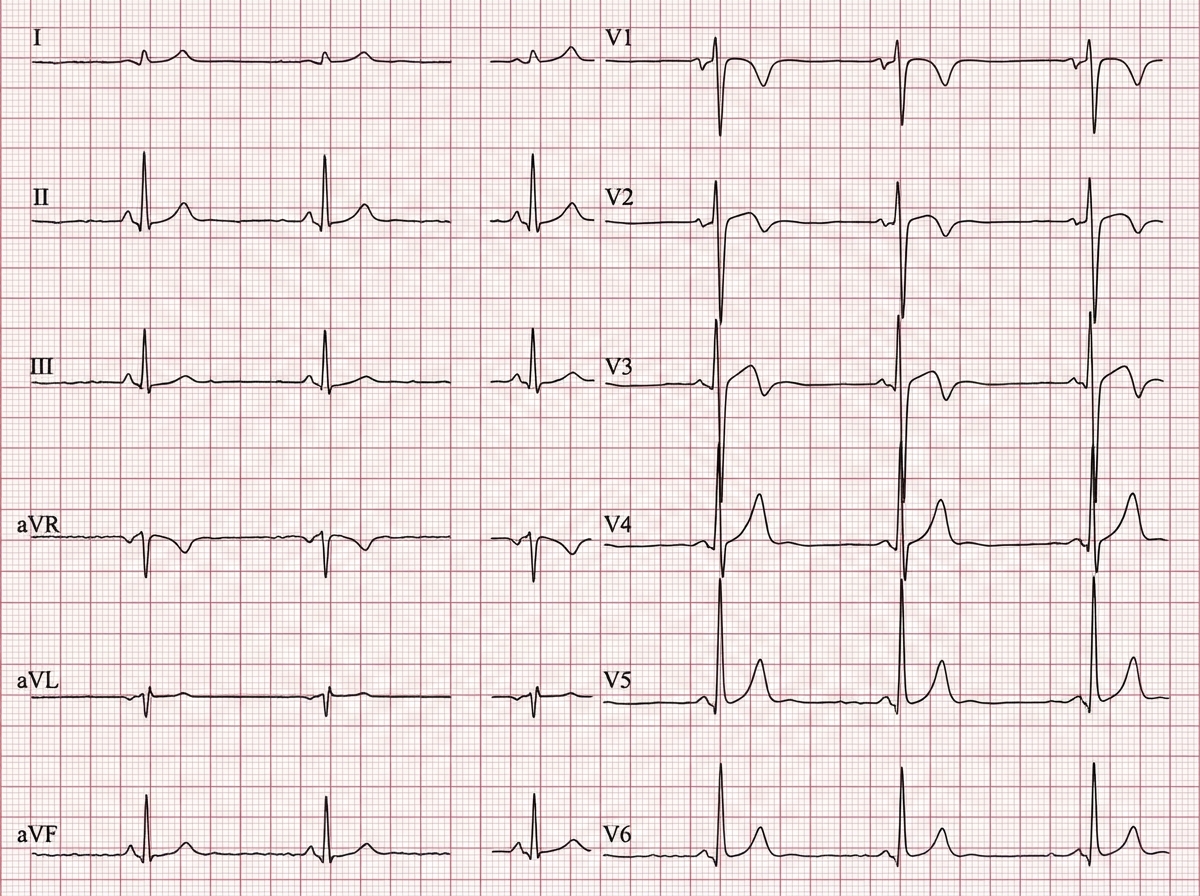
Four weeks after starting hydrochlorothiazide, a 49-year-old man with hypertension comes to the physician because of muscle cramps and weakness. His home medications also include amlodipine. His blood pressure today is 176/87 mm Hg. Physical examination shows no abnormalities. The precordial leads of a 12-lead ECG are shown. The addition of which of the following is most likely to have prevented this patient's condition?
A 55-year-old man with hypertension, hyperlipidemia, type 2 diabetes mellitus, and asthma comes to the physician because of a 2-month history of intermittent dry, hacking cough. He does not have fever, chest pain, or shortness of breath. He does not smoke cigarettes. Current medications include simvastatin, metformin, albuterol, and ramipril. His temperature is 37°C (98.6°F), pulse is 87/min, and blood pressure is 142/88 mm Hg. Cardiopulmonary examination shows no abnormalities. Which of the following is the most appropriate next step in management?
A 60-year-old African-American male with no active medical problems presents to his primary care physician for a general checkup. His blood pressure on the previous visit was 145/90, and his blood pressure at this visit is found to be 150/95. He is prescribed hydrochlorothiazide, a thiazide diuretic, to treat his hypertension. The serum level of which of the following is likely to decrease in response to his treatment?
A 52-year-old man presents to his primary care physician for an annual check-up. He says that he has no significant developments over the last year and that he has been feeling well in general. On presentation, his temperature is 98.6°F (37°C), blood pressure is 140/95 mmHg, pulse is 85/min, and respirations are 12/min. This is the third time that he has had elevated blood pressure so his physician suggests that he start taking a medication for hypertension. The patient is a biologist so he researches this medication after returning home. He finds that the medication can either decrease or increase the level of cyclic adenosine monophosphate depending on whether there is endogenous substrate around. Which of the following medications is most likely being described here?
Practice by Chapter
Diuretic classes and mechanisms
Practice Questions
ACE inhibitors
Practice Questions
Angiotensin II receptor blockers
Practice Questions
Calcium channel blockers (dihydropyridine/non-dihydropyridine)
Practice Questions
Beta-blockers (cardioselective/non-selective)
Practice Questions
Alpha-blockers
Practice Questions
Alpha-2 agonists
Practice Questions
Direct vasodilators
Practice Questions
Direct renin inhibitors
Practice Questions
SGLT2 inhibitors in hypertension
Practice Questions
Mineralocorticoid receptor antagonists
Practice Questions
Combination antihypertensive therapy
Practice Questions
Resistant hypertension management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
