Antihypertensives — MCQs

On this page
A 60-year-old woman sought evaluation at an urgent care clinic after developing breathlessness 30 minutes earlier. She also developed swelling of the tongue and lips. She has heart failure and was recently diagnosed with hypertension. She was started on a medication, the first dose of which she took this afternoon before her symptoms started. Her blood pressure is 167/88 mm Hg, the respiratory rate is 17/min, and the pulse is 78/min. The physical examination reveals a skin rash on the back and abdomen. There is a mild swelling of the lips and tongue. Chest auscultation does not reveal any abnormal breath sounds. Which of the following medications most likely led to her current symptoms?
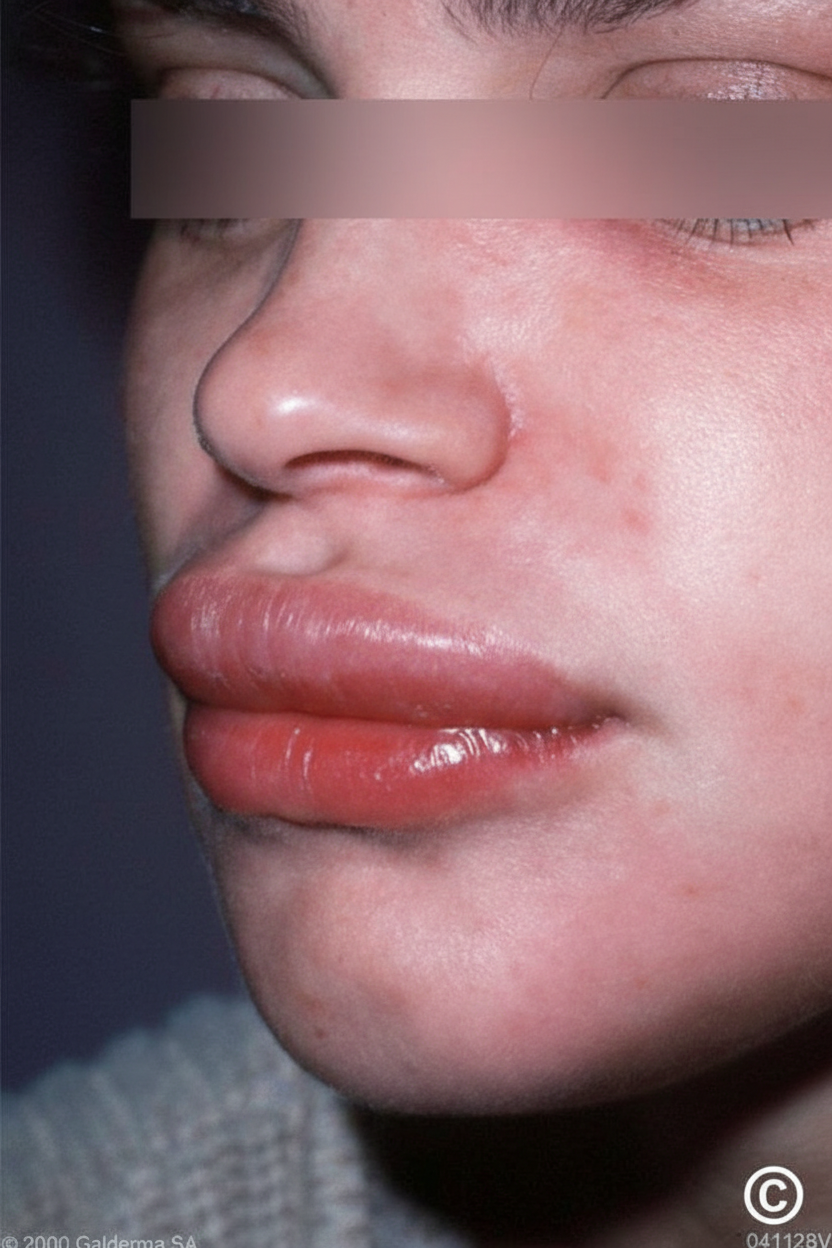
A 45-year-old man was shown to have a blood pressure of 142/90 mm Hg at a health fair. Despite modifying his lifestyle, his blood pressure remained elevated on 2 separate subsequent occasions. He was prescribed an anti-hypertensive medication. After 3 weeks, the swelling of the lips shown in the accompanying photograph was observed. What is the most likely cause of this finding?
A 62-year-old man comes to the physician for a follow-up examination. One month ago, therapy with lisinopril was initiated for treatment of hypertension. His blood pressure is 136/86 mm Hg. Urinalysis shows a creatinine clearance of 92 mL/min. The patient's serum creatinine concentration is most likely closest to which of the following values?
A 45-year-old woman comes to the physician because of a 2-week history of fatigue and excessive thirst. During this period, she has not been able to sleep through the night because of the frequent urge to urinate. She also urinates more than usual during the day. She drinks 4–5 liters of water and 1–2 beers daily. She has autosomal dominant polycystic kidney disease, hypertension treated with lisinopril, and bipolar disorder. Therapy with valproic acid was begun after a manic episode 3 months ago. Vital signs are within normal limits. Irregular flank masses are palpated bilaterally. The remainder of the examination shows no abnormalities. Laboratory studies show: Serum Na+ 152 mEq/L K+ 4.1 mEq/L Cl− 100 mEq/L HCO3− 25 mEq/L Creatinine 1.8 mg/dL Osmolality 312 mOsmol/kg Glucose 98 mg/dL Urine osmolality 190 mOsmol/kg The urine osmolality does not change after 3 hours despite no fluid intake or after administration of desmopressin. Which of the following is the most appropriate next step in management?
A 60-year-old man comes to the physician because of flank pain, rash, and blood-tinged urine for 1 day. Two months ago, he was started on hydrochlorothiazide for hypertension. He takes acetaminophen for back pain. Examination shows a generalized, diffuse maculopapular rash. Serum studies show a creatinine concentration of 3.0 mg/dL. Renal ultrasonography shows no abnormalities. Which of the following findings is most likely to be observed in this patient?
A 52-year-old man presents to the emergency department with chest pain radiating to his left jaw and arm. He states that he had experienced similar symptoms when playing basketball. The medical history is significant for diabetes mellitus, hypertension, and GERD, for which he takes metformin, hydrochlorothiazide, and pantoprazole, respectively. The blood pressure is 150/90 mm Hg, the pulse is 100/min, and the respirations are 15/min. The ECG reveals ST elevation in leads V3-V6. He is hospitalized for an acute MI and started on treatment including lisinopril. The next day he complains of dizziness and blurred vision. Repeat vital signs were as follows: blood pressure 90/60 mm Hg, pulse 72/min, and respirations 12/min. The laboratory results were as follows: Serum chemistry Sodium 143 mEq/L Potassium 4.1 mEq/L Chloride 98 mEq/L Bicarbonate 22 mEq/L Blood urea nitrogen 26 mg/dL Creatinine 2.3 mg/dL Glucose 120 mg/dL Which of the following drugs is responsible for this patient's lab abnormalities?
Practice by Chapter
Diuretic classes and mechanisms
Practice Questions
ACE inhibitors
Practice Questions
Angiotensin II receptor blockers
Practice Questions
Calcium channel blockers (dihydropyridine/non-dihydropyridine)
Practice Questions
Beta-blockers (cardioselective/non-selective)
Practice Questions
Alpha-blockers
Practice Questions
Alpha-2 agonists
Practice Questions
Direct vasodilators
Practice Questions
Direct renin inhibitors
Practice Questions
SGLT2 inhibitors in hypertension
Practice Questions
Mineralocorticoid receptor antagonists
Practice Questions
Combination antihypertensive therapy
Practice Questions
Resistant hypertension management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
