Antifungals — MCQs

On this page
A 19-year-old woman comes to the physician because of worsening pain with swallowing for 3 days and a dry sensation in the mouth over the past week. She has a history of asthma controlled with inhaled fluticasone and albuterol. Physical examination shows white plaques on the dorsal surface of the tongue and buccal mucosa that bleed when scraped off. Which of the following is the most appropriate pharmacotherapy?
A 55-year-old man, who underwent a kidney transplant 2 years ago, presents in septic shock. He is compliant with his immunosuppressive therapy. He does not use any drugs and is sexually active with one male partner. His complete blood count returns as follows: Hemoglobin: 13.7 g/dL, white blood cell count: 4000 cells/microliter, platelets 250,000 cells/microliter. Of note, from his differential: neutrophils: 10%, lymphocytes: 45%, and monocytes: 7%. His basic metabolic profile is notable for a creatinine remaining at his baseline of 0.9 mg/dL. The patient is started on broad spectrum antibiotics, but his condition does not improve. Fungal blood cultures are obtained and grow Candida species. Which of the following was the most-likely predisposing factor?
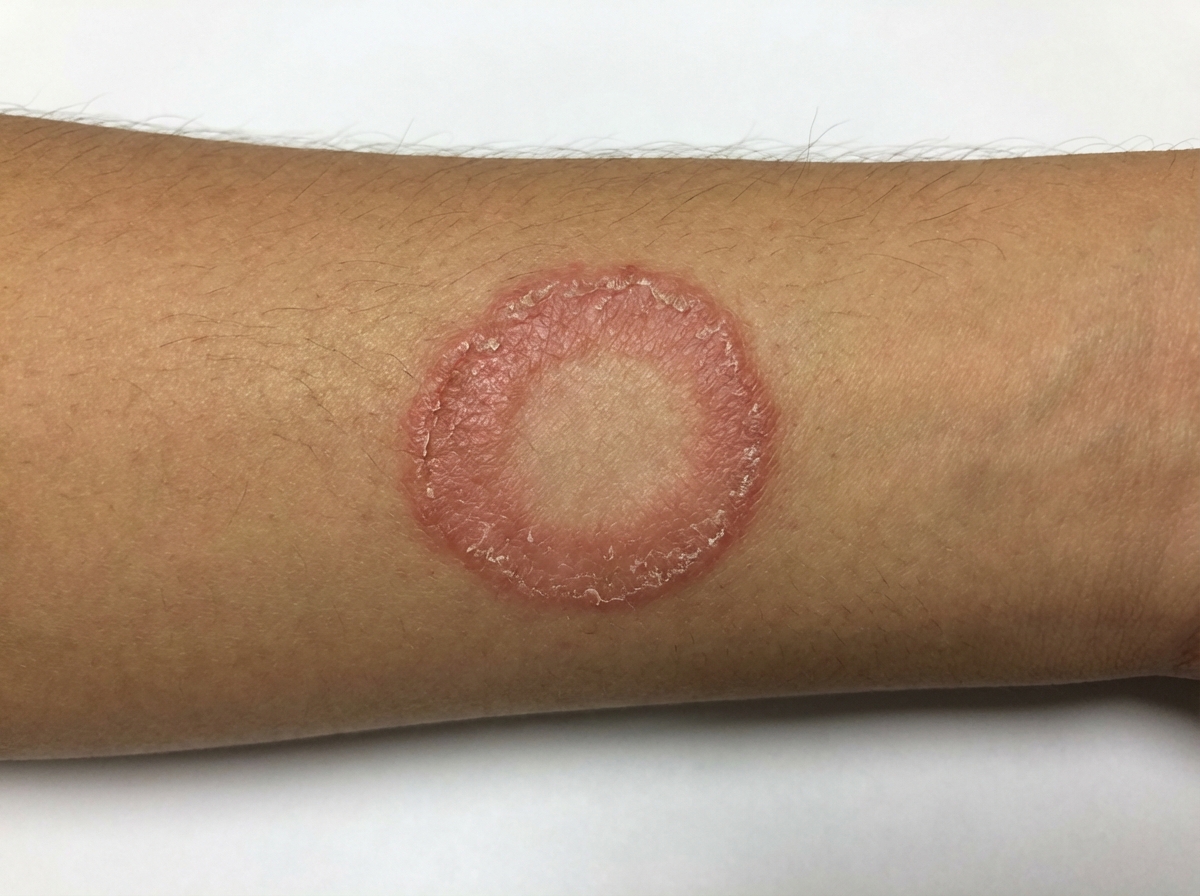
A 15-year-old boy is brought to the physician with an ongoing pruritic rash for 1 week. The rash is on his right forearm (refer to the image). He has not had a similar rash in the past. He has no history of allergies, and he is not taking any medications. He frequently enjoys gardening in their backyard. They have no household pets. The physical examination reveals no other abnormalities. Given the most likely diagnosis, which of the following is the most appropriate treatment of the condition described in this case?
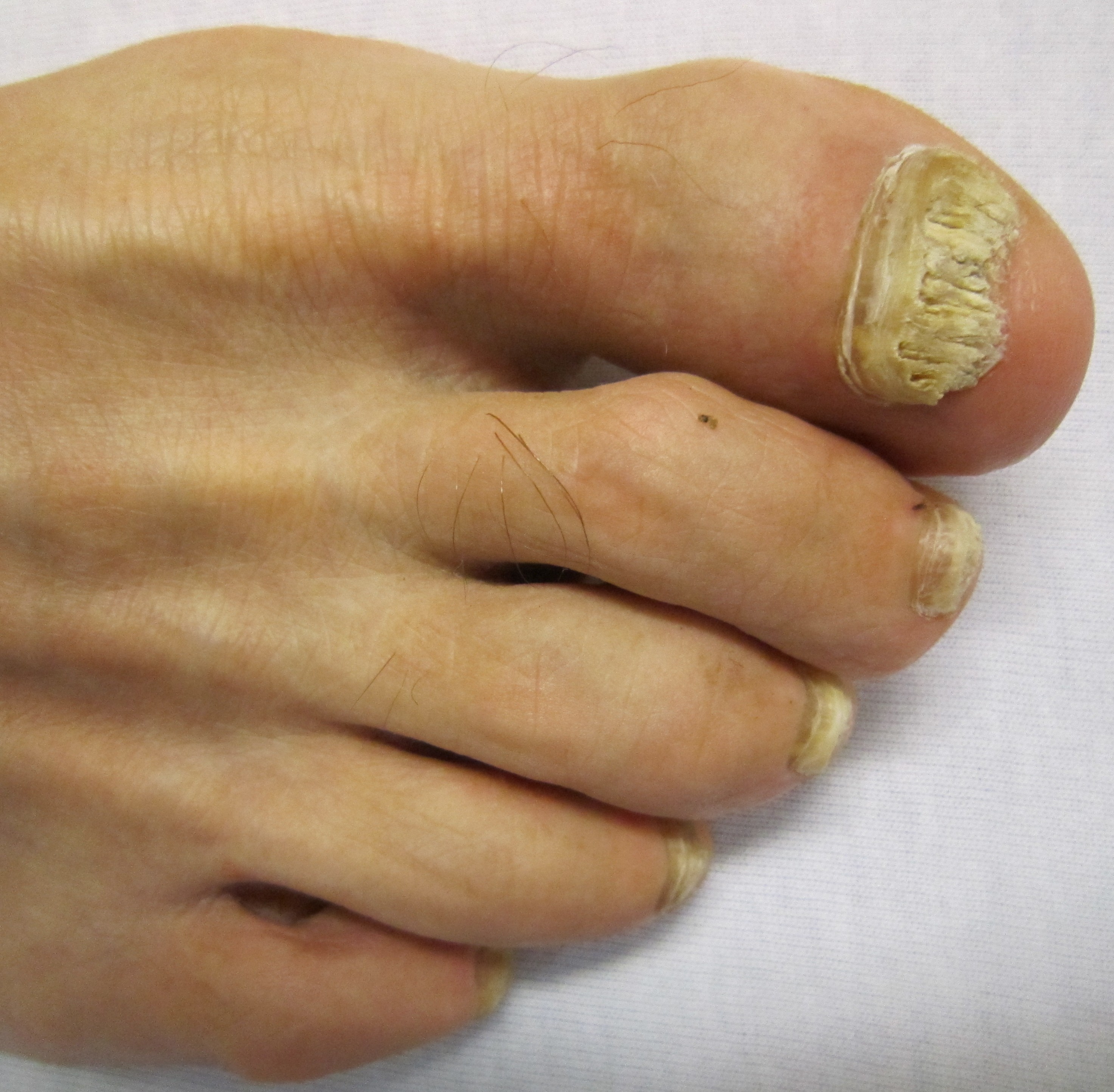
A 62-year-old man presents with dry and brittle toenails. On physical examination, his toenails are shown in the image. Which of the following is an adverse effect of the recommended treatment for this patient’s most likely condition?
A 57-year-old florist presents to his family physician with nodular lesions on his right hand and forearm. He explains that he got pricked by a rose thorn on his right "pointer finger" where the first lesions appeared, and the other lesions then began to appear in an ascending manner. The physician prescribed a medication and warned him of gynecomastia as a side effect if taken for long periods of time. Which of the following is the mechanism of action of the medication?
Practice by Chapter
Polyenes (amphotericin formulations)
Practice Questions
Azoles (imidazoles and triazoles)
Practice Questions
Echinocandins
Practice Questions
Flucytosine
Practice Questions
Griseofulvin
Practice Questions
Terbinafine
Practice Questions
Topical antifungal agents
Practice Questions
Antifungal prophylaxis protocols
Practice Questions
Antifungal spectrum of activity
Practice Questions
Antifungal resistance mechanisms
Practice Questions
Antifungal therapeutic drug monitoring
Practice Questions
Drug interactions with antifungals
Practice Questions
Treatment guidelines for invasive fungal infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
