Antifungals — MCQs

On this page
A 69-year-old man with metastatic colon cancer is brought to the emergency department because of shortness of breath, fever, chills, and a productive cough with streaks of blood for the past 5 days. He has a history of emphysema. The patient does not have abdominal pain or headache. He receives chemotherapy with 5-fluorouracil, leucovorin, and oxaliplatin every 6 weeks; his last cycle was 3 weeks ago. His temperature is 38.3°C (101°F), pulse is 112/min, and blood pressure is 100/70 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 83%. A few scattered inspiratory crackles are heard over the right lung. His mucous membranes are dry. Cardiac examination is normal. Laboratory studies show: Hemoglobin 9.3 mg/dL Leukocyte count 700/mm3 Segmented neutrophils 68% Lymphocytes 25% Eosinophils 4% Monocytes 3% Platelet count 104,000/mm3 Serum Glucose 75 mg/dL Urea nitrogen 41 mg/dL Creatinine 2.1 mg/dL Galactomannan antigen Positive Which of the following is the most appropriate initial pharmacotherapy?
A 45-year-old HIV-positive male presents to his primary care physician complaining of decreased libido. He reports that he has been unable to maintain an erection for the past two weeks. He has never encountered this problem before. He was hospitalized four weeks ago for cryptococcal meningitis and has been on long-term antifungal therapy since then. His CD4 count is 400 cells/mm^3 and viral load is 5,000 copies/ml. He was previously non-compliant with HAART but since his recent infection, he has been more consistent with its use. His past medical history is also notable for hypertension, major depressive disorder, and alcohol abuse. He takes lisinopril and sertraline. His temperature is 98.6°F (37°C), blood pressure is 120/85 mmHg, pulse is 80/min, and respirations are 18/min. The physician advises the patient that side effects like decreased libido may manifest due to a drug with which of the following mechanisms of action?
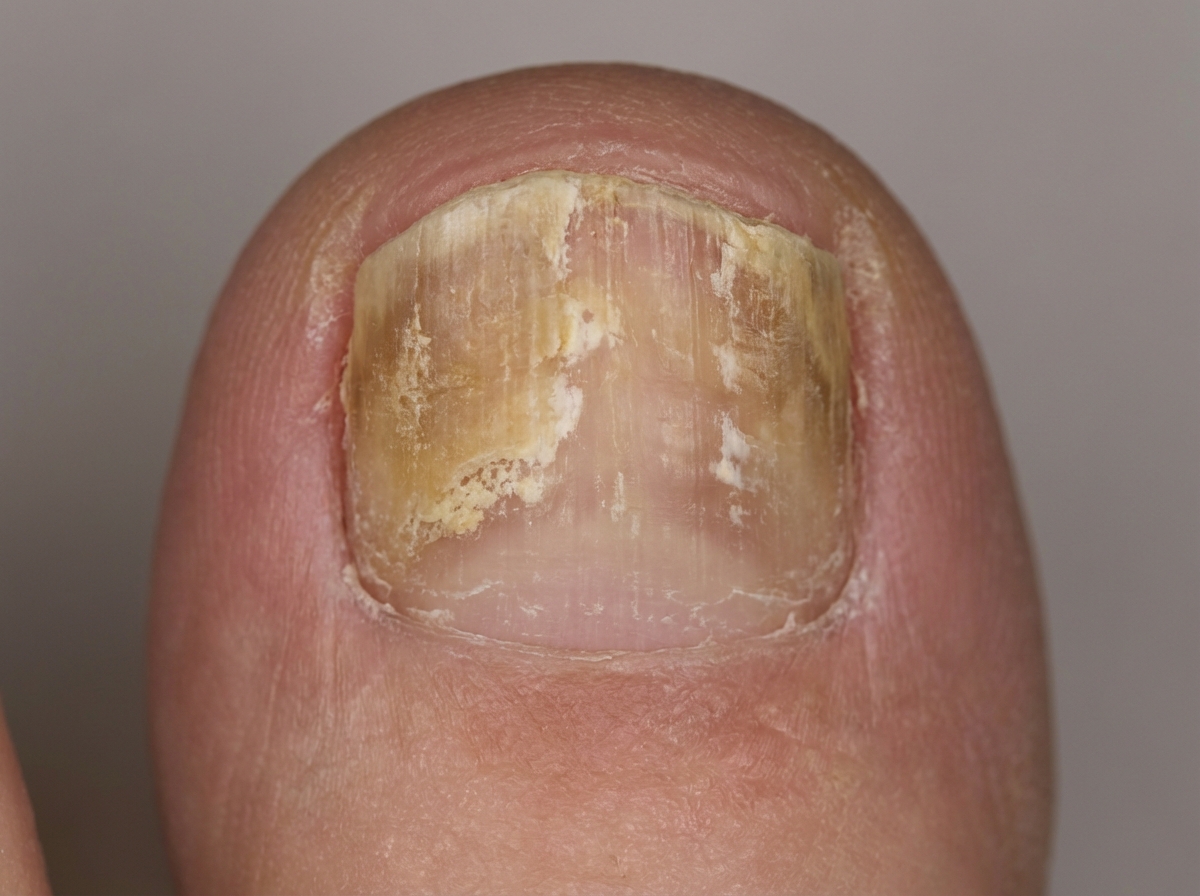
A 67-year-old man presents to his family physician’s office for a routine visit and to discuss a growth on his toenail that has been gradually enlarging for a month. He has a history of diabetes mellitus, hyperlipidemia, and hypertension and is on metformin, atorvastatin, and lisinopril. He admits to smoking 2 packs of cigarettes daily for the past 45 years. His blood pressure reading today is 132/88 mm Hg, heart rate is 78/min, respiration rate is 12/min and his temperature is 37.1°C (98.8°F). On exam, the patient appears alert and in no apparent distress. Capillary refill is 3 seconds. Diminished dull and sharp sensations are present bilaterally in the lower extremities distal to the mid-tibial region. An image of the patient’s toenail is provided. A potassium hydroxide (KOH) preparation of a nail clipping sample confirms the presence of hyphae. Which of the following treatment options will be most effective for this condition?
An 11-year-old boy with HIV and esophageal candidiasis is being treated with caspofungin. What is the mechanism of action of this drug?
A 38-year-old man comes to the physician because of white lesions in his mouth for 4 days. He also has intense pain while chewing food. He was diagnosed with non-Hodgkin lymphoma around 8 months ago. He is undergoing chemotherapy and is currently on his fourth cycle. He was treated for herpes labialis 4 months ago with acyclovir. He has smoked half a pack of cigarettes daily for 15 years. He appears healthy. Vital signs are within normal limits. Cervical and axillary lymphadenopathy is present. Oral examination shows white plaques on his tongue and buccal mucosa that bleed when scraped off. The remainder of the examination shows no abnormalities. Which of the following is the next best step in management?
A 42-year-old man comes to the physician because he is concerned that he is balding. Over the past few months, he has noticed patchy areas of hair loss on his head. He also mentions that he has felt depressed since the death of his wife last year and has unintentionally lost about 18 kg (40 lbs). He is constantly fatigued. He has little appetite because he feels food does not taste the same way anymore. He also has occasional episodes of watery diarrhea. He drinks 5–6 cans of beer daily. Vital signs are within normal limits. Examination shows dry, scaly skin on both feet. There is patchy alopecia of the scalp, axillae, chest, and mons pubis. Which of the following is most likely to directly improve this patient's alopecia?
A 41-year-old man comes to the physician because of a 3-week history of fatigue, cough, and a 4.5-kg (10-lb) weight loss. He does not smoke or drink alcohol. He appears emaciated. A chest x-ray shows a calcified nodule in the left lower lobe and left hilar lymphadenopathy. The physician initiates therapy for the condition and informs him that he will have to return for monthly ophthalmologic examination for the next 2 months. These examinations are most likely to evaluate the patient for an adverse effect of a drug with which of the following mechanisms of action?
A 72-year-old woman with type 2 diabetes mellitus comes to the physician because she is concerned about the appearance of her toenails. Examination shows yellowish discoloration of all toenails on both feet. The edges of the toenails are lifted, and there is subungual debris. Potassium hydroxide preparation of scrapings from the nails shows multiple branching septate hyphae. Treatment with oral terbinafine is begun. Which of the following is the primary mechanism of action of this drug?
You are taking care of a patient with renal failure secondary to anti-fungal therapy. The patient is a 66-year-old male being treated for cryptococcal meningitis. This drug has a variety of known side effects including acute febrile reactions to infusions, anemia, hypokalemia and hypomagnesemia. What is the mechanism of action of this drug?
A 26-year-old man comes to the physician because of discoloration of the toenails. He has a history of peptic ulcer disease treated with pantoprazole. The physician prescribes oral itraconazole for a fungal infection and temporarily discontinues pantoprazole. Which of the following best describes the reason for discontinuing pantoprazole therapy?
Practice by Chapter
Polyenes (amphotericin formulations)
Practice Questions
Azoles (imidazoles and triazoles)
Practice Questions
Echinocandins
Practice Questions
Flucytosine
Practice Questions
Griseofulvin
Practice Questions
Terbinafine
Practice Questions
Topical antifungal agents
Practice Questions
Antifungal prophylaxis protocols
Practice Questions
Antifungal spectrum of activity
Practice Questions
Antifungal resistance mechanisms
Practice Questions
Antifungal therapeutic drug monitoring
Practice Questions
Drug interactions with antifungals
Practice Questions
Treatment guidelines for invasive fungal infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
