Antifungals — MCQs

On this page
A previously healthy 16-year-old boy comes to the physician because of a pruritic rash on the chest that has become progressively larger over the past 10 days. It is not painful. He is sexually active with two female partners and uses condoms inconsistently. He works part-time as a lifeguard. He has no family history of serious illness. He does not smoke. He drinks 5–6 beers on weekends. His temperature is 36.7°C (98°F), pulse is 66/min, and blood pressure is 110/70 mm Hg. A photograph of the rash is shown below. Which of the following is the most appropriate next step in management?
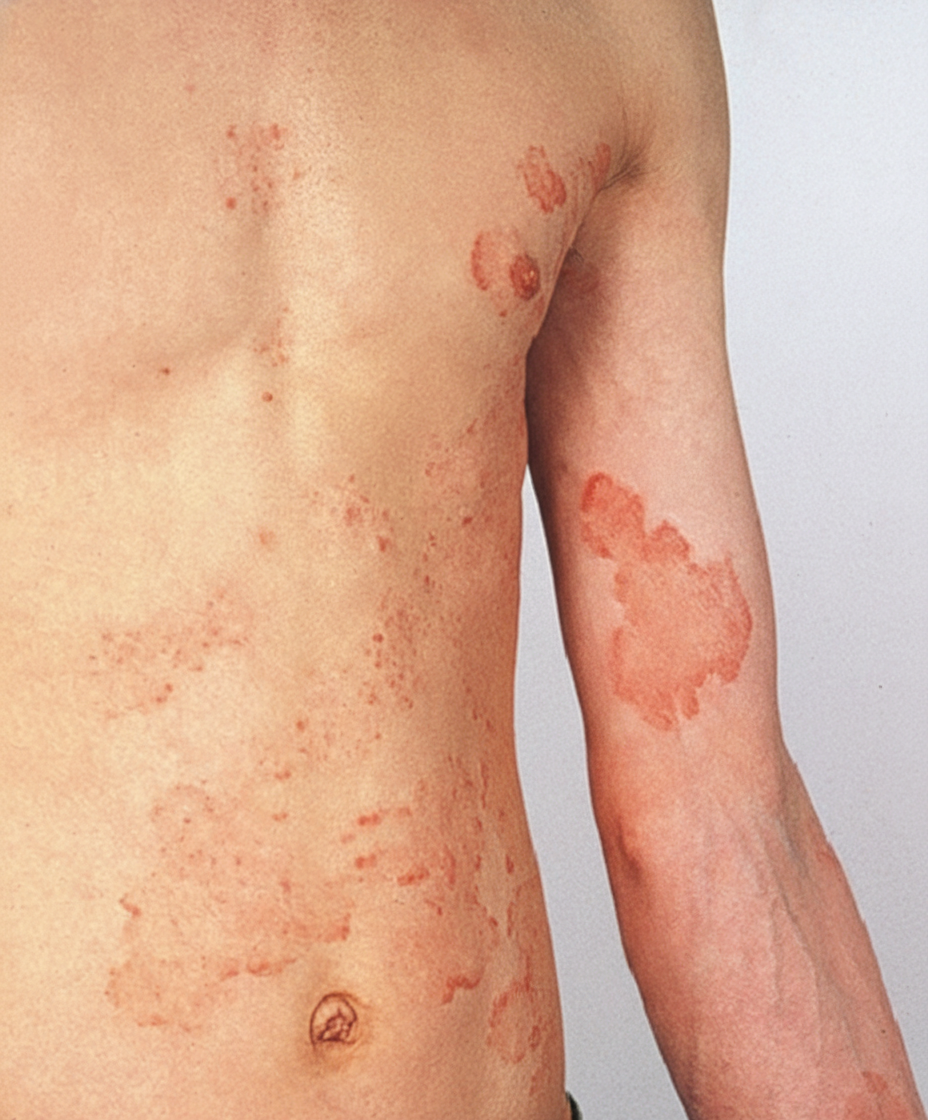
A 35-year-old African American male is admitted to the hospital following a recent diagnosis of systemic histoplasmosis and subsequently treated with an intravenous anti-fungal agent. During the course of his hospital stay, he complains of headaches. Work-up reveals hypotension, anemia, and elevated BUN and creatinine. His medication is known to cause these side-effects through its binding of cell membrane ergosterol. With which anti-fungal is he most likely being treated?
A 28-year-old woman with HIV comes to the physician because of an 8-day history of severe pain while swallowing. She has been hospitalized several times with opportunistic infections and has poor adherence to her antiretroviral drug regimen. Endoscopy shows extensive, white, plaque-like lesions in the proximal esophagus. Culture of a biopsy specimen grows Candida albicans. Treatment with intravenous anidulafungin is initiated. Which of the following is the primary mechanism of action of this drug?
A 12-year-old girl is brought to the physician for a follow-up examination. Two months ago, she was diagnosed with asthma and treatment was begun with an albuterol inhaler as needed. Since then, she has had episodic chest tightness and cough 2–3 times per week. The cough is intermittent and nonproductive; it is worse at night. She has been otherwise healthy and takes no other medications. Her vital signs are within normal limits. Pulmonary examination shows mild expiratory wheezing of all lung fields. Spirometry shows an FEV1:FVC ratio of 81% and an FEV1 of 80% of predicted; FEV1 rises to 93% of predicted after administration of a short-acting bronchodilator. Treatment with low-dose inhaled beclomethasone is begun. The patient is at greatest risk for which of the following adverse effects?
A 45-year-old man presents to the emergency department with difficulties swallowing food. He states that he experiences pain when he attempts to swallow his medications or when he drinks water. He reveals that he was diagnosed with HIV infection five years ago. He asserts that he has been taking his antiretroviral regimen, including emtricitabine, rilpivirine, and tenofovir. His temperature is 98°F (37°C), blood pressure is 100/60 mmHg, pulse is 90/min, respirations are 22/min, and oxygen saturation is 99% on room air. His physical exam is notable for a clear oropharynx, no lymphadenopathy, and a normal cardiac and pulmonary exam. No rashes are noted throughout his body. His laboratory results are displayed below: Hemoglobin: 12 g/dL Hematocrit: 37 % Leukocyte count: 8,000/mm^3 with normal differential Platelet count: 160,000/mm^3 Serum: Na+: 138 mEq/L Cl-: 108 mEq/L K+: 3.5 mEq/L HCO3-: 26 mEq/L BUN: 35 mg/dL Glucose: 108 mg/dL Creatinine: 1.1 mg/dL CD4+ count: 90/mm^3 HIV viral load: 59,000 copies/mL What is the best next step in management?
A 9-year-old African-American boy is brought to the physician by his mother because of an itchy rash on the right side of his scalp and progressive loss of hair for 1 month. He has no history of serious illness. His younger sibling was treated for pediculosis capitis 3 months ago. The boy attends elementary school, but has not been going for the last week because he was too embarrassed by the rash. He appears anxious. A photograph of his scalp is shown. Occipital lymphadenopathy is present. The remainder of the examination shows no abnormalities. Which of the following is the most appropriate next step in management?
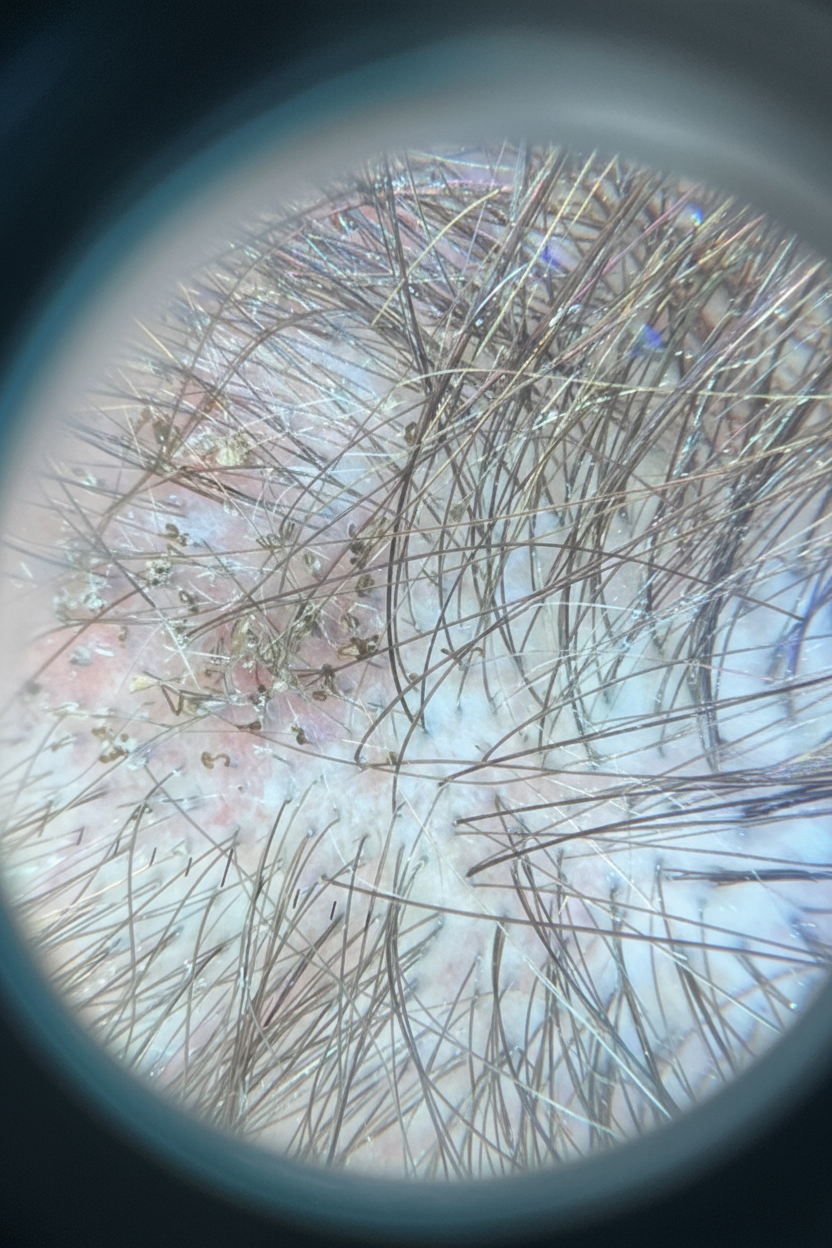
A 45-year-old man comes to the physician because of a 3-day history of pain in his mouth and throat and difficulty swallowing. He has a history of COPD, for which he takes theophylline and inhaled budesonide-formoterol. Physical examination shows white patches on the tongue and buccal mucosa that can be scraped off easily. Appropriate pharmacotherapy is initiated. One week later, he returns because of nausea, palpitations, and anxiety. His pulse is 110/min and regular. Physical examination shows a tremor in both hands. Which of the following drugs was most likely prescribed?
A 74-year-old man is admitted to the medical ward after he developed a fungal infection. He has aplastic anemia. The most recent absolute neutrophil count was 450/µL. An anti-fungal agent is administered that inhibits the fungal enzyme, (1→3)-β-D-glucan synthase, and thereby disrupts the integrity of the fungal cell wall. He responds well to the treatment. Although amphotericin B is more efficacious for his condition, it was not used because of the side effect profile. What was the most likely infection?
A 57-year-old woman with non-small cell lung cancer comes to the physician 4 weeks after her tumor was resected. She takes no medications. The physician starts her on a treatment regimen that includes vinblastine. This treatment puts the patient at highest risk for which of the following?
A 46-year-old man with HIV infection comes to the physician because of a 1-week history of severe retrosternal pain while swallowing. He has not been compliant with his antiretroviral drug regimen. His CD4+ T-lymphocyte count is 98/mm3 (N ≥ 500). Endoscopy shows white plaques in the esophagus. The most appropriate immediate treatment is a drug that inhibits which of the following enzymes?
Practice by Chapter
Polyenes (amphotericin formulations)
Practice Questions
Azoles (imidazoles and triazoles)
Practice Questions
Echinocandins
Practice Questions
Flucytosine
Practice Questions
Griseofulvin
Practice Questions
Terbinafine
Practice Questions
Topical antifungal agents
Practice Questions
Antifungal prophylaxis protocols
Practice Questions
Antifungal spectrum of activity
Practice Questions
Antifungal resistance mechanisms
Practice Questions
Antifungal therapeutic drug monitoring
Practice Questions
Drug interactions with antifungals
Practice Questions
Treatment guidelines for invasive fungal infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
