Nursery outbreaks — MCQs

A 6-year-old boy and his parents present to the emergency department with high-grade fever, headache, and projectile vomiting. The boy was born at 39 weeks gestation via spontaneous vaginal delivery. He is up to date on all vaccines and is meeting all developmental milestones. Past medical history is noncontributory. He has had no sick contacts at school or at home. The family has not traveled out of the area recently. He likes school and playing videogames with his younger brother. Today, his blood pressure is 115/76 mm Hg, heart rate is 110/min, respiratory rate is 22/min, and temperature is 38.4°C (101.2°F). On physical exam, the child is disoriented. Kernig’s sign is positive. A head CT was performed followed by a lumbar puncture. Several aliquots of CSF were distributed throughout the lab. Cytology showed high counts of polymorphs, biochemistry showed low glucose and elevated protein levels, and a gram smear shows gram-positive lanceolate-shaped cocci alone and in pairs. A smear is prepared on blood agar in an aerobic environment and grows mucoid colonies with clearly defined edges and alpha hemolysis. On later evaluation they develop a ‘draughtsman’ appearance. Which one of the following is the most likely pathogen?
A 12-month-old girl is brought to her pediatrician for a checkup and vaccines. The patient’s mother wants to send her to daycare but is worried about exposure to unvaccinated children and other potential sources of infection. The toddler was born at 39 weeks gestation via spontaneous vaginal delivery. She is up to date on all vaccines. She does not walk yet but stands in place and can say a few words. The toddler drinks formula and eats a mixture of soft vegetables and pureed meals. She has no current medications. On physical exam, the vital signs include: temperature 37.0°C (98.6°F), blood pressure 95/50 mm Hg, pulse 130/min, and respiratory rate 28/min. The patient is alert and responsive. The remainder of the exam is unremarkable. Which of the following is most appropriate for this patient at this visit?
A 15-year-old boy is brought to the Emergency department by ambulance from school. He started the day with some body aches and joint pain but then had several episodes of vomiting and started complaining of a terrible headache. The school nurse called for emergency services. The boy was born at 39 weeks gestation via spontaneous vaginal delivery. He is up to date on all vaccines and is meeting all developmental milestones. Past medical history is noncontributory. He is a good student and enjoys sports. At the hospital, his blood pressure is 120/80 mm Hg, heart rate is 105/min, respiratory rate is 21/min, and his temperature is 38.9°C (102.0°F). On physical exam, he appears drowsy with neck stiffness and sensitivity to light. Kernig’s sign is positive. An ophthalmic exam is performed followed by a lumbar puncture. An aliquot of cerebrospinal fluid is sent to microbiology. A gram stain shows gram-negative diplococci. A smear is prepared on blood agar and grows round, smooth, convex colonies with clearly defined edges. Which of the following would identify the described pathogen?
A 20-week-old infant is brought to an urgent care clinic by her mother because she has not been eating well for the past 2 days. The mother said her daughter has also been "floppy" since yesterday morning and has been unable to move or open her eyes since the afternoon of the same day. The child has recently started solid foods, like cereals sweetened with honey. There is no history of loose, watery stools. On examination, the child is lethargic with lax muscle tone. She does not have a fever or apparent respiratory distress. What is the most likely mode of transmission of the pathogen responsible for this patient’s condition?
An 8-year-old boy is brought to the physician because of worsening confusion and lethargy for the last hour. He has had high-grade fever, productive cough, fatigue, and malaise for 2 days. He was diagnosed with sickle cell anemia at the age of 2 years but has not seen a physician in over a year. His temperature is 38.9°C (102°F), pulse is 133/min, respirations are 33/min, and blood pressure is 86/48 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 92%. The patient does not respond to verbal commands. Examination shows conjunctival pallor and scleral icterus. Inspiratory crackles are heard at the left lung base. Laboratory studies show: Hemoglobin 8.1 g/dL Leukocyte count 17,000/mm3 Platelet count 200,000/mm3 Which of the following is most likely to have prevented this patient's condition?
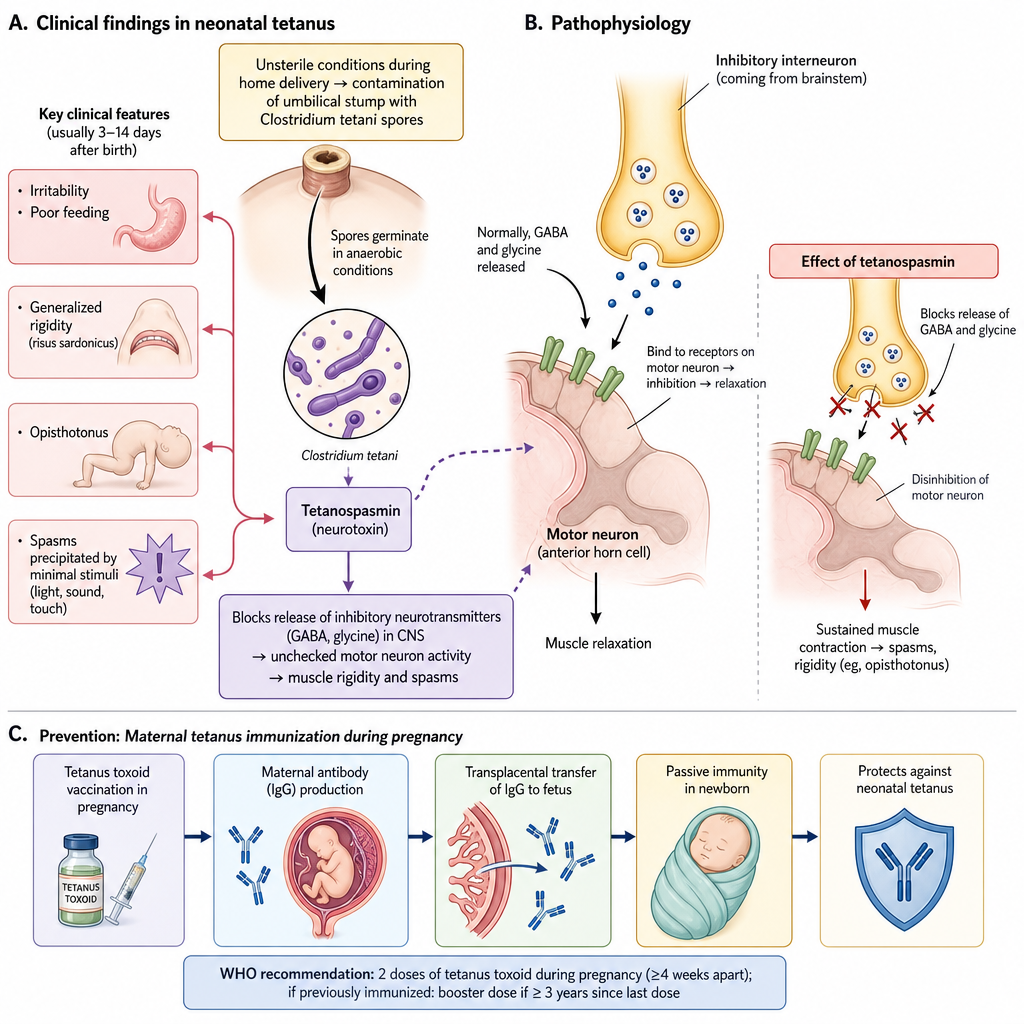
A one-week-old boy is brought to the emergency department by his mother, who recently immigrated to the United States and does not have health insurance. He was born at home, and has not received any medical care since birth. The mother states the boy has become irritable and has been feeding poorly. In the last day, she said he seems "stiff" and is having apparent muscle spasms. On your exam, you note the findings in figure A. Which of the following interventions might have prevented this disease?
A 4-year-old boy is brought to the emergency department with difficulty breathing. His mother reports that he developed a fever last night and began to have trouble breathing this morning. The boy was born at 39 weeks gestation via spontaneous vaginal delivery. He is unvaccinated (conscientious objection by the family) and is meeting all developmental milestones. At the hospital, his vitals are temperature 39.8°C (103.6°F), pulse 122/min, respiration rate 33/min, blood pressure 110/66 mm Hg, and SpO2 93% on room air. On physical examination, he appears ill with his neck hyperextended and chin protruding. His voice is muffled and is drooling. The pediatrician explains that there is one particular bacteria that commonly causes these symptoms. At what age should the patient have first received vaccination to prevent this condition from this particular bacteria?
A 24-year-old newly immigrated mother arrives to the clinic to discuss breastfeeding options for her newborn child. Her medical history is unclear as she has recently arrived from Sub-Saharan Africa. You tell her that unfortunately she will not be able to breastfeed until further testing is performed. Which of the following infections is an absolute contraindication to breastfeeding?
A 3-year-old boy is brought to the physician because of a 3-day history of a pruritic skin rash on his chest. His mother says that he has no history of dermatological problems. He was born at term and has been healthy except for recurrent episodes of otitis media. His immunizations are up-to-date. He appears pale. His temperature is 37°C (98.6°F), pulse is 110/min, respirations are 26/min, and blood pressure is 102/62 mm Hg. Examination shows vesicles and flaccid bullae with thin brown crusts on the chest. Lateral traction of the surrounding skin leads to sloughing. Examination of the oral mucosa shows no abnormalities. Complete blood count is within the reference range. Which of the following is the most likely diagnosis?
A 16-month-old male patient, with no significant past medical history, is brought into the emergency department for the second time in 5 days with tachypnea, expiratory wheezes and hypoxia. The patient presented to the emergency department initially due to rhinorrhea, fever and cough. He was treated with nasal suctioning and discharged home. The mother states that, over the past 5 days, the patient has started breathing faster with chest retractions. His vital signs are significant for a temperature of 100.7 F, respiratory rate of 45 and oxygen saturation of 90%. What is the most appropriate treatment for this patient?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
