Neonatal candidiasis — MCQs

A neonate born at 33 weeks is transferred to the NICU after a complicated pregnancy and C-section. A week after being admitted, he developed a fever and became lethargic and minimally responsive to stimuli. A lumbar puncture is performed that reveals the following: Appearance Cloudy Protein 64 mg/dL Glucose 22 mg/dL Pressure 330 mm H20 Cells 295 cells/mm³ (> 90% PMN) A specimen is sent to microbiology and reveals gram-negative rods. Which of the following is the next appropriate step in management?
A 74-year-old man is admitted to the medical ward after he developed a fungal infection. He has aplastic anemia. The most recent absolute neutrophil count was 450/µL. An anti-fungal agent is administered that inhibits the fungal enzyme, (1→3)-β-D-glucan synthase, and thereby disrupts the integrity of the fungal cell wall. He responds well to the treatment. Although amphotericin B is more efficacious for his condition, it was not used because of the side effect profile. What was the most likely infection?
A 3-month-old male is brought to the emergency room by his mother who reports that the child has a fever. The child was born at 39 weeks of gestation and is at the 15th and 10th percentiles for height and weight, respectively. The child has a history of eczema. Physical examination reveals an erythematous fluctuant mass on the patient's inner thigh. His temperature is 101.1°F (38.4°C), blood pressure is 125/70 mmHg, pulse is 120/min, and respirations are 22/min. The mass is drained and the child is started on broad-spectrum antibiotics until the culture returns. The physician also orders a flow cytometry reduction of dihydrorhodamine, which is found to be abnormal. This patient is at increased risk of infections with which of the following organisms?
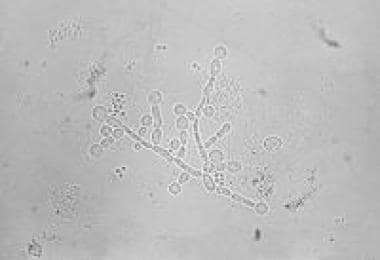
A 29-year-old woman, gravida 2, para 1, at 10 weeks' gestation comes to the physician for a prenatal visit. Over the past two weeks, she has felt nauseous in the morning and has had vulvar pruritus and dysuria that started 5 days ago. Her first child was delivered by lower segment transverse cesarean section because of macrosomia from gestational diabetes. Her gestational diabetes resolved after the child was born. She appears well. Ultrasound confirms fetal heart tones and an intrauterine pregnancy. Speculum exam shows a whitish chunky discharge. Her vaginal pH is 4.2. A wet mount is performed and microscopic examination is shown. Which of the following is the most appropriate treatment?
A 41-year-old HIV-positive male presents to the ER with a 4-day history of headaches and nuchal rigidity. A lumbar puncture shows an increase in CSF protein and a decrease in CSF glucose. When stained with India ink, light microscopy of the patient’s CSF reveals encapsulated yeast with narrow-based buds. Assuming a single pathogenic organism is responsible for this patient’s symptoms, which of the following diagnostic test results would also be expected in this patient?
A mother delivers in a rural area under the guidance of a skilled care attendant. Which of the following statements is incorrect regarding the care provided by the skilled care attendant at birth?
A 15-month-old boy is brought to the pediatrician’s office by his mother due to abnormal muscle tone and an inability to walk. He was able to control his head at 5 months of age, roll at 8 months of age, sit at 11 months of age, and develop hand preference at 13 months of age. On physical exam, he is observed to asymmetrically crawl. He has a velocity-dependent increase in tone and 3+ biceps and patellar reflexes. His startle, asymmetric tonic neck, and Babinski reflexes are present. Which of the following is the most common risk factor for developing this patient’s clinical presentation?
A 4-week-old male presents with his parents to the pediatrician for a well-child visit. The patient’s mother reports that the patient was eating well until about one week ago, when he began vomiting after breastfeeding. His mother has tried increasing the frequency of feeds and decreasing the amount of each feed, but the vomiting seems to be getting worse. The patient now vomits after every feed. His mother states the vomitus looks like breastmilk. The patient’s mother is exclusively breastfeeding and would prefer not to switch to formula but worries that the patient is not getting the nutrition he needs. Two weeks ago, the patient was in the 75th percentile for weight and 70th for height. He is now in the 60th percentile for weight and 68th percentile for height. On physical exam, the patient has dry mucous membranes. His abdomen is soft and non-distended. Which of the following is the best next step in management?
A 3-year-old boy is brought to the physician because of a 3-day history of a pruritic skin rash on his chest. His mother says that he has no history of dermatological problems. He was born at term and has been healthy except for recurrent episodes of otitis media. His immunizations are up-to-date. He appears pale. His temperature is 37°C (98.6°F), pulse is 110/min, respirations are 26/min, and blood pressure is 102/62 mm Hg. Examination shows vesicles and flaccid bullae with thin brown crusts on the chest. Lateral traction of the surrounding skin leads to sloughing. Examination of the oral mucosa shows no abnormalities. Complete blood count is within the reference range. Which of the following is the most likely diagnosis?
A 13-month-old girl is brought to the physician because of a pruritic rash for 2 days. The girl's mother says she noticed a few isolated skin lesions on her trunk two days ago that appear to be itching. The girl received her routine immunizations 18 days ago. Her mother has been giving her ibuprofen for her symptoms. The patient has no known sick contacts. She is at the 71st percentile for height and the 64th percentile for weight. She is in no acute distress. Her temperature is 38.1°C (100.6°F), pulse is 120/min, and respirations are 26/min. Examination shows a few maculopapular and pustular lesions distributed over the face and trunk. There are some excoriation marks and crusted lesions as well. Which of the following is the most likely explanation for these findings?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
