Neonatal infections — MCQs

On this page
Vitamin K supplementation is given to neonates to prevent _____ .
A mother delivers in a rural area under the guidance of a skilled care attendant. Which of the following statements is incorrect regarding the care provided by the skilled care attendant at birth?
A baby presents with hydrocephalus, intracranial calcifications, and chorioretinitis. What is the most probable diagnosis?
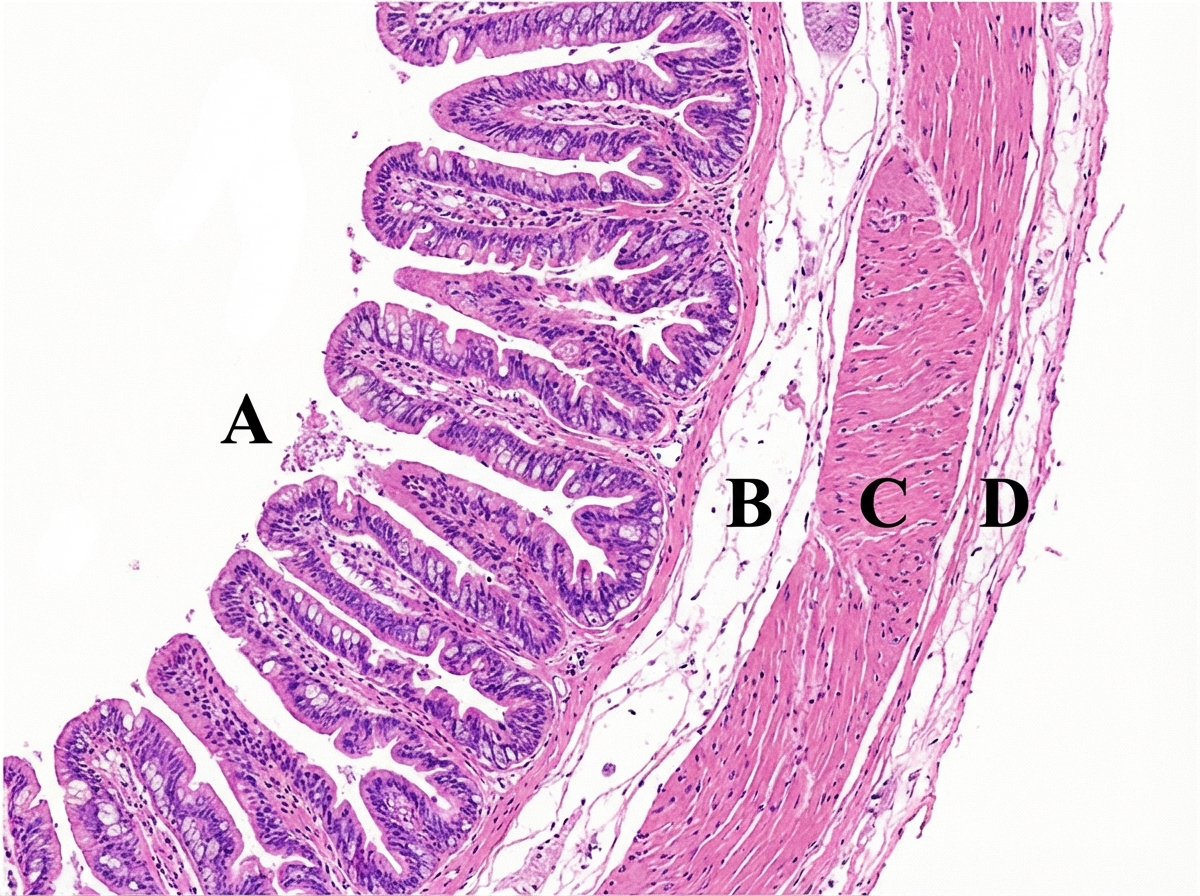
A neonate presents with failure to pass meconium. The structure absent in the pathology lies in which of the following layers?
A 5-day-old, 2200 g (4 lb 14 oz) male newborn is brought to the physician because of poor feeding and irritability. He was born at 36 weeks' gestation after the pregnancy was complicated by premature rupture of membranes. His APGAR scores at delivery were 5 and 8 at 1 and 5 minutes, respectively. He appears lethargic. His temperature is 38.5°C (101.3°F), pulse is 170/min, and respirations are 63/min. Examination shows scleral icterus. Subcostal retractions and nasal flaring are present. Capillary refill time is 4 seconds. Laboratory studies are ordered and an x-ray of the chest is scheduled. Which of the following is the most appropriate next step in management?
A 9-hour-old newborn female is found in the newborn nursery with a diffuse swelling of the scalp not present at birth. The child was born at 38 weeks of gestation to a 28-year-old gravida 3. The mother went into spontaneous labor, but the delivery was complicated by a prolonged second stage of labor. A vacuum-assisted vaginal delivery was eventually performed. The child’s Apgar scores were 8 and 9 at 1 and 5 minutes, respectively. The pregnancy was complicated by preeclampsia in the mother which was well-controlled throughout the pregnancy. On physical exam, the child appears to be in mild distress and has a 4x5 cm ecchymotic area of swelling over the bilateral parietal bones. Serial assessments of the child’s head circumference over the next 12 hours show no change in the size of the swelling. This patient’s condition affects which of the following spaces or potential spaces?
A 2-week-old neonate in the intensive care unit presents as severely ill. His mother says he was a bit irritated earlier this week, and his condition deteriorated quickly. It is apparent that he is in constant pain. He could not be fed easily and vomited three times since yesterday alone. The physical examination is remarkable for a distended abdomen and diminished bowel sounds. The neonate is sent for an abdominal/chest X-ray, which shows pneumatosis intestinalis and pneumoperitoneum. The neonate was born at 32 weeks of gestation by a normal vaginal delivery. Which of the following is the best next step for this patient?
A 4670-g (10-lb 5-oz) male newborn is delivered at term to a 26-year-old woman after prolonged labor. Apgar scores are 9 and 9 at 1 and 5 minutes. Examination in the delivery room shows swelling, tenderness, and crepitus over the left clavicle. There is decreased movement of the left upper extremity. Movement of the hands and wrists are normal. A grasping reflex is normal in both hands. An asymmetric Moro reflex is present. The remainder of the examination shows no abnormalities and an anteroposterior x-ray confirms the diagnosis. Which of the following is the most appropriate next step in management?
A 1-month-old girl is brought to the physician for evaluation of a rash on her face that first appeared 3 days ago. She was delivered at term after an uncomplicated pregnancy. She is at the 25th percentile for length and 40th percentile for weight. Examination shows small perioral vesicles surrounded by erythema and honey-colored crusts. Laboratory studies show: At birth Day 30 Hemoglobin 18.0 g/dL 15.1 g/dL Leukocyte count 7,600/mm³ 6,830/mm³ Segmented neutrophils 2% 3% Eosinophils 13% 10% Lymphocytes 60% 63% Monocytes 25% 24% Platelet count 220,000/mm³ 223,000/mm³ Which of the following underlying conditions is most likely responsible for this patient's predisposition to skin infections?
A newborn is evaluated by the on-call pediatrician. She was born at 33 weeks gestation via spontaneous vaginal delivery to a 34-year-old G1P1. The pregnancy was complicated by poorly controlled diabetes mellitus type 2. Her birth weight was 3,700 g and the appearance, pulse, grimace, activity, and respiration (APGAR) scores were 7 and 8 at 1 and 5 minutes, respectively. The umbilical cord had 3 vessels and the placenta was tan-red with all cotyledons intact. Fetal membranes were tan-white and semi-translucent. The normal-appearing placenta and cord were sent to pathology for further evaluation. On physical exam, the newborn’s vital signs include: temperature 36.8°C (98.2°F), blood pressure 60/44 mm Hg, pulse 185/min, and respiratory rate 74/min. She presents with nasal flaring, subcostal retractions, and mild cyanosis. Breath sounds are decreased at the bases of both lungs. Arterial blood gas results include a pH of 6.91, partial pressure of carbon dioxide (PaCO2) 97 mm Hg, partial pressure of oxygen (PaO2) 25 mm Hg, and base excess of 15.5 mmol/L (reference range: ± 3 mmol/L). What is the most likely diagnosis?
Practice by Chapter
Early-onset sepsis
Practice Questions
Late-onset sepsis
Practice Questions
Group B streptococcal disease
Practice Questions
Neonatal meningitis
Practice Questions
Congenital TORCH infections
Practice Questions
Neonatal HSV
Practice Questions
Neonatal candidiasis
Practice Questions
Necrotizing enterocolitis
Practice Questions
Omphalitis
Practice Questions
Nursery outbreaks
Practice Questions
Antibiotic stewardship in NICU
Practice Questions
Diagnostic approach to neonatal sepsis
Practice Questions
Maternal factors and neonatal infection risk
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
